Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-6070
Research Article(ISSN: 2638-6070) 
Does Nutrition Education Improved Complementary Feeding Practices in Ondo State, Nigeria? a Cluster Randomized Controlled Trial
Volume 2 - Issue 2Akinrinmade Remilekun1*, Ogada IA2, Njogu E3 and Keshinro OO4
- 1Rufus Giwa Polytechnic Owo, Nigeria
- 2St. Francis Xavier University, Canada
- 3Kenyatta University, Nairobi, Kenya
- 4University of Ibadan, Ibadan Nigeria
Received: July 24, 2019; Published: August 16, 2019
*Corresponding author: Akinrinmade Remilekun, Rufus Giwa Polytechnic Owo, Nigeria
DOI: 10.32474/SJFN.2019.02.132
Abstract
This study showed the effect of nutrition education on complementary feeding practices among caregivers in Ondo State, Nigeria. The study was a cluster randomized controlled-trial design. The study participants were in two groups. One was intervention and the other one was the control group in a ratio of 1:1. The sample size was 282; the intervention group was 142 and the control group was 142. Intervention on complementary feeding was carried out inform of nutrition education among the caregivers in the intervention group and the control group received no intervention. The intervention group received four 4 lesson sessions per group. The sessions were based on continued breastfeeding, timely introduction of complementary feeding, minimum meal frequency, minimum dietary diversity, minimum acceptable diet, feeding with iron rich foods, responsive feeding and hygiene. Data were analyzed using SPSS version 22.0. From Kaplan-Meier analysis, continued breastfeeding survival at age 11 months was 94.4% in the intervention group and it was 69.7% in the control group. Adjusted Relative Risk [ARR] was used to determine the effect of nutrition education on the intervention group and control group for variables such as Minimum Acceptable Diet [ARR: 3.13; CI: 2.53-5.16; P<0.001] at the end line. This study concluded that nutrition education based on complementary feeding guidelines improved the feeding practices of the caregivers. Therefore, the study recommends that Ministry of Health in Ondo State should encourage complementary feeding training for caregivers and CHEWs at the various Basic Health Centers in the State.
Abbreviation: ARR: Adjusted Relative Risk; BHC: Basic Health Centre; CFP: Complementary Feeding Practices; CHEW: Community Health Extension Workers; EBF: Exclusive Breastfeeding; FAO: Food and Agriculture Organization; HIV: Human Immunodeficiency Virus; ICF: International Classification of Functions, disability and health; IEC: Information Education Communication; IG: Intervention Group; IYCF: Infant and Young Child Feeding; LGA: Local Government Areas; MDD: Minimum Dietary Diversity; MMF: Minimum Meal Frequency; MAD: Minimum Acceptable Diet; NCP: National Population Commission [Nigeria]; NDHS: Nigeria Demographic and Health Survey; NGOs: Non-governmental organizations; NNHS: National Nutrition and Health Survey; OSHREC: Ondo State Health Research Ethics Committee; OSPHCDB: Ondo State Primary Health Care Development Board; SMART: Standardized Monitory and Assessment of Relief and Transition
Introduction
The UNICEF showed that globally 66% of children aged 6 to 8 months received semi-solid, solid or soft foods, with cases of nutrition deficiencies due to untimely introduction of complementary foods [1]. The timely introduction of complementary feeding among caregivers in sub-Sahara Africa was 71% and 68% for West and Central African countries while it was 67% for Nigeria [1]. Children receiving MAD was 11% in sub-Sahara Africa, 9% in West and Central African countries and 10% in Nigeria [1]. Infants feeding practices reports available in some other West African nations showed poor practices of MAD by caregivers in Ghana [13%] and in Benin Republic [9%] [1]. The report of the Nigerian National Demographic and Health Survey [2] indicated that only 11% of the breastfed infants received complementary foods from at least
four food groups. Globally, about 45% of infants less than 6 months of age were exclusively breastfed [EBF], with 42% in sub-Sahara Africa and 29% for West and Central African countries. In Nigeria, EBF rate is at 17%, which implies that 83% have had untimely introduction of complementary feeding [1]. The issues of poor infants feeding knowledge and practices among caregivers which result to poor nutrition status among the infants call for action due to the present level of malnutrition in Nigeria.Standardized Monitory and Assessment of Relief and Transition reported that 21.1% of children less than five years of age in South West Nigeria, the Geo-political Zone of this study were stunted [3]. Malnutrition caused the death of 53% of children less than five years of age in Nigeria [4]. It also showed that 13% of the death could be averted if 90% of mothers in Nigeria practiced exclusive breastfeeding for the first six months. If the same mothers practiced timely introduction of complementary feeding, a further 6% of the death rate could be prevented [5]. Inadequacy in complementary feeding during infancy and childhood has been demonstrated by researchers as a factor that leads to malnutrition, resulting in higher mortality and morbidity rate among the children [6]. In Nigeria, poor infants feeding practices rate is high. Apart from lack of adequate complementary feed being provided to the infants, force-feeding practices rather than responsive feeding is reported among 83.8% respondents in Enugu, Nigeria [7]. Only 10% of infants received minimum acceptable diet in the country [1]. The report of National Demographic and Health Survey showed that only 17.6% of infants in the South West Geo-Political Zone received minimum adequate diet [2].
