Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2643-6760
Case Report(ISSN: 2643-6760) 
Otoplasty for Bilateral Bat Ear Deformity – A Case Report Volume 7 - Issue 1
Leena Sreekumar1, Thanzilahemed1, Surya Rao Venkata Mahipathy2*, Alagar Raja Durairaj2, Narayanamurthy Sundaramurthy2, Anand Prasath Jayachandiran3 and Suresh Rajendran3
- 1Postgraduate, Department of General surgery, Saveetha Medical College & Hospital, India
- 2Professor & Head, Department of Plastic & Reconstructive Surgery, Saveetha Medical College & Hospital, India
- 3Associate Professor, Department of Plastic & Reconstructive Surgery, Saveetha Medical College & Hospital, India
Received:August 11, 2022; Published:August 24, 2022
Corresponding author: Surya Rao Venkata Mahipathy, Professor & Head, Department of Plastic & Reconstructive Surgery, Saveetha Medical College & Hospital, Tamilnadu, India
DOI: 10.32474/SCSOAJ.2022.07.000253
Abstract
The incidence of the bat ear or prominent ear is 5% of the general population. There are no anatomic or physiologic abnormality among several cases, yet the social and psychological issues cause a significant difficulty and angst for the patients. A congregation of surgical procedures of the prominent ear has been described in the literature as far back as 1845 and is still a subject of exploration. We must tailor the procedure best suited for a particular patient and for this a thorough understanding of ear anatomy is one of the most essential steps in the preoperative management of an otoplasty candidate. Here, we present a patient with bilateral prominent ears who underwent a combination of Mustardé and Furnas’ procedures.
Keywords: Congenital; Prominent ear; Otoplasty; Complications
Introduction
The protruding ear is a trivial ear abnormality found in approx. 5% of the population and may give rise to serious emotional problems in children and also in adults [1]. Otoplasty is an amalgamation of procedures which includes incision, scoring and suture techniques. The severity of the ear abnormality and the individual characteristic of the auricular cartilage decides the choice of surgical procedure [2-6]. In children up to the age of ten years, a soft, elastic or easily pliable auricular cartilage is often still present. In this situation, gentle suture techniques, such as a suturing technique described by Mustardé, are frequently enough to achieve a cosmetically good and lasting result [7-10]. In adults, the auricular cartilage has already become stiff. Therefore, a combination of incision, scoring and suture techniques is usually required. Apart from reducing the cephaloauricular angle to 15- 20°, emphasis on the antihelical fold and a smooth rim of the helix without interruption of the contour are desirable outcomes of this operation. surgical fixation (lobulopexy) may be required to treat protruding lobules or, in rare cases, an additional conchal reduction may become necessary in cases of conchal hyperplasia. Since postoperative complications can often result in severe auricular deformities, as a matter of principle, each ear should be analysed individually regarding its problem areas, and the surgical approach that causes the least injury to the cartilage should be used.
Case Report
A 27 year old male patient came to our department with complaints of bilateral prominent ears since birth. There was no history of ear trauma, discharge, ear pain, hearing difficulty or previous surgery to the ear. He was born of parents of a non consanguineous marriage by full term normal vaginal delivery. His prenatal and postnatal period was uneventful. There was no history of radiation exposure or ingestion of teratogenic drugs in pregnancy. On examination, he had bilateral prominent ears with hypoplasia of antihelix with an incomplete antihelical fold. The cephaloauricular angle was increased with a flattening of the scapha and the fossa triangularis, and a ventral protrusion of the helix in the upper and middle third of the pinna with an enlarged and deep conchal bowl (Figures 1a, b, c).
Figure 1: Pre-operative photographs showing the bilateral prominent ears (frontal (a), left lateral (b) and right lateral (c) views).

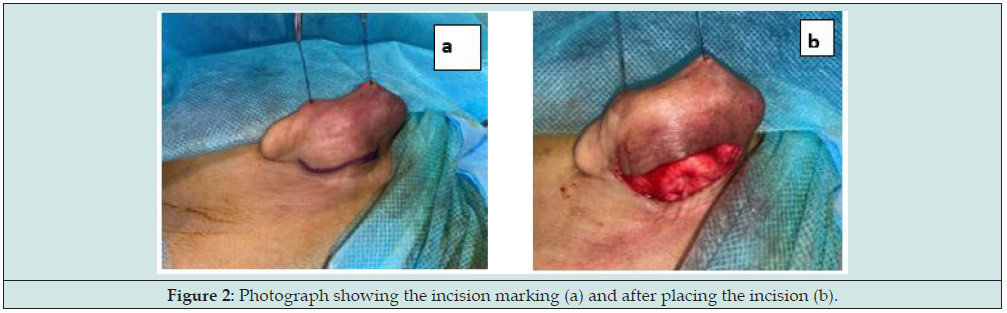
The patient was explained regarding the problems and the need for an otoplasty. Under general anaesthesia, a retroauricular sulcus incision was made and skin flaps were raised (Figures 2a & 2b). Five Mustardé scapho-conchal sutures were placed to augment the antihelix and triangular fossa. 2mm x 0.3mm conchal cartilage excision was done. Two Furnas concho-mastoid sutures were placed to narrow the cephaloauricular angle. The excess skin in the inferior third was excised to correct the lobule position. Skin closure was done after securing haemostasis. Similar procedure was done on the opposite side. Post-operative was uneventful with the patient being happy with the result at 1 month (Figures 3a, 3b) and at 6 months follow-up (Figures 4a, 4b).
