Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2644-1217
Research Article(ISSN: 2644-1217) 
Timing in Efficacy of Traditional Chinese Medicine and Acupuncture Volume 1 - Issue 2
Tong Zheng Hong*
- As-You-Wish Healthcare Institute, Taiwan
Received: October 11, 2018; Published: October 17, 2018
*Corresponding author: Tong Zheng Hong, As-You-Wish Healthcare Institute, MS in Acupuncture awarded by National University of Health Sciences in IL, Taiwan
DOI: 10.32474/OAJCAM.2018.01.000107
Abstract
Increasing scientific research on traditional Chinese medicine and acupuncture provides science-based explanations like deqi. However, most of the research focuses on diseases instead of following TCM and acupuncture theories about pattern identification. Timing is closely connected with therapeutic effects and surely plays a key role in the clinical efficacy that is often ignored. On the other hand, whether or not timing-related efficacy can be influenced with age, gender, and the processing of materia medica in Chinese herbs and acupuncture needs more attention and research.
Keywords: Pattern identification; Chinese herb; Needle retaining; Deqi
Introduction
Both Traditional Chinese medicine (hereinafter TCM) and acupuncture originated in ancient China and has evolved for more than two thousand years. However, most of the people generally present themselves to the medical doctors first when they are in need of medical treatments. Part of this fact is because there is not sufficient scientific evidence to prove the efficacy and safety of TCM, acupuncture, moxibustion, acupressure, cupping, Tui na, and tai chi. TCM and acupuncture have undoubtedly established their status in the health system in the West, though they’re totally different from the Western medicine with the philosophy, diagnosis approaches, and pattern identification for treatment. The literature shows TCM, which is developed on the base of observation of nature and is at present an essential part of the healthcare system in most Asian countries and areas like Taiwan, China, Hong Kong, and Korea, mostly relies on natural products and has been playing an important role with acupuncture in health protection and disease control for thousands of years. In addition to acupuncture, TCM therapeutic efficacy usually attributes to the synergistic property of multiple herbs and constituents with timing that has advocated combinatorial therapeutic strategies called formulas for the improvement of efficacy through targeting on syndromes and patient characteristics guided by the TCM theory.
Except Single Ginseng Decoction (Du Shen Tang) composed of only Ginseng, all the formulas are designed and developed to contain a combination of various kinds of herbs with the assumption that the maximum of therapeutic efficacy can be expected with a synergism of all ingredients. Integration of TCM and acupuncture and Western medicine draw more and more attention, but increasing attention has not been paid to the issue of timing, which is the key without doubt to successful treatment. In this study, discussions about the relation between efficacy and timing are provided.
Quick Look at Timing-Related Examples
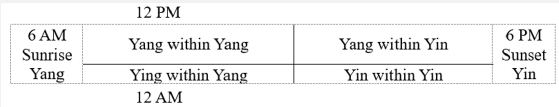
The philosophical concepts like Yin-Yang, the Five Element, pattern identification, and Qi and Blood are, to some extents, unique and abstract to catch the whole picture with the functions broader than the anatomical knowledge in the Western medicine and are absolutely different from the theories of the Western medicine. In terms of relation of the human beings and the Heaven that interacts with each other in providing solutions to the health issues, it is totally different from the Western medicine that TCM views the human body as a whole and as a microcosm of the universe in diagnosis and treatment, bringing the body, mind and spirit into harmony with Yin-Yang balance [1]. Yin-Yang, the earliest concept presented in the I Ching (Book of Changes) in 700 BC, is one of the most fundamental concepts in TCM and acupuncture. With the historical development. Yin-Yang balance is the unique concept and the dominating key of the TCM, including acupuncture, throughout the history of Chinese medicine for many centuries. All phenomena are reduced to Yin-Yang. It is also believed that this concept absolutely distinguishes TCM from the Western medicine with the definitions that Zang organs are classified as Yin, and Fu organs, Yang [2]. In the meantime, this concept of Yin-Yang balance also serves as the foundation and the guidelines for the etiology of diseases, diagnosis, and treatments [3]. 24 hours a day from the aspect of TCM is divided philosophically into Yin (night) and Yang (day), as shown in Figure 1. On the base of this concept, a disease thus represents the loss of the balance of Yin-Yang. In general, all the physiological processes, signs, and symptoms can be reduced to Yin-Yang that can be treated with modality aimed at:
a. Tonification of Yang
b. Tonification of Yin
c. Dispersing excess Yang
d. Dispersing excess Yin
