Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1709
Research Article(ISSN: 2690-5752) 
Foreign Pharyngoesophagial Bodies of Children: Epidemiological and Diagnostic Profile at The Omar Bongo Ondimba Army Training Hospital Volume 10 - Issue 4
Miloundja J1,2*, Lekassa P1,2, Manfoumbi Manfoumbi KD1, Manfoumbi Ngoma AB1, and Nzouba L1,2
- 1ENT and CFS Department, Omar Bongo Ondimba Army Instruction Hospital, Libreville, Gabon.
- 2Department of Surgery and Surgical Specialties, University of Health Sciences, Owendo, Gabon.
Received: January 18, 2023; Published: February 05, 2024
Corresponding author: Miloundja J, Department of Surgery and Surgical Specialties, University of Health Sciences, ENT and CFS Department, Omar Bongo Ondimba Army Instruction Hospital, Libreville, Gabon.
DOI: 10.32474/JAAS.2024.10.000341
Abstract
Introduction:b> The ingestion of foreign bodies is a frequent reason for consultation with an ENT specialist. It is often accidental in children.
Objective:b> to study the epidemiological and diagnostic profile of pharyngo-esophageal foreign bodies in children in our context.
Patients and method: This was a retrospective and descriptive study conducted in the ENT and CFS department of HIAOBO involving 213 medical records of patients under 16 years of age hospitalized for ingestion of EC from January 2012 to December 2022 (11 years old).
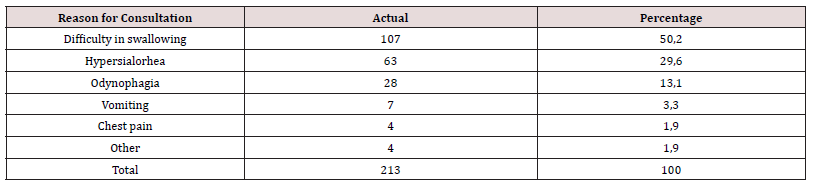
Results: There were 213 patients including 116 boys (54.5%) and 97 girls (45.5%), i.e. a sex ratio of 1.2. The median age was 4 years, with extremes of 8 months and 15 years. Children under 6 years of age accounted for 169 cases (79.4%). The place of residence was Libreville in 192 cases (90.1%). Ingestion was accidental in 206 cases (96.7%). The reason for consultation was dysphagia in 98 cases (46%), hyper sialorrhea in 61 cases (28.7%) and odynophagia in 43 cases (20.2%). The mean time to consultation was 27.46 hours with extremes of 1 hour and 1464 hours. Physical signs were salivary stasis in 174 cases (81.7%), fishbone in 2 cases (0.9%). Examination was normal in 37 cases (17.4%). Cervico-thoracic X-ray performed in 211 cases showed opacity in 209 cases (99%).
Conclusion: Pharyngo-esophageal foreign bodies are common in children. Their ingestion is accidental and can lead to serious complications. Physical examination and X-rays contribute to the diagnosis.
Keywords: CE pharyngo-esophageal; child; radiography; complications
Introduction
Ingestion of a foreign body (FB) is a common household accident in children. Its incidence cannot be properly estimated be cause many children swallow objects without the ingestion being known [1]. This ingestion most often occurs accidentally during games or meals regardless of the age of the child, with a greater incidence in those aged 6 months to 4 years [2, 3]. The frequency increases from the age of 6 months as soon as manual gripping are possible, with a peak between 6 months and 3 years estimated at 70% [4]. Ingestion of EC can be asymptomatic or result in neck or retrosternal pain, odynophagia, dysphagia, food refusal, hyper sialorrhea, vomiting, coughing, or respiratory distress, when it gets stuck in the esophagus [1]. Prolonged blockage can cause complications such as ulcerations that can lead to perforation or esophageal stenosis. Pharyngeal localization can lead to serious cellulitis-like complications and be life-threatening [5, 6]. Cervicothoracic X-rays are performed routinely [6]. Coins represent the most common EC in children [1]. In Gabon, no study on pharyngo-esophageal EC in children has been carried out, hence the interest of this work. The objective of this study was to describe the epidemiological and diagnostic profile of pharyngoesophageal foreign bodies in children in our context.
