Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2644-1217
Research ArticleOpen Access
Smoking May Not Increase Systolic and Diastolic Blood Pressures Volume 4 - Issue 2
Mehmet Rami Helvaci1*, Semih Salaz2, Engin Altintas1, Orhan Ekrem Muftuoglu1, Abdulrazak Abyad3 and Lesley Pocock4
1Specialist of Internal Medicine, Turkey
2Ministry of Health of Turkey, Turkey
3Middle-East Academy for Medicine of Aging, Turkey
4Medi-WORLD International, Turkey
Received: November 02, 2022 Published: November 16, 2022
*Corresponding author: Mehmet Rami Helvaci, Specialist of Internal Medicine, Turkey
DOI: 10.32474/OAJCAM.2022.04.000185
Abstract
Background: We tried to understand whether there are some effects of smoking on systolic and diastolic blood pressures (BP).
Method: Consecutive daily smokers at least with six pack months and age and sex-matched non-smokers were taken into the study. Cases with regular alcohol consumption (one drink a day) for at least six months and patients with inflammatory, infectious, or devastating disorders or heart failure were excluded.
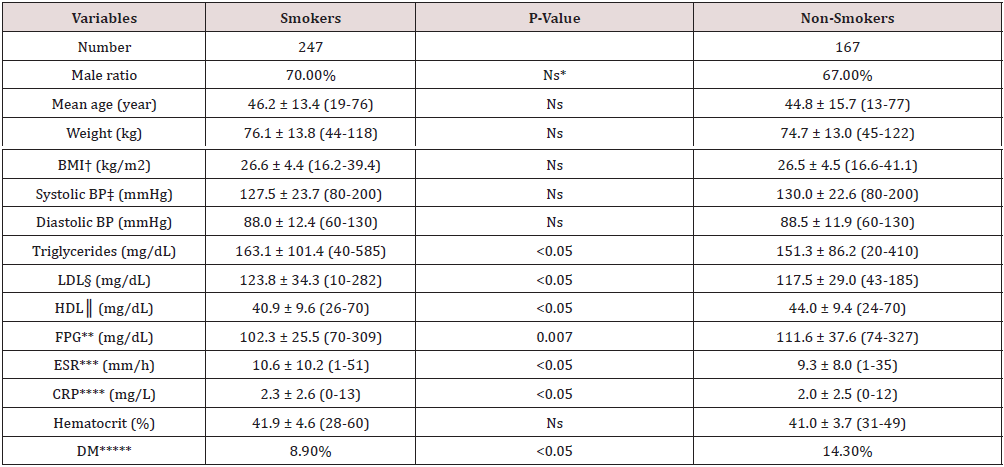
Results: The study included 247 smokers (173 males) and 167 non-smokers. Mean age of the smokers was 46.2 years, and 70.0% of them were males. Although the plasma triglycerides (163.1 versus 151.3 mg/dL, p<0.05), low density lipoproteins (LDL) (123.8 versus 117.5 mg/dL, p<0.05), erythrocyte sedimentation rate (ESR) (10.6 versus 9.3 mm/h, p<0.05), and C-reactive protein (CRP) (2.3 versus 2.0 mg/L, p<0.05) values were all higher in the smokers, the body weight, body mass index (BMI), and systolic and diastolic BP were not changed in them. On the other hand, high density lipoproteins (HDL) (40.9 versus 44.0 mg/dL, p<0.05) and fasting plasma glucose (FPG) (102.3 versus 111.6 mg/dL, p= 0.007) values and prevalence of diabetes mellitus (DM) (8.9% versus 14.3%, p<0.05) were all lower in the smokers.
Conclusion: Smoking causes a low-grade systemic inflammation on vascular endothelium terminating with an accelerated atherosclerosis-induced end-organ insufficiencies all over the body. Although the plasma triglycerides, LDL, ESR, and CRP were increased, and HDL, FPG, and DM were decreased in the smokers, the body weight, BMI, and systolic and diastolic BP were not changed in them, significantly.