The goal to balancing Yin and Yang can be achieved by stimulations through techniques, such as acupuncture, acupressure, moxibustion, cupping, and Tui Na on acupoints. The classic and well-known protocol of Four Gates (LV 3, Yin and LI 4, Yang) used for the successful treatment of the sub-health demonstrates the application of this concept and highlights the importance of Yin-Yang balance [4]. Qi courses through the body in an endless 24-hour cycle to ensure that energy can flows through the 12 main meridians in the two-hour blocks. Meanwhile, the law of Qi- Blood circulation of the twelve meridians indicate the circulation spends two hours as a period in each of the Zang and Fu organs for health, maintaining Yin-Yang balance with the regular Qi flow [2]. Acupuncture is a medical intervention in which needles are used to stimulate specific and selected acupoints for regulating the function of internal organs for therapeutic effects to prevent and treat diseases. Acupuncture theories indicate that acupuncture stimulation can elicit a composite of unique sensations called deqi, which literally means “arrival of energy” in Chinese. Deqi is usually described as a sensation of a deep pain with an involvement of sensations such as aching, soreness, tingling, numbness, throbbing, involuntary movements of the limbs, and sometimes stabbing pain, and felt by the acupuncturists grasping needles as tense, tight, and full. Deqi, on the other hand, is not only recognized as a prerequisite for the best clinical effects because it tells that whether or not the Qi and Blood in the meridians are activated, but also an important judgment criterion of the exuberance and decline of the meridian Qi and the prognosis of disease, and may be one of great important factors to understand the acupuncture mechanisms [5,6].
Since deqi sensation in TCM and acupuncture is believed to be closely related to clinical efficacy, TCM doctors and acupuncturists elicits deqi sensations with intention in patients and sees deqi as the sign of treatment efficacy with correct manipulation and retaining the needle to strengthen the deqi sensation and improve clinical efficacy to their expectations. The observation in 2014 of a total of 32 patients with primary hyperuricemia, to whom acupuncture was performed on the Five Shu acupoints on the Spleen meridian each morning with the needles retained for 30 minutes when deqi occurred, highlights the importance of deqi in the treatment and shows that the blood uric acid level after acupuncture significantly decreased in patients with increased production (overproduction) of uric acid, decreased excretion (underexcretion) of uric acid, and mixed type [7]. In terms of efficacy, acupuncture stimulation with correct manipulations can elicit deqi, which is suggested to be the main mechanism to produce effects of acupuncture with the releasing spinal and supraspinal beta-endorphins, proinflammatory neuropeptides, and an increase in peripheral circulation [8]. Another point attracting attention is the time to retain the needles for 30 minutes. Classical Chinese philosophy has it that Qi is the force that circulate in the body every 15 minutes a time and can makes up and binds together all things in the universe, including the interaction of body and the universe. This principle suggests acupuncturists that the needles must be retained for at least 15 minutes to ensure the treatment efficacy. The use of Chinese herb must be based on the patient’s conditions with accurate diagnosis, following the principles of pattern identification. Licorice root (Gancao) with properties of sweet and neutral to tonify and strengthen the Spleen qi is effective for sore throat, bronchitis, cough, and infections caused by bacteria or viruses. This herb is the good example highlighting the time to collect herb is an attention that cannot be ignored. Literature shows the best time to collect and dry Licorice root is in the autumn two to three years after planting, but no detailed information is found for the reasons. The possible explanation for harvest time and cultivation time may be much to do with the compound differentiation, which can vary with moisture, temperature, and sunshine [1]. Compared to the granules commonly used in the West, choosing crude herbs or processed material medica shall be the factor that cannot be ignored as well for the best clinical effects. In order to find out the corresponding changes of chemical compositions in Baizhu Shaoyao San (BSS), a famous and widely used traditional Chinese medicinal formula for treating painful diarrhea, intestinal inflammation, and diarrheapredominant irritable bowel syndrome, after processing and to elucidate the material basis of the changed curative effects, Xu et al. developed an optimized ultra-high-performance liquid chromatography-quadrupole/time-of-flight mass spectrometry in positive and negative ion modes coupled with multivariate statistical analyses. The result shows 62 marker compounds with significant differences between crude and processed BSS were found in a total of 186 compounds ultimately identified in crude and processed BSS by principal component analysis and t-test. Compared with BSS without stir-frying processing, the contents of 23 compounds were remarkably decreased and the contents of 39 compounds showed the large increase in processed BSS [9]. The classical theories