Patients and Method
This is a retrospective study with descriptive intent conducted in the ENT and Head and Neck Surgery department of the Omar Bongo Ondimba Army Training Hospital (HIAOBO). She carried medical records of patients under the age of 16 hospitalized for ingestion of EC from January 2012 to December 2022. Records of patients aged 1 to 15 years who were hospitalized for foreign body ingestion were included and were not retained, as the records of patients seen on an outpatient basis did not require extraction in the operating room. Data was collected from the hospitalization registry and collected on a standardized survey sheet. The parameters studied were age, sex, time of consultation, origin, circumstances of occurrence, call signs, nature of the foreign body, location of the CE, paraclinical signs. Data entry and analysis were performed using Epi Info7 software.2.30; SPSS 23 and R 4.2.1 and Excel 2013. The agreements of the director of the HIAOBO, the head of the ENT department and the parents have been obtained. The anonymity and dignity of the patients were respected.
Results
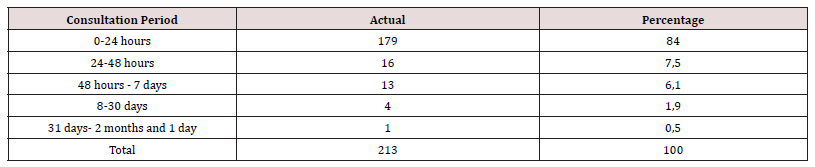
Over a period of 11 years, 213 records of children under 16 years of age with pharyngeal esophageal EC were collected. There were 116 boys (54.5%) and 97 girls (45.5%), a sex ratio of 1.2. The median age was 4 years, with the extremes of 8 months and 15 years. Children under 6 years of age accounted for 169 cases (79.4%). The place of residence was Libreville in 192 cases (90.1%), the province in 10 cases and Yaoundé in Cameroon in 1 case. Ingestion was accidental during gambling in 206 cases (96.7%) and during meals in 7 cases (3.3%). The reason for consultation was dysphagia with difficulty in swallowing in 98 cases (46%) and hyper sialorrhea in 61 cases (28.7%) and odynophagia in 43 cases (20.2%) (Table I). The mean time to consultation was 27.46 h with the extremes of 1 and 1464 hours (2 months and 1 day). This 2-month delay concerned a child evacuated from the provinces for the treatment of an esophageal foreign body discovered on an X-ray carried out following repeated lung infections with a chronic cough. Post-ingestion consultation was carried out within the first 24 hours in 179 cases (84%), between 24 and 48 hours in 16 cases (7.5%), between 48 hours and 7 days in 13 cases (6.1%) (Table II). The physical signs observed were salivary stasis in 174 cases (81.7%) and fishbone in the amygdala in 2 cases (0.9%). Examination was normal in 37 cases (17.4%).
