Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2637-6636
Case Report(ISSN: 2637-6636) 
Self-Inflicted Oral Mucosal Injuries in Pediatric Patients: A Case Series Volume 6 - Issue 4
Stoufi DE1,2*, Georgaki M1, Tsouri I3 and Nikitakis NG4
1Scientific Associate, Department of Oral Medicine & Pathology and Hospital Dentistry, School of Dentistry, National and Kapodistrian University of Athens (NKUA), Athens, Greece
2Visiting Lecturer, Harvard School of Dental Medicine, Greece
3Postgraduate Student, Department of Oral Medicine & Pathology and Hospital Dentistry, School of Dentistry, Greece
4Professor and Chair, Department of Oral Medicine & Pathology and Hospital Dentistry, School of Dentistry, Greece
Received:August 23, 2021 Published: August 31, 2021
*Corresponding author: Stoufi DE, Scientific Associate, Department of Oral Medicine & Pathology and Hospital Dentistry, School of Dentistry, National and Kapodistrian University of Athens (NKUA), Athens, Greece
DOI: 10.32474/IPDOAJ.2021.06.000244
Abstract
Self-Injurious Behaviour (SIB) is a deliberate harm that may lead to factitial injuries in various parts of the body including the oral mucosa. It may present with a confusing clinical appearance leading to misdiagnosis as a variety of oral diseases [1]. A case series is presented here outlining 2 cases of self-induced oral mucosal injury, which presented initially with extensive oral ulcers. These cases were investigated to rule out systemic or local causes, in order to establish an accurate diagnosis. A multidisciplinary approach to treating these conditions, which may be associated with several medical conditions, is necessary, necessitating the engagement of patients, parents and medical and dental teams [2].
Introduction
Oral self-injuries may sometimes pose one of the more frustrating problems for the diagnostician. The self-injury can be premeditated, accidental or can be the result of an unconscious habit [3]. Those injuries that are premeditated have underlying causes that are functional or organic in origin [4]. Functional self-injurious behaviour (SIB) describes a form of behavioral disorder characterized by an intentional damage to a part of the body without suicidal intent. It may be used as a means of escape from responsibility or attention seeking and has been found to occur more often at times of stress, hunger, anger, frustration and as a reaction to bullying. Organic causes of SIB are secondary to genetic defects and abnormal neurophysiology, such as Lesch- Nyhan syndrome, Munchausen syndrome, familial dysautonomia and congenital insensitivity to pain, as well as other entities, such as autism, mental retardation, hereditary sensory neuropathies and encephalitis. In these patients, the injuries are inflicted unconsciously, in a compulsive form without specific intent [1,4]. SIB is more prevalent in children under 12 years of age. Its prevalence has appeared to be growing markedly over the last 20 years, from affecting 400 per 100,000 in the early 1980s to 1000 per 100,000 in the late 1990s in the general population with a 23- 40% increase among severely developmentally delayed individuals [4]. However, because such behaviors are not considered socially acceptable, the exact prevalence of self-mutilation in the world is uncertain and probably undereported and underestimated.
About 75% of SIB lesions are located in the head and neck region and ican be caused by repeated biting of tissues or by inserting foreign objects and fingernails to the oral mucosa. Clinically, these actions can present as hyperkeratotic, erythematous or ulcerated painful lesion and more rarely may result in tissue loss in extreme cases of self-mutilation. Due to chronic inflammation, the ensuing ulcers may become irregular with vegetations, raised border and indurated base, clinically resembling more ominous conditions. Differential diagnosis is made among other ulcerative and erythematous lesions, ranging from mechanical injuries, thermal or electrical burns, aphthous ulcers, tuberculosis, and eosinophilic ulcer, to squamous cell carcinoma, leukemia, and other malignancies. The diagnosis depends on a strong clinical suspicion, detailed history and a thorough examination. Occasionally, when a diagnostic dilemma exists, or ulceration persists longer than 10-14 days, biopsy and histopathologic examination is suggested to rule out other diseases. Microscopically, a non-specific ulcer is seen; the surface is covered by fibrinopurulent exudate containing inflammatory cells, while the floor of the ulcer consists of granulation tissue intermixed with neutrophils, lymphocytes, histiocytes, plasma cells and eosinophils.
