Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1709
Mini Review(ISSN: 2641-1709) 
“Ten” Differentials for this “Gen” like Mass at Nape of Neck Volume 7 - Issue 5
Sphoorthi Basavannaiah*
- Associate Professor, Department of ENT, Subbaiah Institute of Medical Sciences, India
Received: December 11, 2021; Published: January 05, 2022
Corresponding author: Sphoorthi Basavannaiah, Associate Professor, Department of ENT, Subbaiah Institute of Medical Sciences, India
DOI: 10.32474/SJO.2022.07.000274
Abstract
Neck swellings/masses are one of the most common encounters in the ENT outpatient department. As a known fact, fascial planes in the neck are dense and deep containing rich network of arterial, venous and nerve supply which bridges head with the rest of the body. Hence, it is important to assess any simple to complicated neck swellings which have a diverse origin as well as varied differential. It is crucial to remember that early and timely intervention of any neck swellings will lead to apt and prompt management. Here, is one such “GEN” like swelling over the nape of the neck which is (Gigantic, Erratic, Necrotic) encountered at the ENT outpatient department which was definitely one of a kind
Keywords: Neck swellings; necrotic; hyperpigmentation; differential
Introduction
Neck swellings are encountered at all ages with an extensive and exclusive differential diagnosis ranging from a congenital mass to a cancerous growth. It is hence significant that we surgeons have an in-depth knowledge about the root of its origin that is the embryology and anatomy of the swelling so as to aid a pertinent conclusion and provide applicable management algorithm.
Case Report
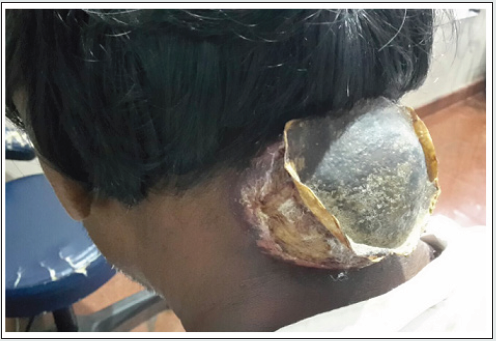
(Figure 1) Here, is this patient who consults the ENT outpatient
department on a regular basis with this huge swelling over the nape
of the neck since 6 months. The growth was initially small in size
(smaller than a lemon, now to have attained more than the size of
the orange roughly) about 2 years back but has begun increasing
in its size over a period of 6 months now. He also gives history of
foul-smelling discharge along with peeling of skin from over the
growth. There is pain on head and neck movements, heaviness
around the neck, disturbances while sleeping and difficulty in
taking shower. Patient has consulted at various places and tried his
hands at various modes of treatment, with no symptomatic relief
and barely satisfactory results. Patient ended up at this Tertiary
care hospital on somebody’s suggestion regarding good facilities
and treatment care available at this place. He also gives history of
compromised social and family life since the time of origin of this
swelling; making him feel lonely, depressed and abandoned. A
farmer by occupation who is with bare minimum financial build-up
has now got habituated to smoking and consuming alcohol. Patient
is a known case of both Hypertension and Diabetes (due to high
levels of stress) and is on treatment for the same, which is said to
be under control. His relatives have also mentioned on him taking
antidepressants and sedatives due to the depression he is with
off-lately. They have also mentioned hospital admissions several
times due to alcohol withdrawal symptoms (as he is having chronic
alcohol dependency). They have also hinted that he is having
suicidal tendencies and tried to commit suicide at few times.
On general physical examination, he is normal built and
nourished and oriented to time, place and person but showing signs
of being depressed in life and living. His vitals were stable. There
are hesitant marks on both of his forearm near the wrist. Systemic
examination was within normal limits. There were no positive
clinical findings on local examination of Ear, Nose and Throat. On
local examination of neck- 5X5 cm huge, irregular, necrotic, firm to
hard, foul-smelling mass over the nape of the neck, which was nontender,
adherent to the base while surface showing hyperpigmented,
peeling skin with irregular borders and margins. The swelling was
immobile in both horizontal and vertical directions and there was
no bleed on touch. There was no induration around the swelling
but with certain area of hyperpigmentation all around it. There was
bleeding seen when tried to peel off the superficial hyperpigmented
skin from over the swelling. There were no pulsations over and
around the swelling plus there was no engorgement of veins noted
over the swelling. Biopsy was planned under local examination. But,
when explained to the patient the possible next line of treatment is
based on the histo-pathological report, the patient was not willing
for the same as he wanted relief only through symptomatic line of
treatment. Following this OPD visit, the patient did not follow up.
