Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2690-5760
Case report(ISSN: 2690-5760) 
Importance of the Dynamic in Head and Neck Trauma: A Case Report and Review of Literature Volume 2 - Issue 4
Collura Simone* and Andreoli Giovanni
- Department of Molecular and Translational Medicine, University of Brescia, Italy
Received: November 09, 2020 Published: December 13, 2020
Corresponding author: Collura Simone, Department of Molecular and Translational Medicine, University of Brescia, Italy
DOI: 10.32474/JCCM.2020.02.000143
Abstract
Introduction: The dynamic is one of the most important aspect to evaluate in a trauma even if the first clinical findings are poor. Sometimes it can be the most relevant aspect.
Case report: Here we report a case of a 73 year-old woman who was invested by a car running about 30 km/h. The patient was projected a few meters away. There were contusions of the right hemithorax, the left leg and particularly of the right orbital region with hyperextension of the neck. The CT scan revealed fracture of the orbital and maxillary bones on the right side with frontal acute subarachnoid hemorrhage. There were also fractures of the posterior arch of C1 and a complex fracture of C2 without any neurological sign. The patient was then recovered in our hospital and underwent fixation of the first three cervical vertebrae three days after. Ten days after surgery the patient was discharged in good health with perfect neurological exam.
Discussion: The evaluation of the dynamic is really important in every trauma. Even where the clinical findings are poor, careful attention must be taken to dynamic like in our case. Particular dynamic features of the trauma can give indication to CT scan of the head and neck. Some clinical scales can be significant and very useful when evaluating the risk of cervical vertebral lesions with eventual indication to radiological exams.
Conclusion: When evaluating a trauma, attention to dynamic is strictly important. The physician must keep in mind appropriate and validated criteria for evaluation of the trauma in order to choose as soon as possible the best clinical process for the patient.
Introduction
The management of trauma has evolved significantly in the last
past decades [1]. In its improvement a main role has been played
by the introduction of validated criteria to evaluate the trauma in
its clinical and dynamic aspects.
Dynamic of trauma is relevant and it is more significant in the
first evaluation when the clinical findings can be poor.
Case report
We report a case of a 73 year-old female patient affected by
hypertension and diabetes type II both in oral and insulin therapy.
The patient was taking aspirin for preventive purposes. While
crossing a street during the evening the patient was invested by
a car running 30 km/h. The patient was projected about three
meters away with trauma of the right hemithorax, the left leg and
particularly of the right orbital region with hyperextension of the
neck.
The patient was always conscious and was brought to our
Emergency Department. At the first evaluation the patient was
hemodynamically stable with normal values of heart rate, blood
pressure and respiratory rate. GCS was 15. The only clinical
important sign was a right raccoon eye.
The radiological exams of thorax and abdomen were negative.
In particular the patient underwent at first a radiography of the
chest and in a second time a CT scan of thorax and abdomen. The
radiological exams of the extremities found only a fracture of left
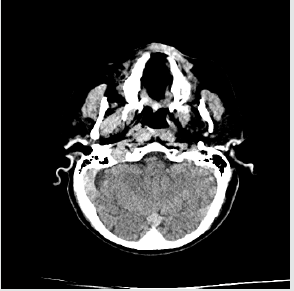
fibula. Indeed the CT scan of the head found a complex fracture of
the orbital and maxillary bones on the right side with a right frontal
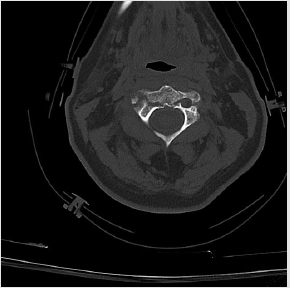
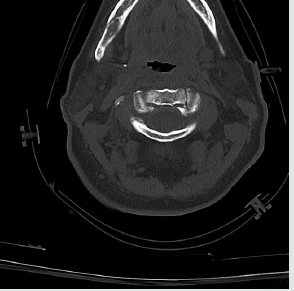
acute subarachnoid hemorrhage of about 1 cm in size.The CT scan of the cervical column demonstrated a fracture of the posterior
arch of the first cervical vertebra and a complex fracture of the
second one. There were no particular findings at the blood exams.
The patient was also evaluated by the anesthesiologist with no
indication for recovery in the Intensive Care Unit.
Then the patient was recovered in the Unit of Neurosurgery
and three days later she underwent the fixation of the first three
cervical vertebrae. During surgery also a ganglionectomy of C2
was performed. No significant surgical blood loss was recorded
and the general anesthesia was well tolerated by the patient. After
surgery the patient was recovered for a day in the Intensive Care
Unit and then she came back to the Neurosurgical Unit. In the postoperative
period hypernatremia was found, successfully treated
with parenteral infusions. Ten days after surgery the patient was
discharged in good health with a perfect neurological exam.
Two months after hospital discharge the patient underwent a
CT scan of head and neck which demonstrated a normal healing
of the previous lesions. At two years after the traumatic event the
patient is in good health with no neurological sequelae. Nowadays
the patient is able to attend to all her daily activities such as before
the trauma.
Discussion
Age is a risk factor for trauma [1]. About 30% of minor traumas
of the elderly are at risk for major lesions. Road accidents [2,3]
are one of the most relevant traumatic cause of death between 65
and 74 years old and the second one over 75 years. In the elderly
the pedestrian investment is one of the most common situation
especially for women.
So this kind of trauma is really important for community both
because of health problems and costs for society. The dynamic of
trauma is very significant in the evaluation of the possible lesions.
