Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2644-1403
Research Article(ISSN: 2644-1403) 
Phenylephrine Effectiveness in Handling Hypotensive Issues During Spinal Anesthesia Conductance for Cesarean Section Deliveries Volume 1 - Issue 5
Mohamed Sayed Fahim*
- Anesthesia, Intensive Care and Pain Management Department, Ain Shams University, Egypt
Received:August 01, 2019; Published:August 08, 2019
Corresponding author: Mohamed Sayed Fahim, Anesthesia, Intensive Care and Pain Management Department, Faculty of Medicine, Ain Shams University, Cairo, Egypt
DOI: 10.32474/GJAPM.2019.02.000126
Abstract
Background: Hypotension is frequent clinical challenge during spinal mode of anesthetic induction for cesarean delivery. Requiring an effective and prompt management mode since it has unfavorable clinical outcomes such as hemodynamic cardiovascular instability issues besides reduced uteroplacental perfusion.
Aim: Investigating the impact and effectiveness of different prophylactic dosages of Phenylephrine on hypotensive issues during spinal anesthesia for cesarean section deliveries.
Methodology: A prospective, randomized, clinical research study involved 184 cases That are classified as American Society of Anesthesiologists physical status I and II with term singleton pregnancies scheduled for elective cesarean section under spinal anesthesia randomized to receive 0.9% saline 2mL (Control Group) or phenylephrine1.0ug/kg (PHE1 research Group), 1.5ug/kg (PHE1.5 research Group), or 2.0ug/kg (PHE2 research Group) immediately after induction of spinal anesthesia.
Results: The adverse effects of prophylactic bolus of Phenylephrine among the research groups control, Phenylephrine 1,1.5,2 in which there was statistically significant difference as regards hypotension, rescue Phenylephrine, lowest SBP, highest SBP, early highest SBP, mean SBP, occurrence of hypertension (p values=<0.001, <0.001,0.002, <0.001, <0.001, <0.001, <0.001 consecutively) there was no statistical significant difference as regards nausea and bradycardia (p values=0.929, 0.823 consecutively).
Conclusions: The research findings obtained denote and imply that a prophylactic Phenylephrine 1.5ug/kg bolus followed by additional boluses when necessary could be an alternative management protocol to decrease the frequency of hypotensive issues occurrence during spinal anesthetic mode for cesarean deliveries.
Keywords: Cesarean section; Phenylephrine; Spinal hypotension
Introduction
Spinal anesthesia mode for cesarean deliveries could prevent critical maternal complications linked and correlated to general mode of anesthetic practice [1]. Hypotension is frequent clinical challenge during spinal mode of anesthetic induction for cesarean delivery. Requiring an effective and prompt management mode since it has unfavorable clinical outcomes such as maternal nausea, vomiting, dizziness, and hemodynamic cardiovascular instability issues besides reduced uteroplacental perfusion causing fetal bradycardia, acidosis, and hypoxic issues. Reduced cardiac output is an issue of concern in obstetric anesthesia practice [2]. Phenylephrine as an alpha agonist is a vasopressor of choice for avoidance and management of spinal anesthesia triggered hypotension. Prior research groups of investigators have shown that Phenylephrine is an agent correlated to baroreceptormediated bradycardia and therefore causes a consecutive decrease in cardiac output having an incidence of around 30%, in physiologically healthy maternal and fetal status, those changes occurring from Phenylephrine are considered of trivial impact on the other hand heart rate and cardiac output conservation is of critical value in high-risk clinical scenarios e.g. maternal cardiac illnesses, placental inadequate vascular performance issues, and fetal distress challenges and concerns [3,4].