Objectives
a) To implement a nutrition education program using World Health Organization guidelines on complementary feeding for caregivers in Ondo State, based on complementary feeding practices, knowledge and attitudes.
b) Establish the effects of nutrition education on complementary feeding, knowledge, attitudes and practices among caregivers in Ondo State.
Materials and Methods
Research Design
This was a cluster-randomized controlled trial. A randomized controlled trial reduces bias in interventional studies by controlling for known and unknown confounders. It also provides evidence of a causal-effect relationship between the intervention and the outcomes [8,9]. The Basic Health Centres were randomized and not the caregivers to enhance participation by caregivers, by reducing loss to follow-up.
The study had two phases: the needs assessment phase and the intervention phase.
Sample Size
Sample size was determined using [10] for continuous assessment. A total of 290 caregivers were achieved. During the study 6 caregivers were lost to follow-up which resulted to 284 caregivers that completed the study. They were distributed as follows; This resulted into 70 caregivers in the first Basic Health Center for intervention group, 72 in the second BHC for intervention group, 69 in the first BHC for control group and 73 in the second BHC at the end of the study depending on eligibility criteria and willingness of the caregivers to participate in the different communities.
Sampling Techniques
Multi-stage sampling method was adopted for this study. Purposive sampling method was used for the selection of Ondo North Senatorial District out of the three Senatorial Districts in the State. Owo Local Government Area [LGA] due to existing literature [11]. Simple random sampling method was used for the selection of the 4 Basic Health Centres [BHC] out of ten [10] BHCs in the LGA. Randomization was then conducted to assign the BHCs into intervention groups and control group by a biostatistician using MS EXEL at a ratio of 1:1, with each study group having two BHCs. Caregivers were allocated to study group based on the BHCs they attend for post-natal care.
The recruitment of study participants into the study
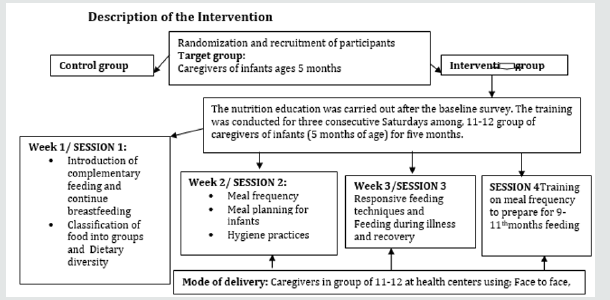
The study participants were recruited by the researcher, assisted by the Community Health Extension Workers [CHEWs]. The researcher together with the CHEWs in the selected BHCs recruited and registered eligible participants [caregivers with infants] into the study at the weekly routine meetings in the BHCs. Daily recruitment was carried out when the caregivers visited the health centres for routine meetings for immunization, appointments and check-ups. Eligible caregivers were recruited in 13, 11 and 10 in numbers in each Basic Health Centres, until the required sample size was achieved. The screening was conducted by the researcher and the Community Health Extension Workers (Figures 1 & 2).
