
Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1709
Mini Review(ISSN: 2641-1709) 
How to Prevent Nasal Obstruction After Rhino Septoplasty. Could A Routine Turbinate Reduction Improve the Outcomes in Quality of Life of Patients? Volume 4 - Issue 1
Bianca H de Moura*
- Department of Otolaryngology and Head and Neck Surgery, Hospital de Clinicals de Porto Alegre (HCPA), Brazil
Received: February 08, 2020; Published:February 19, 2020
Corresponding author: Bianca H de Moura, Department of Otolaryngology and Head and Neck Surgery, Universidade Federal do Rio Grande do Sul, Hospital de Clinicals de Porto Alegre (HCPA), Brazil
DOI: 10.32474/SJO.2020.04.000176
Abstract
The Objective of this article is to Review current literature about performing a turbinectomy associated with Rhinoseptoplasty. Three clinical trials with level one of evidence about the issue have been published recently. All of them selected patients with nasal obstruction who were submitted to Rhinoseptoplasty. The NOSE scale to measure quality of life in these patients was used. Other tools of objective measurement as Acoustic rhinometry and rhinomanometry or subjective scales, Snot-20 WHOQOl and ROE were also explored. Each study used a different technique for turbinate reduction. All of the three found the same results discussed below. To review the scientific evidences of these articles can bring new outlook about this controversial topic.
Abbreviations: QOL: Quality of Life; NOSE: Nasal Obstruction Symptom Evaluation; ROE: Rhinoplasty Outcome Evaluation
Mini- Review
Rhinoplasty is often performed to restore nasal function and
form. The development or maintenance of nasal obstruction after
rhinoplasty is a complication that negatively affects quality of
life (QOL), and priority should be given to prevention strategies
[1]. However, the available surgical techniques to prevent this
obstruction have been empirically developed and are often
used based on the surgeon’s preference rather than on objective
criteria. Currently, strategies like spreaders grafts, support grafts,
reconstruction or repositioning cartilages and even a good
septoplasty are used to enlarge the nasal valve [2-6]. Another
technique widely used is the Reduction of the inferior turbinate
[3,7-9]. Otherwise, an established technique to reduce turbinate
with hypertrophy is still debatable [10-13]. Reviews pointed
that research in this field appears to be driven by technological
advancement rather than by establishment of patientsʹ benefit.
Partly, because of the lack of properly conducted randomized
controlled trial with long term results. Some articles even question
the efficacy of this procedure in cases of nasal obstruction explained
for other reasons rather than turbinate hypertrophy isolated [14].
A Recent clinical trial reveal that the association of turbinectomy
with septoplasty, though widespread, does not improve the nasal
obstruction clinical outcomes and can add risks to patients [15].
Therewithal an objective standardized tool that links anatomy
measures with clinical results is not available yet [16]. To address
this issue, Stewart et al. have developed and validated the Nasal
Obstruction Symptom Evaluation (NOSE) scale, a disease specific
QOL instrument designed to determine the presence of nasal
obstruction [17]. Since then, several studies have compared
preoperative versus postoperative NOSE scores to assess QOL
associated with nasal obstruction. A recent survey by the American
Society of Plastic Surgeons shows that 90% of surgeons address
the inferior turbinate in at least a portion of their cases, with 8%
routinely reducing the turbinate in all cases. However, 10% of the
respondents in this survey did not address the inferior turbinate
in any of their cases [18]. Such variability in addressing this
potential cause of/risk factor for nasal obstruction deserves closer
attention. Guyuron [19] has pointed out that the position of the
inferior turbinates contributes to airway narrowing after nasal
bone osteotomy. On account of that, surgical treatment of inferior
turbinates seems to be a good option to avoid postoperative nasal
obstruction, which would be great because of the accessibility,
simple technique and relative low risks. Unfortunately, all three
latest trials could not prove any improvement in QOL when the
turbinate reduction is associated even by using different techniques. Furthermore, to access the turbinate does not seem to improve the
rates of nasal obstruction and satisfaction with respiratory scales
outcomes [20-22].
In 2013, Lavinsky-Wolff et al. [20] compared QOL in patients
undergoing primary Rhinoseptoplasty, with or without turbinate
reduction by submucosal electrocautery. There was no difference
between subjects submitted or not to inferior turbinate reduction
in NOSE score (-75% vs. -73%; P = 0.893); all WHOQOL-bref score
domains (P > 0.05), NO-VAS (-88% vs. -81%; P = 0.89) and acoustic
rhinometry recordings (P > 0.05). Besides the literature does
not show difference between the techniques, this study receives
some critique about the conservative reduction by submucosal
electrocautery chosen. In order to answer this question de Moura
et al. [21], in 2017, randomized other 50 patients undergoing
primary Rhinoseptoplasty associated with inferior turbinate
reduction through endoscopic partial inferior turbinectomy (EPIT)
reduction or not. There was no difference between the groups
in absolute score changes for NOSE (-50.5 vs. -47.6; P = 0.723),
Rhinoplasty Outcome Evaluation (ROE) (47 vs. 44.8; P=0.742),
and all (WHOQOL-bref) score domains (P >0.05) (Table 1). There
were no differences between the groups regarding presence
of the complications. Surgical duration was higher in the EPIT
group (212 minutes ±7.8 vs. 159.1±5.6; P > 0.001). Both articles
do not present any improvement at short-term outcomes (three
months). Nevertheless, a long-term result was needed to reinforce
these findings. Wherefore this year Sommer et al. [22] published
a clinical Trial with nine months follow up. They randomized
patients to perform anterior turbinoplasty or not during septo- or
Rhinoseptoplasty.