Henylephrine being used for management of hypotensive issues have been revealed and displayed by various research groups of investigators to enhance the fetal acid base physiological balance, by raising fetal pH and decreasing PCO2 in comparison and contrast to other agents such as ephedrine [5]. Investigators in previous research studies have shown among their findings that prophylactic infusion using rescue Phenylephrine boluses is an efficient mode for maternal maintenance of hemodynamic physiologic stability, and furthermore could reduce physician interventions in comparison to rescue boluses alone [5]. The optimum protocol for Phenylephrine administration haven’t been elucidated by researchers as it was shown by prior research groups of investigators in prior studies that continuous infusion protocols of Phenylephrine which are frequently implemented in obstetric anesthetic practice is linked and correlated to very low statistically estimated incidence of hypotension and decreased nausea and vomiting clinical incidence [6]. On the other hand, even though infusion in a continuous manner is an efficient and convenient in nature, it necessitates appropriately trained personnel with necessary tools such as infusion pump [7]. A prior research study have compared and contrasted Phenylephrine bolus and infusion management protocols, and revealed among their research study findings that blood pressure is superiorly sustained using boluses, particularly within the initial 6 min after spinal anesthesia conductance [8]. It is statically estimated from prior research groups that the hypotension clinical after spinal anesthesia is around 32.5 percent in cases that were administered Phenylephrine as a prophylactic bolus in comparison to 85 percent among a research group that was administered Phenylephrine as a therapeutic dosage only after occurrence of hypotension [9].
Aim of the work
Investigating the impact and effectiveness of different prophylactic dosages of Phenylephrine on hypotensive issues during spinal anesthesia for cesarean section deliveries (Tables 1-5).
Table 1: Research study subjects basic and demographic characteristics.
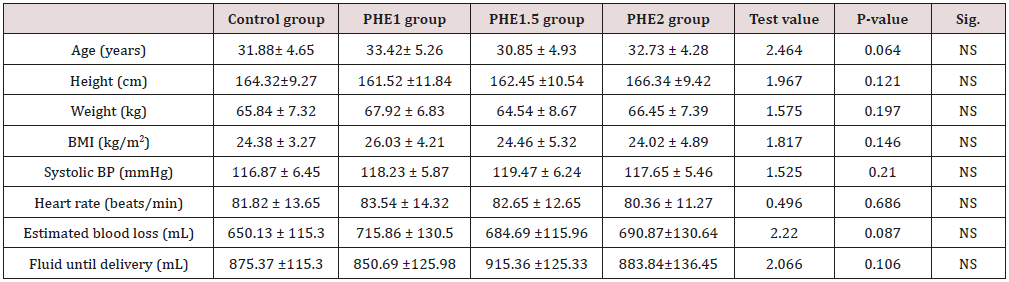
•: Data were presented as mean and standard deviations and compared between groups using One Way ANOVA
Table 2: RAdverse effects of prophylactic bolus of Phenylephrine.

*: Data were presented as number and percentages and compared using Chi-square test.
•: Data were presented as means and standard deviations and compared using One Way ANOVA followed by
post hoc using LSD test; ≠: Data were presented as medians with inter-quartile ranges and compared using
Kruskall-Wallis test followed by post hoc using Mann-Whitney test (a: Significant from Control; b: Significant
from PHE1; c: Significant from PHE1.5).
P < 0.05: Significant; P < 0.01: Highly significant.
Table 3: Changes in the systolic blood pressure (mmHg) during the time of measurement in the four groups.
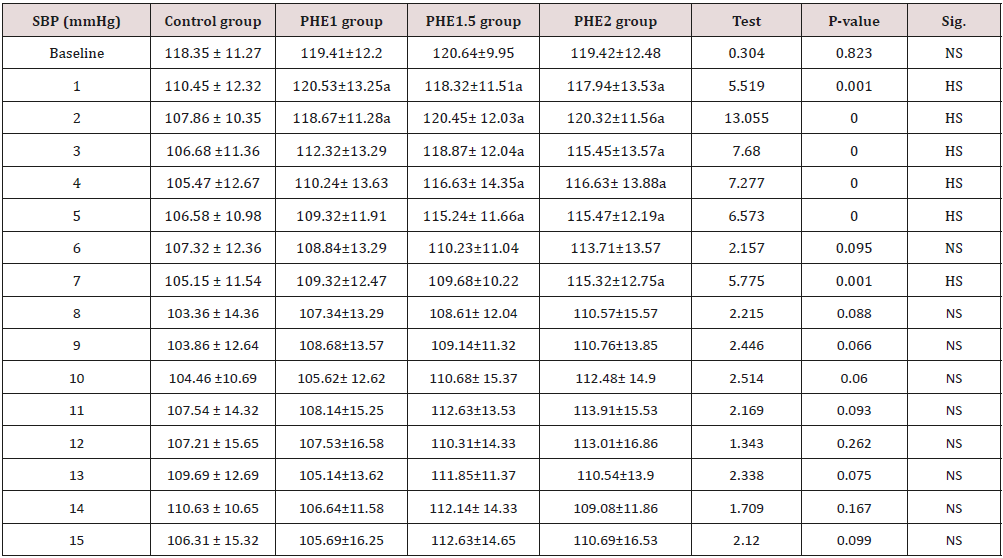
Data were presented as means and standard deviations and compared using One Way ANOVA followed by post hoc analysis using LSD test.a: Significant difference from control group; b: Significant difference from PHE1, c: significant difference from PHE1.5.
