Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2637-6636
Review Article(ISSN: 2637-6636) 
Congenital Infections and Dental and Oral Involvement Volume 6 - Issue 4
Sayan Bhattacharyya1* and Satarupa Ghosal Bhattacharyya2
1Assistant Professor, Department of Microbiology, AIIH&PH, India
2BDS, Dental Surgeon, India
Received:August 05, 2021 Published: August 16, 2021
*Corresponding author: Sayan Bhattacharyya, Assistant Professor, Department of Microbiology, AIIH&PH, India
DOI: 10.32474/IPDOAJ.2021.06.000242
Abstract
Many congenital bacterial, viral and parasitic infections can lead to dental and oral involvement. Studying them is important from clinical and epidemiology point of view. They can lead to myriad signs and symptoms. Hence they have to be detected, differentiated and managed early as far as possible. They can be prevented also by vaccination. We here have tried to collate available information in medical literature about these.
Introduction
Many bacterial, viral and parasitic infections can be transmitted congenitally. They can lead to congenital infection in the newborn in utero, producing many clinical features involving the teeth, lips and mouth cavity. These features are seen along with other systemic involvements. These have to be studied well for proper management. Unfortunately, no comprehensive literature is there to review such infections. We hence try here to collect and present existing information about it.
Materials and Methods
We reviewed literature available in books and journals across internet to prepare the review article.
Congenital Rubella syndrome
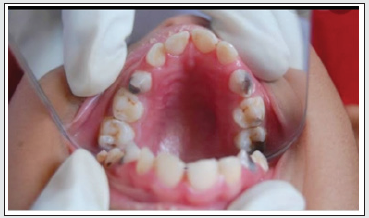
This infection was very commonly reported once upon a time and still not very rare. Congenital rubella syndrome (CRS) has a quite low rate of occurrence now. It has been expected to reduce to 1 case per 100000 live births. The infection can be acquired by contact with the Rubella virus belonging to the Togaviridae family of RNA viruses during pregnancy. Fetal development is completely deranged once the virus is transmitted to the developing foetus in utero [1]. Patients with CRS are usually considered special patients with exaggerated dental problems. This is usually due to lacking manual skills and failure on the part of caretakers to provide timely oral disease prevention , as because they consider it secondary owing to the grave systemic problems the patient suffers from [2]. The infected child may be unable to chew, and her diet usually comprises soft foods. Intraoral examination can reveal caries of teeth. The lower anterior teeth can be diagnosed congenitally missing owing to a knife edged alveolar ridge . Also, the maxillary arch can be unusually narrow, and the palate can be deep [2].Prevention can be done by MMR (Measles-Mumps- Rubella) Vaccination of the mother before pregnancy (Figure 1).
Congenital Cytomegalovirus (CMV) infections
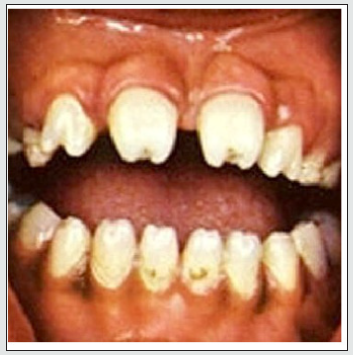
CMV is a DNA virus and member of the Herpesviridae family. Congenital CMV infection can involve many organs and tissues in the newborn, and teeth and oral cavity can also be sometimes involved. Hypoplasia and hypocalcification of tooth enamel are commonly seen in children having congenital CMV infection and hence, regular dental visits are an important part of the long-term care of these infants [3] (Figure 2).
Figure 2: Defects of tooth structure seen in congenital CMV infection (Source: American Academy of Pediatrics).
