
Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-6003
Mini Review(ISSN: 2638-6003) 
Bone Marrow Edema and Joint Overuse in Athletes: a Mini-Review Volume 4 - Issue 2
Calvin L. Cole1,2, Kostantinos Vasalos1,2, Gregg Nicandri1,2, Cameron Apt1,2, Emmalyn Osterling1,2, Zachary Ferrara1,2 Michael D Maloney1,2, Edward M Schwarz1,2 and Katherine Rizzone1,2*
- 1Center for Musculoskeletal Research, University of Rochester Medical Center, USA
- 2Department of Orthopedics and Rehabilitation, University of Rochester Medical Center, USA
Received: June 16, 2020; Published: July 10, 2020
Corresponding author: Katherine Rizzone, Center for Musculoskeletal Research, University of Rochester Medical Center, USA
DOI: 10.32474/OSMOAJ.2020.04.000184
Abstract
A marginal number of adolescents meet the recommended guidelines of 60 minutes of moderate to vigorous daily physical
activity, and even fewer underrepresented minority females achieve this metric as compared to their male and white counterparts.
While potential interventions exist to address these low levels of activity, which is a known risk for acute injuries and chronic
disease, there is lack of consensus on the devices used to measure the intensity of daily activity levels. Wearable activity trackers
such as FitbitTM have been utilized to quantify human motion and exercise intensity, but there is little precedence for these measures
being assessed in adolescent wearers. Thus, our objective was to assess the feasibility of using Fitbit to assess daily physical activity
levels in underrepresented minority adolescent females, who attend an economically challenged urban high school, over the course
of a physical activity intervention. We also aimed to identify candidate Fitbit outcome measures for future prospective studies.
A 10-week physical activity intervention was implemented in a cohort of 24 high school female athletes. From within this
cohort, a sample of five students was provided FitbitTM devices, from which we obtained data sets from three students. Activity on
the days of the exercise intervention was measured and compared to activity on non-intervention days. Post-hoc assessments were
performed based on individual heart rate reserves, the predefined levels set by the Inspire FitbitTM device and the American College
of Sports Medicine (ACSM) 2009 guidelines.
The results showed that while compliance is challenging, wearable devices can be used to assess daily physical activity levels
and intensities in underrepresented minority high school female athletes during an extended physical activity intervention. Of the
Fitbit outcomes currently available, assessment of moderate-vigorous activity (min/day) appeared to be the best as a measure of
global physical activity. Prospective research is now warranted to validate these thresholds, and to test novel interventions for their
ability to transition inactive adolescents at risk of sports-related injuries and long-term chronic disease, into a more active lifestyle.
Keywords: Fitbit; Physical Activity Recommendations; Physical Activity Intensity Levels
Introduction
The recommended physical activity guidelines for adolescents are 60 daily minutes of moderate to vigorous activity with at least three days a week involving vigorous activity [1]. Moderate physical activity examples include bike riding, brisk walking and dancing; examples of vigorous level activities include running, martial arts and active games like tag [1]. According to NHANES data, only 20% of young adults and adolescents meet this requirement, which is worrisome in light of the United States’ obesity epidemic [2]. Even more concerning is that a large gender and racial disparity exists within these numbers [3-7]. Females, particularly those of underrepresented racial minorities, most often do not meet these recommended levels in comparison to their male and white counterparts [5,8]. This activity gap has short-term effects, with lower activity adolescents being observed to have a higher incidence of obesity and glucose intolerance during their adolescent years, in addition to long-term effects such as increased risk for development of cardiovascular disease and associated co-morbidities such as hypertension and diabetes, all of which decrease life expectancy [9-11]. An opportune time to intercede and decrease prevalence of these diagnoses, which greatly shortens lifespans and negatively impacts quality of life, may be during the formative, teenager years [12,13]
Until recently, the gold standard for daily objective physical
activity assessment was accelerometers [14]. While there is a
plethora of supportive evidence on the validity of these devices,
drawbacks and limitations also exist [15]. Their utility, which has
been demonstrated within the lab setting, is not always able to be
replicated pragmatically in real life settings [16]. Although these
devices have continued to diminish in size, they are relatively
larger on children, leading to discomfort. They also require specific
instructions in location of placement on the body, which needs to
be consistent throughout the intervention [17-18]. Accelerometers
can be expensive, limiting the ability of researchers to be able to
study large populations [15,16]. Additionally, they may be viewed
as a research implement and therefore less likely to be utilized
by participants as designed in the study methodology [19,20]
More recently, fitness monitors have introduced an alternative
technological method to objectively quantifying activity levels.