Table 4: Number of boluses used in each period among the four research groups.
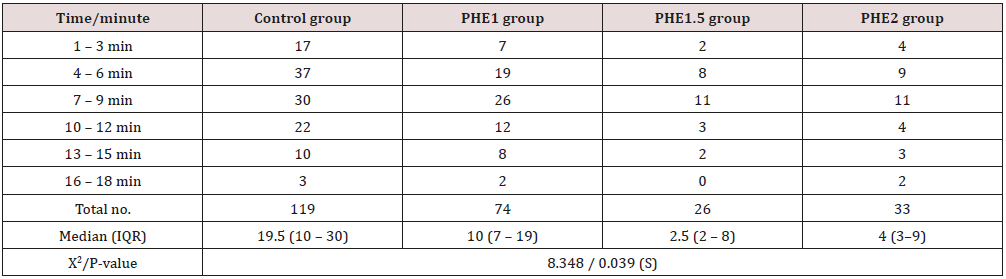
Data were presented as number of boluses used in each period and compared using median and inter-quartile range with Kruskall- Wallis test
Methodology
A randomized (using computer-generated random allocation) double blinded clinical; research trial conducted from January 2017 till January 2019, after approval of local ethical committee on the current research study and written informed consent was taken from all participant, conducted at Mohamed Saleh Bashrahil Hospital in Holy Makka, Saudi Arabia. Current clinical research study involved 184 cases that are classified as American Society of Anesthesiologists physical status I and II with term singleton pregnancies scheduled for elective cesarean section under spinal anesthesia randomized to 4 groups; receive 0.9% saline 2mL (Control Group) or Phenylephrine 1.0ug/kg (PHE1 research Group), 1.5ug/kg (PHE1.5 research Group), or 2.0ug/kg (PHE2 research Group) immediately after induction of spinal anesthesia. Maternal blood pressure and heart rate were recorded at 1min intervals until delivery. Hypotension, defined as systolic blood pressure <80% of baseline, was treated with rescue doses of Phenylephrine 100ug at 1min intervals until hypotension resolved. The incidence of nausea, vomiting, bradycardia, and hypertension, as well as Apgar scores and umbilical blood gases (GEM premier 3500, USA) were recorded. Exclusive research criteria involved the following pre-existing or pregnancy-induced hypertension, cardiac or respiratory disease, cerebrovascular disease, fetal anomalies or contraindications to spinal anesthesia. Cases among Control research Group were administered 0.9% saline 2mL, while cases among Phenylephrine research groups 1, 1.5, and 2 were administered Phenylephrine 1.0, 1.5, and 2.0ug/kg, consecutively, diluted in 2ml of saline .Before the induction of anesthesia, an 18gauge intravenous cannula was inserted. Typical monitoring devices was attached, involving non-invasive blood pressure, electrocardiogram, three lead ECG (Carestation monitor B650, GE healthcare, Helsinki, Finland), blood pressure and heart rate were measured at 1min intervals. Cases have been positioned in the left lateral decubitus position for the spinal procedure. After skin decontamination and injection of cutaneous local anesthetic, a 27G needle (Polymed spinal needle with Quincke type point, Brussels, Belgium) was inserted at the L3-4 or L4-5 interspace and the dura mater was punctured, After verifying free flow of cerebrospinal fluid, a mixture of 0.5% hyperbaric bupivacaine 11mg and fentanyl 15ug was administered over 10s.