Discussion
By the age of six years the development of the auricle regarding the transverse growth and the growth of the conchal depth is complete. Based on Weerda’s classification of the auricular deformities, grade 1 includes mild deformities of the auricle in which the anatomical structures of the auricular basic architecture are completely preserved like protruding ears, cryptotias, macrotias, colobomas, as well as mild cup ear deformities [11,12]. In grade 2 auricular deformities, moderate malformations of the basic architecture of the cartilage are already apparent including severe cup ear deformities and the mini-ear. In grade 3 or severe auricular deformities, only isolated remains of the cartilage or appendages without signs of normal auricular shape are apparent like microtia and anotia, which is the most extreme form of a severe auricular deformity where the auricle or the presence of an auricular basic architecture is completely missing. These deformities are predominantly unilateral and have a male preponderance.
Prominent ear anatomically signifies absence of antihelical folding, flat scapha and conchal hypertrophy. Prominent ear is defined as a conchoscaphal angle equal to or more than 90°, auriculocephalic angle greater than 30°, increasing of distances of height (normal 5-7 cm) and width (normally 50-60% of height) and increased helical rim distances from scalp (normally 10-12 mm superiorly, 16-18 mm at its middle and 20-22 at the lobule). The aims of prominent ear correction are defining the antihelix and decrease both the conchoscaphal angle and conchal hypertrophy. Many authors have suggested multiple criteria for a perfectly shaped auricle and the axis of the ear should be almost parallel to the bridge of the nose, the position of the auricle should be approx. One auricular length behind the lateral orbital margin (55-70 mm), the width of the auricle should be 50-60% of the auricular length (width: 30-45 mm, length 55-70 mm), the anterolateral angle should be 21-30 degree and the lobule should be parallel in position to the antihelical fold in the same plane.
McDowell’s Goals of Otoplasty mentioned that a) the emphasis should be placed on the correction of the upper third of the protruded ear. b) the helix should be visible behind the antihelix, when the patient is observed anteriorly c) the helix should have a smooth and continuous contour, not broken or sharp, d) the postauricular sulcus should not be distorted or markedly decreased in size, e) each part of the helix should be at an appropriate distance away from the mastoid skin. This is between 10 to 12 mm in the upper third, 16 to 18 mm in the middle third, and 20 to 22 mm in the lower third of the ear and f) at any point between the two ears, the position of the lateral ear border to the head should match within 3 mm of each other [13]. In protruding ears, deviations from the normal shape are especially apparent at the antihelix, the concha, the mastoid-helix angle, and the lobule. The enlargement of the helixmastoid angle is enough to cause a protrusion of the entire auricle, especially in the mid portion. This situation is sometimes referred to as pseudo-conchal hyperplasia Very frequently, hypoplasia of the antihelix associated with an incomplete or unformed antihelical fold is found in combination with an increased helix-mastoid angle. This results in a flattening of the scapha and the fossa triangularis, as well as in a ventral protrusion of the helix in the upper and/or middle region [14-16].
Numerous methods have been reported for its correction which poinst that the ideal technique is not yet available. The recent available methods can be divided into cartilage splitting (cutting) and non-cartilage splitting techniques (cartilage sparing). Non cartilage splitting techniques include cartilage molding only, skin excision, cartilage suturing, cartilage scoring and cartilage fixation or their combinations. Nevertheless these techniques give only momentary results, increased rates of recurrences and the likelihood of suture extrusion [17,18]. Cartilage cutting techniques were formerly started by Ely, 1881 who described a resection of skin and conchal cartilage followed by skin closure only. In 1910 Luckett devised a similar technique but he added horizontal mattress cartilagenous sutures for better definition of antihelix. Crikelair and Cosman (1964) performed skin excision, cartilage cutting and anterior scoring using a scalpel. Others executed two parallel cartilaginous incisions for designing cartilage tubing to create the antihelical folding. Also, these methods have the problem of creating a sharp antihelical fold, deep concha, prominent lobule and also have high recurrence rates as it occasionally did not address the cartilage tendency to recoil to its old shape. By 1963, Mustarde developed a technique to create the antihelical tubing using permanent conchoscaphal mattress sutures without excision of cartilage. in 1968, Furnas introduced a method in which retroauricular soft tissues, including posterior auricular muscle and ligament, were resected and attached by conchomastoid sutures [19,20].