Congenital Syphilis
Although many physicians, dentists and pathologists in developed countries will be aware of the dental features of congenital syphilis, most will never have seen a case or made the diagnosis. The earliest reference to the dental manifestations of congenital syphilis was by Sir Jonathan Hutchinson, Assistant Surgeon at The London Hospital, England, in 1861 [4]. Dental defects are the most consistent clinical manifestation of syphilis and are pronounced in teeth, which calcify in the first year of life such as permanent incisors and first molars [4]. According to Putkonen (1962) who investigated 235 syphilis patients, 45 % children with permanent incisors showed features of Hutchinson’s form. About 22 % with first permanent molars had Moon’s form. However, only 12 % showed cortical thickening related to periosteitis on radiographs of the limbs .
Hutchison’s incisors
Sir Jonathan Hutchinson also noted that the dental defects were restricted to the permanent teeth. According to Hutchinson the colour of the teeth is also abnormal, the affected teeth being semitranslucent rather than the ivory colour of normal teeth. In incisors affected by congenital syphilis the incisal edge has been described as either notched or ‘screwdriver shaped’. The bulbous crown is described as ‘barrel shaped’ [4].
Moon’s molars
The first description of the characteristic defect of permanent first molars was given by Henry Moon, Dental Surgeon at Guy’s Hospital (1877) [4,5]. He described these teeth as being small and dome shaped, with cusps set closer together than normal. The crowns are widest at the base and the narrowest at the cusps, have no grooves running around the cusps and the crown surface is smooth. These teeth were later referred to as ‘Moon’s molars’ and in some cases as ‘bud molars’, the latter term aptly describing their morphology [4].
Fournier’s molars or mulberry molars
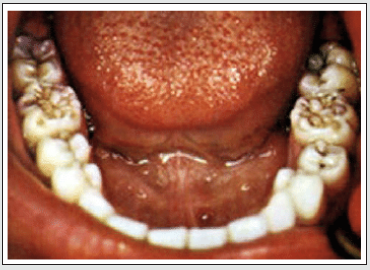
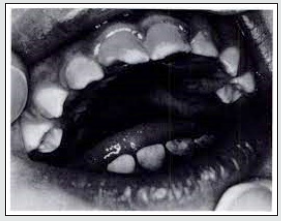
Fournier (1884) described a different form of permanent molar tooth defect associated with congenital syphilis. In this there is a deep groove around the base of each cusp caused by enamel hypoplasia. He described it as ‘a smaller tooth growing out of a larger one, a stump growing from a normal crown’ [4,6]. The defect is clearly very different from that described by Moon and probably results from infection at a slightly different time of development. Though the two defects are distinct, the terms have often been confused, even by the originator of the term mulberry molar, Karnosh, who proposed it to describe both types, though his illustration clearly shows Fournier molars. Syphilitic canine: Several studies describe typical features of a syphilitic canine, but this defect is less commonly found than other incisor and molar defects. According to an archeological study, maxillary and mandibular canines are as characteristic in morphology as the upper central incisors and are bulbous column-like pegs with an occlusal notch. They also have an elevated ring of enamel on the occlusal surface [4,7]. The tell-tale feature in Congenital syphilis is Hutchinson’s triad which is characterized by peg shaped upper central incisors, and interstitial keratitis which consists of blurred vision, abnormal tearing, eye pain and abnormal sensitivity to light, saddle nose, bony prominence of the forehead (frontal bossing), high arched palate, short upper jawbone, neural deafness and fissuring around mouth and anus [8]. Interestingly, Mercurial poisoning was noted by Sir Hutchinson to grossly affect tooth development producing abnormalities of enamel formation . Mercury had been used to treat congenital syphilis but can also involve teeth in the newborn. These may interfere with the expression of “classic” dental signs of congenital syphilis [9] (Figures 3 & 4).
Congenital Toxoplasmosis
Congenital toxoplasmosis leads to CNS and pulmonary involvement in the newborn, and does not cause dental affection per se. However, the sugar suspending agents used for delivering drugs like Pyrimethamine and Leucovorin, that are used to treat the babies infected with congenital toxoplasmosis, can lead to dental caries. Hence teeth have to be cleaned well after medicine administration [10].