Table 1: Source de Moura et al. [21].
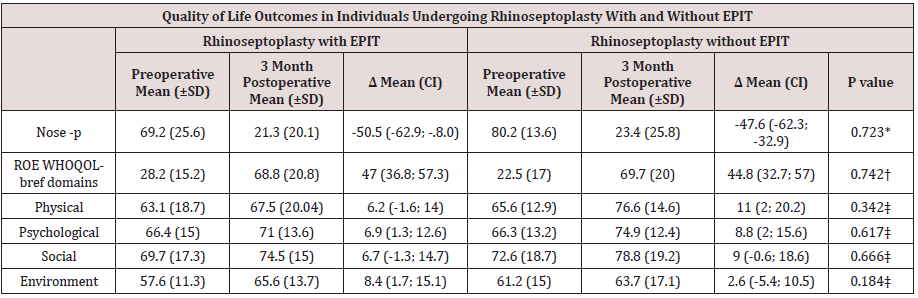
Dependent variable Δ scores = (postoperative score-preoperative score)
*P Value: ANCOVA of Δ adjusted for baseline NOSE -p value, nasal itching, rhinorrhea and use of spreader graft.
†P Value: ANCOVA of Δ adjusted for baseline ROE score, nasal itching, rhinorrhea and use of spreader graft.
*P Value: ANCOVA of Δ adjusted for baseline WHOQOL -bref score, nasal itching, rhinorrhea and use of spreader graft.
ANCOVA: analysis of covariance; CI: Confidence Interval; EPIT: Endoscopic Partial Inferior Turbinectomy; NOSE-p: Nasal
Obstruction Symptom Evaluation Portuguese; ROE: Rhinoplasty Outcome Evaluation; SD: Standard Deviation; WHOQOL-bref:
World Health Organization Quality of Life Scale
The results enhanced previous trials. Patient satisfaction after functional septo- and septorhinoplasty is high and does not seem to be affected by turbinate surgery. There was no statistically significant difference in the postoperative results regarding objective rhinological measurements with or without turbinoplasty (Table 2). They concluded that extensive resections of the turbinates can have a negative impact on nasal physiology, so the indication for turbinoplasty must be carefully considered. Considering these results, clearly has no reason to proceed a turbinate reduction, at least as routine, to patients submitted at rhinoplasty. As medical science is not so hard, presumably some phenotypes of noses probably could benefit of it. Although these patients are not identified, at least it can be justifying by other reasons, this turbinate access should be avoided. This finding changes the focus of discussion to which method should be used to reduce the turbinate to there are another surgical strategy that could be used to improve our functional results and which technique is it. Be like these finds fortify positively the discussion about structured Rhinoplasty and the importance of the reconstruction and reinforce of the nasal valve.
Conclusion
The indications for the reduction of the turbinate were well established in context of a turbinate inferior hypertrophy [23,24]. The studies have not shown, until now, a superior technique for the inferior reduction. Although techniques which preserve mucosa and have partial resection instead of total resection are indicated [10-12]. Trends in Rhinoplasty research do not show relevant benefits at patients’ quality of life outcomes associated with nasal obstruction when Rhinoplasty is performed combined with reduction turbinate. More clinical trial must be develop comparing other methods of enlargement and preservation of nasal valve and objective measurement instruments need to be developed to clarify these findings [25] (Table 3).
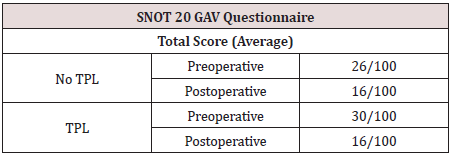
Table 3: Pre-and Postoperative values of the SNOT 20 GAV questionnaire within the groups (TPL vs. No TPL).
References
- Christophel JJ, Park SS (2009) Complications in Rhinoplasty. Facial Plastic Surgery Clinics of North America 17: 145-156.
- Constantian MB, Clardy RB (1996) The relative importance of septal and nasal valvular surgery in correcting airway obstruction in primary and secondary rhinoplasty. PlastReconstr Surg 98(1):38-54.
- Becker DG, Ransom E, Guy C, Bloom J (2010) Surgical Treatment of Nasal Obstruction in Rhinoplasty. Aesthetic Surg J 30(3):347-378.
- Wulkan M (2012) Comparative study in cadavers of the use of septal and costal cartilaginous grafts to increase the external sectional area of the thesis presented to the Faculty of Medicine of the University of São Paulo to obtain the title of Doctor in. PhD thesis, Brazil.
