Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-6003
Research Article(ISSN: 2638-6003) 
Role of Autologous Conditioned Serum in Triangular Fibrocartilage Complex Injuries Volume 5 - Issue 1
Satya Kumar Koduru1*, V V Narasimha Rao2, V Satya Kiran Raju3 and Sateesh Kumar4
- 1Professor & HOD, Department Of Orthopaedics, NRI Academy Of Sciences, India
- 2Junior Resident,Department Of Orthopaedics, India
- 3Junior Resident,Department Of Orthopaedics, India
- 4Junior Resident,Department Of Orthopaedics, India
Received:February 06, 2021; Published:February 12, 2021
Corresponding author:Satya Kumar Koduru, Professor & HOD, Department of Orthopaedics, NRI Academy of Sciences, India
DOI: 10.32474/OSMOAJ.2021.05.000202
Introduction
The Triangular Fibrocartilage Complex (TFCC) Is A Well Defined Structure Located on The Ulnar Aspect Of The Wrist Functioning Primarily To Stabilize The Distal Radio –Ulnar Joint (DRUJ) And Also To Act As A Shock Absorber Across The Ulno-Carpal Joint. The TFCC is vulnerable to either acute or chronic injuries. Positive ulnar variance And Forced ulnar deviation may cause TFCC injuries. Patients with Triangular Fibro Cartilaginous Complex injuries will present with ulnar-sided wrist pain associated with clicking or point tenderness between the pisiform bone and the ulnar. Magnetic Resonance Imaging is a primary diagnostic modality; wrist arthroscopy is the gold standard investigation. Treatment options are conservative therapies such as rest, NSAIDs, corticosteroid injections, and operative management.
Anatomy
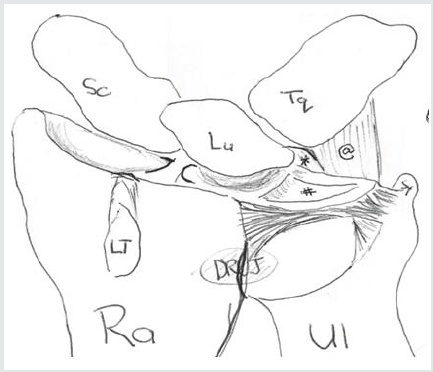
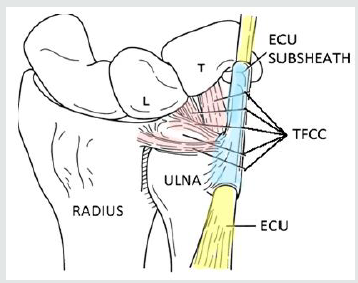
Palmer and Werner Explained the Anatomic Details of The TFCC And Described Its Biomechanical Role at The Wrist. The TFCC Comprises of the (Figure 1)
a) Fibro-Cartilaginous Disc
b) The Dorsal and Palmar Ligaments Spanning Across Radius and Ulna
c) The Ulno-Carpal Ligaments
d) A Meniscal Homolog
e) The Sub Sheath of Ulnar Extensor of The Wrist
Origin: Medial Border of The Distal Radius
Insertion: At the Base of Ulnar Styloid Process
Vascular Supply: The Central Disc Is Avascular, Peripheral Blood Vessels Penetrate Margins Of TFCC
Function: Main Stabilizer Of DRUJ-Distal Radioulnar Joint (Dorsal Portion of TFCC Prevents Volar Displacement of Ulna and Is Tight in Supination and Volar Portion of TFCC Prevents Dorsal Displacement of Ulna and Is Tight In Pronation). Contributes to Ulnocarpal Stability
a) The Complex Anatomy of This Area and The Load Transmission Kinematics Renders It Vulnerable to Injury and Attrition. Both Degenerative and Traumatic Insults Produce Specific Injury Patterns and Can Present as Vague Ulnar-Sided Wrist Pain Particularly During Forearm Rotation.
Aetiology
A TFCC Tear Occurs from
a) Occurs with a compressive load on TFCC during marked ulnar deviation.
b) Associated with positive ulnar variance (radial shortening of 4.5mm)
c) Forced ulnar deviance (i.e., swinging bat, rachet)
d) Advanced Age
There are two types of TFCC tears.
a) Type 1: They occur when a person falls on an extended hand or over-rotates their wrist joint.
b) Type 2: They occur gradually over time. Typically, they result from an underlying condition such as gout or rheumatoid arthritis.
c) The type of TFCC tear will help guide your doctor’s treatment plan.