The Training
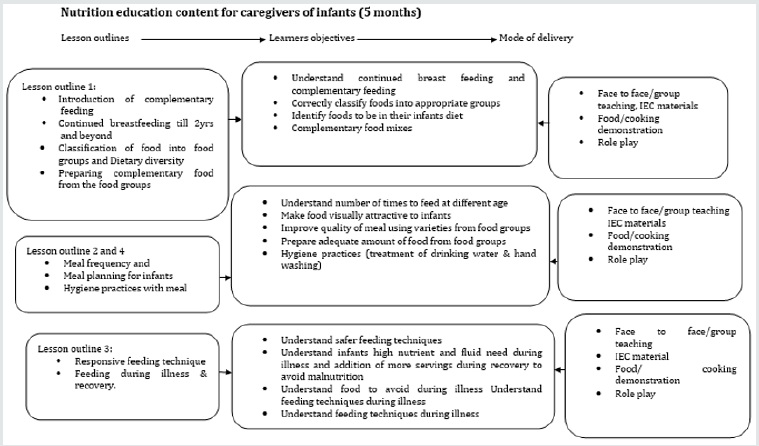
Caregivers in the control group were selected from 2 BHCs and did not receive any intervention from the research team. Meanwhile, the caregivers in the intervention group which were also selected from 2 BHCs received the complementary feeding nutrition education from the research team. The education session began with creating rapport between the researcher [assisted by CHEWs in the research group] and the participants. The training was conducted in the local Yoruba language for better understanding. The content of the nutrition education on complementary feeding was based on the guidelines [12] as well as the knowledge, attitude and practices gaps identified during the need’s assessment. The caregivers received training on continued breastfeeding, dietary diversity, meal frequency, responsive feeding techniques, meal planning for infants, infants’ meal planning during illness and recovery and hygiene [water treatment]. This training was carried out in three consecutive weekends as the caregivers were recruited per group in the respective health centers weekly. After the recruitment and training, the caregivers were followed up during the program. The phone numbers of the caregivers and the CHEW in that zone, where the caregivers resided were also written down by the researchers in case of questions or if need arises to attend to some unclear area of the training pertaining to the study. Two days to and on the eve of visitation day, the enumerator allocated to the area would call to remind the caregivers about the visitation day.
Research Instruments
WHO [2010a] IYCF indicators [13]
WHO [2010b] 24hr. dietary recall on complementary feeding practices [14]
WHO [2004] Complementary feeding guidelines [12] Data analysis
Pilot study was carried out. During the pilot study, training was conducted for caregivers in the intervention group and there was standardization of data collection procedures. Each questionnaire was administered twice on the same group of participants at an interval of two days. A correlation co-efficient of more than 0.7 was considered adequate [Mukaka, 2012]. They are as follows:
a) Baseline questionnaire for the caregivers: 0.89[0.82- 0.92].
b) Second questionnaire for all the caregivers: 0.77[0.61- 0.84].
c) Third questionnaire for all the caregivers: 0.88[0.71- 0.91].
Complementary feeding practices were determined based on the [13] IYCF indicators. Early initiation of breastfeeding was determined thus; proportion of infants who were put to breast within one hour of birth; for exclusive breastfeeding; [proportion of infants 0-5 months who were fed exclusively with breast milk]. For continued breastfeeding, [proportion of infants fed with breast milk in the previous day], For meal frequency [a frequency of 2 times for ages 6-8 months and 3 times for 9-11 months was considered adequate and milk feeding frequency for non-breastfed infants [proportion of infants 6-11 months who received at least 2 milk feedings during the previous day] was considered adequate]. For dietary diversity, a daily intake of 4 or more out of 7 food groups was considered adequate [15]. For consumption of iron rich and iron fortified foods, proportion of infants who received iron rich food or iron fortified food that is designed for infants or that is fortified at home. For responsive feeding, caregivers were expected to encourage the infant to eat the food served. Also, for hygiene, treatment of water by boiling water to boiling point and allow it to cool in a clean container was the acceptable practice.