Keywords: Smoking; Systolic Blood Pressure; Diastolic Blood Pressure; Triglycerides; Low Density Lipoproteins; High Density Lipoproteins; Fasting Plasma Glucose
Introduction
The endothelium is a monolayer of endothelial cells which constitutes the inner lining of artery, vein, capillary, and lymphatics. It may be the major player in the control of blood fluidity, platelets aggregation, and vascular tone. It may be the major actor in immunology, inflammation, and angiogenesis. It may also be important in endocrinology. The endothelial cells control vascular tone and blood flow by synthesizing and releasing nitric oxide, metabolites of arachidonic acid, and reactive oxygen species. Additionally, they are also important for generation of vasoactive hormones such as angiotensin II. An endothelial dysfunction linked to an imbalance in the synthesis or release of these endothelial factors may explain the initiation of several cardiovascular pathologies including hypertension (HT) and atherosclerosis. On the other hand, overweight, obesity, smoking, and alcohol are wellknown causes of chronic endothelial inflammation terminating with an accelerated atherosclerosis-induced end-organ insufficiencies in human body [1]. Chronic endothelial damage may be the major underlying cause of aging and death by causing end-organ insufficiencies in human being [2]. Much higher blood pressures (BP) of the afferent vasculature may be the major accelerating factor by causing recurrent injuries on vascular endothelium. Probably, whole afferent vasculature including capillaries are mainly involved in the process. Therefore the term of venosclerosis is not as famous as atherosclerosis in the literature. Due to the chronic endothelial damage, inflammation, edema, and fibrosis, vascular walls thicken, their lumens narrow, and they lose their elastic natures, those eventually reduce blood supply to the terminal organs, and increase systolic and decrease diastolic BP further. Some of the well-known accelerating factors of the inflammatory process are physical inactivity, animal-rich diet, overweight, smoking, alcohol, chronic inflammations, prolonged infections, and cancers for the development of terminal consequences including obesity, HT, diabetes mellitus (DM), cirrhosis, peripheric artery disease (PAD), chronic obstructive pulmonary disease (COPD), coronary heart disease (CHD), chronic renal disease (CRD), mesenteric ischemia, osteoporosis, stroke, dementia, other end-organ insufficiencies, early aging, and premature death [3]. Although early withdrawal of the accelerating factors can delay terminal consequences, after development of HT, DM, cirrhosis, COPD, CRD, CHD, PAD, mesenteric ischemia, osteoporosis, stroke, dementia, other end-organ insufficiencies, and aging, endothelial changes cannot be reversed due to their fibrotic natures, completely. The accelerating factors and terminal consequences are researched under the headings of the metabolic syndrome, aging syndrome, and accelerated endothelial damage syndrome in the literature [4, 5]. We tried to understand whether or not there are some effects of smoking on systolic and diastolic BP in the present study.
Material and Methods
The study was performed in the Internal Medicine Polyclinic of the Dumlupinar University between August 2005 and March 2007. Consecutive daily smokers with at least six pack months were taken into the study. Cases with regular alcohol consumption (one drink a day) at least with six months and patients with inflammatory, infectious, or devastating disorders including eating disorders, malignancies, acute or chronic renal failure, cirrhosis, COPD, hyper- or hypothyroidism, and heart failure were excluded. A routine checkup procedure including hemogram, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), fasting plasma glucose (FPG), triglycerides, low density lipoproteins (LDL), high density lipoproteins (HDL), albumin, creatinine, thyroid function tests, hepatic function tests, markers of hepatitis A, B, C, and human immunodeficiency viruses, urinalysis, a posterior-anterior chest x-ray graphy, and an electrocardiogram was performed. An additional Doppler echocardiogram and/or an abdominal ultrasonography were performed just in case of requirement. Body mass index (BMI) of each case was calculated by measurements of the Same Physician instead of verbal expressions. Weight in kilograms is divided by height in meters squared [6]. Office BP were checked after a 5-minute of rest in seated position with mercury sphygmomanometer. Cases with an overnight FPG level of 126 mg/ dL or higher on two occasions were defined as diabetics. An oral glucose tolerance test with 75-gram glucose was performed in cases with a FPG level between 110 and 125 mg/dL, and diagnosis of cases with a 2-hour plasma glucose level of 200 mg/dL or greater is DM [6]. Eventually, all smokers were collected into the first, and age and sex-matched non-smokers were collected into the second groups. Mean body weight, BMI, systolic and diastolic BP, triglycerides, LDL, HDL, FPG, ESR, CRP, and hematocrit values and prevalences of DM were detected in each group and compared in between. Mann-Whitney U test, Independent-Samples T test, and comparison of proportions were used as the methods of statistical analyses.
Results
The study included 247 smokers (173 males and 74 females) and 167 non-smokers (112 males and 55 females). The mean age of smokers was 46.2 years, and 70.0% of them were males. Although the plasma triglycerides (163.1 versus 151.3 mg/dL, p<0.05), LDL (123.8 versus 117.5 mg/dL, p<0.05), ESR (10.6 versus 9.3 mm/h, p<0.05), and CRP (2.3 versus 2.0 mg/L, p<0.05) values were all higher in the smokers, the body weight, BMI, and systolic and diastolic BP were similar in both groups. On the other hand, mean HDL (40.9 versus 44.0 mg/dL, p<0.05) and FPG values (102.3 versus 111.6 mg/dL, p= 0.007) and prevalences of DM (8.9% versus 14.3%, p<0.05) were all lower in the smokers, significantly (Table 1). The smokers had a mean history of 20.5 ± 15.0 (1-100) packyear.