But, looking at this swelling there are numerous differentials that
cross the mind which possibly could be the final diagnosis in this
case which have been discussed below.
Discussion
There are various swellings occupying the head and neck
region ranging from infective to neoplastic. As per this case report,
the top 10 most likely swellings at the nape of neck that can be
taken as probable differentials are elaborated below: Necrotising
fasciitis (NF) secondary varicella zoster infection, Acne Keloidalis
nuchae(AKN), Pyoderma gangrenosum(PG), Erysipelas, Gas
gangrene(GG), Calciphylaxis, Ecthyma gangrenosum(EG), Purpura
fulminans complicating varicella, Vibrio vulnificus(VV) infection,
Subcutaneous acute febrile neutrophilic dermatosis (subcutaneous
Sweet syndrome). Necrotizing fasciitis [1,2] is an infection that
spreads along fascial planes causing subcutaneous tissue death
characterized by rapid progression, systemic toxicity and even
death. It appears as red, hot, painful and swollen wound with an
ill-defined border. As the infective process continues, local pain
is replaced by numbness or analgesia. As the disease process
continues, skin initially becomes pale, mottled & purple and finally
gangrenous. It then moves rapidly along fascial planes and causes
tissue necrosis; secondary to its polymicrobial composition and
synergistic effect of enzymes produced by bacteria. Treatment
involves securing airway, broad-spectrum antimicrobials, intensive
care support and prompt surgical debridement. Reducing mortality
rests on early diagnosis and prompt aggressive treatment.
Acne Keloidalis nuchae [3-7] is a chronic inflammatory
condition that leads to scarring of hair follicles, development of
keloid-like papules and plaques, scarring alopecia on nape of
the neck and occipital scalp. The incidence is between 0.45- 9%,
occurring mostly in darker skinned races with curly or kinky hair.
It is most common in blacks and in Caucasians with M: F = 20:1
and starts after adolescence. The natural course of disease starts
with early formation of inflamed papules with marked erythema
[3]. Secondary infection can lead to pustules and abscess formation.
This continued inflammation leads to pronounced fibrosis and
keloid formation with coalescence of papules into plaques and
later nodules. The exact underlying pathogenesis is not known
but two predominant theories suggest skin injury and existence of
aberrant immune reactions. Skin injuries from irritation, occlusion,
trauma, friction and hair cutting practices are all risk factors. It has
been proposed that due to an immune reaction that can lead to
cicatrical alopecia [5,7]. On histology, there is mixed, neutrophilic,
lymphocytic infiltration. In this theory, intrafollicular antigens
attract inflammatory cells to the follicle resulting in damage to
sebaceous gland and follicular wall. This in turn leads to rupture
of follicle and release of antigens into hair follicle that precipitates
inflammatory process and epithelial destruction leading to fibrosis
[4]. Traditional management focuses on preventing disease
progression, avoidance of mechanical irritation from clothing and
use of antimicrobial cleansers to prevent secondary infection.
Treatment involves use of topical, intralesional or systemic steroids
in combination with retinoids and/or antibiotics to decrease
inflammation [7]. When disease progresses from early to late stage,
surgical excision and skin grafting may be performed which require
long periods of healing. Recent advances in light and laser therapies
[3] offer an alternative treatment option. This condition matches
the features of the patient in this study. Pyoderma gangrenosum
[8,9] is a serious, progressive, necrotising, ulcerative skin disorder
usually associated with underlying systemic diseases such as ulcerative colitis, arthritis, polycythemia vera. Head and neck
involvement is rare, but possibly more common. The etiology is
unclear but may be due to abnormal immunologic response [8].
There are no pathognomonic histologic or laboratory findings; the
diagnosis is made by the clinical appearance of lesions and disease
course. Many management regimens have been recommended,
but treatment must be individualized and must include concern
for the physical and psychologic needs of the patient [9]. This
particularly stressful and uncertain lesion is a challenge to both
surgeons and physicians. Treatment is usually non-surgical and
consists of immunosuppression and local wound care of ulcers in
addition to find underlying primary systemic disorder. Systemic
and intralesional steroids are the treatment of choice.