Feeding practices was determined using the feeding practices variable for the questionnaire according to 24hr. dietary recall on complementary feeding practices [14]. The caregivers that answered yes to right practices was awarded 1 while the caregivers that answered no to right complementary feeding practices was awarded 0. The proportion of each variable was subjected to regression analysis. In addition, adjustment/ controlling for the covariates such as caregivers age and parity was done during the analysis to cater for the design effect because it was the BHCs that were randomized into study groups and not the caregivers.
Logistical and ethical considerations
Ethical clearance was obtained from Ondo State Health Research Ethics Committee [OSHREC]. Letter of introduction to the coordinator of Owo LGA, BHCs was obtained from Ondo State Primary Health Care Development Board [OSPHCDB], Nigeria.
Results
The influence of nutrition education on complementary feeding practices of the caregivers
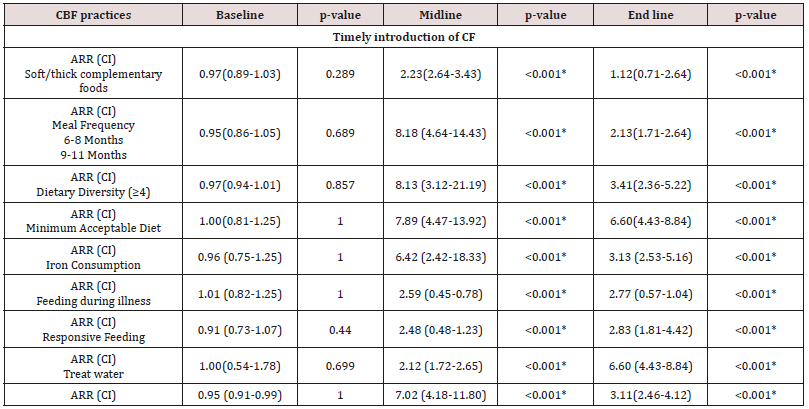
A regression analysis using Adjusted Relative Risk was carried out to determine the effect of the nutrition education on the feeding practices of the caregivers. The caregivers in the intervention group were 8 times more likely to feed the infant with minimum meal frequency than the caregivers in the control group at the midline [ARR: 8.13; CI: 3.12-21.19; p<0.001] and 3.4 times at the end line [ARR: 3.41; CI: 2.36-5.22; p<0.001]. The result showed that caregivers in the intervention group were 7 times more likely to feed their infants with diversified diet in terms of the complementary foods at midline [ARR: 7.89; CI: [4.47-13.92; p<0.001] and 6.7 times at the end line [ARR: 6.66; CI: 4.43-8.84; p p<0.001]. Feeding the infants with minimum acceptable diet was 6.4 times more likely among the caregivers in the intervention group [ARR: 6.42; CI: 2.42-18.33; p<0.001] at the midline and 3 times more likely at the end line [ARR: 3.13; CI: 2.53-5.16; p<0.001] compared to the control group. This shows that the infants in the intervention group were more like to meet the minimum acceptable diet requirement compared to the infants in the control group, both at the midline and at the end line of the study.
Responsive feeding was more likely to be practiced among the caregivers in the intervention group than the caregivers in the control group [ARR: 2.12; CI: 1.72-2.65; p<0.001] at the midline and 6 times more likely at the end line [ARR: 6.60; CI: 4.43-8.84; p<0.001]. The responsive feeding practices were also established by caregivers during the FGDs. This was what a caregiver from the intervention group had to say; I did not believe that the different ways of encouraging the infants to accept complementary food could be achievable because of my experience with my first daughter, but this training helped me. Since the time we were taught on responsive feeding which was demonstrated to us in the health centre, I practiced responsive feeding on my infant and it was achievable.” [CAREGIVER3, FGD2 2017] (Table 1).