Primary Research Outcome
Have been determination of the incidence of hypotension, defined as systolic blood pressure (SBP) <80% of baseline. Hypotension was managed using rescue doses of Phenylephrine 100ug every 1min till hypotension was resolved. The total rescue dosage of Phenylephrine that has been administered to each patient was recorded. Cases that have been experiencing bradycardia in conjunction to hypotension were administered atropine 0.5mg Apgar scores at 1 and 5min, estimated blood loss, and fluid administration till time of delivery were recorded (Figures 1-3).
Figure 1: Changes in systolic blood pressure in the four studied groups during time. aP <0.05 compared with the PHE1 group; bP <0.05 compared with the PHE1.5 group and cP <0.05 compared with the PHE2 group.
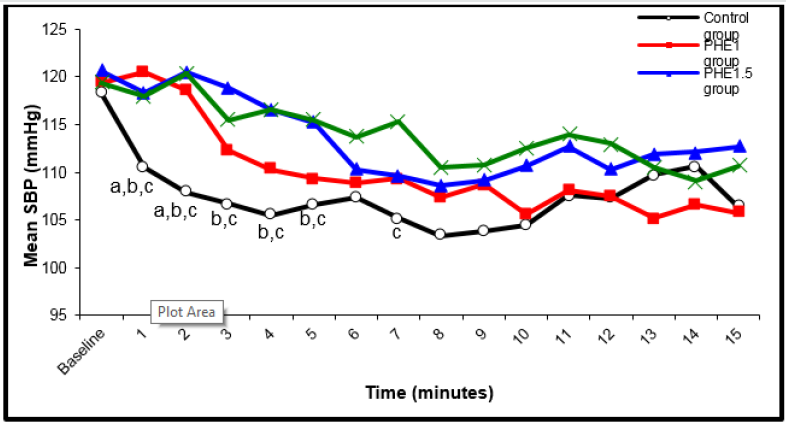
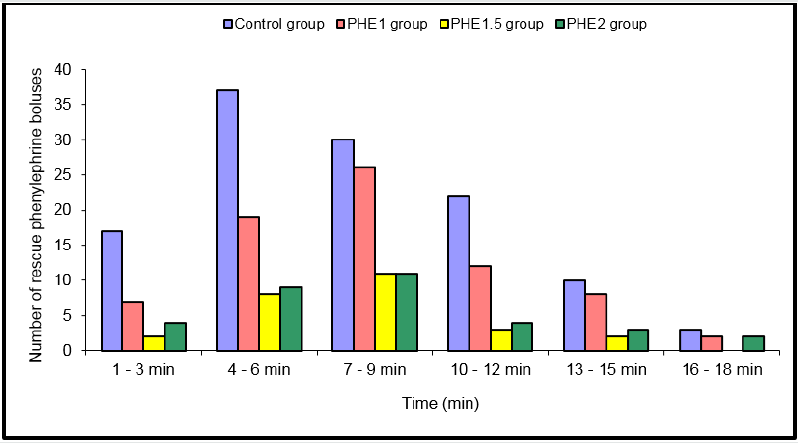
Figure 3: Display the number of rescue boluses that were administered over time among the four research groups.
Statistical Analysis
Data were collected, revised, coded and entered to the Statistical Package for Social Science (IBM SPSS) version 23. The distribution of quantitative data was tested by Kolmogorov- Smirnov test of normality. So, the quantitative data were presented as means, standard deviations and ranges when parametric and compared between groups using One Way ANOVA followed by post hoc analysis using LSD test while non-parametric were presented as medians with inter-quartile ranges (IQR) and compared between groups using Kruskall-Wallis test followed by post hoc analysis using Mann-Whitney test. Also, qualitative variables were presented as numbers and percentages and compared between groups using Chi-square test. The confidence interval was set to 95% and the margin of error accepted was set to 5%. So, the p-value was considered significant at the level of < 0.05.