Complications of otoplasty can be classified as early and late. Initial complications include haematomas, wound infections, perichondritis, pain, postoperative bleeding, allergic reactions, and cartilage-skin necroses. The delayed complications include, hypertrophic scars, keloids, suture material rejection with fistula formation, hypoesthesia or paraesthesia, auricular deformities or a recurrence. Periodic follow-up examinations and care are strongly recommended for the early detection of complications and should be performed by the surgeon [21-23].
Conclusion
Surgery to correct the prominent ear can be more complicated than it looks. Even in the hands of an experienced surgeon, delicate discussion, preoperative planning, and intra-operative decision all play a role in the outcome of the procedure. Otoplasty for the prominent ear can offer the patient substantial aesthetic and psychological relief. Only a handful of techniques were described that may benefit the patient with prominent ears but there are other techniques which will allow the surgeon to utilize the collection of corrective measures best fitted for each individual patient.
References
- Cihandide E, Kayiran O, Aydin EE, Uzunismail A (2016) A new approach for the correction of prominent ear deformity: the distally based perichondrio-adipo-dermal flap technique. J Craniofac Surg 27: 892-897.
- Gualdi A, Daniel JC, Gatti J, Wurzer P, Sljivich M (2018) Double triangular cartilage excision otoplasty. Plast Reconstr Surg 141: 348-356.
- Weerda H (1998) Classification of congenital deformities of the auricle. Facial Plast Surg 5: 385-388.
- JG Hoehn, Ashruf S (2005) Otoplasty: sequencing the operation for improved results. Plast Reconstr Surg 115(1): 5e-16e.
- Nazarian R, Eshraghi AA (2011) Otoplasty for the protruded ear. Semin Plast Surg 25: 288-293.
- Janz BA, Cole P, Hollier LH, Stal S (2009) Treatment of prominent and constricted ear anomalies. Plast Reconstr Surg 124(1, Suppl): 27e-37e.
- Valente ASC (2010) Separating the helix from the antihelix: a new concept in prominent ear correction. Aesthetic Surg J 30: 139-153.
- Cho BC, Chung HY, JW Park (2003) Surgical correction of prominent ear using modified tube technique and posterior approach. J Craniofac Surg 14: 767-773.
- Tolleth H (1978) Artistic anatomy, dimensions, and proportions of the external ear. Clin Plast Surg 5: 337-341.
- Tolleth H (1990) A hierarchy of values in the design and construction of the ear. Clin Plast Surg 17: 193-199.
- Bozkir MG, Karakas P, Yavuz M, Dere F (2006) Morphometry of the external ear in our adult population. Aesthetic Plast Surg 30: 81-85.
- Janis JE, Rohrich RJ, Gutowski KA (2005) Otoplasty. Plast Reconstr Surg 115(4): 60e-72e.
- McDowell AJ (1968) Goals in otoplasty for protruding ears. Plast Reconstr Surg 41(1): 17-27.
- Petersson RS, Friedman O (2008) Current trends in otoplasty. Curr Opin Otolaryngol Head Neck Surg 16: 352-358.
- Mustardé JC (1967) The treatment of prominent ears by buried mattress sutures: a ten-year survey. Plast Reconstr Surg 39: 382-386.
- Furnas DW (1968) Correction of prominent ears by conchomastoid sutures. Plast Reconstr Surg 42: 189-193.
- Ely E (1987) A classic reprint: An operation for prominence of the auricles (with two wood-cuts). By Edward T Ely 1881. Arch Otolaryngol 11: 73-74.
- Luckett WH (1910) A new operation for prominent ears based on the anatomy of the deformity. Surg Gynecol Obstet 10: 635-637.
- Crikelair GF, Cosman B (1964) Another solution for the condition of the prominent ear. Ann Surg 160: 314-324.
- Converse JM, Wood-Smith D (1963) Technical details in the surgical correction of lop ears. Plast Reconstr Surg 31: 118-128.
- Pitanguy I, Muller P, Piccolo N, Ramalho E, Solinas R (1987) The treatment of prominent ears: a 25-year survey of the island technique. Aesthetic Plast Surg 11: 87-93.
- Werdin F, Wolter M, Lampe H (2007) Pitanguy's otoplasty: report of 551 operations. Scand J Plast Re Constr Surg Hand Surg 41: 283-287.
- Mustarde JC (1963) The correction of prominent ears using simple mattress sutures. Br J Plast Surg 16: 170-178.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...