of TCM say that the therapeutic effects of BSS can be significantly enhanced after processing with the changes of curative constituents mainly resulted from the processing procedure. Three medicinal herbs Atractylodis Macrocephalae Rhizoma, Paeoniae Radix Alba, and Citri Reticulatae Pericarpium included in BSS must be processed using some specific methods of stir-frying [9]. The nature, flavor, and therapeutic effects of Chinese herbs are closely linked to the cooking time. Therefore, the time of cooking herbs is one of the factors that has much to do with the treatment. In the research for understanding the law of changing the chemical constituents, the result shows that the main factors which can influence the chemical constituents of Radix et Rhizoma Rhei (Dahuang) decoction pieces before and after processing include the kinds of excipients, temperature and heating time. The higher temperature or longer heating time can reduce the content of anthraquinone glycosides and increase the content of free anthraquinone in varying degrees [10].
It is very important to look at each herb carefully as each herb contains different constituents. Knowledge discussed in the ancient and traditional TCM classics suggest the temperature energetic can come out of the herb during the first steeping, which usually affects the patient mostly at the Qi level related to more superficial and more Yang in nature. However, the patients are affected more on the Blood level during the second steeping with the taste energetics coming out of the herb. Some herbs like Bie Jia (Turtle Shell) and Ci Shi (Magnetite) are made from substances that may require much more time to leach out the therapeutic ingredients. These herbs generally need 20 to 30 minutes longer for cooking. On the contrary, aromatic herbs, such as Bo He (Peppermint) and Mu Xiang (Radix Auklandiae Lappae), are used in clinic to moves Qi, relieve Pain, and regulate the Middle Jiao with the property of spicy, so they should be cooked for periods shorter than 20 minutes. For the purpose keeping aroma, cook the rest of the herbs first and finally add these aromatic herbs to keep volatile oils from quick evaporation.
Discussion
Deqi, which is believed to be an important variable in the studies of the mechanism and efficacy of acupuncture treatment, has attracted much more attention in recent years and great efforts like to qualify and quantify deqi sensations with questionnaires, neuroimaging studies of deqi and acupuncture, physiological mechanisms of deqi, and the relation between deqi and clinical efficacy have been made to learn more about deqi and explore if deqi sensation can be achieved through manipulation and the needle retaining to strengthen deqi sensation [11]. Hyperuricemia in TCM is viewed as the result of dampness, which is classified as Yin, in the body on the base of Spleen qi deficiency. Qi is Yang that can result in dampness when it is deficient. Based on the law of the Qi-Blood circulation, 9-11 a.m. should refer to Yang with Yang in the time block, corresponding to Stomach and Spleen organs. This law also suggests that the treatment in this two-hours block can tonify Yang and replenish Spleen and Stomach Qi. Needle retaining duration also plays a key factor in the successful and effective treatment. In general, it takes 15 minutes per session based on the law of Qi circulation in acupuncture theory. However, it remains uncertain if the longer retaining can bring about the better or the best effect. A total of 251 ischemic apoplexy patients were randomly divided into 20 min, 40 min and 60 min groups respectively and punctured and stimulated electrically with parameters of 2 Hz, 2-6 mA for 20 min, 40 min and 60 min separately, once a day for 10 times, according to their state (mild, moderate and severe) of disease. The result shows the effective rate of 60 min group was significantly higher than those of 20 min and 40 min groups (P<0.01, 0.05) [12]. The same result is included in another study of a total of 82 patient with post-stroke hemiplegia. The patients who met the inclusion criteria were randomly allocated into control group (22 cases), short-time needle-retaining group (30 cases), and long-time needle-retaining group (30 cases) with scalp acupuncture. Cases in the long-time needle-retaining group obtained better effects in motor function of the limbs and activities of daily living (ADL) than the other two groups [13]. The two studies presented above seem to suggest the longer needle retaining, the better result to patients with ischemic stroke and with post-stroke hemiplegia. Unfortunately, TCM pattern identification, which is the unique concept that distinguishes TCM and acupuncture from the Western medicine and seen as the guideline for diagnosis and treatment, was not discussed and whether or not the results can apply to hemorrhage stroke, other diseases, or even different patterns in TCM deserves more research. With the cases about Chinese herbs discussed above, processing methods of herbs cannot apply to granules mostly used in the West. In other words, this may be the key to unsuccessful treatments and suggest that the use of crude herbs needs more research and deserves much attention [14].