Erysipelas [10,11] is an infection of superficial layers of
skin. The most common cause is group A streptococcal bacteria,
especially Streptococcus pyogenes. Erysipelas results in a fiery
red rash with raised edges that can easily be distinguished from
the skin around it. The affected skin may be warm to touch. It
was thought to affect mostly face, but off-lately the distribution
of inflammation is changing where in legs are involved in 80%
of cases. The lesion is seen affecting adults between 60-80 years
of age also seen occurring in infants as well. The rash may also
appear on the arms or trunk. Erysipelas [10,11] begins at the site
of minor surgery or trauma: bruise, burn, wound, or incision or it
may be due to lymphatic obstruction. When rash appears on the
trunk, arms, or legs, it is usually at the site of a surgical incision
or a wound. It first appears as a localized lesion that is tender and
red with accompanying high fever, chills, headache, nausea and
malaise. The skin in the affected area resembles peel of an orange
[10]. The lesion quickly develops a bright red, shiny color with a
spreading, raised border. The typical lesion is so characteristic that
its presence is diagnostic. The treatment of choice is penicillin. For
the penicillin-allergic patient, erythromycin or cephalexin may be
used [11]. Gas gangrene [12,13] is a very rare but life-threatening
necrotizing soft tissue infection (NSTI) caused by anaerobic, sporeforming,
and gas-producing clostridium subspecies. It is the most
rapidly spreading and lethal infection in humans, also affecting
muscle tissue. The high mortality mediated by potent bacterial
exotoxins. Gas gangrene common in the extremities is a relatively
rare affliction of the head and neck [12]. The involvement of neck
spaces as a sequel to acute pharyngolaryngeal inflammation, dental
causes, trauma and unknown etiology. The causative organism is
Clostridium perfringens in 80–95% of cases. Gas gangrene can
rapidly progress to serious morbidity and even mortality, and
prompt surgical intervention is clearly indicated [13]. Management
of non-clostridial gas gangrene [12,13] of the neck is a challenge for
the surgeons which houses major vessels and vital structures and
in ensuring complete drainage and at times surgical debridement.
But recently recommended use of hyperbaric oxygen
therapy in tandem with antibiotics for soft tissue infections. Gas
gangrene [12,13] of the neck needs to be diagnosed quickly and
managed aggressively for desirable results to follow. However,
they warrant prompt recognition and immediate treatment
because of their potential risk of rapid spread to the deep neck
spaces, thrombophlebitis, mediastinitis and cardiac tampanode.
Calciphylaxis [14,15] is a serious, uncommon disease in which
calcium accumulates in small blood vessels of the fat and skin
tissues. It causes blood clots, painful skin ulcers and may cause
serious infections that can lead to death. The exact cause of
calciphylaxis is unknown, but recent studies have revealed that
most people with the condition have abnormalities in bloodclotting
factors. People with calciphylaxis have an imbalance in the
metabolism of calcium [14]. This causes calcium to be deposited
in the smallest parts of the arteries (arterioles), which eventually
leads to the formation of blood clots in the arterioles. Blood
clots can cause fat tissues and skin to be deprived of oxygen and
nourishment. Calciphylaxis most commonly affects people who
have end-stage kidney failure [15]. Possible risk factors include
female, Obesity, Diabetes, Abnormalities in blood-clotting factors,
Long-term dialysis and sometimes kidney transplantation, have
kidney failure and are on dialysis or have had a kidney transplant,
imbalance of calcium, phosphorus and aluminum in the body,
medications (warfarin, calcium-binding agents or corticosteroids),
Hyperparathyroidism, Uremia. Surgical approach for calciphylaxis
[14,15] can stimulate the sympathetic nerves and may cause the
formation of new ulcers. Therefore, surgery may worsen the
calciphylaxis prognosis, suggesting that surgical treatment should
be selected with caution after careful consideration of the risks
to the patient’s condition and general risks. Currently, treatment
for calciphylaxis [14,15] involves whole-body management,
including prevention of infection, correction of the abnormal
metabolism of calcium and phosphate, local management of ulcers
by debridement. In recent years, treatment with sodium thiosulfate
has been gaining attention. Cinacalcet acts directly on the calcium
receptors in the parathyroid cells and inhibits parathyroid hormone
without elevating blood serum calcium levels. It also lowers blood
serum phosphate levels.
Ecthyma gangrenosum [16,17] is a rare, invasive, cutaneous
lesion frequently associated with Pseudomonas aeruginosa,
although it may develop in the absence of bacteremia and may
originate from other bacterial and fungal organisms. It is most often
occurring in patients with neutropenia and immunocompromised
hosts. It typically occurs on the extremities, gluteal and perineal
regions. It can also occur in Head and Neck region also [16].