These devices offer multiple benefits over accelerometers.
They can be less expensive; they are often easier to position, are
lightweight and are accepted in mainstream culture as wearables.
This may increase the probability that they are more consistently
worn which then leads to increased quantity and improved quality
and reliability of the collection of the data they generate as previous
data has shown their validity for physical activity studies [14-23].
Recently, we developed and implemented a 10 week athletic
performance and injury prevention program for adolescent high
school students, and demonstrated the use of Patient-Reported
Outcomes Measurement Information System (PROMIS) and
Functional Movement System (FMS) outcomes [24]. To expand on
this, we aimed to assess daily activity levels during a similar 10 week
study in underrepresented minority female athletes monitored via
FitbitTM wearable technology. Our hypothesis was that the wearable
devices would be able to distinguish thresholds between low,
moderate and vigorous activity among student participants. Longterm,
these thresholds could be validated for utilization in future
prospective studies.
Materials and Methods
This was a prospective cohort study of adolescent athletes
enrolled in an athletic performance and injury prevention program.
The pilot was administered in an urban high school setting
during a 10-week program led by co-investigators in fall 2019.
Study participants were led through a three day a week exercise
intervention that targeted all major muscle groups [24]. Out of
the cohort’s 24 participants, a sample of five was given a FitbitTM
(Inspire HR, United States, San Francisco, CA). Study participants
were instructed by the research staff in use of the device and also to
wear their assigned FitbitTM device all day, removing only to bathe
or charge the device. Wear age and device charge capacity was
checked during the thrice weekly intervention sessions. All human
subject research was performed following informed consent
from a legal guardian and assent from the study subjects, on an
Institutional Review Board approved protocol. A data agreement
was made with the company for data access. Data was uploaded to
the FitbitTM database multiple times a day and then participant data
was downloaded to an approved, secure University of Rochester
database every 24 hours.
Our primary goals were to demonstrate the ability to
consistently track physical activity levels via the FitbitTM monitoring
system in this pilot feasibility study. Daily FitbitTM output obtained
included minutes of activity, resting heartrate (HR) and heartrate
during activities. Maximum heartrate and heart rate reserve (HRR)
were calculated using participants’ age and resting heartrate.
The American College of Sports Medicine (ACSM) categorizes
physical intensity levels into distinct groups [25, 26]. These levels
are determined from the calculated maximum heart rate and
resting heart rate of individuals’. The levels assigned for heart rate
data were predetermined by FitbitTM, and so we retrospectively
determined which ACSM intensity levels those categories best fit
(Table 1).
Table 1: Physical activity intensity categories of the FitbitTM Inspire, study participants and the American College of Sports Medicine 2009 Guidelines.

The minutes assigned to each activity intensity group were calculated by the FitbitTM device. Days on which the device was detected as being worn less than 12 hours a day were excluded from analyses.
Results
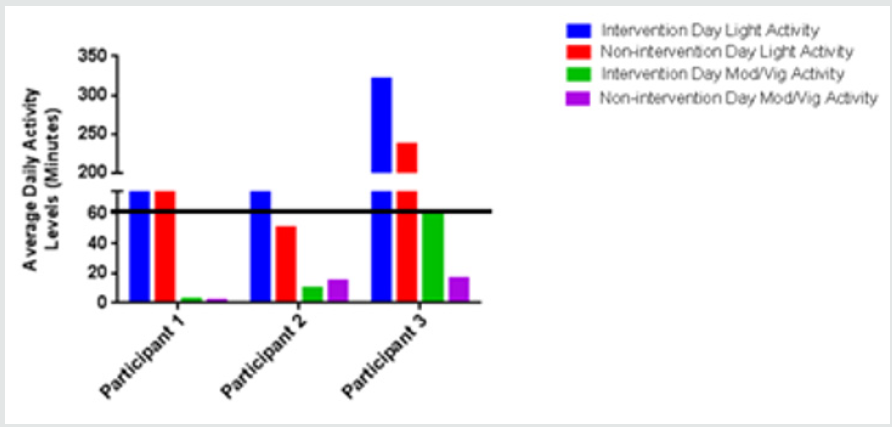
Three female athletes were followed through a subsection of a 10 week physical activity intervention program (Table 2). A fourth athlete had data collected, but it was for less than 50% of the intervention timeframe and so her data was excluded. Another participant had to leave the program for personal reasons; therefore, her data was also excluded. The Fitbit results showed that Participant 1 and Participant 2 did not meet the recommended daily 60 minutes of moderate/vigorous activity throughout the intervention, on either the days of the week with the activity intervention or without (Figure1). However, participant 3 met the average daily activity recommendation on six intervention days. Appropriate device wear age varied from 41% to 97%.
