Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1709
Research Article(ISSN: 2641-1709) 
Pleomorphic Adenoma of Atypical Maxillary Intrasinus Location: Review of Etiopathogenic Theories Based on A Case Report in Yaoundé Volume 10 - Issue 4
Mossus Yannick1,2*, Ngo Nyeki Adèle-Rose1,3, Andjock Christian1,4, Meva’a Roger Christian1,3, Atanga Leonel Christophe1,5, Mbélé Lili Pauline5, Mindja Eko David1,3, Ngaba Mambo-Pouka Olive Nicole1,3, Djomou François1, Njock Louis Richard1, Ndjolo Alexis1
- 1Department of Ophthalmology, ENT and Stomatology
- 2Yaoundé Emergencies Centre
- 3Yaoundé Central Hospital
- 4Yaoundé General Hospital
- 5Yaoundé Gynaeco-Obstetric and Paediatric Hospital
Received:March 14, 2024; Published:March 22, 2024
Corresponding author:Mossus Yannick, Department of Ophthalmology, ENT and Stomatology, Faculty of Medicine and Biomedical Sciences, University of Yaoundé 1.
DOI: 10.32474/SJO.2024.10.000344
Introduction
Pleomorphic adenoma (PA) is a tumor that develops in the main (70%) and accessory salivary glands. Atypical locations in the upper airways are rare, dominated by the nasal cavity (82.5-90%) followed by the maxillary sinuses and nasopharyngeal tract. We report the case of a 57-year-old female patient with a non-contributory past medical history who was admitted with swelling of the left maxillary region that had been progressing slowly for 8 years. Clinical examination and CT scan revealed a tumor of the left maxillary sinus. Transfacial surgery was performed and analysis of the surgical specimen revealed a pleomorphic adenoma. We discuss the various aetiopathogenic theories that may explain this atypical location in the light of the literature.
Keywords:Pleomorphic adenoma; A typical location; Maxillary sinus; Aetiopathogenic hypotheses; Clinical case report; Yaoundé
Introduction
Pleomorphic adenoma (PA) is a tumor that develops in the main and accessory salivary glands. It accounts for 70% of salivary gland tumors, 65% of which are located in the parotid gland [1]. Histologically, it is a combination of epithelioid growth and connective tissue-like growth. Extra-parotid locations of AP are dominated by the palate, followed by the upper lip and oral mucosa [2]. PAs of the upper respiratory tract have rarely been described in the literature and occur almost exclusively in the nasal cavity, with the nasal septum accounting for 82.5 to 90% of reported incidences [3,4]. followed by maxillary sinus and nasopharyngeal tract [5]. Several theories have been put forward in the literature to explain locations in the upper airways. We report a case of maxillary intrasinusal PA and discuss the various theories explaining this entity in the light of the literature.
Patient and Observation
This was a 57-year-old female patient who came to our clinic with a painless swelling of the left subpalpebral region that had been progressing slowly for 8 years without epistaxis or headache. Her past medical history showed that she was a farmer with no known chronic pathology, but with a history of sniffing tobacco and consumption of common alcohols, which could not be quantified. On clinical examination, the patient had a developed curvature in the left maxillary region with healthy, preserved skin and sensitivity. In the mouth, the left hemipalate was puckered without crossing the midline. Endonasal examination without preparation revealed a healthy mucosa and a seromucous discharge from the left middle meatus. The endonasal structures were not compressed. The diagnosis of right maxillary endosinus tumor syndrome was made and a contrast CT scan was ordered. The CT scan showed a sinus tissue process pushing back the bony structures without lysing them. The patient was prepared and taken for surgical removal under general anesthesia and orotracheal intubation.