Tissue and blood cultures will be positive for P aeruginosa which
are diagnostic. This clinical entity should be considered when
otolaryngologists are asked to evaluate necrotic cutaneous lesions of
the head and neck. Treatment is usually broad spectrum antibiotics-
Amikacin. Considering high rate of mortality, early diagnosis and
prompt effective treatment is mandatory [17]. Purpura fulminans
[18,19] is a rare complication after a primary infection with
varicella zoster virus. A varicella infection may lead to protein C
or S deficiency resulting in diffuse intravascular coagulation and
severe skin defects. They usually occur after about 2 weeks after
chickenpox infection. They present with large painful ecchymotic,
necrotizing and retiform plaques on the lower extremities and also in the Head and neck region. Because of the rapidly progressing
purpura, patient presents with clinical signs of hypovolaemic shock
[18]. Laboratory analyses revealed very low protein S levels as
well as anticardiolipin antibodies. Aggressive treatment by lowmolecular-
weight heparin, steroids, intravenous immunoglobulins,
fresh frozen plasma, prednisolone, acyclovir and broad-spectrum
antibiotics- ceftriaxone was able to prevent the extension of the
lesions and to correct the coagulation abnormalities [19].
Vibrio vulnificus [20,21] infection is a rare and causes severe
illness including necrotising soft tissue infection, septicaemia,
gastroenteritis having high mortality. The risk factors include
immunocompromised state, diabetes and cirrhosis. Infection may
be contracted by consuming undercooked seafood or swimming in
contaminated sea water. V. vulnificus [20,21] is usually susceptible
to tetracyclines alone, but adding a cephalosporin is associated
with better therapeutic response. Tetracycline with or without
cephalosporin is usually sufficient to treat this potentially lethal
Gram-negative bacterium. Sweet’s syndrome [22] is uncommon
skin condition characterized by fever, neutrophilia, tender
erythematous, painful skin lesions that appears on the arms, face,
neck and diffuse infiltrate consisting mature neutrophils located
in the upper dermis. The cause of Sweet’s syndrome isn’t known,
but it’s sometimes triggered by an infection, illness or medication.
Sweet’s syndrome presents in three clinical settings: classical (or
idiopathic), malignancy-associated, and drug-induced. Classical
Sweet’s syndrome (CSS) [22] presents in women between 30
to 50 years of age, it is often preceded by an upper respiratory
tract infection and may be associated with inflammatory bowel
disease and pregnancy. 1/3rd with CSS experience recurrence
of dermatosis. Malignancy-associated Sweet’s syndrome (MASS)
[22] can occur as a paraneoplastic syndrome in patients with
established cancer or individuals whose Sweet’s syndrome-related
hematologic dyscrasia or solid tumor was previously undiscovered;
MASS is most commonly related to acute myelogenous leukemia.
The dermatosis can precede, follow, or appear concurrent
with the diagnosis of the patient’s cancer. Hence, MASS can be the
cutaneous harbinger of either an undiagnosed visceral malignancy
in a previously cancer-free individual or an unsuspected cancer
recurrence in an oncology patient. Drug-induced Sweet’s
syndrome (DISS) [22] occurs in patients who have been treated
with granulocyte-colony stimulating factor. The pathogenesis
of Sweet’s syndrome may be multifactorial and still remains
definitively established. Clinical and laboratory evidence suggests
that cytokines have an etiologic role. Systemic corticosteroids are
the therapeutic gold standard for Sweet’s syndrome. After initiation
of treatment with systemic corticosteroids, there is improvement of
dermatosis-related symptoms and skin lesions. Topical application
of high potency corticosteroids or intralesional corticosteroids
may be efficacious for treating localized lesions. Other first-line
oral systemic agents are potassium iodide and colchicine. Secondline
oral systemic agents include indomethacin, clofazimine,
cyclosporine and dapsone. The symptoms and lesions of Sweet’s
syndrome [22] may resolve spontaneously without any therapeutic
intervention; however, recurrence may follow either spontaneous
remission or therapy-induced clinical resolution.
