Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1768
Case ReportOpen Access
Neuroleptic Malignant Syndrome: An Undiagnosed Case Volume 2 - Issue 5
Haris Chaudhry1*, Cesar Figueroa2, Mohammad Alasker2, Saher Aslam3, Usama Nasir4 and Ibrar Anjum5
- 1Loma Linda University, Department of Surgery, USA
- 2University of California Irvine, Department of surgery, USA
- 3University at Buffalo, Catholic Health System, Department of Medicine, USA
- 4CMH Lahore Medical College and Institute of Dentistry, Department of Medicine, Pakistan
- 5The University of Texas MD Anderson Cancer Center, USA
Received: August 26, 2019; Published: September 04, 2019
Corresponding author: Haris Chaudhry, Loma Linda University, Department of Surgery Loma Linda, USA
DOI: 10.32474/SJPBS.2019.02.000147
Background
Neuroleptic malignant syndrome (NMS) was first described six decades ago after the introduction of neuroleptic drugs for the treatment of psychotic disorders [1]. NMS is an infrequent yet potentially fatal adverse effect of the neuroleptic class of antipsychotic medications. Signs of NMS include fever, muscular rigidity, altered mental status, elevation of creatine kinase (CK) with its incidence ranging between 0.07% to 0.2% [2-3]. NMS is possible with all neuroleptics. It can be easily recognized in its classic form but the lack of a specific diagnostic criteria along with its rare occurrence has limited further study in this field [4]. NMS is not generally considered dose-dependent and can occur within the therapeutic dose range of the antipsychotic drugs [5]. The frequency of NMS ranges from 0.07 to 2.2%. Its pathophysiology is not clearly understood but the blockade of dopamine receptors appears to be the central mechanism [6]
Objective
We present an atypical clinical presentation overlapping with dissociative symptoms, illustrating various problems linked to the diagnosis of NMS. Furthermore, differentiating dissociative symptoms from those of NMS and recognition of early signs and symptoms is of paramount importance for early recognition of NMS as a medical emergency to reduce morbidity and mortality.
Case Report
An 18-year-old female with a history of mental illness presents to her local physician with complaints of worsening insomnia for the last 3 days. She has a recent history of intermittent insomnia for the last three months. She was treated with long-acting haloperidol and was sent home. Two days later, the patient presents o the emergency department of a tertiary care hospital with intense lower back pain, jaw stiffness and fluctuating fever. Patient was stabilized, given antibiotics and baseline investigations were done including a CT scan; the patient was admitted to the medical ward. All of the results were within normal limits and any infectious pathology was ruled out. Patient was given analgesics (NSAIDs and Acetaminophen) for pain relief. On her 4th hospital day, she developed a new onset of non-epileptic, jerky, seizure-like episodes 4-5 times per day, each episode lasting 4-5 minutes followed by intense back pain, associated with headache and increased body stiffness. Patient was referred to the psychiatry ward to rule out dissociative symptoms; blood creatine phosphokinase (CPK) measured 1257mg/dl. After taking a careful history, examination and investigation, a provisional diagnosis of NMS with dissociative overlay was made and treatment was started accordingly. Patient was given bromocriptine, amantadine, lorazepam and fluoxetine. After one week of treatment her body stiffness improved but the patient still complained of left-sided back pain and headache. Individual psychotherapy sessions over the next 2 to 3 weeks resolved all of her remaining symptoms and patient was discharged on medication.