*Nonsignificant (p>0.05) †Body mass index ‡Blood pressures §Low density lipoproteins ║High density lipoproteins **Fasting plasma glucose ***Erythrocyte sedimentation rate ****C-reactive protein *****Diabetes mellitus
Discussion
Higher BP indicates that heart and blood vessels are being overworked. In most people with HT, increased peripheral vascular resistance accounts for HT while cardiac output remains normal [7]. The increased peripheral vascular resistance is mainly attributable to structural narrowing of the small arteries and arterioles, although a reduction in the number of capillaries may also contribute [8]. HT is rarely accompanied by symptoms in short term. Symptoms attributed to HT in that period may actually be related with associated anxiety rather than HT alone. However, HT may be one of the major risk factors for CHD, CRD, cirrhosis, COPD, stroke, dementia, and PAD-like end-organ insufficiencies in long term. For example, a reduction of the BP by 5 mmHg can decrease the risk of stroke by 34% and CHD by 21%, and reduce the likelihood of dementia, heart failure, and cardiovascular mortality [9]. On the other hand, we cannot detect any absolute cause in the majority of patients with HT. Physical inactivity, sedentary lifestyle, animal-rich diet, overweight, obesity, smoking, alcohol, chronic inflammations, prolonged infections, and cancers may be the possible risk factors. Particularly, the increased body weight and BMI may be the major determining factors of systolic and diastolic BP in human body [10]. For example, the mean body weight (71.6 versus 57.8 kg) and BMI (24.9 versus 20.7 kg/m2) were retarded in patients with sickle cell diseases (SCD), significantly (p= 0.000 for both) [10].
Parallel to the retarded body weight and BMI, mean values of the systolic (113.3 versus 118.8 mmHg) and diastolic BP (72.3 versus 83.6 mmHg) were also suppressed in the SCD, significantly (p<0.01 for both) [10]. Excess weight-induced chronic low-grade endothelial inflammation may accelerate atherosclerosis and increase systolic and diastolic BP in the human body [11]. The effects of excess weight on BP were also shown in the literature [12, 13]. For example, incidence of sustained normotension (NT) was higher in the underweight (80.3%) than the normal weight (64.0%, p<0.05) and overweight groups (31.5%, p<0.05) [14], and 52.8% of patients with HT had obesity against 14.5% of patients with the sustained NT (p<0.001) [15]. Eventually, excess weight leads to myocardial hypertrophy terminating with decreased cardiac compliance. Combination of these cardiovascular risk factors terminate with increased risks of arrhythmias, cardiac failure, and sudden death. On the other hand, obesity may be one of the terminal consequences of the metabolic syndrome since after development of the obesity, pharmaceutical and nonpharmaceutical approaches provide limited benefit either to heal obesity or to prevent its complications.
Risk of death from all causes including cardiovascular diseases and cancers increases parallel to the range of excess weight in all age groups [16]. The chronic low-grade inflammation may even cause genetic changes in the endothelial cells, and the systemic atherosclerosis may decrease clearance of the malignant cells. So the dominant underlying cause of the metabolic syndrome appears as weight gain, which may be the main cause of insulin resistance, hyperlipoproteinemias, impaired fasting glucose, impaired glucose tolerance, white coat hypertension (WCH), and HT via the prolonged low-grade inflammation on vascular endothelium in whole body [14]. Prevention of the weight gain with physical activity, even in the absence of a prominent weight loss, will probably result with resolution of many parameters of the syndrome [15-19]. According to our experiences, excess weight may actually be a consequence of physical inactivity instead of an excessive eating habit therefore prevention of weight gain cannot be achieved by diet, alone (10). Additionally, limitation of excess weight as an excessive fat tissue around abdomen under the title of abdominal obesity is meaningless, instead it should be defined as overweight or obesity via the BMI since adipocytes function as an endocrine organ, and they produce leptin, tumour necrosis factor (TNF)-alpha, plasminogen activator inhibitor-1, and adiponectin-like cytokines in the plasma [20]. The eventual hyperactivities of sympathetic nervous system and reninangiotensin- aldosterone system are probably associated with elevated systolic and diastolic BP, insulin resistance, and chronic endothelial inflammation. Similarly, the Adult Treatment Panel III reported that although some people classified as overweight with larger muscular masses, most of them also have excessive fat tissue predisposing to the end-points of the metabolic syndrome [6].