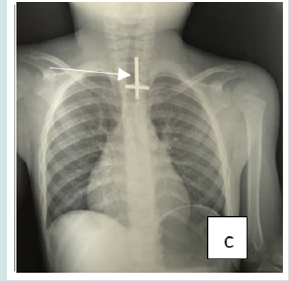
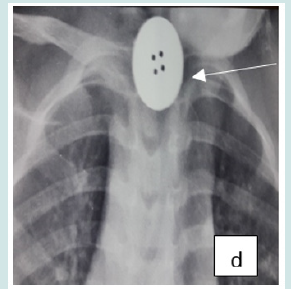
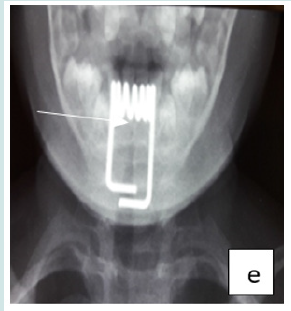
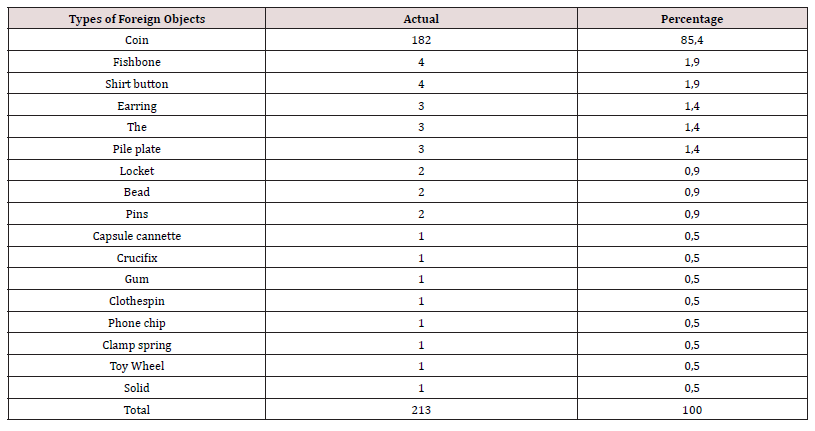
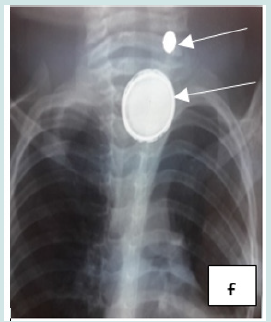
Cervico-thoracic X-ray performed in 211 cases (99%) showed opacity in 209 cases (99%). In one case, 2 circular opacities were observed, one of which had a double contour, indicating the ingestion of 2 foreign bodies (Figure 1: a, b, c, d, e, f). Foreign objects were a coin in 182 cases (85.4%), a shirt button in 4 cases (1.88%), a food in 7 cases (3.27%), and a flat battery in 3 cases (1.41%) (Table III). In 2 cases (1%) the EC was radiolucent.
Figure 1: Front cervico-thoracic radiograph showing different radiopaque foreign bodies (a,b,c,d,e,f). a: Circular esophageal CE of metallic tone, round opacity (coin).
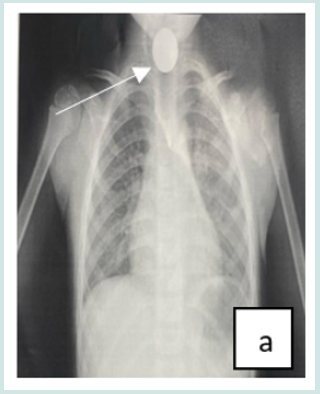
Figure 2: b: Circular esophageal CE of metallic tone, round opacity with an opening (metallic toy piece).
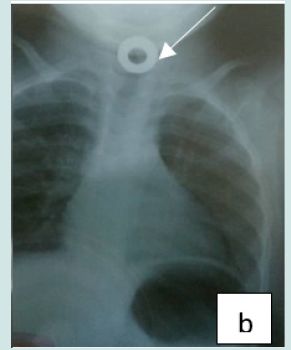
Figure 6: f: circular esophageal CE of metallic tone, 2 opacities including one with a double contour (button batteries).