Epidemiology
a) The prevalence of TFCC injuries increases with advancing age. There is a 49% prevalence in patients above 70 years and 27% in patients above 30 [1]. And according to another study, most TFCC injuries were identical in patients with ulnar-sided pain when compared to other patients who had wrist imaging for conditions other than ulnar-sided pain [2]. Another research suggests that not all TFCC injuries cause ulnar-sided pain.
Pathophysiology
a) The Attachment of TFCC On the Radial Side Is to Hyaline Cartilage, Which Makes It Weak Compared to The Bony Attachment on The Ulnar Side.
b) Positive Ulnar Variance Can Cause TFCC Injury.
c) Ulnar Variance Will Decreases with Supination and Increases with Pronation of Forearm.
d) Minute Changes in Ulnar Length Have Been Shown to Have Significant Effects on The Load Transmitted to The Ulna.
e) The Extensor Carpi Ulnaris (ECU) Relies on The TFCC For Movement. Any Alteration of The Extensor Carpi Ulnaris (ECU) Motion May Lead to Abnormal Force Through The TFCC, Predisposing It to Injury.
Clinical Presentation
a) Patients Usually Complain of Ulnar-Sided Wrist Pain That Gets Worse with Increasing Activity
b) There May Also Be Instability, A Weakness in The Grip, Or Clicking
c) There Is A History of Pain Which Can Occur in Relation With Baseball-Specific Acute Injury Can Be Due To Forced Wrist Extension When A Hitter Attempts To Hit An Inside Pitch And Gets “Jammed’ Or While Doing A Head-First Slide.
d) Chronic Injury Can Occur in Baseball Players Because Of The Heavy Load Placed on The Wrist During the Swing. They Can Sustain TFCC Injuries Even If They Do Not Have Positive Ulnar Variance.
e) In Gymnastics, The TFCC Can Be Injured Because Of Overuse (Both Hanging Elements and Support Skills). With Repetitive Weight Bearing, This Area Can Become Inflamed, And Tendonosis/Tendonitis Can Develop in The Anchoring Wrist Ligaments.
f) TFCC stress test: Symptoms are reproduced by applying a force over the ulna with the wrist in ulnar deviation.
g) Press test: The Patient is asked to lift themselves out of a chair using the wrists in an extended position. Pain indicates a positive test.
h) Supination test: The Patient is asked to grab the underside of a table with the forearms in supination; this causes a load on the TFCC and dorsal impingement, causing pain if there is a peripheral, dorsal tear.
i) Piano key test: Place both hands on a table and press them on the exam table. If the distal ulna becomes prominent on the affected side, it suggests distal radioulnar joint instability, which might have TFCC injury. When palms are relaxed, if the ulnar head goes back to the normal position, it is a positive piano key test.
j) Grind test: Compress radius and ulna and ask the patient to rotate the forearm. Pain could indicate a degenerative process [3].
Imaging
a) Plain Radiographs: Avulsion Fractures of Ulnar Styloid Process, Fractures of Scaphoid, Distal Radial Fracture, Ulnar Variance, Volar Tilt of Lunate or Triquetrum
b) Triple Injection Arthrography: Identification of A Tear
c) Magnetic Resonance Imaging: Identification of Tear (High Sensitivity and Specificity)
Conservative Management
a) It Should Consist of Rest, Ice Application, Activity Modification to Remove the Inciting Force of Injury and Immobilisation In A Splint For 3 - 6 Weeks [4].
b) After the Immobilisation Period, Patient Should Receive Physical Therapy
Autologous Conditioned Serum
a) Autologous conditioned serum (ACS) is an autologous blood product enriched in the interleukin-1 receptor antagonist (IL-1Ra), a naturally occurring inhibitor of interleukin-1 (IL-1).
b) ACS is administered locally to treat conditions in which IL-1 is an important agent of pathologic conditions.
c) Study Participants Treated with ACRS Have Improved Pain and Function; However, These Results Are Preliminary and Need Confirmation [5].