Here,
Cases Presentation
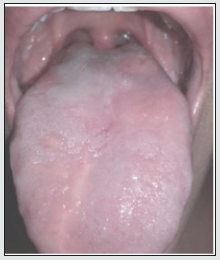
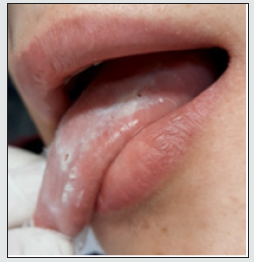
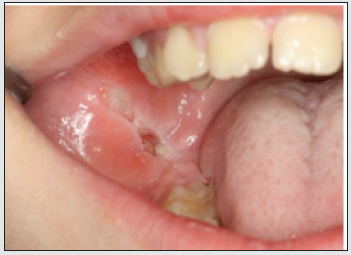
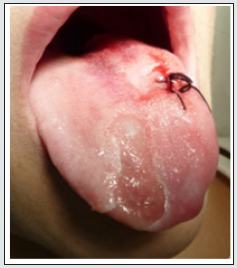
Case 1: A 12-year-old boy was referred with a 4-month history of extensive tongue ulcers (Figure 1). He was healthy and denied any habit of tongue biting. A biopsy was performed (Figure 2) and histopathology examination showed non-specific chronic inflammation. Results of other laboratory studies, including full blood count, were normal. Detailed patient’s social history revealed that the patient had a new sibling and felt neglected. Therefore, we hypothesized self-harm for attention seeking, which led to the presumptive diagnosis of factitial oral ulcers. Treatment consisted of low dose of corticosteroids per os for 1 week. We also advised parents to seek specialized psychological treatment to help the boy with the new family routine. At 3-months follow-up appointment (Figure 3), we observed total remission of the lesions. Thus, the diagnosis of factitial oral ulcers was clinically confirmed by the case resolution. However, the same patient 6 years later returned on his own seeking for help. He had started again biting his tongue (Figure 4), because he was emotionally distressed from school exams. He was administered low dose of corticosteroids per os and was referred to a psychologist for mental support. Follow-up revealed that the patient was able to handle his problem.
Case 2: A 12-year-old male boy was referred from Children’s Hospital due to ulcerations in the right buccal mucosa (Figure 5). The lesion was persistent for 3 months with regional lymphadenopathy; low fever and loss of weight were also reported. The origin of the lesions was not suspected initially by the various clinicians who examined the patient. Detailed history revealed family problems, due to parents’ divorce; after careful questioning, it was revealed that the patient was injuring himself with a stapler. Upon palpation, one staple popped out from the lesion. The patient and his parents were referred for counseling and psychological support.
Figure 1: Extensive self-inflicted tongue lesions persistent for 4 months at first clinical examination.
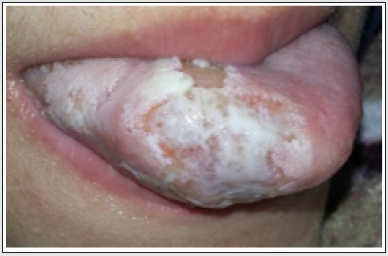
Figure 2: Clinical examination after biopsy and initiation of treatment; the clinical apperance has been improved with partial repair of the lesions.
Discussion
The wide range of the clinical presentation of the oral lesions induced by self-injury, often not specific and mimicking several other diseases, could make the diagnosis a challenge for clinicians, especially when the lesions are the first or the unique signs of psychological distress [2]. The denial of the causative parafunctional habit by the patient, as well as the frequent unwillingness of the parents to accept the emotional and psychological disturbance of their child, may further perplex diagnosis and management.
The presented clinical cases were linked directly to emotional stress caused by a change in the family dynamics. Therefore, we emphasize the great importance of taking a good medical, family, and social history, which provides significant information about the development of current and previous lesions, the patient’s habits and the current emotional status [5]. Early diagnosis of these lesions and the recognition of their risk factors enable a more conservative clinical approach and the maintenance of the anatomical and physiological health of oral and perioral structures. Due to the lack of available literature on this topic, the establishment of a standardized treatment protocol is difficult. To achieve successful outcomes, the treatment should be individually tailored for each patient, with focus on a multidisciplinary approach, including psychotherapy and periodic clinical control of possible recurrences [5,6]. A compassionate and professional approach by the whole team increases rapport with the patient and the family and facilitates both the realization of the problem and its successful management.
References
- Limeres J, Feijoo JF, Baluja F, Seoane JM, Diniz M, et. al. (2013) Oral self-injury: an update. Dent Traumatol 29: 8-14.
- Gonçalves PS, Mendez DA, Santos PS, Damante JH, Rios D, et al. (2017) The Diagnosis and Treatment of Multiple Factitious Oral Ulcers in a 6-Year-Old Boy. Case Rep Dent 2017:1986834.
- Rawal SY, Claman LJ, Kalmar JR, Tatakis DN (2004) Traumatic lesions of the gingiva: a case series. J Periodontol 75(5): 762-769.
- Medina AC, Sogbe R, Gomez-Rey AM, Mata M (2003) Factitial oral lesions in an autistic paediatric patient. Int J Paediatr Dent 13: 130-137.
- Kotansky K, Goldberg M, Tenenbaum HC, Mock D (1995) Factitious Injury of the Oral Mucosa: A Case Series. Journal of Periodontology 66(3): 241–245.
- Cannavale R, Itro A, Campisi G, Compilato D, Colella G (2015) Oral self-injuries: clinical findings in a series of 19 patients. Med Oral Patol Oral Cir Bucal 20(2): e123-e129.
Editorial Manager:
Email:
pediatricdentistry@lupinepublishers.com

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...