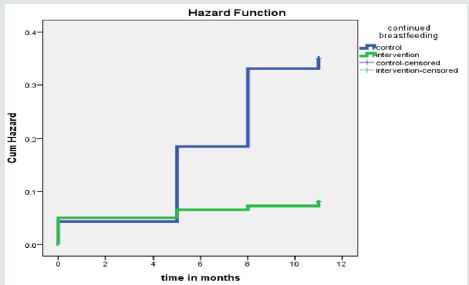
Continued breastfeeding survival analysis
Adjusted Relative Risk analysis showed that 30% of the caregivers in the control group were less likely to continue breastfeeding, compared to the intervention group at the end line [ ARR 0.30; CI: 0.16-0.56; p<0.001]. Additionally, survival analysis was performed on the continued breastfeeding practices of the caregivers in both groups to determine the probability of continued breastfeeding along with complementary feeding among the caregivers. From Kaplan-meire analysis, 69.7% of the caregivers in the control group continued with breastfeeding at age 11 months, compared to 94.4% of the caregivers in the intervention group [p<0.001].
Discussion
Despite research-based evidence on association of adequate complementary feeding practices and child survival. In Nigeria, 70% of caregivers did not have good adequate complementary feeding practices [16,17]. Only 17.5% of Nigerian infants received minimum acceptable diet during complementary feeding by the caregivers [18]. In South western Nigeria, the geopolitical zone where this study was carried out, only 17.8% of infants received minimum acceptable diet [MAD] while in Ondo State, only 11.4% received MAD [2]. This study showed the effect of nutrition education which improved the caregivers’ complementary feeding practices. Prior to the commencement of complementary feeding practices at the baseline, there was no significant difference in the complementary feeding practices in the two groups. Some of the caregivers that introduced complementary feeding earlier than six months were among caregivers that participated in this study. Whether they introduced complementary feeding earlier or at appropriate time there was a significant improvement in the feeding practices among the caregivers that received nutrition education (Figure 3 & 4).
Force feeding ways of introducing complementary feeding among the caregivers in the control group showed poor feeding practices of the caregivers. There was lack of knowledge on responsive feeding which made the caregivers in the control group lack confidence to feed the infants. This resulted to force feeding as determined in this study, which could affect the timely introduction of the complementary feeding practices. Majority of the caregivers in the control group started force feeding due to the refusal of the complementary foods by the infants. The issue of early intolerance of the complementary foods by the infants was handled during the nutrition education using different techniques of responsive feeding through posters and food demonstrations. This study is in line with guiding principle of complementary feeding stated by the National Policy on infant and young child feeding in Nigeria [19], which declared that responsive feeding using psycho-social care should be adopted by mothers in Nigeria. To foster a reciprocal relationship between the parent or caregiver and the child, and thus practicing responsive feeding, was hypothesized to be beneficial to both parties [20]. Accelerated rate of death and pneumonia as a result of force feeding was a concern [21]. They further stated that force feeding leads to infections, collapsed lungs, digestive and pancreatic problems. Acceptable ways of introducing complementary feeding that will be acceptable by the infants and will not frustrate the effort of the caregivers which could lead to introduction of force feeding, was learnt by the caregivers in the intervention group during the nutrition education on complementary feeding. Lack of responsive feeding practices caused growth flattering among the infants in low- and middle-income countries [22].
Therefore, responsive feeding techniques should be among the package for complementary feeding guidelines. To corroborate the effectiveness of nutrition education on responsive feeding, it was revealed that there was an improvement in the complementary feeding practices of caregivers in the intervention group as the caregivers in Kosova were able to see more reasons to have patience and encourage the infants to eat complementary foods [23]. Consumption of iron rich foods was high among the infants in both groups and this agrees with the reports on consumption of iron rich foods in South-West Nigeria by [19]. The report revealed that 60.1% of infants in this geo-political zone consumed iron rich foods. Despite the high rate of consumption of iron rich foods in both groups, there was a wide margin of iron rich foods intake between the infants in the intervention group and control group in the present study. Increase in the intake of iron rich foods was due to the nutrition education that the caregivers in the intervention group received. Intakes of iron were lower by 16% among infants of 6-12 months than children of 13-36 months in an observational study in Brazilian Well Child Clinic [24]. There was an association between complementary foods and haemoglobin concentration among Indian infants [25]. The author stated that there was a positive association between the infants’ haemoglobin concentration and fortified baby foods, breast milk and infant formula as well as fruits and vegetables to a lesser extent on the contrary to porridge or gruel. Iron deficiency [ID] is the most common micronutrient deficiency world-wide and young children are the special risk group because their rapid growth leads to high iron requirements [26].