Smoking may be the second common cause of vasculitis in the world. It is one of the major risk factors of the atherosclerotic endorgan insufficiencies [1, 21]. Its atherosclerotic effect is the most obvious in Buerger’s disease. Berger’s disease is an obliterative vasculitis characterized by inflammatory changes in small and medium-sized arteries and veins, and it has never been reported in the absence of smoking. Beside the well-known atherosclerotic effects of smoking, some studies reported that smoking in human beings and nicotine administration in animals are associated with the lower BMI values [22]. Some evidence revealed an increased energy expenditure during smoking both on rest and light physical activity [23], and nicotine supplied by patch after smoking cessation decreased caloric intake in a dose-related manner [24]. According to an animal study, nicotine may lengthen intermeal time, and simultaneously decrease amount of meal eaten [25]. Additionally, the BMI seems to be the highest in the former, the lowest in the current, and medium in never smokers [26]. Smoking may be associated with a postcessation weight gain, but evidence suggest that risk of the weight gain is the highest during the first year after quitting and decreases with the following years [27]. Interestingly, the mean weight and BMI were similar both in the smokers and non-smokers in the present study (p>0.05 for both) that may be the main cause of similar systolic and diastolic BP in the nonsmokers and smokers. On the other hand, although the CHD was detected with similar prevalences in both genders, prevalences of smoking and COPD were higher in males against the higher BMI, LDL, triglycerides, WCH, HT, and DM in females [28].
Besides that, the incidence of myocardial infarctions is increased six-fold in women and three-fold in men who smoked at least 20 cigarettes per day [29]. In another word, smoking may be more harmful for women about the atherosclerotic endpoints probably due to the higher BMI and its consequences in them. Similarly, smoking is consistently higher in men in the literature [21]. Several toxic substances found in cigarette smoke get into the circulation via the respiratory tract and cause vascular endothelial inflammation in all systems of the body. For example, smoking may even terminate with irritable bowel syndrome (IBS) and its consequences including chronic gastritis, hemorrhoids, and urolithiasis. There may be several underlying mechanisms terminating with the IBS and its consequences in smokers [30]. First of all, smokinginduced vascular endothelial inflammation may disturb epithelial functions for absorption and excretion in the gastrointestinal and genitourinary tracts. These functional problems may terminate with the symptoms and components of the IBS including loose stool, diarrhea, constipation, and urolithiasis. Secondly, diarrheal losses-induced urinary changes may even cause urolithiasis [31,32]. Thirdly, smoking-induced sympathetic nervous system activation may cause motility disorders in the gastrointestinal and genitourinary tracts. Finally, immunosuppression secondary to smoking-induced vascular endothelial inflammation may even terminate with gastrointestinal and genitourinary tract infections causing loose stool, diarrhea, and urolithiasis since some types of bacteria can provoke urinary supersaturation and modify the environment to form crystal deposits in the urine. In fact, 10% of urinary stones are struvite stones which are built by magnesium ammonium phosphate produced during infection with bacteria that possess the enzyme, urease. Similarly, urolithiasis was detected in 17.9% of cases with the IBS versus 11.6% of cases without (p<0.01) [31].
Alcohol may be the third common cause of vasculitis in the world. Alcohol is the most dangerous drug, and the only drug that mostly damaged the others. It is causally linked to more than 200 different diseases, conditions, and injuries [33]. For instance, people hospitalized with alcohol use disorder (AUD) have an average life expectancy of 47-53 years in men and 50-58 years in women and die 24-28 years earlier than the general population [34]. People with AUD have three-fold higher mortality in men and four-fold higher mortality in women [35]. A very substantial part of the Danish excess mortality and lower life expectancy compared to Sweden can be attributed to higher mortality related to alcohol and tobacco consumption [16]. Women are generally more sensitive to harmful effects of alcohol, primarily due to their smaller body weight, lower capacity to metabolize alcohol, and higher proportion of body fat. Alcohol can damage liver and brain, and its consumption is one of the major causes of cancers all over the world [33]. Alcohol may even cause loss of consciousness and death in high amounts. Hepatic alcohol dehydrogenase is the main enzymatic system to metabolize alcohol that requires the cofactor nicotinamide adenine dinucleotide (NAD), and the products are acetaldehyde and reduced NAD.