Figure 1: Participant Daily Activity Levels. Each participant’s daily activity was tracked via a Fitbit wearable device. Daily activity was segmented into two pre-defined sub-groups (Light Activity or Moderate/Vigorous Activity), and then further characterized as occurring on Intervention or Non-intervention Days. The ACSM Physical Activity recommendation for adolescents is also shown (line). The data shows that while neither participant achieved the average recommended daily activity level on non-intervention Days (purple), participant three did attain this level on Intervention Days (green).
Discussion
To the end of establishing thresholds values to characterize an
individual’s activity as low, moderate, or vigorous, we performed
post hoc analyses on various daily Fitbit measurements including:
Steps, Minutes Sedentary, Minutes Lightly Active, Minutes Fairly
Active, Minutes Very Active, Activity Calories, Resting Hours, Out of
Range, Fat Burn, Cardio, and Peak. Of these, moderate-to-vigorous
physical activity (MVPA) was best defined by the predefined Cardio
and Peak FitbitTM categories.
While various commercial wearable devices are now available
to quantify daily activity in human subject research, we chose the
Fitbit Inspire HR device largely due to its secure internet interfaces
with the study subjects and our research database. Of note, some
studies have shown that in comparison to validated accelerometers,
FitbitTM devices provided comparatively accurate estimates of
sedentary activity, but overestimates MVPA under free-living
conditions [27]. Additionally, it has been shown that the test-rest
reliability of Fitbit is dependent on activity type and has greater
variation between sessions compared to other wearable devices
[28]. Nonetheless, we found FitbitTM suitable for the intended
purpose, and the development of threshold values to evaluate
groups of people a potential solution to the device’s limitations in
precision measurements.
Obtaining Fitbit daily activity data on underrepresented
minority high school female athletes during a 10-week training
program is feasible. Fitbit MVPA thresholds for moderate and vigorously active levels can be derived and used to evaluate the
efficacy of an intervention aimed at improving sedentary life-styles.
Acknowledgements
This work was supported by research grants from the Konar Foundation and the National Institutes of Health (P30 AR069655).
References
- Haskell W, Lee I, Pate R, Kenneth E Powell,et al. (2007) Physical Activity and Public Health Updated Recommendation for Adults from the American College of Sports Medicine and the American Heart Association. Circulation 116(9): 1081-1093.
- Song M, Carroll D, Fulton J (2013) Meeting the 2008 physical activity guidelines for Americans among U.S. youth. American Journal of Preventive Medicine44(3): 216-222.
- Gortmaker S, Lee R, Cradock A, Sobol A, Duncan D, et al. (2012) Disparities in youth physical activity in the United States: 2003-2006. Medicine & Science in Sports and Exercise44(5): 888-893.
- Gordon-Larsen P, Adair L, Popkin B (2002) Ethic Differences in Physical Activity and Inactivity Patterns and Overweight Status. Obesity Research10(3): 141-149.
- Haughton C,Wang M, Lemon S(2016)Racial/ethnic disparities in meeting 5-2-1-0 recommendations among children and adolescents in the United States. The Journal of Pediatrics175: 188-194.
- Mallee W, Weel H, Dijk Cv, TulderMv, Kerkhoffs G, et al. (2015) Surgical versus conservative treatment for high-risk stress fractures of the lower leg (anterior tibial cortex, naivcular and fifth metatarsal base): a systematic review. British Journal of Sports Medicine49(6): 370-376.
- Whitt-Glover M, Taylor W, Floyd M, Yore M, Yancey A, et al. (2009) Disparities in physical activity and sedentary behaviors among US children and adolescents: prevalence, correlates, and intervention implications. Journal of Public Health Policy30 1: S309-S334.
- Joseph R, Ainsworth B, Keller C, Dodgson J (2015) Barriers to physical activity among African American women: an integrative review of the literature. Women & Health55(6): 679-699.