Conclusion
Correct use of Chinese herbal medicine can lead to a profound depth in treating a fantastically enormous array of conditions and to the improvement of clinical efficacy to the last degree. It is notable that most of the contemporary scientific research for the verification of clinical efficacy of TCM and acupuncture cannot accurately verify the TCM and acupuncture theories to a great extent because they only focus on diseases, instead of following the pattern identification that distinguishes TCM and acupuncture from the Western medicine. Factors like age, gender, and the processing of materia medica may affect the therapeutic efficacy. No studies to our knowledge have systemically investigated the relationship between different aspects of timing related to TCM herbs, including acupuncture, and treatment effects with pattern identification, which deserves more attention and research in the future.
References
- Hong TZ (2018) Challenges in learning and understanding traditional Chinese medicine and acupuncture.
- Hong TZ (2017) Exploring a new extra point for sub-acute cough: A case report. J Complement Med Alt Healthcare J 3(4).
- Maciocia G (1989) The foundations of Chinese Medicine. Library of Congress Cataloging in Publication Data. NY.
- Hong TZ (2009) Application of four gates to treating sub-health. Hsinchu City Community Policing (15): 13-17.
- Kong J, Gollub R, Huang T, Polich G, Napadow W, et al. (2007) Acupuncture De Qi, from qualitative history to quantitative measurement. J Altern Complement Med 13(10): 1059-1070.
- Beissner F, Marzolff I (2012) Investigation of acupuncture sensation patterns under sensory deprivation using a geographic information system. Evidence-Based Complementary and Alternative Medicine, p. 10.
- Sun BG, Meng J, Xiang T, Chen ZX, Zhang SJ (2014) Acupuncture of the Five Shu Acupoints in spleen meridian to lower blood uric acid level. Ann Palliat Med 3(1): 22-7.
- Liu S, Zhou WH, Ruan XZ, Li R, Lee T, et al. (2007) Activation of the hypothalamus characterizes the response to acupuncture stimulation in heroin addicts. Neurosci let 421(3): 203-208.
- Xu Y, Cai H, Cao G, Duan Y, Pei KJ, et al. (2018) Profiling and analysis of multiple constituents in Baizhu Shaoyao San before and after processing by stir-frying using UHPLC/Q-TOF-MS/MS coupled with multivariate statistical analysis. J Chromatogr B Analytical Technol Biomed Life sci 1083: 110-123.
- Li L, Zhang C, Xiao YQ, Lin N, Liu CF, et al. (2009) Change laws of chemical constituents of 5 kinds of Dahuang (Radix et Rhizoma Rhei) decoction pieces. Journal of Beijing University of Traditional Chinese Medicine 32: 839-841.
- Hui KK, Marina O, Claunch JD, Nixon EE, Fang J, et al. (2009) Acupuncture mobilizes the brain’s default mode and its anti-correlated network in healthy subjects. Brain Res 1287: 84-103.
- He YZ, Han B, Zheng SF, Wang LN, Chen ZM, et al. (2007) Effect of different acupuncture needle-retaining time on hemorheology in ischemic stroke patients. Zhen Ci Yan Jiu 32(5): 338-341.
- Li HZ, Xie K, Zhou LF, Fu QL, Zheng PH (2013) Effect of needle-retaining time on therapeutic efficacy for post-stroke hemiplegia. J Acupunct Tuina Sci 11(4): 222-225.
- Hong TZ (2017) Acupressure or Acupuncture at Sanyinjiao (SP6) for Primary Dysmenorrhea. J Network Med Target Ther 1(1).

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...