Conclusion
Neck masses can be dicey and dubious. Each type of neck swelling has a unique location in the neck pertaining to its embryological origin. There must be one line that should be bored in the minds is that “not all neck masses are metastatic” and “not all neck swellings are carcinogenic”. Neck swellings can sometimes have a multidisciplinary approach through Otorhinolaryngologists, Surgeons, Dermatologists, as clinical presentation of them are too vast and vague. There are a variety of fancy names associated with these neck masses making their diagnosis and treatment both massive and elusive. There can be a rarest of the neck swelling to commonest of the neck mass both appearing intricate and elaborate making the management of these masses in the neck picky and finicky.
References
- Moon-Gi Choi MG (2015) Necrotizing fasciitis of the head and neck: a case report. Korean Assoc Oral Maxillofac Surg 41: 90-96.
- Ord R, Coletti D (2009) Cervico-facial necrotizing fasciitis. Oral Dis 15: 133-141.
- Maranda EL, Simmons BJ, Nguyen AH (2016) Treatment of Acne Keloidalis Nuchae: A Systematic Review of the Literature. Dermatol Ther (Heidelb) 6: 363–378.
- Verma SB, Wollina U (2010) Acne keloidalis nuchae: another cutaneous symptom of metabolic syndrome, truncal obesity, and impending/overt diabetes mellitus? Am J Clin Dermatol 11(6): 433–436.
- Salami T, Omeife H, Samuel S (2007) Prevalence of acne keloidalis nuchae in Nigerians. Int J Dermatol 46(5): 482–484.
- Adegbidi H, Atadokpede F, do Ango-Padonou F (2005) Keloid acne of the neck: epidemiological studies over 10 years. Int J Dermatol 44(Suppl 1): 49–50.
- Sperling LC, Homoky C, Pratt L (2000) Acne keloidalis is a form of primary scarring alopecia. Arch Dermatol 136(4): 479–84.
- Yco MS, Warnock GR, Cruickshank JC (1988) Pyoderma gangrenosum involving the head and neck. Laryngoscope 98(7): 765-768.
- Schwarz MB, Petroff MA, Anonsen CK (1987) Pyoderma gangrenosum of the head and neck. Laryngoscope 97(7 Pt 1): 806-809.
- Bonnetblanc JM, Bedane C (2003) Erysipela: recognition and management. Am J Clin Dermatol 4: 157-163.
- Stulberg DL, Penrod MA, Blatny RA (2002) Common bacterial skin infections. Am Fam Physician 66: 119-124.
- Vaidya S, Natarajan S, Ahuja SA (2017) Gas Gangrene in the Neck Caused by an Odontogenic Infection- A Case Report. J Surg 129(6): 1-3.
- Ohi K, Inamura N, Suzuki M (1993) Three patients with gas gangrene of the head and neck. Nihon Jibiinkoka Gakkai Kaiho 96: 1079-1085.
- Miura S, Takahashi K, Akasaka T (2017) Calciphylaxis Presenting with various symptoms: A Case Report. Case Rep Dermatol 9: 25–29.
- Nigwekar SU, Kroshinsky D, Nazarian RM (2015) Calciphylaxis: risk factors, diagnosis, and treatment. Am J Kidney Dis 66: 133–146.
- Singh TN, Devi KM, Devi KS (2005) Ecthyma gangrenosum: a rare cutaneous manifestation caused by pseudomonas aeruginosa without bacteraemia in a leukaemic patient--a case report. Indian J Med Microbiol 23(4): 262-263.
- Solowski NL, Yao FB, Agarwal A (2004) Ecthyma gangrenosum: a rare cutaneous manifestation of potentially fatal disease. Ann Otol Rhinol Laryngol 113(6): 462-464.
- Laarman AR, Schoor vdSR, Verhoeven BH (2008) Purpura fulminans: a rare complication of chickenpox. Ned Tijdschr Geneeskd 152(46): 2526-2529.
- Campanelli A, Kaya G, Ayse Hulya Ozsahin AH (2004) Purpura fulminans in a child as a complication of chickenpox infection. Dermatology 208(3): 262-264.
- Alsaad AA, Sotello D, Kruse BT (2017) Vibrio vulnificus tonsillitis after swimming in the Gulf of Mexico. BMJ Case Rep.
- Yu W, Shen X, Pan H (2017) Clinical features and treatment of patients with Vibrio vulnificus infection. Int J Infect Dis 59: 1–6.
- Cohen PR (2007) Sweet's syndrome: a comprehensive review of an acute febrile neutrophilic dermatosis. Orphanet Journal of Rare Diseases 2(34): 1-28.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...