Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2637-4692
Case Report(ISSN: 2637-4692) 
Implant Impression: What about Splinted Impression Copings? Volume 2 - Issue 3
Debbabi Imen1*, Saafi Jilani2, Harzallah Belhassen2 and Cherif Mounir2
- 1DDM, Department of Fixed Prosthodontics, faculty of dental medicine, Tunisia
- 2Department of Fixed Prosthodontics, Faculty of dental medicine, Tunisia
Received: May 24, 2018; Published: June 05, 2018
Corresponding author: Debbabi Imen, Department of Fixed Prosthodontics, Faculty of dental medicine, Tunisia
DOI: 10.32474/MADOHC.2018.02.000140
Abstract
Dental implants are an exciting field of dentistry that are helping clinicians restore patients to better function and more esthetic outcomes than ever before. An important factor for the success with implant-supported restoration is the passive fit between the superstructure and the abutments. Various implant impression techniques, such as pick-up, transfer techniques have been introduced, and some techniques may be more accurate than others. Clinically, some factors, including the angulation or depth of implants, may affect the accuracy of the implant impressions. This article deals with the procedure of splinted impression copings and its clinical factors affecting implant impression.
Keywords: Implant Impression; Impression Techniques; Open Tray; Splinted Impression Technique; Self-Curing Acrylic Resin; Dental Floss
Introduction
The object of making an impression in implant dentistry is to accurately relate an analogue of the implant or implant abutment to the other structures in the dental arch. This is achieved by use of an impression coping which is attached to the implant or implant abutment. This impression coping is incorporated in an impression much as a metal framework is ‘picked up’ in a remount impression for fixed prosthodontics. With implant copings the coping is usually attached to the implant or abutment with screws. The impression material used is usually an elastomeric impression material; the two types most widely used and shown to be the most appropriate are polyether and polyvinyl siloxane impression materials [1]. Many articles have been written and many in vivo studies have been carried out to improve the fidelity of impressions over the use of pick up type impression copings alone [2]. Characteristics of the pickup type impression coping are that they are removed from the mouth together with the set impression. They require access to the retaining screw to allow release of the screw prior to removal of the impression coping impression assembly the analogues are attached to the impression copings while they are embedded in the impression tray. A custom tray with access to the impression coping screws is required [1].
An accurate transfer of relationship of multi-unit implants from mouth to the master cast demands a rigid splinting of impression copings. Auto-polymerizing acrylic resin, the most commonly used material for such splinting, exhibits polymerization shrinkage resulting inaccurate transfer of spatial relationship of implants from mouth to the master cast [3]. Numerous impression techniques have evolved to improve accuracy [4,5]. One technique involves tying open-tray impression copings together with floss, then splinting them together with self-curing resin [6].
Case Report
Splinted Impression Copings Procedure
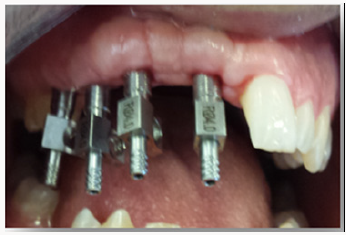
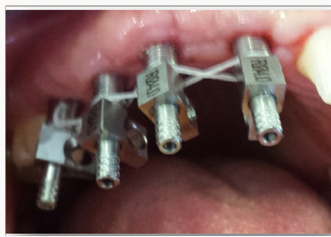
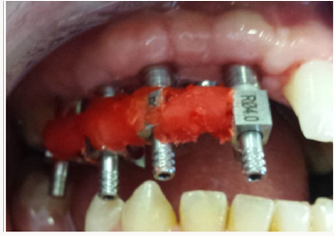
In the first time, impression copings were connected to each implant after removing of healing screws. Then, check-up retro alveolar X-rays were performed to ensure the proper cervical adaptation of the transfers (Figure 1). In the second time, Impression copings were splinted with dental floss (Figure 2) then with auto polymerizing acrylic resin (Figure 3). The resin is placed away from the gum so as not to affect it and to do not interfere with the impression of the peri-implant periodontal environment by the impression material [7]. Before impression procedure, we were waiting, several minutes, the complete polymerization of the resin to avoid a setting contraction of the resin that could affect the fidelity of the impression [8]. During the setting, the resin around the transfers was cooled using the spray of the air-water syringe to fight against the exothermic reaction of the resin which can be transmitted to the transfers [7]. The effect of heat on the implantbone interface has been studied by Ormianer [9]. Direct application of Duralay® or GC Pattern® auto polymerizing resin on transfer’s results in an average increase of 4 to 5° C (up to 6° C maximum) at the implant / bone cervical interface [9].
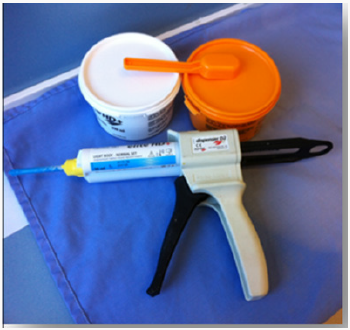
The impression procedure was then accomplished. The heavy consistency polyvinylsiloxane impression material (Figure 4) was loaded inside the impression tray and light consistency polyvinylsiloxane. Impression material was meticulously syringed around the impression copings to ensure complete coverage of the copings. Coping are removed from the mouth together with the set impression. Implant analogs were fastened to the impression copings in the impression. The impression was now poured to create a model (Figure 4-7).
Discussion
Implant-supported prosthodontics requires precise impressions to achieve a passive fit. The fidelity of the impression with respect to dimensional stability is critical; small discrepancies can lead to difficulty when the restoration is fabricated and delivered [1]. Since the early 1990s, in vitro studies comparing different implant impression techniques were performed, capturing the data mostly mechanically [10].