Normally, NAD is used to metabolize fats in the liver, but alcohol competes with these fats for the use of NAD in drinkers. In another definition, prolonged exposure of alcohol means that fats accumulate in the liver, leading to the term of fatty liver. Acetaldehyde is subsequently metabolized by the aldehyde dehydrogenase into acetate which in turn is broken down into carbon dioxide and water. Ethanol is the only type of alcohol that is found in alcoholic beverages. Ethanol crosses biological membranes and blood-brain barrier via passive diffusion, easily. Alcohol works in the brain primarily by increasing the effects of the gamma aminobutyric acid that is the major inhibitory neurotransmitter in the brain. Alcohol produces happiness and euphoria, decreased anxiety, increased sociability, sedation, impairment of cognitive, memory, motor, and sensory functions, and generalized depression of central nervous system. Drinking in pregnancy may terminate with fetal disorders, since ethanol is classified as a teratogen. Alcohol is addictive to humans, and can result in AUD, dependence, and withdrawal. Continued alcohol consumption leads to cell death in liver, scarring, cirrhosis, and hepatocellular carcinoma. Prolonged heavy consumption may even cause permanent brain damage. Similarly, alcohol is the major contributing factor of elevated triglycerides in the plasma. It is well that plasma triglycerides are sensitive acute phase reactants (APR) in the body [12]. Although the cases with regular alcohol consumption were excluded, plasma triglycerides were higher in smokers in the present study (163.1 versus 151.3 mg/dL, p<0.05), indicating the inflammatory properties of smoking in the human body.
An acute phase response occurs in case of infection, infarction, foreign body, autoimmune disorder, allergy, neoplasm, trauma, and burn-like stresses of the body. Certain mediators known as APR are increased or decreased during the acute phase response [36,37]. These markers are commonly measured in clinical practice as indicators of acute inflammation in the body. The terms of acute phase proteins and APR are usually used synonymously, although some APR are polypeptides rather than proteins. Positive and negative APR are those whose concentrations increase or decrease during the acute phase response, respectively. The acute phase response is predominantly mediated by the proinflammatory cytokines including TNF, interleukin (IL)-1, and IL-6 secreted by immune cells. In case of inflammation, infection, or tissue damage, neutrophil and macrophages release such cytokines into the circulation. The liver and some other organs respond by producing many positive APR to the cytokines. Some of the well-known positive APR are ESR, CRP, fibrinogen, ferritin, procalcitonin, hepcidin, haptoglobin, ceruloplasmin, complement proteins, and serum amyloid A. CRP is responsible for activation of the complement pathway. Serum CRP rises rapidly, with a maximal concentration reached within two days, and falls quickly once the inflammation has resolved. Measurement of CRP is a useful indicator of inflammation in the body. It correlates with ESR, but not always directly.
This is due to the ESR being largely dependent upon elevation of fibrinogen with a half-life of one week, approximately. Therefore ESR remains higher for a longer period of time despite the removal of the inflammatory stimulus. Whereas CRP rises with a half-life of 6-8 hours rapidly, and then returns to normal in case of a successful treatment, quickly. On the other hand, productions of the negative APR are suppressed at the same time. Some of the well-known negative APR are albumin, transferrin, retinol-binding protein, antithrombin, transcortin, alpha-fetoprotein, and hemoglobin. The suppression of such APR is also used as an indicator of inflammation in the human body. Suppression of the synthesis of such negative APR may be due to the protection of amino acids for the production of positive APR, sufficiently. As also observed in the present study, productions of HDL may also be suppressed in the liver during the acute phase responses [38]. Similarly, triglycerides, DM, and CHD were significantly higher in patients with plasma HDL values of lower than 40 mg/dL, [38]. So HDL may actually behave as negative, and triglycerides behave as positive APR in the plasma. Similarly, the highest CHD of the group with HDL values of lower than 40 mg/dL can also be explained by the same hypothesis in the other study [12]. Additionally, plasma triglycerides increased whereas HDL decreased during infections [39]. On the other hand, a 10 mg/dL increase of plasma LDL values was associated with a 3% lower risk of hemorrhagic stroke [40]. Similarly, the highest prevalences of HT and DM parallel to the increased values of LDL and HDL, and the highest prevalences of COPD, CHD, and CRD in contrast to the lowest values of LDL and HDL may show initially positive but eventually negative behaviors of LDL and HDL as the APR [41]. Interestingly, the most desired values were between 80 and 100 mg/dL for LDL, between 40 and 46 mg/dL for HDL, and lower than 60 mg/dL for triglycerides in the plasma [12]. Parallel to ESR and CRP, plasma triglycerides and LDL may behave as positive whereas HDL and FPG behave as negative APR in smokers in the present study. In another definition, low HDL values should alert clinicians about searching of additional inflammatory pathologies [42-44].
