Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-6003
Review Article(ISSN: 2638-6003) 
Intramedullary Nailing Compared with Spica Casts for Isolated Femoral Fractures in Four and Five-Year-Old Children Volume 1 - Issue 5
Ahmed H Amin*, Mohamed El-Sadek, Mohamed A Sebai and Ibrahim Mehrez
- The Study performed at Zagazig University Hospitals, Sharkia, Police Hospital, Mounira General Hospital, Sayeda Zeinb, Cairo, Egypt
Received: August 28, 2018; Published: September 04, 2018
Corresponding author: Ahmed H Amin, The Study performed at Zagazig University Hospitals, Sharkia, Police Hospital, Mounira General Hospital, Sayeda Zeinb, Cairo, Egypt
DOI: 10.32474/OSMOAJ.2018.01.000125
Abstract
Purpose: To discuss the best method of management of femoral fractures in four and five year old children.
Methods: A cohort of 100 children with 100 fractures (non- pathological; not involving condyles or cervicotrochanteric area; No Associated injuries; and not open fractures) were prospectively examined (50 patients managed with spica casts and another 50 patients managed with intramedullary nailing). Radiographic and clinical outcomes were compared between the groups. Statistical analysis of the results has been done.
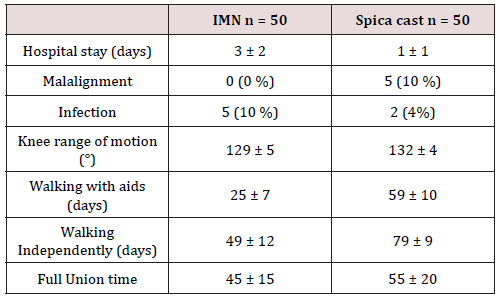
Results: The mean follow-up was 12 ± 4.3 months, the mean hospital stay was 3.2 ± 1.1 days for IMN and 1±1 for spica cast, and the mean time to nail removal was 22.3 ± 10.2 weeks. The mean time to union was 45 ± 15 days in IMN and 55 ± 20 days ln spica cast. Union was significantly correlated to age (p=0.000) and fracture shape (p = 0.005), but not to the fracture level, nature, or mechanism.
Conclusion: IMN is a dependable, safe, and cost-effective alternative to traction and cast in four and five year old children.
Keywords: Femur fractures Intramedullary nailing four and five year children Elastic Nancy nail Spica cast
Introduction
Femoral diaphyseal fractures are the most common major pediatric injuries treated by the orthopedic surgeon [1]. They represent about 1-2 % of all bony injuries in children [2]. Seventy percentage of femoral fractures involve the shaft [3]. The cause of these injuries varies with age; in preschool children the most common mechanism is a fall from a height. In children aged 4-12 years accidental injury during sport is the predominant cause [4]. A vast majority of femur fractures in children heal without any longterm sequelae [4]. With better understanding of biology of fracture healing and with advances in fixation methods and operative techniques, there has been a general trend toward operative stabilization of femoral shaft fractures in children. Operative treatment options for femoral fractures in children include plating, rigid intramedullary nailing, flexible intramedullary nailing, and external fixation.
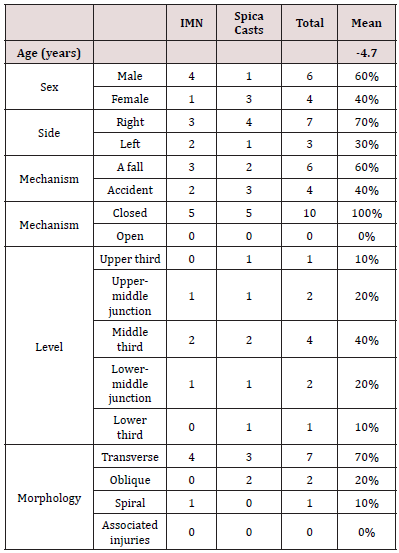
However, Martinez [5] reported excessive shortening and angular deformity in around 43 % of their patients treated by an early spica cast. Hughes [6] studied the impact of immediate spica casting on patients and families following femoral shaft fractures. They found that the greatest problems encountered by the family in caring for a child in a spica cast were transportation, cast intolerance by the child, and keeping the child clean [4-6]. Although most authors still recommend conservative methods of treatment in pediatric femur fractures in preschool children, there is still confusion regarding the optimal method for children beyond this age group [7]. In this study we compare two main methods in the treatment of isolated femoral fractures in four and five years old children which are intramedullary nailing and spica casts to assess the best method of management of femoral fractures in this age (Table 1).