Congenital Epstein-Barr virus infection
Congenital infection by Epstein-Barr virus usually produces no or little symptoms in the newborn. Rarely micrognathia or small jaw may be reported along with other constitutional symptoms like Cryptorchidism, thrombocytopenia, hypotonia and petechial hemorrhagic spots [11].
Congenital Zika virus infections and dental affection
Children born to mothers infected with Zika virus can have incomplete deciduous dentition. The abnormal chronology of dental eruption and dental development disturbances in children with microcephaly infected with ZIKV born to infected mothers indicate a possible role of the virus in odontogenesis [12]. In another study, a higher frequency of the following oral conditions was observed in Zika virus infected mothers: delayed eruption chronology (100%), dental biofilm (55.88%) and enamel defects (DDE) (22.06%). Bohn nodules (6.85%), micro dents (2.70%) and ectopically positioned dental elements (1.35%) were less frequent. Only one of the cases showed incipient caries lesion (1.47%). In this study, the occurrence of DDE was more frequent among those with ogival palate, normal weight at birth and who did not have an eruptive delay (p <0.05) [13]. Hence, monitoring oral health conditions is necessary to minimize oral health problems in these children.
Discussion
Many congenital infections can have oral and dental involvement. Either they themselves affect the teeth or oral cavity of the newborn child, or it is due to the drugs administered to treat these conditions. Hence proper history taking, and investigations are needed to pick them. It is also important to study this because many congenital diseases can involve teeth and oral cavity and features may also be overlapping.
Conclusion
Congenital infections affecting teeth and oral cavity can present variably and hence have to be managed and detected early for optimum results.
Acknowledgement
Authors acknowledge the works of all scientists which have been quoted here.
References
- Chakravarti A, Jain M (2006) Rubella prevalence and its transmission in children. J Clin Virol 35: 285-291.
- Ahuja R, Shigli AL, Thakur G, Jain U (2015) Dental manifestations of congenital rubella syndrome. BMJ Case Rep 2015: bcr2015209382.
- Swanson EC, Schleiss MR (2013) Congenital cytomegalovirus infection: new prospects for prevention and therapy. Pediatr Clin North Am 60(2): 335-349.
- Nissanka-Jayasuriya EH, Odell EW, Phillips C (2016) Dental Stigmata of Congenital Syphilis: A Historic Review With Present Day Relevance. Head Neck Pathol 10(3): 327-331.
- Moon H (1877) On irregular and defective tooth development. Trans Odontol Soc GB 9: 223-243.
- Fournier A (1884) Syphilitic teeth. Dent Cosmos 26: 12-25.
- Jacobi KP, Cook DC, Corruccini RS, Handler JS (1992) Congenital syphilis in the past: slaves at Newton Plantation, Barbados, West Indies. Am J Phys Anthropol 89(2): 145-158.
- Congenital Syphilis.
- Ioannou S, Henneberg M, Henneberg RJ, Anson T (2015) Diagnosis of Mercurial Teeth in a Possible Case of Congenital Syphilis and Tuberculosis in a 19th Century Child Skeleton. Journal of Anthropology 2015(1): 11.
- Goldberg GN, Fulginiti VA, Ray CG, Ferry P, Jones JF, et al. (1981) In utero Epstein-Barr virus (infectious mononucleosis) infection. J Am Med Assoc 246(14): 1579-1581.
- McLeod R, Lykins J, Gwendolyn Noble A (2014) Management of Congenital Toxoplasmosis. Curr Pediatr Rep 2: 166-194 .
- Silva MCPMD, Arnaud MA, Lyra MCA, Alencar Filho AV, Rocha MÂW, et al. (2020) Dental development in children born to Zikv-infected mothers: a case-based study. Arch Oral Biol 110: 104598.
- Agostino ESD, Chagas JRLP, Almeida TF (2020) Developmental enamel defects and other oral problems in children with microcephaly associated with fetal exposure to zika virus (ZIKV). Int J Pregn & Chi Birth 6(3): 67-74.
Editorial Manager:
Email:
pediatricdentistry@lupinepublishers.com

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...