Discussion
Administration of a Phenylephrine infusion can reduce the incidence and severity of hypotension and nausea during spinal anesthesia for cesarean delivery. However, good hemodynamic control may not be attained if the drug is administered as a prophylactic fixed rate infusion. A variable rate infusion adjusted based on changes in arterial blood pressure and heart rate may better maintain baseline blood pressure [10]. Over time, methods have changed for managing blood pressure (BP) changes during spinal anesthesia for cesarean delivery. Phenylephrine is now the preferred vasopressor for treating hypotension, but how it should be used is still debated. One method is the use of a prophylactic infusion after the block is placed [11]. A prior research study similar to the current study in approach and methodology have revealed and displayed among its findings that prophylactic administration of hypotension during conductance of spinal anesthetic mode for cesarean deliveries [1,3]. Furthermore it was shown by a prior research team of investigators the total additional dosages used for managing hypotensive issues in spinal anesthetic techniques in cesarean section of Phenylephrine agent was small among the investigated cases [2,5]. Another research team of investigators have shown among their study findings that the large Phenylephrine dosage of 2ug/kg is correlated and linked to higher rates of hypertension. Interestingly according to Phenylephrine dosages best suiting managing and preventing hypotensive attacks during spinal anesthesia conducted for cesarean delivery is administering a prophylactic Phenylephrine bolus of 1.5ug/kg [5,8]. A previous group of investigators have compared three dissimilar dosage protocols: continuous infusion (0.15ug/kg/min) versus prophylactic bolus (50ug) versus therapeutic bolus (50ug) it was revealed and displayed that the incidences of hypotension have been 17.5%, 32.5% and 85%, consecutively. Even though the best results have been observed among the continuous infusion research group, a 50ug prophylactic dosages was also efficient in preventing hypotensive attacks during spinal anesthesia for cesarean sections [4,7].
Conclusion and Recommendation for Future Research
The research findings obtained denote and imply that a prophylactic Phenylephrine 1.5ug/kg bolus followed by additional boluses when necessary could be an alternative management protocol to decrease the frequency of hypotensive issues occurrence during spinal anesthetic mode for cesarean deliveries. Future research efforts are recommended to consider racial and ethnic differences in conjunction to BMI differences.
References
- Cooper DW (2012) Cesarean delivery vasopressor management. Curr Opin Anaesthesiolgy 25: 300-308.
- Langesaeter E, Dyer RA (2011) Maternal hemodynamic changes during spinal anesthesia for Cesarean section. Curr Opin Anaesthesiol 24: 242- 248.
- Cooper D, Schofield L, Hynd R, Lloyd A, Meek T, et al. (2012) Prospective evaluation of systolic arterial pressure control with a Phenylephrine infusion regimen during spinal anesthesia for Cesarean section. Int J Obstet Anesth 21: 245-252.
- Siddik-Sayyid SM, Taha SK, Kanazi GE, Aouad MT (2014) a randomized controlled trial of variable rate Phenylephrine infusion with rescue Phenylephrine boluses versus rescue boluses alone on physician interventions during spinal anesthesia for elective cesarean delivery. Anesth Analg 118: 611-618.
- Doherty A, Ohashi Y, Downey K, Carvalho JC (2012) Phenylephrine infusion versus bolus regimens during cesarean delivery under spinal anesthesia: a double-blind randomized clinical trial to assess hemodynamic changes. Anesth Analg 115: 1343-1350.
- Ngan Kee WD (2014) Phenylephrine infusions for maintaining blood pressure during spinal anesthesia for cesarean delivery: finding the shoe that fits. Anesth Analg 118: 496-498.
- Ngan Kee WD, Lee SW, Ng FF, Tan PE, Khaw KS (2015) Randomized double-blinded comparison of norepinephrine and Phenylephrine for maintenance of blood pressure during spinal anesthesiafor cesarean delivery. Anesthesiology 122: 736-745.
- Onwochei D, Ngan Kee W, Fung L, Downey K, Ye X, et al. (2017) Norepinephrine to prevent hypotension during spinal anesthesia for cesarean delivery: a sequential allocation dose finding study. Anesth Analg 125: 212-218.
- Liu H, Huang Y, Diao M (2015) Determination of the 90% effective dose (ED90) of Phenylephrine for hypotension during elective cesarean delivery using a continual reassessment method. Eur J Obstet Gynecol Reprod Biol 194: 136-140.
- Medlej K, Kazzi AA, El Hajj Chehade A (2018) Complications from administration of vasopressors through peripheral venous catheters: an observational study. J Emerg Med 54: 47-53.
- Ngan Kee WD (2017) A random-allocation graded dose-response study of norepinephrine and Phenylephrine for treating hypotension during spinal anesthesia for cesarean delivery. Anesthesiology 127: 934-941.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...