d) With the Help of Innovative and Tested Technology, A Regenerative & Anti Inflammatory Serum Is Obtained from The Patients Own Blood. The Same Is Injected into The Affected Area. Acs Helps in Activating the Body’s Regenerative Capacity
e) IL-1Ra has been produced in Escherichia coli as the recombinant molecule anakinra, marketed as Kineret.
f) ACS was first used clinically in 1997.
g) The Focus of Acs Is on The Production of Positive Interleukins & Growth Factors. These Are Crucial in Intervening the Pain Cascade, Causing It to Stop and Subsequently Triggering the Regeneration Process [6-10].
Preparation
a) Beginning in 2001, ACS was manufactured as Orthokine in a Good Manufacturing Process (GMP) facility.
b) Participating physicians were provided with syringes containing treated glass beads.
c) The beads are 3.5 mm in diameter, comprise borosilicate glass of maximum hydrolytic resistance, and polished according to a proprietary process.
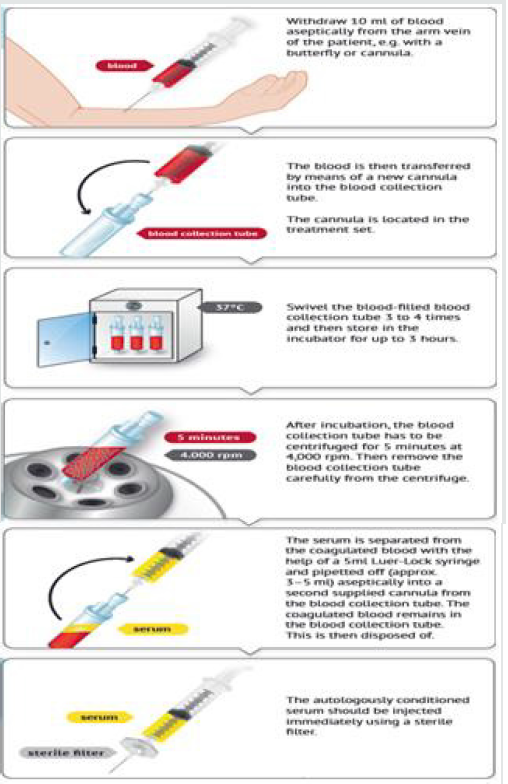
d) Blood was drawn into syringes and shipped to the GMP facility for the production of ACS.
e) The syringe and its contents are then incubated at 37 degrees for several hours, during which time platelets degranulate and mononuclear cells synthesize and secrete IL-1Ra along with a variety of additional anti-inflammatory products.
f) During this period, synthesis of the inflammatory cytokines IL-1b and tumor necrosis factor-a (TNF-a) does not increase significantly.
g) After incubation, the ACS is recovered and sterilized by filtration.
h) ACS is then injected locally into sites of injury or disease. Typically, six injections of ACS, each 2 mL, were injected into knee joints over a period of 3 to 6weeks (Figure 2 & 3).
Purpose of The Study: Material & Methodology
a) To Evaluate Functional & Clinical Results of ACS In TFCC Injuries.
b) Duration of the Study: 06 Months.
Material & Methodology
a) A Study Of 12 Cases Done in Nri Medical College & Orthocare, Vijayawada Over 12 Months.September 2019 To August 2020.
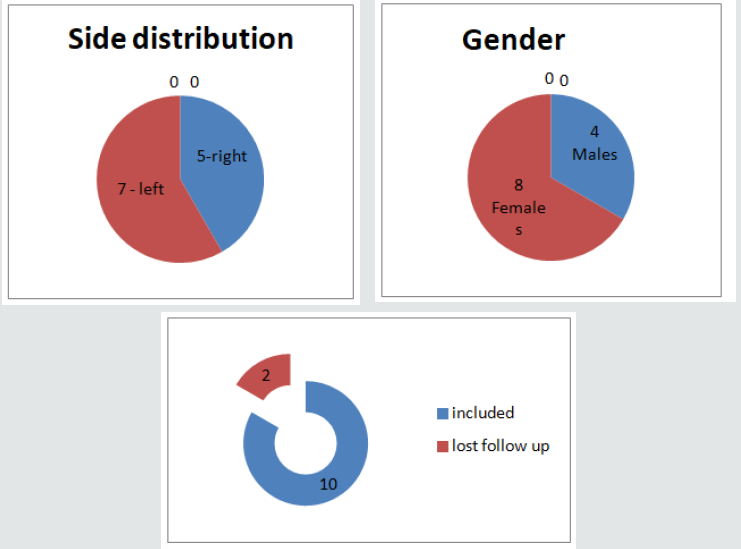
b) Twelve patients Clinical and Radiological Evidence of TFCC Injuries Secondary to Sporting Activities Were Recruited For This Study.02 patients lost to follow up. So only 10 cases results are taken into consideration.