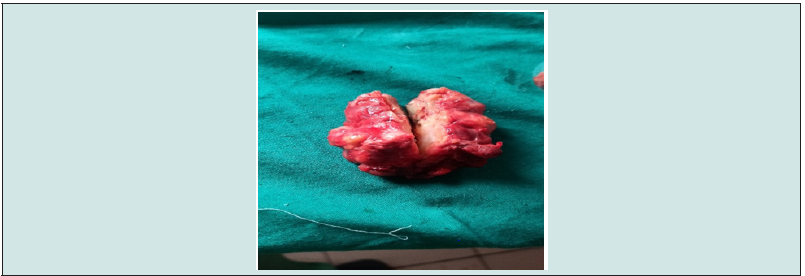
The approach was lateronasal incision with a labial extension and the findings were a fully encapsulated mass of elastic consistency with a bumpy surface (Figure 1). The orbital floor, although weakened, was spared. At the end of the operation, there was a bucconasal communication approximately 10 cm in diameter, which was closed by a simple mucosal suture. The immediate post-operative course was straightforward and the patient was discharged on the 3rd post-operative day. Analysis of the surgical specimen revealed a pleomorphic adenoma. After three weeks, there was a buccosinusal communication approximately 5 mm in diameter with infected edges. Controlled healing was recommended along with antibiotics. At 3 months, the patient was reviewed with a satisfactory facial scar and complete bucco-nasal closure (Figure 2). After 22 months of follow-up, no local recurrence had been noted.
Discussion
Age et Sex
Pleomorphic adenomas of a typical location are a fact, without explanation, of female subjects whose usual age is between the third and sixth decade of life at the onset of the disease [7-9]. This fact was also noted in our clinical observation.
Extraglandular location
Pleomorphic adenomas are most often found in the salivary glands. Neoplasms of the minor salivary glands can occur at any site. The palate, upper lip and buccal mucosa are the three most common sites, accounting for 82.2% of all minor salivary gland tumors [1,10]. Pleomorphic adenomas of the upper respiratory tract have been rarely described in the literature and occur almost exclusively in the nasal cavity, with the nasal septum accounting for 82.5 to 90% of reported incidences [3-5] followed by maxillary sinus and nasopharyngeal tract [6]. Berenholz et al. and Ishikawa et al. have described mixed intranasal tumors without primary involvement of the paranasal sinuses, which confirms their rarity [9,11] Although the vast majority of minor mucous and serous glands are located in the lateral nasal wall, pleomorphic adenomas in the nasal cavity get their origin mainly from the nasal septum [8].
Aetiopathogenic theories
Since the discovery of various sites of pleomorphic adenomas, the literature has continued to question the aetiopathogenesis of these so-called a typical localization. The origin of sino-nasal PA remains debated. Several aetiopathogenic theories have emerged since the late 1980s. A distinction is made between so-called embryological or congenital theories and acquired theories. In embryological terms, three theories have been put forward to explain nasosinusal PA: i/ Matthew et al suggest that a misplaced embryonic epithelial cell in the mucosa of the nasal septum could be the cause of a nasosinusal PA [12]; ii/ PAs may have their origin from remnants of the vomeronasal organ early in foetal life [13] and iii/ Evans RW and al suggest that PAs origin is from fully mature salivary gland tissue [14]. The acquired theories were reported in a systematic review of maxillary sinus PAs [15].
These theories are underpinned by the proximity of the maxillary sinus to the hard palate and nasal cavity. We know that PA can come from glands in the buccal mucosa and approach the maxillary sinus from the side of the palate [16,17]. Similarly, the nasal PA also develops close to the maxillary sinus [2,9,18,19]. Since CB maintained that the sinus PA in his case occurred after removal of an endobuccal tumor that had weakened the sinus floor [16]. Histologically, cellularity is generally greater in PAs from the nasal septum than in those from the main salivary glands. From an immune histological point of view, the round epithelial cells of the ductal structures are immunoreactive for cytokeratin and the spindle-shaped myoepithelial cells for S-100 protein [20]. The presence of a preoperative palatal curvature and a postoperative buccosinusal communication in our patient would suggest the theory of an extension by contiguity of an AP having reached the maxillary sinus from the accessory salivary glands of the palate.
Conclusion
AP is a nosological and histological entity that is well described in the literature. The atypical forms, which develop from the accessory salivary glands, are found in a variety of locations, ranging from the oral cavity to the upper airways. There is no single aetiopathogenic theory to explain the atypical nasosinus locations. Histological and immune histological analyses can only distinguish between forms of pure salivary origin and those of nasal origin.
