Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-6070
Research Article(ISSN: 2638-6070) 
Body Mass Index of Kaani Tribes from Kanyakumari District in Tamil Nadu, India
Volume 1 - Issue 1Jemima Beryl Mohankumar* and M Velvizhi
- Department of Nutrition & Dietetics, PSG College of Arts & Science, Coimbatore, India
Received: April 03, 2018; Published: April 11, 2018
*Corresponding author: Jemima Beryl Mohankumar, Department of Nutrition & Dietetics, PSG College of Arts & Science, Coimbatore, India
DOI: 10.32474/SJFN.2018.01.000101
Abstract
BMI provides the most useful population-level measure of overweight and obesity as it is the same for both sexes and for all ages of adults. However, it should be considered a rough guide because it may not correspond to the same degree of fatness in different individuals. There is a difference in BMI values for the Asians as compared to the WHO criteria. Our study focused on the BMI of the Kaani tribes in Kanyakumari District of Tamil Nadu, India. We categorized them as two groups, viz. those who lived in the forest area and those who had moved out of the forest into neighbouring villages. We found that among the forest dwellers there was a greater percentage in the underweight category, indicating energy deficiency, while those in the rural areas were moving to a greater BMI. This is of concern as the sequel of thinness and overweight represent major public health problems.
Keywords: BMI, Kaani tribes, Public health, Lifestyle, Chronic energy deficiency, Obesity
Abbreviations: BMI: Body Mass Index, WHO: World Health Organization, CED: Chronic Energy Deficiency
Introduction
Body mass index is considered as an index for assessing the nutritional status. The 1993 WHO Expert Committee WHO [1] reported that weight gain in adult life was associated with increased morbidity and mortality at higher BMI range. Therefore, BMI cutoff for overweight should be interpreted based on risk factors of morbidity and mortality. Smalley et al. [2] reported that type 2 diabetes mellitus, cardiovascular disease and increased mortality are the most important sequels of obesity and abdominal fatness, but other associations like musculoskeletal disorders, limitations of respiratory function and reduced physical functioning and quality of life were also observed.
Methodology
The study area Kanyakumari is located in Tamil Nadu in South India, about 700 Kms. from Chennai the capital city of Tamil Nadu. The nearest major city is Trivandrum in the neighbouring state of Kerala. Kerala border is very near to Kanyakumari, which is why a mixed culture of Kerala and Tamil Nadu is seen in the area. A crosssectional study was carried out as it provides a clear ‘snapshot’ of the outcome and the characteristics associated with it, at a specific point in time. The investigator collected quantitative data; the Auxiliary Nurse Midwife accompanied her from the Primary Health Centre to establish a rapport with the local leaders and Kaani heads. Anthropometric measurements were collected using standard instruments and protocol. Measurements were recorded for adult’s males and females in the age group of 25 to 55 years from the forest and rural areas. The sample size was calculated based on the 2011 census population size of Kaanis in Kanyakumari district.
Result and Discussion
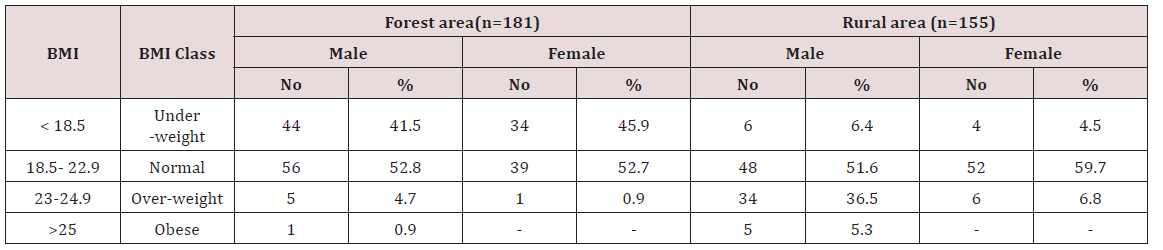
A BMI< 18.5 kg/m² is widely used as a practical measure of chronic energy or hunger deficiency (CED), i.e., a “steady” underweight in which an individual is in energy balance irrespective of a loss in body weight or body energy stores Khongsdier [3]. Thus, the use of BMI as an anthropometric indicator of nutritional status can be more appropriate in a country with diverse ethnic groups, such as India Khongsdier [4] (Table 1). Majority of the male and female in forest area (52.8 % and 52.7%) and in rural area (51.65% and 59.7%) belonged to normal weight with a BMI of 18.5 - 22.9, followed by (45.9%) percent of the female in forest areas being underweight with a BMI of < 18.5. Alarmingly about 41.5 percent of the male in forest area were underweight with a BMI of < 18.5. 5.3 percent of male in rural were obese. Body mass index is used as an index to assess the extent of chronic energy deficiency (CEO) in adults. In adult males, the mean BMI was 20.38kg/m2, 19.53kg/m2, 20.25kg/m2 for the age groups 30-35 years, 36-55 years and above 55 years respectively.