Patients and Methods
A retrospective comparative analysis of two groups of children aged 4-5 years who sustained a non-pathological femoral shaft fracture was performed. Number of patients with Isolated Femoral Fractures that has been admitted to orthopedic department is equal to (100) as follow;
a) Group I: 50 patients managed with spica cast.
b) Group II: 50 patients managed with IMN.
Inclusion criteria were Four and Five-Year-Old Children, both genders were included, Patients with stable and unstable Isolated Femoral fractures, and Mode of trauma: including both low and high velocity injuries. Exclusion criteria were Patients with bilateral femoral fractures, Multiple trauma patients with other surgical injuries, Open and comminuted fractures, medically unfit patients who can’t undergo anesthesia and surgery in general, Sever soft tissue problems in area of surgical approach (burns, necrosis, acute infection), and pathological fractures. The clinical data of the patients fulfilling the inclusion criteria has been evaluated as follows;
Clinical data: History has been taken from the family, including the date of the injury to define the type and mechanism of trauma. Physical examination has been documented.
Radiographic examination: The patients had the following radiological examinations: An antero-posterior (AP) view of the pelvis and an (AP) and a cross table lateral view of the involved femur. Computed tomography (CT) and magnetic resonance imaging (MRI) was not necessary for any case.
Laboratory investigation: The patients had the following pre-operative routine lab.
Investigations: Complete blood count and Bleeding profile.
Management plane
A -For intramedullary nailing:
The patient has been positioned supine on a standard radiolucent orthopedic table with traction piece and fluoroscopic control. The nail was applied in the standard manner. At the level of the distal femoral metaphysis, the femur was reached with medial and lateral incisions. To avoid residual angulation, the nails had introduced at the same level. The medullar canal was reached through the first opening. The tip of the commercial nail has been ready to bend with an angle of 450.
The implant diameter was selected to be one-third or 40 % of the narrowest diameter of the femoral diaphysis. The titanium elastic nails were bent with a similar gentle curvature, so as to have contact at three points. Following closed reduction under fluoroscopy, the medial and lateral nails have been advanced to the proximal. To avoid soft-tissue irritation, only a small part of nail was left outside. Open reduction was not been necessary for any case. Splint must be done after IMN.
Post-operative follows up: Postoperative radiographs have been requested to check for reduction and nail length. discrepancy and rotational malalignment were performed. Stitches was removed after 10 days. Partial weight-bearing will be allowed after 3-5 weeks, according to the stability of reduction, type of fracture, weight, and compliance of the child. Full weight-bearing will be allowed after union has achieved. Nail removal has been done at least 7 months after surgery.
B - For spica casts
spica cast has been applied with the patient under general anesthesia. A plaster cast or a sitting spica cast, which allows the child to be placed in a sitting position in the chair, was applied. The plaster has applied with 15° up to 90° of flexion, 30° of abduction, and 15° of external rotation at the hip and with 15° up to 90° flexion at the knee. The plaster was molded anteriorly and laterally to prevent anterior and varus bowing. Acceptable reduction comprises less than 15° of angulation and less than 2cm of shortening. If reduction is not acceptable, the spica cast has been reapplied after.
Result
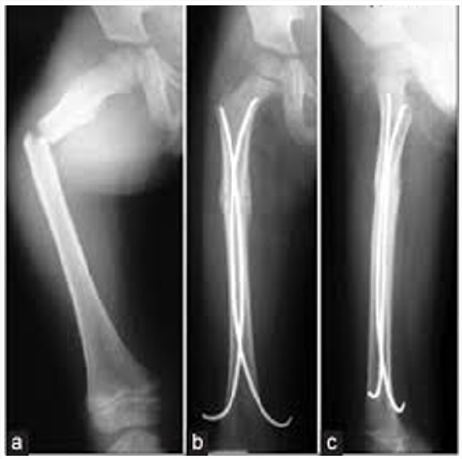
A total of 100 patients diagnosed with and treated for isolated femoral fracture were evaluated throughout this study. Fifty patients were treated with elastic nail fixation (Figure 1) and another fifty remanipulation. The spica cast has been kept in place for 4-8 weeks.