Informed Consent
The patient’s consent had been requested and obtained prior to surgery. The consent form mentioned the possibility of using de-identified images and information in order to share our experience.
Conflicts of Interest
The authors declare no conflicts of interest.
Author’s Contributions
All the authors have contributed to read and approved the final version of this article.
References
- Ray D, Mazumder D, Ray J, Bhattacharya S (2015) Massive ossifying pleomorphic adenoma of the maxillary antrum: A rare presentation. Contempt Clin Dent 6(1): 139-41.
- Othman B, Atmane Z, Mohammed C, Mohammed E and Youssef R et al., (2022) Degeneration of a Huge Pleomorphic Adenoma in the Nasal Cavity Extended to the Hard Palate: A Case Report and Review of the Literature. Indian J Otolaryngol Head Neck Surg 74(s3): 4780-3.
- Sciandra D, Dispenza F, Porcasi R, Kulamarva G and SC et al., (2008) Pleomorphic adenoma of the lateral nasal wall: Case report. Acta Otorhinolaryngol Ital 28(3):150-3.
- Lee KC, CJC (1992) Ossifying pleomorphic adenoma of the maxillary antrum J Laryngol Otol 106(1): 50-2.
- Kumagai M, Endo S, Koizumi F, Kida A and Yamamoto M et al., (2004) A case of pleomorphic adenoma of the nasal septum. Auris Nasus Larynx.31(4): 439-42.
- Batsakis JG (1984) Tumors of the Head and Neck. In: Wilkins W liams and, editor 2nd editio Baltimore p: 76-99.
- Lygeros S, Tsapardoni F, Mastronikolis S, Axioti AM and Grypari IM et al (2021) Pleomorphic adenoma of the maxillary sinus with orbital extension presenting with exophthalmos: a case report. AME case reports Oct 5: 39.
- Gana P, Liam Masterson (2008) Pleomorphic adenoma of the nasal septum: A case report. J Med Case Rep 2: 349.
- Ishikawa CC, Romano FR, Voegels RL, BO (2008) Pleomorphic adenoma of maxillary sinus - A case report. Int Arch Otorhinolaryngol 12: 459-62.
- Waldron CA, SK el-Mofty, DR Gnepp (1988) Tumors of the intraoral minor salivary glands: A demographic and histologic study of 426 cases. Oral Surg Oral Med Oral Patho 66(3): 323-33.
- Berenholz L, Kessler A, S Segal (1998) Massive pleomorphic adenoma of the maxillary sinus. A case reports. Int J Oral Maxillofacial Surg 27(5): 372-3.
- Matthew S, Ersner MD, SM (1944) A mixed tumor of the nasal septum: report of a case. Laryngoscope 54(6): 287-96.
- Stevenson HN (1932) Mixed tumor of the septum. Ann Otol Rhino Laryngol 41: 563-70.
- Evans RW, CA (1970) Epithelial tumors of the salivary glands. In Major Problem in Pathology 1: 1-229.
- Chęciński M, Nowak Z (2022) Maxillary Sinus Pleomorphic Adenoma: A Systematic Review. Surgeries (Switzerland) 3(3): 153-61.
- Sınacı CB (2018) A Rare Localization of Recurrent Pleomorphic Adenoma: The Maxillary Sinus. South Clin Istanbul Eurasia 28(4): 295-6.
- Cai H, Zhang ZH, Zhou MZ, Wu YJ and Yue JX et al. (2023) A Rare Case of Sinonasal Pleomorphic Adenoma. Ear, Nose Throat J.
- Rastogi N, Gupta A (2016) Pleomorphic adenoma of right lateral nasal wall- unusual presentation. Asian Pacific J Heal Sci 3(4): 239-41.
- TG Olajide 1, BS Alabi, BK Badmos, OTB (2009) Pleomorphic adenoma of the lateral nasal wall-a case report. Niger Postgr Med J 16(3): 227-9.
- Jassar P, Stanfford ND, MA (1999) Pathology in focus pleomorphic adenoma of the nasal septum. J Laryngol Otol 113: 483- 5.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...