Discussion
The ingestion of EC is a very common accident in children and begins at the age of acquisition of grip, motor autonomy and the ability to put objects in the mouth. The study by Togo et al. [8] in Mali reports 83.33% of children under 13 years of age and 16.67% of adults for 4 years. The study by Elmehdi Elansari et al. [9] in Mali about 38 cases, shows that 81.6% were aged 0 to 10 years. In this series over 11 years, 213 cases of EC ingestion in children under 15 years of age were collected. The incidence of EC ingestion in children cannot be adequately estimated. In fact, many children swallow objects without showing clinical manifestations [1]. Its frequency increases from the age of 6 months as soon as manual gripping are possible, with a peak between 6 months and 3 years estimated at 70% [4, 5]. A retrospective study carried out by Kacouchia et al at the University Hospital of Bouaké for 4 years and 8 months on 64 cases of digestive foreign bodies, there was a predominance of children under 6 years of age with 69.9%. Their mean age was 4.5 years with extremes of 7 months and 14 years [10]. In this study, children under 6 years of age are also the most affected. This can be explained by the infant’s curiosity to explore the environment and by the fact that children in the oral phase and with oropharyngeal immaturity have a high risk of involuntary ingestion of foreign bodies. In fact, the natural tendency of infants and small children to put to their mouths all the objects that are in their hands favours this accident.
The male predominance reported by several authors [6, 8, 11] was also noted in this study. However, Deguenovo et al in Senegal report a female predominance [12]. This male predominance can be explained by the turbulence and nature of the little boys’ games that resembles a handyman. The nature of the foreign bodies ingested by the child corresponds to all the objects that the child can apprehend and bring to his mouth [13, 14]. Coins are the most common digestive ECs found in children. Other ingested ECs are toys or parts of toys, sharp or pointed objects (pins, nails, razor blades), button batteries or, more rarely, food objects (bones, fish bones) [1]. In the series of Bakyono et al in Burkina Faso, coins were the most common foreign bodies found in the esophagus with 57.08% of cases [11]. The study by Elmehdi Elansari et al in Mali also reports a predominance of coins with 78.9% of cases [9]. Deguenovo et al. [12] in Senegal, a study of 212 cases of esophageal foreign bodies reports a predominance of coins with 67% of cases.
The time to consultation in the study of Hssaine et al. in Morocco, was on average 5.34 days with the extremes of (1h-4 years) [6]. Bakri et al. [15] in Algeria report an average time to care of 19.14 ±0.729. In the present study, the time to visit ranged from 1 hour to 2 months and 1 day, with an average of 27 hours and 46 minutes. This rather long consultation period can be explained by the lack of equipped health centers in the hinterland, the distance from specialized centers, and the lack of financial resources and transport characteristic of developing countries. The diagnosis of ingestion of EC is obvious during an accident occurring in the presence of the entourage or reported by the child himself, but it can be misunderstood, especially in young children, and only the manifestations will lead to consultation.
Classically, ingestion of EC is manifested by odynophagia, dysphagia, hyper sialorrhea, retrosternal pain, or vomiting [4]. Bakyono et al report dysphagia as a reason for consultation with 25.86% of cases, followed by hyper sialorrhea and vomiting with 18.97% and 10.37% of cases respectively [11]. Coulibaly et al in Mali, find dysphagia in 56.8% of cases, dysphagia associated with hyper sialorrhea in 22.7% of cases, and other functional signs such as cough (4.6%), odynophagia (2.3%), and vomiting (2.3%) [16]. Mahfouza et al. [17] in Jordan report 72% hyper sialorrhea, 71% dysphagia, and 24% vomiting. These signs were also found in our results. These different symptoms can be explained by the size, nature and obstructiveness of the pharyngo-esophageal EC. Meanwhile, Bakri et al report asymptomatic ingestion in 47 cases out of a total of 62 cases, followed by hyper sialorrhea in 10 cases, odynophagia in 3 cases, and dysphagia in 2 cases [15].
Standard cervico-thoracic or cervico-thoracic or cervico-thoraco- abdominal X-rays are routine. It makes it possible to locate radiopaque foreign bodies in the digestive tract, to determine their size and nature, and to detect complications such as pneumothorax, pneumomediastinum or pneumoperitoneum [18]. In this study, ECs were radiopaque in the majority of cases. The study by Bakyono et al in Burkina Faso shows the presence of radiopaque CE in 95.74% of cases out of 97.87% of standard radiographic cases performed [11]. Deguenonvo et al in Senegal found 87% of radiopaque ECs [12]. Radiolucent ECs are diagnosed during endoscopic exploration, including the pharyngo-esophagoscope.