Early initiation of complementary food using semi-solid, solid/ soft food consistency and food diversification was improved among the caregivers in the intervention group. The knowledge acquired during the nutrition education was put into practice during the period of complementary feeding before the first birthday of the infants [age 12 months]. It was recommended that nutrition education is needed in West African countries to improve the knowledge of caregivers on complementary foods consistency as majority of mothers in West African countries feed the infants with thin gruel during complementary feeding [27]. Poor timing of initiation of complementary feeding led to 70% malnutrition among infants in Konaseema region of India therefore recommended nutrition intervention on complementary feeding [28]. Untimely initiation of complementary feeding was prevalent among caregivers in North eastern part of Ethiopia and that nutrition education on timely introduction of complementary feeding could improve the practices among mothers [29]. The infants in the intervention group had higher minimum meal frequency rates than the infants in the control group. This was similar to the findings which revealed that meal frequency increased according to the age of children study in South eastern of Ethiopia [30]. The increase in the percentage of the infants who were fed with minimum meal frequency was higher in the intervention group than the control group due to the effect of the nutrition education on the intervention group. This is in line with the findings which showed that there was an increase in meal frequency of infants whose mothers were in intervention group than the infants whose mothers were in the control group in Ethiopia [31]. The intervention group caregivers increased the meal frequency during illness of the infants during the study compared to the caregivers in the control group. Children poor appetite induced by illness can contribute to perpetuate vicious cycle of infectious diseases [32].
Dietary diversity during complementary feeding was achieved among the caregivers in the intervention earlier at midline of the study than the caregivers in the control group. The effect of the knowledge of the caregivers in the intervention group was noticeable in the minimum dietary diversity achieved during the feeding practices. There was higher number of infants who were fed on minimum dietary diversity in the intervention group than the control group. This study was in line with the study which showed significant difference between dietary diversity, meal frequency and feeding infants with iron containing foods among caregivers the intervention group and those in the control group in Uganda [33]. However, literature on intervention to improve the feeding practices of caregivers prior the commencement of the complementary feeding practices, and at different age of the infants’ months was limited. Nutrition education improved dietary diversity among caregivers of infants between 6-23 months in Malawi [34]. Also, UNICEF showed that nutrition education is a catalyst for improving dietary diversity among caregivers in Lilongwe, Malawi [35]. Treatment of drinking water by the caregivers showed that the caregivers in the intervention group practiced good hygiene as compared to the caregivers in the control group. This could be the effect of the nutrition education received by the intervention group. The underlying determinants of undernutrition include food insecurity, inappropriate care practices, poor access to health care, and an unhealthy environment, including access to portable water, sanitation, and hygiene [36] in [37]. In 2018 UNICEF declared that 88% of diarrhea deaths were due to lack of access to safe drinking water, poor sanitation and hygiene [38]. World Health Organization stated that nutrition outcome could be improved with better intervention on water, sanitation and hygiene [39].
The improvement in complementary feeding practices in the intervention group could be linked to the knowledge acquired during nutrition education. The intended feeding practices as noted at the baseline study as well as during FGDs and KIIs was to feed the infants with thin consistency. However, nutrition education was able to change the understanding of the caregivers on food consistency which in turn improved the feeding practices among the caregivers in the intervention group. Several studies have proved the need for nutrition education to improve complementary feeding practices of caregivers. Nutrition education was recommended as a viable tool to improve complementary feeding practices among mothers in Cross River State, Nigeria [18]. Nutrition education on complementary feeding is needed by caregivers in Sagamu, Nigeria to improve the infant feeding practices among mothers [40]. It was 30% of infants in Nigeria were adequately fed and therefore recommended nutrition education for the improvement of caregivers feeding practices [41].
References
- Unicef (2017) State of the world’s children 2017. Children in a digital world. pp. 146-177.