HDL may behave as negative APR in the body. Normally, HDL may show various anti-atherogenic properties including reverse cholesterol transport and anti-oxidative and anti-inflammatory properties [43]. However, HDL may become ‘dysfunctional’ in pathologic conditions which means that relative compositions of lipids and proteins, as well as the enzymatic activities of HDL are altered [43]. For example, properties of HDL are compromised in patients with DM by means of the oxidative modification, glycation, and transformation of HDL proteomes into proinflammatory proteins. Additionally, the drugs increasing HDL values in the plasma such as niacin, fibrates, and cholesteryl ester transfer protein inhibitors did not reduce all-cause mortality, CHD mortality, myocardial infarction, and stroke [45]. In other definition, HDL may just be some indicators instead of being the main actors of the human health. Similarly, BMI, DM, and CHD were the lowest between the HDL values of 40 and 46 mg/dL, and the prevalence of DM was only 3.1% between these values against 22.2% outside these limits [46]. Similar to the present study, FPG and HDL were also suppressed in SCD, probably due to the severe inflammatory nature of the diseases [47]. Smoking may reduce HDL in the plasma due to the systemic inflammatory effects on vascular endothelium. On the other hand, plasma triglycerides were the only lipids those were not suppressed in pathological weight losses in the body. For example, plasma triglycerides were not decreased, even increased in contrast to the suppressed body weight and BMI in the SCD [48]. Similarly, prevalences of excess weight, DM, HT, and smoking were all higher in the hypertriglyceridemia group (200 mg/dL and higher) [49]. On the other hand, the greatest number of deteriorations in the metabolic parameters was observed just above the plasma triglycerides value of 60 mg/dL [50].
FPG may also be found among the negative APR in the body. The body’s homeostatic mechanism keeps blood glucose levels within a narrow range. There are two groups of mutually antagonistic hormones affecting the blood glucose levels. Glucagon, cortisol, and catecholamines are the catabolic hormones increasing the blood glucose, whereas insulin is the anabolic hormone decreasing the blood glucose levels. Glucagon is secreted from the alpha cells, while insulin is secreted from the beta cells of pancreatic islets which are the bundles of endocrine tissues. They regulate the blood glucose levels together through a negative feedback mechanism. When the blood glucose level is too high, insulin tells muscles to take up excess glucose for storage. When the blood glucose level is too low, glucagon informs the tissues to produce more glucose. Glucagon and insulin are secreted into the portal vein and extracted from the portal vein by the liver. Epinephrine prepares the muscles and respiratory system for a ‘fight to fight’ response. Cortisol prepares the body for the stresses. Glucose is stored in the skeletal muscles and hepatocytes in the form of glycogen. A blood glucose level of four grams, or about a teaspoon, is critical for the normal function of millions of cells in the human body [51].
The brain consumes about 60% of the blood glucose at rest. The four grams of glucose circulates in the blood stream of a person with a body weight of 70 kg. This amount is kept constant with a sophisticated control system of the body. The constant blood glucose levels are maintained at the expense of hepatic and muscular glycogen stores at rest. FPG, which is measured after a fast of 8 hours, is the most used indication of overall glucose homeostasis. Infection, inflammation, surgical operation, depression, alcohol, smoking, and various stresses may affect the overall glucose homeostasis of the body. For example, smoking was negatively associated with FPG and type 2 DM in Chinese men of normal weight, but no significant association was found in men with excess weight or in women [52]. On the other hand, smoking was positively associated with nonfatal stroke, particularly in patients with type 2 DM [52]. Similarly, smokers have a lower likelihood of newly diagnosed DM among Chinese males with a lower BMI [53]. The mean FPG value (102.3 versus 111.6 mg/dL, p= 0.007) and prevalence of DM (8.9% versus 14.3%, p<0.05) were also decreased in the smokers in the present study. As a conclusion, smoking causes a low-grade systemic inflammation on vascular endothelium terminating with an accelerated atherosclerosis-induced end-organ insufficiencies all over the body. Although the plasma triglycerides, LDL, ESR, and CRP were increased, and HDL, FPG, and DM were decreased in the smokers, the body weight, BMI, and systolic and diastolic BP were not changed in them, significantly.
References
- Helvaci MR, Aydin Y, Gundogdu M (2012) Smoking induced atherosclerosis in cancers. HealthMED 6(11): 3744-3749.
- Helvaci MR, Kaya H, Borazan A, Ozer C, Seyhanli M et al (2008) Metformin and parameters of physical health. Intern Med 47(8): 697-703.
- Helvaci MR, Algin MC, Abyad A, Pocock L (2018) Physical inactivity or an excessive eating habit. Middle East J Nursing 12(1): 14-8.
- Eckel RH, Grundy SM, Zimmet PZ (2005) The metabolic syndrome. Lancet 365(9468): 1415-28.
- Helvaci MR, Ayyildiz O, Muftuoglu OE, Yaprak M, Abyad A, et al. (2017) Aging syndrome. World Family Med 15(3): 39-42.
- Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation 2002; 106(25): 3143-3421.
- Conway J (1982) Hemodynamic aspects of essential hypertension in humans. Physiol Rev 64(2): 617-660.
- Folkow B (1982) Physiological aspects of primary hypertension. Physiol Rev 62(2): 347-504.
- Law M, Wald N, Morris J (2003) Lowering blood pressure to prevent myocardial infarction and stroke: a new preventive strategy. Health Technol Assess 7(31): 1-94.
- Helvaci MR, Ayyildiz O, Gundogdu M, Aydin Y, Abyad A, et al. (2019) Body mass and blood pressure. World Family Med 17(1): 36-40.
- Yudkin JS, Stehouwer CD, Emeis J J, Coppack SW (1999) C-reactive protein in healthy subjects: associations with obesity, insulin resistance, and endothelial dysfunction: a potential role for cytokines originating from adipose tissue? Arterioscler Thromb Vasc Biol 19(4): 972–978.
- Helvaci MR, Yapyak M, Tasci N, Abyad A, Pocock L (2020) The most desired values of high and low density lipoproteins and triglycerides in the plasma. World Family Med 18(8): 21-27.
- Calle EE, Thun MJ, Petrelli JM, Rodriguez C, Heath CW Jr (1999) Body-mass index and mortality in a prospective cohort of U.S. adults. N Engl J Med 341(15): 1097-1105.
- Helvaci MR, Kaya H, Yalcin A, Kuvandik G (2007) Prevalence of white coat hypertension in underweight and overweight subjects. Int Heart J 48(5): 605-613.
- Helvaci MR, Kaya H, Duru M, Yalcin A (2008) What is the relationship between white coat hypertension and dyslipidemia? Int Heart J 49(1): 87-93.
- Juel K (2008) Life expectancy and mortality in Denmark compared to Sweden. What is the effect of smoking and alcohol? Ugeskr Laeger 170(33): 2423-2427.
- Franklin S S, Barboza M G, Pio J R, Wong N D (2006) Blood pressure categories, hypertensive subtypes, and the metabolic syndrome. J Hypertens 24(10): 2009-2016.
- Azadbakht L, Mirmiran P, Esmaillzadeh A, Azizi T, Azizi F (2005) Beneficial effects of a Dietary Approaches to Stop Hypertension eating plan on features of the metabolic syndrome. Diabetes Care 28(12): 2823-2831.
- Helvaci MR, Ayyildiz O, Gundogdu M, Aydin Y, Abyad A, Pocock L (2018) Excess weight or smoking. World Family Med 16(10): 14-19.
- Funahashi T, Nakamura T, Shimomura I, Maeda K, Kuriyama H et al (1999) Role of adipocytokines on the pathogenesis of atherosclerosis in visceral obesity. Intern Med 38(2): 202-206.
- Fodor JG, Tzerovska R, Dorner T, Rieder A (2004) Do we diagnose and treat coronary heart disease differently in men and women? Wien Med Wochenschr 154(17-18): 423-425.
- Grunberg NE, Greenwood MR, Collins F, Epstein LH, Hatsukami D, Niaura R, et al (1992) National working conference on smoking and body weight. Task Force 1: Mechanisms relevant to the relations between cigarette smoking and body weight. Health Psychol 11: 4-9.
- Walker JF, Collins LC, Rowell PP, Goldsmith LJ, Moffatt RJ, Stamford BA (1999) The effect of smoking on energy expenditure and plasma catecholamine and nicotine levels during light physical activity. Nicotine Tob Res 1(4): 365-370.
- Hughes JR, Hatsukami DK (1997) Effects of three doses of transdermal nicotine on post-cessation eating, hunger and weight. J Subst Abuse 9: 151-159.
- Miyata G, Meguid M M, Varma M, Fetissov S O, Kim H J (2001) Nicotine alters the usual reciprocity between meal size and meal number in female rat. Physiol Behav 74(1-2): 169-176.
- Laaksonen M, Rahkonen O, Prattala R (1998) Smoking status and relative weight by educational level in Finland, 1978-1995. Prev Med 27(3): 431-437.
- Froom P, Melamed S, Benbassat J (1998) Smoking cessation and weight gain. J Fam Pract 46(6): 460-464.
- Helvaci MR, Kaya H, Gundogdu M (2012) Gender differences in coronary heart disease in Turkey. Pak J Med Sci 28(1): 40-44.
- Prescott E, Hippe M, Schnohr P, Hein HO, Vestbo J (1998) Smoking and risk of myocardial infarction in women and men: longitudinal population study. BMJ 316(7137): 1043-1047.