Even when the clinical findings are poor, an accurate anamnesis
with particular reference to the features of the accident scene is
really important. Features of major trauma are rolling by a vehicle,
ejection from a vehicle, precipitation from a height more than 3
meters, presence of a dead in the same vehicle, investment of a
pedestrian by a car or a truck especially if with projection.
In our case the dynamic can be considered important both
because the patient was a pedestrian hit by car and there was
projection. Even the velocity of the vehicle was significant in this
kind of dynamic. In the evaluation of head trauma the first thing
to assess is the Glasgow Coma Scale: if normal (15) the indication
to CT scan is to be taken according to the features of patient such
as age, anticoagulant or antiplatelet therapy. Otherwise with GCS
inferior to 15 CT is mandatory. There are some cases in which
assumption of alcohol or drugs [4] can make difficult the evaluation
of GCS and so in such cases CT is also recommended.
Other factors [1] leading to the choice of performing a CT scan [5-9] of the head are: presence of retrograde amnesia lasting more than 30 minutes, age> 65 years old, more than two episodes of vomit, assumption of anticoagulant or anti platelet therapy, suspect signs of skull fractures such as hemo tympanum, raccoon eyes and Battle’s sign, relevant dynamic such as described before, disorientation after trauma (Figures 1-4).
In our case GCS at the arrival to the Emergency Department
was 15 and the indication to the CT scan [5] was taken particularly
because of the dynamic of the event, in taking of aspirin, age and
presence of raccoon eye. In the evaluation of neck trauma [10-
13] the first thing to evaluate are the presence of cervical pain,
contracture and tenderness. In our case no particular pain or
contracture was found during the first clinical evaluation and the
neurological exam was normal. Only the dynamic of the trauma and
the coexistence of the head trauma with hyperextension of the neck
suggested radiological exams of the cervical column.
Usually the importance of neck trauma and consequently
the indication to radiological exams are established trough some
clinical scales such as Canadian C-spine rules and Nexus criteria.
According to Canadian C-spine rules [10,11, 13] age > 65 years
old and presence of a dangerous mechanism (fall from 5 stairs,
axial load to the head, high-speed motor vehicle collision, rollover,
ejection,…) such as in our case are indications to radiological study
of the cervical spine. On the other side Nexus [11] criteria are not
reliable with elderly patients, such as in the present case. A good
knowledge of the dynamic event and of the criteria and scales
here cited are very useful for a prompt and correct management
of trauma.
Conclusion
It’s really important to know every aspect of the dynamic of the event in the management of trauma. Validated scales and criteria are really useful to identify major traumas even if the first clinical findings are poor. The correct knowledge of these criteria can guarantee a prompt and perfect management of the traumatic patient. The head trauma in the elderly is a frequent problem in community everyday life and this makes the correct management of this kind of trauma even more relevant.
References
- Osvaldo G, Gordini G, Nardi G, Sanson G (2012) Trauma care. Elsevier.
- Liu G, Chen S, Zeng Z, Cui H, Fang Y, et al. (2018) Risk factors for extremely serious road accidents: Results from national Road Accident Statistical Annual Report of China. PLoS One 13(8): e0201587.
- Iaccarino C, Carretta A, Nicolosi F, Morselli C (2018) Epidemiology of severe traumatic brain injury. J Neurosurg Sci 62(5): 535-541.
- Carfora A, Campobasso CP, Cassandro P, Petrella R, Borriello R (2018) Alcohol and drugs use among drivers injured in road accidents in Campania (Italy): A 8-years retrospective analysis. Forensic Sci Int 288: 291-296.
- Kuo KW, Bacek LM, Taylor AR (2018) Head Trauma. Vet Clin North Am Small Anim Pract 48(1): 111-128.
- Bonhomme V, Hans P, Brichant JF (2006) Head trauma. Acta Anaesthesiol Belg 57(3): 239-247.
- Gioffrè-Florio M, Murabito LM, Visalli C, Pergolizzi FP, Famà F (2018) Trauma in elderly patients: a study of prevalence, comorbidities and gender differences. G Chir 39(1): 35-40.
- Peeters N, Lemkens P, Leach R, Gemels B, Schepers S, et al. (2016) Facial trauma. B-ENT 26(2): 1-18.
- Perry M, Morris C (2008) Advanced trauma life support (ATLS) and facial trauma: Can one size fit all? Part 2: ATLS, maxillofacial injuries and airway management dilemmas. Int J Oral Maxillofac Surg 37(4): 309-320.
- Michaleff ZA, Maher CG, Verhagen AP, Rebbeck T, Lin CW (2012) Accuracy of the Canadian C-spine rule and NEXUS to screen for clinically important cervical spine injury in patients following blunt trauma: A systematic review. CMAJ 184(16): E867-876.
- Stiell IG, Clement CM, McKnight RD, Brison R, Schull MJ, et al. (2003) The Canadian C-spine rule versus the NEXUS low-risk criteria in patients with trauma. N Engl J Med 349(26): 2510-2518.
- Kanwar R, Delasobera BE, Hudson K, Frohna W (2015) Emergency department evaluation and treatment of cervical spine injuries. Emerg Med Clin North Am 33(2): 241-282.
- Ngatchou W, Beirnaert J, Lemogoum D, Bouland C, Youatou P, et al. (2018) Application of the Canadian C-Spine rule and nexus low criteria and results of cervical spine radiography in emergency condition. Pan Afr Med J 30: 157.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...