Follow up
The patients were followed until full union and walking undependably occur which may take from two to six months. follow-up, we documented the range of motion of the hip and knee, evidence of soft tissues irritation by nail ends, length discrepancy (measured by a tape from the anterior superior iliac spine to the medial malleolus), rotational alignment (by comparing hip rotation to the normal side), infection, gait, and status of weight-bearing. Radiographs were requested to document union, mal- union, nail position, and remodeling. Fracture union was defined as the ability to fully bear weight (or resume previous level of activity for nonwalkers) without pain in the presence of bridging callus on at least three cortices. Delayed union was defined as the persistence of bone pain and tenderness 3 months after the reduction without complete radiological union. Non-union was defined as absence of osseous union more than 6 months after injury. Nail removal was done when the fracture line completely disappeared on radiographs.
Statistical analysis
The data are shown in the form of mean ± standard deviation (SD) and range. All statistical analyses were done using the SPSS program. The results regarding the fixation of isolated femoral fractures with spica casts has include the following: Time of hospital stay, Time of mobilization after operation, Time of walking alone, Malalignment and infiction, and knee range of motion with early reduction and spica cast. All the fractures were closed fractures. Full union was achieved in all cases. An important difference is that other studies (105) represented all femoral fractures regardless of associated injuries whereas we limited our study population to isolated femoral fractures in otherwise healthy children. it is not common practice to perform IMN in two to three-year-olds, and sixyear- olds are generally managed operatively, so we narrowed the age range for our investigation to 4.0 to 5.9 years of age.
The mechanism of the injury, fracture location and fracture types of groups are listed. No significant difference was determined when the groups were compared according to these parameters. When the groups compared, the spica cast group was found to have a shorter duration of hospital stay (1 ± 1) compared with elastic nail group (3 ± 2). The knee range of motion of the spica cast group (132° ± 4) two (months after operation) was found to be better compared with the elastic nailing group (129° ± 5) (after removal of the cast). The elastic nailing group was found to have started walking earlier both with and without support (Table 2). Patients with intramedullary nailing started to walk with aid after one month and independently after 2 weeks. Patients with spica cast start to walk with aid after 2 months and independently after 12 weeks.
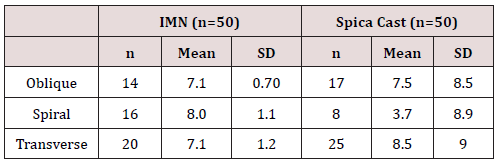
The clinical measurement of patients’ limb length discrepancy was within the acceptable limits (Table 3) in this group. Malrotation was not detected in any of the patients in both groups. One superficial infection with implant irritation developed on the incision site in one patient. The implant was removed in this patient. Malalignment was detected in one (20%) patients as complication in spica cast group and it was in Coronal view immediate after operation within normal values, and Zero (0%) as complication in intramedullary nailing. Intramedullary nailing has psychological, social, educational, and some economic advantages over hip spica. parents found difficulties in dealing with the spica cast, and it wasn’t acceptable by some high social and educat ED families.
Discussion
The last few decades have seen an increasing trend toward operative management of children’s fractures that had previously been treated non operatively. As with all treatment choices, there are logical advantages and disadvantages to each approach. The positive attributes of IMN of femoral fractures in children include the reduced need for postoperative immobilization, an earlier range of motion of the hip and knee joints, and perhaps greater ease of care since the family can avoid the challenges associated with a child wearing a spica cast for several weeks. The negative attributes of surgery include permanent visible scars and the introduction of the risk of infection, a theoretical risk of injury to adjacent neurovascular structures (an unlikely but potentially serious complication), and the frequent necessity for a second surgical procedure to remove the instrumentation (either electively or because the implant is symptomatic). Additionally, operative treatment necessitates the use of an operating theater whereas spica casts can be applied in the emergency room or in procedural units.