- Helvaci MR, Dede G, Yildirim Y, Salaz S, Abyad A, Pocock L (2019) Smoking may even cause irritable bowel syndrome. World Family Med 17(3): 28-33.
- Helvaci MR, Kabay S, Gulcan E (2006) A physiologic events’ cascade, irritable bowel syndrome, may even terminate with urolithiasis. J Health Sci 52(4): 478-481.
- Helvaci MR, Algin M C, Kaya H (2009) Irritable bowel syndrome and chronic gastritis, hemorrhoid, urolithiasis. Eurasian J Med 41(3): 158-161.
- Rehm J (2014) Alcohol and mortality. Alcohol Res 35(2): 174-183.
- Westman J, Wahlbeck K, Laursen TM, Gissler M, Nordentoft M, Hällgren J et al (2015) Mortality and life expectancy of people with alcohol use disorder in Denmark, Finland, and Sweden. Acta Psychiatr Scand 131(4): 297-306.
- Roerecke M, Rehm J (2013) Alcohol use disorders and mortality: a systematic review and meta-analysis. Addiction 108(9): 1562-1578.
- Gabay C, Kushner I (1999) Acute-phase proteins and other systemic responses to inflammation. N Engl J Med 340(6): 448-454.
- Wool GD, Reardon CA (2007) The influence of acute phase proteins on murine atherosclerosis. Curr Drug Targets 8(11): 1203-1214.
- Helvaci MR, Abyad A, Pocock L (2020) High- and low-density lipoproteins may be negative acute phase proteins of the metabolic syndrome. Middle East J Nursing 14(1): 10-16.
- Pirillo A, Catapano A L, Norata G D (2015) HDL in infectious diseases and sepsis. Handb Exp Pharmacol 224: 483-508.
- Ma C, Na M, Neumann S, Gao X (2019) Low-density lipoprotein cholesterol and risk of hemorrhagic stroke: a systematic review and dose-response meta-analysis of prospective studies. Curr Atheroscler Rep 21(12): 52.
- Helvaci MR, Abyad A, Pocock L (2020) The safest values of low density lipoproteins in the plasma. World Family Med 18(4): 18-24.
- Toth PP (2005) Cardiology patient page. The "good cholesterol": high-density lipoprotein. Circulation 111(5): 89-91.
- Femlak M, Gluba-Brzόzka A, Cialkowska-Rysz A, Rysz J (2017) The role and function of HDL in patients with diabetes mellitus and the related cardiovascular risk. Lipids Health Dis 16(1): 207.
- Ertek S (2018) High-density lipoprotein (HDL) dysfunction and the future of HDL. Curr Vasc Pharmacol 16(5): 490-498.
- Keene D, Price C, Shun-Shin MJ, Francis DP (2014) Effect on cardiovascular risk of high-density lipoprotein targeted drug treatments niacin, fibrates, and CETP inhibitors: meta-analysis of randomised controlled trials including 117,411 patients. 349: 4379.
- Helvaci MR, Abyad A, Pocock L (2020) What a low prevalence of diabetes mellitus between the most desired values of high density lipoproteins in the plasma. World Family Med 18(7): 25-31.
- Helvaci MR, Altintas E, Yalcin A, Muftuoglu OE, Abyad A, Pocock L (2022) Positive and negative acute phase reactants in sickle cell diseases. World Family Med 20(3): 36-42.
- Helvaci MR, Salaz S, Yalcin A, Muftuoglu OE, Abyad A, Pocock L (2021) Cholesterol may be a negative whereas triglycerides positive acute phase reactants in the plasma. Asclepius Med Res Rev 4(1): 1-8.
- Helvaci MR, Aydin LY, Maden E, Aydin Y (2011) What is the relationship between hypertriglyceridemia and smoking? Middle East J Age and Ageing 8(6).
- Helvaci MR, Abyad A, Pocock L (2020) The safest upper limit of triglycerides in the plasma. World Family Med 18(1): 16-22.
- Wasserman DH (2009) Four grams of glucose. Am J Physiol Endocrinol Metab 296(1): E11-21.
- Wang S, Chen J, Wang Y, Yang Y, Zhang D, Liu C et al (2019) Cigarette smoking is negatively associated with the prevalence of type 2 diabetes in middle-aged men with normal weight but positively associated with stroke in men. J Diabetes Res 1853018 p. 8.
- Hou X, Qiu J, Chen P, Lu J, Ma X, Lu J et al (2016) Cigarette smoking is associated with a lower prevalence of newly diagnosed diabetes screened by OGTT than non-smoking in Chinese Men with normal weight. PLoS One 11(3): e0149234. 1.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...