- Tasca I, CeroniCompadretti G, Sorace F (2013) Nasal valve surgery. Acta Otorhinolaryngol Ital 33(3):196-201.
- Surowitz JB, Most SP (2013) Complications of Rhinoplasty. Facial Plast Surg Clin NA21(4):639-651.
- Batra PS, Seiden AM, Smith TL (2009) Surgical management of adult inferior turbinate hypertrophy: a systematic review of the evidence. Laryngoscope119(9):1819-1827.
- Leong SC, Eccles R (2010)Inferior turbinate surgery and nasal airflow: evidence-based management. CurrOpinOtolaryngol Head Neck Surg 18(1):54-59.
- Omranifard M, Adib M, Ebrahimpour S (2019) Comparative Study of the Effectiveness of sub mucosal Partial Inferior Turbinectomy and Out fracture of Inferior Turbinate in the Nasal Respiratory Function of Rhinoplasty Patients. Aesthetic Plast Surg 43(5): 1281-1285.
- Passali D, Passali F, Passali G, Damiani V, Belussi L (2003) Treatmeant of Inferior Turbinate Hypertrophy: A randomized Clinical Trial. Ann OtolRhinolLaryngol112(8):683-688.
- Stölzel K, Bandelier M, Szczepek AJ, Dommerich S (2017) Effects of surgical treatment of hypertrophic turbinates on the nasal obstruction and the quality of life. Am J Otolaryngol 38(6):668-672.
- Veit JA, Nordmann M, Dietz B, Sommer F, Rotter N, Greve J, et al. (2016) Three Different Turbinoplasty Techniques Combined with Septoplasty : Prospective Randomized Trial. Laryngoscope 127(2):303-308.
- Rodrigues MM, Dibbern RS, Oliveira LF De, Dirce M, Marques O, Bella MF, et al. (2011) Comparison between turbinoplasty and endoscopic turbinectomy : Efficacy and clinical parameters Comparação entre turbinoplastia e turbinectomiaendoscópicas : Eficácia e parâmetrosclí Arq Int Otorrinolaringolpp. 426-430.
- Clement WA, White PS (2001) Trends in turbinate surgery literature: a 35-year review. Clin Otolaryngol Allied Sci 26(2):124-128.
- Egmond MMHT Van, Rovers MM, Hannink G, Hendriks CTM, Heerbeek N Van (2019) Septoplasty with or without concurrent turbinate surgery versus non-surgical management for nasal obstruction in adults with a deviated septum : a pragmatic, randomised controlled trial. Lancet 6736(19):1-8.
- Rhee JS, Poetker DM, Smith TL, Bustillo A, Burzynski M, et al. (2005) Nasal valve surgery improves disease-specific quality of life. Laryngoscope 115(3):437-440.
- Stewart MG, WitsellDL, Smith TL(2004) Development and validation of the Nasal Obstruction Symptom Evaluation (NOSE) Scale. Otolaryngology- Head and Neck Surgery 130(2): 157-163.
- Afifi AM, Kempton SJ, Gordon CR, Pryor L, Khalil AA., et al. (2015) Evaluating Current Functional Airway Surgery During Rhinoplasty: A Survey of the American Society of Plastic Surgeons. Aesthetic Plast Surg 39(2):181-190.
- Guyuron B (1998) Nasal osteotomy and airway changes. PlastReconstr Surg 102(3):856-860.
- Lavinsky M, Camargo HL, Barone CR, Rabaioli L, Wolff FH, et al. (2013) Effect of turbinate surgery in rhinoseptoplasty on quality-of-life and acoustic rhinometry outcomes: A randomized clinical trial. Laryngoscope123(1):82-89.
- Moura BH De, Migliavacca RO, Lima RK, Brauwers E (2017) Partial Inferior Turbinectomy in Rhinoseptoplasty Has No Effect in Quality-of-Life Outcomes : A Randomized Clinical Trial. Laryngoscope 128(1):57-63.
- Sommer F, Scheithauer MO, Hoffmann TK, Grossi A, Hauck K, Lindemann J (2019) Value of turbinoplasty in rhinosurgery - a controlled randomized study. Rhinology 57(5):352-357.
- Han JK, Stringer SP, Rosenfeld RM, Archer SM, Baker DP, et al. (2015) Clinical Consensus Statement: Septoplasty with or without Inferior Turbinate Reduction. Otolaryngol Head Neck Surg 153(5):708-720.
- Karlsson TR, Shakeel M, Supriya M, Ram B, AhSee KW (2015) Septoplasty with concomitant inferior turbinate reduction reduces the need for revision procedure. Rhinology53(1):59-65.
- Burgos MA, Sevilla A, Rojas S, Pino C Del, Velez F, Piqueras F, et al. (2018) Virtual Surgery for Patients with Nasal Obstruction : Use of Computational Fluid Dynamics ( MeComLand , Digbody&Noseland ) to Document Objective Flow Parameters and Optimise Surgical Results. Acta Otorrinolaringol 69(3):125-133.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...