Adult under nutrition very simply happens, due to hunger and lack of food. Body Mass Index (BMI) can measure adult malnutrition and a BMI below 18.5 indicates chronic under nutrition. Statistics have shown how 37% of adult Indians, 50% of adults belonging to the Scheduled Tribes and 60% of adult Indians belonging to the Scheduled Castes have a BMI below 18.5, which makes them chronically undernourished. The overall CED was highest in Madhya Pradesh (76.0%) followed by Maharastra (71.9%), Jharkhand (58.5%), Tamil Nadu (55.0%), Andhra Pradesh (50.1%), Odisha (49.5%), West Bengal (45.9%), Kerala (37.8%), Andaman & Nicobar Island (29.5%), Assam (21.5%), while Meghalaya shows the least (14.3%) prevalence of under nutrition among the tribes in all the studied states of India Das and Bose [5] . Asian Indians have a characteristic obesity phenotype, consisting of relatively lower BMI, excess body fat percentage, abdominal and truncal adiposity and less lean tissue Banerji et al. [6]; Dudeja et al. [7]. WHO [8] Expert Consultation proposed a new BMI cut-off of 23.0 kg/m2 for public health action in Asia. There has been limited data on the anthropometric and nutritional status of various tribal populations of India Bose et al. [9] to plan intervention strategies.
Conclusion
Many researchers report the relationship between BMI and diabetes mellitus. Misra and Vikram [10] reported that 67% diabetics were found as either over weight (or) obese subjects. We have found that under-weight is predominant in the Kaanis of the forest area, while those who have moved to rural areas outside the forest have a greater percentage who are over-weight. We would like to conclude that life-style in the forest is not conducive to maintaining healthy body weight; while those who have moved out of the forest are heading towards problems of over-weight. One is a consequence of insufficient food intake, the other is leading to overnutrition and consequently to lifestyle diseases in the future.
References
- WHO World Health Organization (1995) Physical status: the use and interpretation of anthropometry- Report of a WHO expert committee. WHO Technical Report Series 854 Geneva.
- Smalley KJ, Knerr AN, Kendrick ZV, Colliver JA, Owen OE (1990) Reassessment of body mass indices. Am J Clin Nutr 52(3): 405-408.
- Das S, Kaushik Bose K (2012) Nutritional deprivation among Indian, Anthropological Notebooks 18(2): 5-16.
- Khongsdier Romendra (2001) Body mass index of adult males in 12 populations of Northeast India. Annals of Human Biology 28(4): 374- 383.
- Das S, Kaushik Bose K (2012) Nutritional deprivation among Indian, Anthropological Notebooks 18(2): 5-16.
- Banerji MA, Faridi N, Atluri R, Chaiken RL, Lebovitz HE (1999) Body composition, visceral fat, leptin and insulin resistance in Asian Indian men. J Clin Endocrin Metab 84(1): 137-144.
- Dudeja V, Mishra A, Pandey RM, Devina G, Kumar G, et al. (2001) BMI does not accurately predict overweight in Asian Indians in northern India. Br J Nutr 86(1): 105-112.
- WHO Expert Consultation (2004) Appropriate body mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363(9403): 157-163.
- Bose Kaushik, Falguni Chakraborty, Samiran Bisai, Argina Khatun, Hironmoy Bauri (2006) Body mass index and nutritional status of adult Savar tribals of Keonjhar District, Orissa, India. Asia Pacific Journal of Public Health 18(3): 3-7.
- Misra A, Vikram NK (2004) Insulin resistance syndrome (metabolic syndrome) and obesity in Asian Indians: Evidence and implications. Nutrition 20(5): 482-491.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...