Mansour [8] compared spica cast placement in the emergency department versus the operating room, and concluded that the outcome and complications were similar, but the children treated in the operating room had longer hospital stays and significantly higher hospital charges [8]. Cassinelli [9] treated 145 femur fractures, all in children younger than age 7, with immediate spica cast application in the emergency department. All children younger than 2 years of age, and 86.5% of children of ages 2 to 5 years old, met acceptable alignment parameters on final radiographs [9]. Rereduction in the operating room was needed in 11 patients. The investigators concluded that initial shortening was the only independent risk factor associated with lost reduction [9]. The treatment for femoral fractures varies according to factors such as the age of the patient, the fracture type, localization and surgical experience. Despite the increase in surgical treatment choices, with the increase in fixation techniques and improved imaging methods, the basic rules described for the treatment for paediatric femoral fractures remain valid today. These basic rules as described by Dameron and Thompson [10] are
a) The simplest treatment is best.
b) The initial treatment should be permanent where possible.
c) Perfect anatomic reduction is not essential for perfect function.
d) Restoration of alignment is more important than fragment position.
e) Overtreatment is usually worse than undertreatment.
f) Immobilise/splint the injured limb before definitive treatment.
Femur fracture is the most disabling fracture in children. Children at school age are treated using various methods, such as compression plating, submuscular plating, locking bridge plates, rigid intramedullary nails. stainless steel or titanium elastic nails, and external fixators [11]. Preschool children are usually treated with traction, immediate spica cast, or traction then delayed spica cast. Although they produce very good union rates, their disadvantages include loss of reduction requiring repeated adjustments under anesthesia, prolonged immobilization, high malunion rate, compartment syndrome, and Volkmann’s ischemic contracture [12].
The care for the child in spica is particularly troublesome. External fixation has been used in children as young as 3 years of age and, despite the simplicity of its insertion, it is cumbersome and has many complications, such as pin tract infection, which might lead to septic shock , limitation of knee motion, refractures of up to 21.6 % , ugly scars, and the need to apply plaster spica after removal in some cases [13], There are no reports of rigid intramedullary nailing in preschool children because of the risk of avascular necrosis of the femoral head and coxa valga [14]. Minimally invasive submuscular and bridging plating for preschool children has been successful. It offers more rigid fixation than flexible nails, which is reflected in easier mobilization and safer weight-bearing. However, it is more invasive, and its invasiveness can increase at the time of metal removal, where bony overgrowth may develop over plate ends, which requires open release of plate ends. Formal plating carries the same risks besides blood loss, periosteal stripping which might lead to femur overgrowth, and infection [14].
Elastic stable intramedullary nailing was introduced by Pre´vot [14], utilizing the three-point fixation principle. The technique offers good reduction, dynamic axial stabilization, and early rehabilitation. However, it has many disadvantages, such as length discrepancy, rotational malalignment, malunion, nail exteriorization, and interference with knee motion by the prominent nail ends [14]. Our surgical time, resorting to open reduction, time to union, incidence of painful nail ends, time to nail removal, rotational malalignment, limb overgrowth, shortening, and angulation are more or less similar to other reported series. Spiral fractures were significantly correlated to shortening, slower union, and overgrowth (which did not reach clinical significance). Care should be practiced during the trimming of nail ends at the completion of surgery because too long nail ends lead to soft tissue irritation and a second surgery for retrimming is definitely an avoidable complication. A bursa overlying one or both ends may imply irritation by the nail ends.
This minimally invasive technique requires short hospital stay compared to other methods of treatment, and this series proved that it can be done with minimum hospital stay, as most children were discharged on the day of surgery [15]. Preschool children constituted a small number of patients treated in many series, but, to the best of our knowledge, only five articles have specifically addressed this age group and only three of them were about elastic nailing. The children studied were treated using the one-surgeonone- technique approach, which would give a better assessment of the results [15].