- Ski C, King-Shier K, Thompson D (2014) Gender socioeconomic and ethnic/racial disparities in cardiovascular disease: a time for change. International Journal of Cardiology170(3): 255-257.
- Singh G, Siahpush M, Azuine R, Williams S (2015) Widening socioeconomic and racial disparaties in cardiovascular disease mortality in the United States. International Journal of MCH and AIDS. 3(2): 106-118.
- Ding D, Lawson K, Kolbe-Alexander T, Eric A Finkelstein, Peter T Katzmarzyk, et al. (2016) The economic burden of physical inactivity: a global analysis of major non-communicable diseases. The Lancet388(10051): 1311-1324.
- Pate R, Saunders R, Dishman R, Addy C, Dowda M, et al. (2007) Long-term effects of a physical activity intervention in high school girls. American Journal of Preventive Medicine33(4): 276-280.
- Kriemler S, Meyer U, Martin E, SlujsEv, Andersen L, et al. (2011) Effect of school-based interventions on physical activity and fitness in children and adolescents: a review of reviews and systematic update. British Journal of Sports Medicine45(11): 923-930.
- Chu A, Ng S, Paknezhad M, Gauterin A, David Koh, et al. (2017) Comparison of wrist-worn Fitbit flex and waist-worn Actigraph for measuring steps in free-living adults. PlosOne12(2): e
- Sylvia L, Bernstein E, Hubbard J, Keating L, Anderson E, et al. (2014) A practical guide to measuring physical activity. Journal of the Academy of Nutrition and Dietitics114(2): 119-208.
- Lee P, Macfarlane D, Lam T (2013) Factors associated with participant compliance in studies using accelerometers. Gait & Posture38(4): 912-917.
- Rosenkranz R, Rosenkranz S, Weber C (2011)Validty of actical accelerometer step-count function in children. Pediatric Exercise Science 23(3): 355-365.
- Cardon G, Bourdeaudhuji ID (2007) Comparison of pedometer and accelerometer measure of physical activity in preschool children. Pediatric Exercise Science19(2): 205-214.
- Sirard J, Slater M (2010) Compliance with wearing physical activity accelerometers in high school students. Journal of Physical Activity and Health6(Suppl): S148-S155.
- Belton S, O'Brian W, Wickel E, Issartel J (2013) Patterns of noncompliance in adolescent field-based accelerometer research. Journal of Physical Activity and Health10(8): 1181-1185.
- Feehan L, Geldman J, Sayre E, Park C, Allison M Ezzat, et al. (2018) Accuracy of Fitbit devices: systematic review and narrative syntheses of quantitative data. JMIR MHealth and uHealth 6(8): e10527.
- Gusmer R, Bosch T, Watkins A, Ostrem J, Dengel D, et al. (2014) Comparison of FitBit ultra to actigraph GT1M for assessment of physical activity in young adults during treadmill walking. The Open Sports Medicine Journal 14(1): 1874-3870.
- Schneider M, Chau L. Validation of the FitBit Zip for monitoring physical activity among free-living adolescents. BMC Research notes 9: 448.
- Cole C, Vasalos K, Nicandri G, Cameron Apt, Osterling E, et al. (2019) Use of PROMIS and Functional Movement System (FMS) Testing to Evaluate the Effects of Athletic Performance and Injury Prevention Training in Female High School Athletes. Orthopedics and Sports Medicine 3(2): 255-258.
- ACSM's Guidelines for exercise testing and prescription. Baltimore: Lippincoot, Williams, & Wilkins, 2006.
- Garber C, Blissmer B, Deschenes M, Barry A Franklin, Michael J Lamonte, et al. (2011) Quantity and Quality of Exercise for Developing and Maintaining Cardiorespiratory, Musculoskeletal, and Neuromotor Fitness in Apparently Healthy Adults: Guidance for Prescribing Exercise. Medicine & Science in Sports and Exercise43(7): 1334-1359.
- Redenius N, Kim Y, Byun W (2019) Concurrent validity of the Fitbit for assessing sedentary behavior and moderate-to-vigorous physical activity. BMC Medical Research and Methodology19: p. 29
- Sushames A, Edwards A, Thompson F, McDermott R, Gebel K, et al. (2016) Validity and realiability of Fitbit Flex for step count, moderate to vigorous physical activity and activity energy expenditure. PLoS One11(9): e0161224.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...