Conclusion
Ingestion of ECs in children is a common household accident. Diagnosis is clinical and radiological. The pharyngo-oesophagoscope is indispensable for the nature of the EC which is most often a coin.
References
- Olives JP, Bellaïche M, Michaud L (2009) Digestive foreign bodies in children. Arch pediatrician 16: 962-4.
- Michaud L, Bellaïche M, Olives JP (2009) Ingestion of foreign bodies in children. Recommendations from the French-speaking Group of Pediatric Hepatology, Gastroenterology and Nutrition. Arch Pediatrician 16(1): 54-61.
- Conners GP (2009) Removal of esophageal foreign bodies. Pediatric Emergency Med 21: 59-70.
- Letard JC, Gay G, Ponchon T, Napoléon B, and Boyer J, et al. (2004) Ingested foreign bodies. Acta Endosc 34(4): 627-629.
- Lachaux A, Letard JC, Laugier R, Gay G (2007) Recommendations from the French Society of Digestive Endoscopy: ingested foreign bodies. Acta Endosc 37(1): 91-3.
- Hssaine K, Belhoucha B, Rochdi Y, Nourri H (2015) Foreign bodies in ENT: Ten years of experience. Pan Afr Med J 21: 91.
- Jafari SA, Kalesi M, Partovi S, Kiani M and Ahanchian H, et al. (2014) Ingested foreign bodies removed by flexible endoscopy in pediatric patients: a 10 year retrospective study. Iran J otorhinolaryngol 26(76): 175-179.
- Togo S, Ouatttara MA, Li Xing (2017) Management for esophageal foreign bodies: about 36 cases. Pan Afr Med J 27: 207.
- Elmehdi Elansari MS, Ag Mohamed EO, Guindo B (2020) Epidemiological and clinical profile of esophageal foreign bodies in a regional hospital. Jaccr Africa 4(2): 67-73.
- Kacouchia N, N gattia KV, Kouassi M, Yoda M and Buraima F, et al. (2006) Foreign bodies in the aero-digestive tract in children. Rev Col Odonto-Stomatol Afr Chir Maxillo-fac 13: 35-9.
- Bakyono KE, Goueta EA, Zagrhe N (2020) Esophageal foreign bodies at the ENT department of Yalgado Ouédraogo University Hospital. Jaccr Africa 4(2): 238-246.
- Deguenonvo REA, Ndiaye M, Loumb B (2009) Foreign bodies in the esophagus: A about 212 cases. Med Afr Noire 56(7): 410-16.
- De Lagausie P (2004) Acquired pathologies of the esophagus in children. EMC Pédiatr 1: 109-17.
- Lheureux P, Cavenaile JC, Cornil A, Nouvelle M and Sermon F, et al. (1996) Foreign body ingestion: Practical attitude. Réan Urg 5: 637-53.
- Bakri S, Batouche D, Sadouk H, Fergoug B (2021) Ingestion of coins in children: Our experience in emergency care at the Oran university hospital. Rev Med l HMRUO 8(2): 23-27.
- Coulibaly SH, Samaké DK, Moussa Younoussou D (2021) Foreign Bodies from the Upper Digestive Tract at University Hospital Center Gabriel Touré: The Contribution of Digestive Endoscopy. Open Journal of Gastroenterology 11(7): 134-139.
- Mahafza T, Batieha A, Suboh M (2002) Esophageal foreign bodies: a jordanian experience. Int J Pediatr Otorhinolaryngol 64(3): 225-227.
- Haennig A, Bournet B, Jean-Pierre O, Buscail L (2011) What to do when faced with the ingestion of foreign bodies. Hepato-Gastro 18:249-57.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...