- National Population Commission and ICF International (NDHS, 2014) Nigeria Demographic and Health Survey (NDHS). NPC and ICF International, Nigeria
- UNICEF (2014) Report on The Nutrition and Health Situation of Nigeria. Data Collection - 9th February - 15th May Nutrition and Health Survey Using SMART Methods doi: 10.1186/s13006-015-0033-x
- United Nations Children Fund (2010) The World’s women, trend, and statistics. New York.
- United Nations Children’s Fund (2012) Infant and young child feeding programming Status Results of 2010-2011 assessment of key actions for comprehensive infant and young child feeding programmes in 65 countries. UNICEF, New York
- Nabugoomu, J, Namuteb A, Kaaya A.N, Nansinyama G (2015) Nutrition education influences child feeding knowledge, attitudes and practices of caregivers in Uganda. American Journal of Health Research 3(2): 82-90.
- Ndu IK, Ekwochi, U, Osuorah CD I, Chinawa J, Asinobi I Eze, et al (2016) The Knowledge and Practice of Forced-Feeding among Mothers and Caregivers in Enugu, South East Nigeria. IJTDH 11(3): 1-7.
- Arnold BF, Null C, Lubby S.P, Unicom L and Stewart C.P et al (2013). Infectious diseases cluster-randomised controlled trials of individual and combined water, sanitation, hygiene and nutritional interventions in rural Bangladesh and Kenya: the WASH Benefits study design and rationale. BMJ Open 3(8).
- Kulwa KBM, Verstraeten R, Bouckaert K, Mamiro P, Kolsteren P, et al (2014). Effectiveness of a nutrition education package in improving feeding practices, dietary adequacy and growth of infants and young children in rural Tanzania: rationale, design and methods of a cluster randomized trial. BMC Public Health 14:1077.
- Chan YH (2003) Randomised controlled trials (RCTs)-sample size: The magic number. Singapore Med J 44(4): 172-174.
- Bolajoko OO, Ogundahunsi GA (2012). The effect of childcare and feeding practices on the nutritional status of children of market women in Ondo State, Nigeria. IOSR Journal of Pharmacy and Biological Sciences 1(2): 22-24.
- World Health Assembly, Geneva World Health Organization (2004) Complementary feeding counseling a training course; trainers guide.
- WHO (2010) Indicators for assessing infant and young child feeding practices - Part3: Country profiles. Geneva, Switzerland: World Health Organization.
- WHO/FAO (2010) Infants and young child feeding practices
- Mukaka MM (2012) A guide to appropriate use of correlation coefficient in medical research. Malawi Med. J 24 (3): 69-71.
- Kennedy G, Ballard T, MarieClaude Dop MC (2011). Guidelines for Measuring Household and Individual Dietary Diversity. Nutrition and Consumer Protection Division, Food and Agriculture Organization of the United Nations.
- Olatona FA, Odozi MA, Amu EO (2014) Complementary feeding practices among mothers of children under five years of age in Satellite Town, Lagos, Nigeria. Food and Public Health 4(3): 93-98.
- Udoh EE, Amodu OK (2016) Complementary feeding practices among mothers and nutritional status of infants in Akpabuyo area, Cross River State Nigeria. Springer Plus 5(1): 2073.
- NNHS (2014) National Bureau of Statistics: Summary findings of National Nutrition and Health Survey using SMART Methods.
- (2010) National Policy on Infant and Young Child Feeding in Nigeria.
- Harbron J, Booley S, Najaar B (2013) Responsive feeding: establishing healthy eating behaviour early on in life. S Afr J Clin Nutr 26(3): 141-149.
- Magorzata, Smulczyk (2011) Handbook of behavior, food and nutrition. 1603-1618.
- Bentley ME, Waseer HM, Creed Kanashiro H.M (2011) Responsive Feeding and Child Undernutrition in Low- and Middle-Income Countries: J. Nutr 141 (3): 502-507.
- Berisha M, Ramadani N, Hoxha R, Gashi S, Zhjeqi V, et al (2017) Knowledge, Attitudes and Practices of Mothers in Kosova About Complementary Feeding for Infant and Children 6-24 Months. Med Arch 71(1): 37-41.