c) 08 CASES FEMALES & 04 CASES MALES. The average age was 41.0 years (range 18–63).
d) RIGHT-SIDED INVOLVEMENT IN 05 &LEFT SIDED IN 07 PATIENTS.e) ETIOLOGY IN THESE CASES WAS RELATED TO SPORTING ACTIVITY OR GYM ACTIVITY.
f) DIAGNOSIS WAS MADE CLINICALLY, PLAIN RADIOGRAPHS, HIGH-RESOLUTION
Ultrasound & Mri
a) Procedure Adopted - The Patients Received One Dose of ACS & wrist immobilization done for Three weeks after the injection. They were Evaluated At the end of 6weeks, 3months & 6 Months for Clinical & Functional Evaluation Using Vas for Pain, DASH& MMWS.
b) Average Length of Follow Up - 06 Months
c) Primary Complete blood picture & Random Blood Sugars Were Assessed Before Taking Up for This Treatment.
d) Patients with More Than 200mg/Dl Blood Sugar Levels Were Advised Physician Consultation to Get Their Sugars Controlled and Come Back for Injection.
e) Patients with More Than 10gm% Of Hemoglobin & Platelet Count More Than 200,000/cubic millimeter. Were Included in This Study.
Inclusion Criteria
a) Type 1 Injuries with Stable Distal Radio Ulnar Joint
Exclusion Criteria
a) Type 2 Injuries Which Are Secondary to Gout or Rheumatoid Arthritis
b) Pregnant Women
c) Previous Surgery Around the Damaged Area
d) Blood Dyscrasias
e) Drug Abuse
Results: Results Were Based on The Following Crieteria.
a) Visual Analog Score for Pain
b) Subjective Evaluation of Pain Reported by Each Patient on Average Since the Last Visit. Minimum = 0. Maximum = 10
c) 2. MMW Score
d) (The Modified Mayo Wrist Score (MMWS) Is A Modification of The Geen And O’Brien Score. There Is A Total Of 100 Points, Which Are Divided Among the Evaluator’s Assessment of Pain (25 Points), Grip Strength (25 Points), Active Flexion/Extension Arc the Ability to Return To Regular Employment Or Activities (25 Points) And As A Percentage Of The Opposite Side (25 Points). Pain Is Rated as None (25 Points), Mild (20 Points), Moderate (10 Points), Or Severe (0 Points) By the Evaluator, Based on The Patient’s Subjective Description. The Total Score Varies between 0 To 100 Points, With Higher Scores Indicating A Better Result. An Excellent Result Is Defined As 90-100 Points, Good Is 80–89, Fair Is 65–79 Points, And Poor Is Less Than 65 Points).
Dash (Disabilities of The Arm, Shoulder, Hand)
(The questionnaire was designed jointly by researchers at the Institute of Work and Health in Canada and the American Academy of Orthopedic Surgeons. “Disabilities of the Arm, Shoulder, and Hand (DASH)” score is a measure of 30-items, designed to assess the patient’s health status. It enquires the amount of difficulty in performing different physical activities due to arm, shoulder, and hand problems (21 items), the impact of the problem on social functioning, work, sleep, and self-image (four items), and the severity of each of the symptoms of pain, activity-related pain, tingling, weakness and stiffness (five items). Each item has five response options. The scores range from 0 (no disability) to 100 (most severe disability)
Results
a) 10 Cases Came for Complete Follow-up.
b) 02 Cases Lost Follow Up After Injection.