Discussion
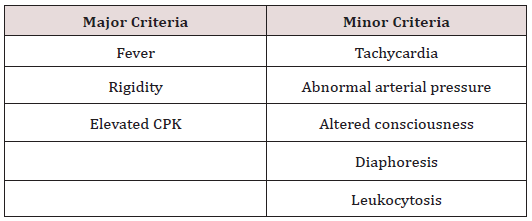
To date NMS has been diagnosis of exclusion. Levenson et al. [7] proposed a set of diagnostic criteria (Table 1) for NMS; major criteria of fever, rigidity, and elevated CPK and minor criteria of tachycardia, abnormal arterial pressure, tachypnea, altered consciousness, diaphoresis, and leukocytosis. The presence of three major criteria or two major and four minor criteria with a supportive clinical history would suggest a diagnosis of NMS. These diagnostic criteria have not seen universal adoption, though all three major criteria were present in our patient. The rarity of this adverse drug reaction (ADR) has resulted in less research in this field and hence most treatment has been based on case reports. Early diagnosis is crucial for the treatment of NMS as delay in diagnosis is associated with increased morbidity and mortality. Guerrera et al convened a multispecialty panel of 17 physicians to assign a priority score for various aspects of history, examination, and test results that add up to 100. To date, however, no total score has been tested or verified as diagnostic of NMS. Unfortunately, a lack of a universal diagnostic criteria as well as uncommon and atypical presentations often result in the delay in diagnosis and treatment. Four symptoms (muscle rigidity, hyperthermia, altered mental status, autonomic instability) and elevation of CK are considered diagnostic of NMS by most physicians. Atypical NMS, therefore, would be any presentation lacking 1 of these signs and symptoms. Atypical NMS can progress to typical NMS if the missing signs and symptoms appear in the patient at a later time [8]. In our case, the patient presented after two days of treatment with a long-acting high-potency antipsychotic with atypical symptoms. This patient had the four cardinal symptoms of a typical NMS presentation. However, jaw stiffness and lower back pain were the main presenting features of the patient in the ER and the lack of a detailed history and physical examination made it difficult for the physicians to consider NMS on the differential diagnosis. An article published by Oruch et al. also emphasized the overlapping presentation of NMS with other pathologies with similar clinical picture resulting in difficulties with diagnosis. These pathologies include serotonin syndrome, malignant hyperpyrexia, malignant catatonia and clozapine-induced hyperpyrexia among others [9].
The experience of the physician as well as the high suspicion of NMS can make the diagnosis possible in a timely manner. A study done by Margetic et al emphasized the importance of physician expertise noting that a detailed history and appropriate physical examination aid in the diagnosis. Non-expert physicians can easily misinterpret NMS as being symptoms of an untreated medical illness [10]. In our case, the atypical presentation along with a low suspicion of NMS by the physician led to the delay in diagnosis and treatment. As the definite diagnostic criteria is lacking due to the various clinical presentations, further studies should be conducted in this regard to find the most common atypical presentations along with a standard treatment plan for NMS. This case is the first of its kind presented in Pakistan and further research in this field would help lead to more appropriate diagnostic and management plans.
Conclusion
This case report highlights the difficulty of reaching a diagnosis in patients with overlapping dissociative symptoms and underlying mental illness who presenting with early signs and symptoms of neuroleptic malignant syndrome. A careful history is invaluable to reach a rapid diagnosis of NMS. Given the potentially deadly outcome of this condition, early diagnosis and treatment are necessary to prevent the associated morbidity and mortality of this ADR. The patient’s NMS and mental illness should be treated simultaneously with care to avoid further use of neuroleptic medications. Given the infrequent nature of this condition, this case report will be a valuable addition to the limited literature of NMS.
References
- Caroff SN (1980) The neuroleptic malignant syndrome. Journal of Clinical Psychiatry 41(3): 79-83.
- Gupta V, Magon R, Mishra BP (2003) Risk factors in neuroleptic malignant syndrome. Indian J Psychiatry 45(1): 30-35.
- Tse L, Barr AM, Scarapicchia V (2015) Neuroleptic Malignant Syndrome: A Review from a Clinically Oriented Perspective. Current Neuropharmacology 13(3): 395-406.
- Gurrera RJ, Caroff SN, Cohen A, Carroll BT, De Roos F, et al. (2011) An international consensus study of neuroleptic malignant syndrome diagnostic criteria using the Delphi method. Journal of Clin Psychiatry 72(9): 1222-1228.
- Langan J, Martin D, Shajahan P (2012) Antipsychotic dose escalation as a trigger for neuroleptic malignant syndrome (NMS): Literature review and case series report. BMC Psychiatry 12: 214.
- Mann SCCS, Fricchione G, Campbell EC (2000) Central dopamine hypoactivity and the pathogenesis of the neuroleptic malignant syndrome. Psychiatr Annals 30(5): 363-374.
- Levenson JL (1985) Neuroleptic malignant syndrome. American Journal of Psychiatry 142: 1137-1145.
- Schreiner NM, Windham S, Barker A (2017) Atypical Neuroleptic Malignant Syndrome: Diagnosis and Proposal for an Expanded Treatment Algorithm: A Case Report. A A Case Report 9(12): 339-343.
- Oruch R, Pryme IF, Engelsen BA (2017) Neuroleptic malignant syndrome: an easily overlooked neurologic emergency. Neuropsychiatry Disease Treatment 13: 161-175.
- Margetic B, Aukst Margetic B (2010) Neuroleptic malignant syndrome and its controversies. Pharmacoepidemiol Drug Safety 19(5): 429-435.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...