- Faleiros FTV, da Silva NV, Carvalho Mde Assis, Machado NC (2016) Intake, bioavailability, and absorption of iron in infants aged 6 to 36 months: an observational study in a Brazilian Well Child Clinic Nutrire 41:10.
- Prieto Patron A, Hutton ZV, Garg P, Rao S, Eldridge AL, et al (2017) The Association between Complementary Foods and Hemoglobin Concentrations in Indian Infants. J Hum Nutr Food Sci 5(1): 1105.
- Domellof M, Braegger C, Campoy C, et al (2014) ESPGHAN Committee on Nutrition. Ironrequirements of infants and toddlers.J Pediatr Gastroenterol Nutr 58: 119-129.
- Akinsola A.O, Onanbanjo O.O, Idowu M.A and Ade-Omowaye B.I.O (2017) Traditional Complementary Foods: A Critical Review. Greener Journal of Agric Science. 7(8): 226-242.
- Sethi R, K Padhy S, Raju DVSLN (2017) Knowledge, attitude and practices regarding complementary feeding among mothers of children 6 to 24 months of age in Konaseema region. International Journal of Contemporary Pediatrics Int J Contemp Pediatr 4(2): 394-398
- Manikyamba D, Vidya DL, Satyavani A, Prasad AK, Deepthi T (2015) Impact of Nutritional Education on the Knowledge of others Regarding Infant and Young Child Feeding Practices Scholars Journal of Applied Medical Sciences (SJAMS): Sch J App Med Sci 3(3A): 1074-1078.
- Tegegne M, Sileshi S, Benti T, Teshome M, Woldie H (2017) Factors associated with minimal meal frequency and dietary diversity practices among infants and young children in the predominantly agrarian society of Bale zone, Southeast Ethiopia: a community based cross-sectional study. Archives of Public Health, 75: 53.
- Mulualem D, Henry CJ, Berhanu G, Whiting SJ (2016) The effectiveness of nutrition education: Applying the Health Belief Model in child-feeding practices to use pulses for complementary feeding in Southern Ethiopia. Journal of Ecology of Food and Nutrition 55(3): 308-323.
- Paintal K, Aguayo VM (2016) Feeding practices for infants and young children during and after common illness. Evidence from South Asia. Maternal Child Nutr 12 (Suppl 1): 39-71.
- Ickles SB, Baguma C, Brahe CA, Myhre JA, Adair LS, et al. (2017) Maternal participation in a nutrition education program in Uganda is associated with improved infant and young child feeding practices and feeding knowledge: a post-program comparison study. BMC Nutrition 3: 32.
- Kuchenbecker J, Reinbott A, Mtimuni B, Krawinkel MB, Jordan I (2017) Nutrition education improves dietary diversity of children 6-23 months at community-level: Results from a cluster randomized controlled trial in Malawi. PLOS 12(4): e0175216.
- UNICEF (2015) Participatory nutrition education catalyst for dietary diversity, Lilongwe, Malawi
- United Nations Children's Fund (1990): Strategies for improving nutrition of children and women in developing countries. New York, NY: United Nations Children's Fund
- Dodos J, Mattern B, Lapegue J, Altmam M, Ait Aissa, M (2017): Relationship between water, Sanitation, Hygiene and Nutrition: what do link NCA nutrition causal analysis say?
- UNICEF (2018) Health, Nutrition, HIV and Aids: Improved learning through better Health, Nutrition and Education for the school age child.
- WHO (2015) Improving outcomes with better water, Sanitation and Hygiene; Practical solution for policies and programmes.
- Sholeye O.O., Akinpelu,A., Bankole, E. and Diya, O. (2016): Knowledge of infant feeding among mothers in sagamu, southwestern ;Nigeria; implications for nutrition education. Amer J Food Nutr 6(3): 69-76.
- Olatona, F.A., Adenihun, O. J., Aderibigbe, S.A. and Adeniyi, O.F. (2017): Complementary Feeding Knowledge, Practices, and Dietary Diversity among Mothers of Under-Five Children in an Urban Community in Lagos State, Nigeria. International Journal of MCH and AIDS 6(1): 46-59.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...