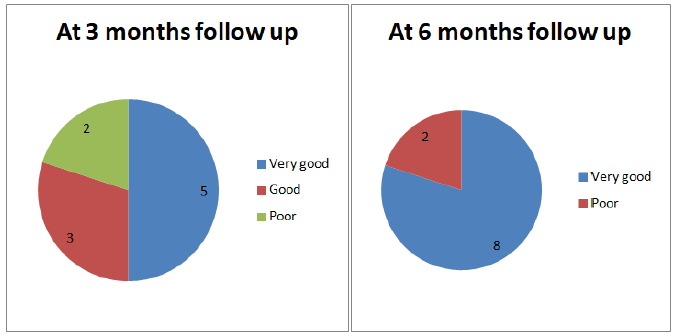
c) 05 Cases Had Excellent Result, 03 Cases Had Good Result and 02 Had Poor Result at The End Of 6 Weeks.
d) But at The End Of 03 Months, Follow Up With 08 Cases Gave Us Total Positive Response and We Labeled Them Under the Excellent Result Category.
e) Return to Gym and Sporting Activity 6weeks After the ACS Injection Seen In 08 Cases.
f) The Remaining 02 Cases Who Had Poor Results at The End Of 6 Weeks Were Given One More Shot of ACS &They Gave Good Response at The End Of 6 Weeks After 2nd ACS Injection.
Conclusion
Through ACS Therapy, We Have Found That Pain Can Be Dramatically Reduced and Healing Stimulated. Treatment Is Fast- Acting While Providing Long-Lasting Relief. Time to Return to Sporting and Gym Activities Also Reduced Compared to Conventional Treatment in Which It Is 3 Months, Whereas In This Study We Found Time Took To Getting Back To Gym & Sports Related Activities Is 6weeks. We Are in The Opinion That ACS Is A Safe Method to Treat Type 1 TFCC Injuries in Terms of Faster Returning to Activities and Also in Getting Rid of Pain Along with No Complications, Which Are Usually Seen in Treatment with Conventional Method of Treatment Which Is Prolonged Immobilisation. In 02 Cases Initial Response Was Poor Later With 2nd Shot of Acs Resulted in Good Outcome. Chances of Getting Good Results With 2nd Acs Injection to Be Kept in Mind.
References
- Kyle Casadei, John Kiel (2020) Triangular Fibrocartilage Complex. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing
- Akram Jawed, Mohammed Tahir Ansari, Vikas Gupta,TFCC injuries: How we treat? Journal of Clinical Orthopaedics and Trauma 11(4): 570-579.
- Effectiveness Between Two Surgical Techniques for reconstruction of proximal humerus fractures
- Correction: Study protocol: a prospective cohort on non-communicable diseases among primary healthcare users living in Kosovo (KOSCO)
- Roh YH, Kim S, Gong HS, Baek GH, et al. (2018) Prevalence and clinical characteristics of radiographic central triangular fibrocartilage complex tears in symptomatic and asymptomatic individuals younger than 50 years. Archives of orthopaedic and trauma surgery. 138(8): 1173-1178.
- Tang JB, Ryu J, Kish V (1998) The triangular fibrocartilage complex: an important component of the pulley for the ulnar wrist extensor. The Journal of hand surgery 23(6): 986-991.
- Andersson JK, Axelsson P, Strömberg J, Karlsson J, Fridén J, et al. (2016) Patients with triangular fibrocartilage complex injuries and distal radioulnar joint instability have reduced rotational torque in the forearm. The Journal of hand surgery, European 41(7): 732-738.
- Barlow SJ (2016) A Non-surgical Intervention for Triangular Fibrocartilage Complex Tears. Physiotherapy research international: the journal for researchers and clinicians in physical therapy 21(4): 271-276.
- Anderson ML, Larson AN, Moran SL, Cooney WP, Amrami KK, Berger RA, Clinical comparison of arthroscopic versus open repair of triangular fibrocartilage complex tears. The Journal of hand surgery. 33(5): 675-682.
- Moldner M, Unglaub F, Hahn P, Muller LP, Bruckner T, etal. (2015) Functionality after arthroscopic debridement of central triangular fibrocartilage tears with central perforations. J Hand Surg Am 40(2):252–258 e252.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...