Advantages of direct technique are minimization of dimensional changes in impression upon removal from patient’s mouth, no need to screw in coping again as it comes along with the impression and useful in patients with angulated implants. Many controlling parts during screwing, some spatial movement of the impression coping while screwing in of implant analog, and blind screwing of the implant analog to the impression coping resulting in misfit of components are among the disadvantages of direct technique [11]. When impressions are required for multi implant restorations the precision of the impression is even more critical. This is because frame-works will be constructed from the master cast and misfit in the frameworks can lead to stress applied to the implants on screwing down the framework. Bone loss and even loss of integration has been attributed to this mis-fit [1].
Splinting of impression copings is one of the approaches to ensure this precise fit by making an accurate impression. Splinting squared impression copings with auto polymerizing acrylic resin, adequate polymerization time, and compensation procedures provided for resin have been considered the most desirable approaches while impressing the multiunit implants [3,12]. Out of the 17 studies conducted in past by various researchers, seven advocated the splint technique [13,14] three advocated the nonsplint technique [15,16] and seven reported no difference between them. These studies indicate that there is not statistically significant improvement when splinting impression copings with acrylic, however, the deviation of these impressions from the standardised cast is smaller. Others advocate use of impression plaster to connect the impression copings [17]. The direct technique may be carried out by using splinted or nonsplinted implants impression copings. Acrylic resin, pattern resin, plaster, composite can be chosen for splinting of impression copings [10].
Manufacturers have developed impression copings with ‘metal wings’ that can be connected with acrylic resin to reduce the bulk of shrinking acrylic to further improve dimensional stability of the impression in order to obtain a passive framework [18]. Yet others have advocated corrected impression techniques where impression copings are connected then with only one impression coping related to the cast. The other analogues are retrofitted to the cast to compensate for distortions of the impression material and the distortions of the setting die master cast material. Other authors have demonstrated that none of the above procedures are likely to improve the fidelity of the impression over use of a rigid custom tray and pick up type impression copings with an elastomeric impression material [1,14,19].
Conclusion
Selection of appropriate impression technique to obtain accurate definitive cast depends upon implant angulation, depth, number, position in arch, interarch space, impression material, operator’s choice. The primary purpose of splinting by some clinicians is to gain additional stability of the connected copings in the impression when the abutment analogs are attached to achieve an accurate impression with passive fit.
References
- W Chee, S Jivraj (2006) Impression techniques for implant dentistry. British Dental Journal 201(7): 429-432.
- Assif D, Marshak B, Schmidt A (1996) Accuracy of implant impression techniques. Int J Oral Maxillofac Implants 11(2): 216-222.
- Suryakant C Deogade (2015) An alternative procedure of splinting multiunit implant copings to minimize the resin shrinkage. Journal of Dental Implants 5(2): 124-127.
- Lee H, So JS, Hochstedler JL, Ercoli C (2008) The accuracy of implant impressions: a systematic review. J Prosthet Dent 100(4): 285-291.
- Carr AB (1991) Comparison of impression techniques for a five-implant mandibular model. Int J Oral Maxillofac Implants 6(4): 448-455.
- Bradley C, Bockhorst A Technique for Obtaining Accurate Full-Arch Implant Impressions. Inclusive Magazine 2(1).
- Thierry Degorce (2002) L’empreinte en prothèse fixe implantaire. Stratégie prothétiqu 2(3).
- Loos LG (1986) A fixed prosthodontic technique for mandibular osseointegrated titanium implants. J Prosthet Dent 55(2): 232-242.
- Ormianer Z, Laufer BZ, Nissan J, Gross M (2000) An investigation of heat transfer to the implant-bone interface related to exothermic heat generation during setting of auto polymerizing acrylic resins applied directly to an implant abutment. Int J Oral Maxillofac Impl 15(6): 837- 842.
- Michael Stimmelmayr, Kurt Erdelt, Jan-Frederik Güth, Arndt Happe, Florian Beuer (2012) Evaluation of impression accuracy for a fourimplant mandibular model—a digital approach. Clin Oral Investig 16(4): 1137-1142.
- Shweta Singh, Alok Kumar (2016) Implant Impression Techniques in Dentistry. Journal of Dental Sciences and Oral Rehabilitation 7(3): 137- 141.
- Lee SJ, Cho SB (2011) Accuracy of five implant impression technique: Effect of splinting materials and methods. J Adv Prosthodont 3(4): 177- 185.
- Assif D, Fenton A, Zarb G, Schmitt A (1992) Comparative accuracy of implant impression procedures. Int J Periodontics Restorative Dent 12(2): 112-121.
- Cabral LM, Guedes CG (2007) Comparative analysis of 4 impression techniques for implants. Implant Dent 16 (2): 187-194.
- Inturregui JA, Aquilino SA, Ryther JS, Lund PS (1993) Evaluation of three impression techniques for osseointegrated oral implants. J Prosthet Dent 69(5): 503-509.
- Burawi G, Houston F, Byrne D, Claffey N (1997) A comparison of the dimensional accuracy of the splinted and unsplinted impression techniques for the Bone-Lock implant system. J Prosthet Dent 77(1): 68-75.
- Assif D, Nissan J, Varsano I, Singer A (1999) Accuracy of implant impression splinted techniques: effect of splinting material. Int J Oral Maxillofac Implants 14(6): 885-888.
- Carr AB, Master J (1996) The accuracy of implant verification casts compared with casts produced from a rigid transfer coping technique. J Prosthodont 5(4): 248-252.
- McCartney JW, Pearson R (1994) Segmental framework matrix: master cast verification, corrected cast guide, and analogue transfer template for implant-supported prostheses. J Prosthet Dent 71(2): 197-200.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...