External fixators were reserved for open fractures of grades II or III (Gustilo’s). Plating was also reserved for comminuted fractures where restoring and retaining the femur length would not be feasible with elastic nails and for solid malunion where an open osteotomy is required [15]. A rigid nailing option is not on the table in these young femurs, so we were left with two options for fractures without inherent instability: spica cast and TEN. Our choice of TEN was based on frequent complications of spica cast, lack of ideal cast care in rural communities which constitute the main referral base of our institution, choice by the child’s parents, and the better results of TEN compared to spica [16]. We limited our indication to TEN to non-comminuted fractures to avoid collapse at the fracture site with subsequent shortening and angulation, which occurred in 10 out of 15 unstable fractures in Sink et al.’s series [15]. So IMN in four and five year old children in our study and in other studies has achieved good results in comparison to spica cast and other methods of fixation [17].
References
- Mukherjee, Kunal Subhas, Amar Nath Gupta (2017) A Comparative study of the results of conservative treatment versus closed titanium elastic nailing for fractures of shaft of femur in children. Asian Journal of Medical Sciences 8(4): 32-37.
- Coffey C, Haley K, Hayes J (2005) The risk of child abuse in infants and toddlers with lower extremity injuries. J Pediatr Surg 40(1): 120-123.
- Baldwin K, Pandya N, Wolf gruber H (2011) Femur fractures in the pediatric population: Abuse or accidental trauma? Clin Orthop 469(3): 798-804.
- Pace J, Lee David L, Skaggs (2016) Femur Fractures in Neonates, Infants and Toddlers with or Without Child Abuse. Pediatric Femur Fractures. Springer US p. 57-73.
- Coyte PC, Bronskill SE, Hirji ZZ (1997) Economic evaluation of 2 treatments for pediatric femoral shaft fractures. Clin Orthop (336): 205- 215.
- Khanna, Mohit (2017) Tens for The Surgical Management of Femoral Shaft Fractures In 6-14 Years Age Group Children. Pediatric Traumatology, Orthopaedics and Reconstructive Surgery 5(2): 13-21.
- John, Rakesh (2017) Current Concepts in Paediatric Femoral Shaft Fractures. The Open Orthopaedics Journal Suppl 2: M4 11: 353.
- Kaiser MM (2011) Biomechanical analysis of a synthetic femur spiral fracture model: influence of different materials on the stiffness in flexible intramedullary nailing. Clinical Biomechanics 26(6): 592-597.
- Sink EL, Hedequist D, Morgan SJ (2006) Results and technique of unstable pediatric femoral fractures treated with submuscular bridge plating. J Pediatr Orthop 26: 177-181.
- Hedin HANNE (2004) External fixation of femoral fractures in children. J Bone Joint Surg (Br) 86: 214.
- Muzzafar, Khalid, (2017) Early result of pediatric shaft femur fractures treated by hip spica cast in children upto 10 years of age. International Journal of Research in Medical Sciences 5(6): 2430-2432.
- Domb BG, Sponseller PD, Ain M, Miller NH (2002) Comparison of dynamic versus static external fixation for pediatric femur fractures. J Pediatr Orthop 22(4): 428-430.
- Mubarak SJ, Frick S, Sink E, Rathjen K, Noonan KJ (2006) Volkmann contracture and compartment syndromes after femur fractures in children treated with 90/90 spica casts. J Pediatr Orthop 26(5): 567- 572.
- Miner T, Carroll KL (2000) Outcomes of external fixation of pediatric femoral shaft fractures. J Pediatr Orthop 20(3): 405-410.
- Hedequist D, Bishop J, Hresko T (2008) Locking plate fixation for pediatric femur fractures. J Pediatr Orthop 28(1): 6-9.
- Ramseier LE, Janicki JA, Weir S, Narayanan UG (2010) Femoral fractures in adolescents: a comparison of four methods of fixation. J Bone Joint Surg Am 92(5): 1122-1129.
- Saseendar S, Menon J, Patro DK (2010) Treatment of femoral fractures in children: is titanium elastic nailing an improvement over hip spica casting? J Child Orthop 4(3): 245-251.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...