Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Research Article(ISSN: 2641-1725) 
Statistical evaluation and global distribution of early COVID-19 outbreak Volume 5 - Issue 3
Faizan Danish1* and Suhail Salam2
- 1Division of Biostatistics, Department of Population Health, School of Medicine, New York University, USA
- 2Ascent Software Development WLL, Qatar
Received: July 31, 2020; Published: August 18, 2020
*Corresponding author: Faizan Danish, Division of Biostatistics, Department of Population Health, School of Medicine, New York University, USA, Ascent Software Development WLL, Qatar
DOI: 10.32474/LOJMS.2020.05.000211
Abstract
Introduction: An epidemic of Coronavirus Disease 2019 (COVID-19) began in December 2019 in China leading to a Public Health Emergency of International Concern (PHEIC). Clinical, laboratory, and imaging features have been partially characterized in some observational studies. No systematic reviews on COVID-19 have been published to date.
Materials and Methods: We performed a statistical analysis and review of literature to assess clinical, laboratory, imaging features, and outcomes of COVID-19 confirmed cases.Observational studies and also case reports, also discussed published on reputed journals. We perform the statistical modelling to predict its affects in certain countries. Using pictorial and mathematical presentation, we predict the future cases.
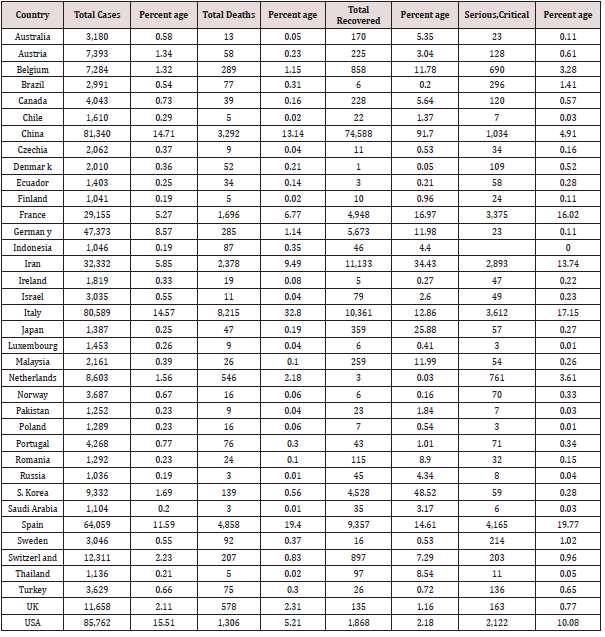
Results: As on 27th March, 2020 as per data available on Johns Hopkins University, World Health Organization etc. , total number of confirmed cases 528171, total deaths is 24599 and the recovered cases 126192. It is observed that the highest number of cases have been noted in USA 85762 which constitutes 15.51% of the total cases in the world followed by China 81340 which constitutes 14.71% of the total cases confirmed in the world. Further, travel restrictions on the country which has become main hub for the COVID-19 showed less number of confirmed cases. Qatar has recorded 562 confirmed cases, 0 death and 43 recovered.
Conclusion: we present an effort to compile and analyze epidemiological outbreak information on COVID-19 based on the several open datasets on Novel Corona Virus 2019 provided by the Johns Hopkins University, World Health Organization, Chinese Center for Disease Control and Prevention, National Health Commission, and DXY. Using different statistical tools, we tried to identify the way through which its affect can be minimized to a large extend..
Keywords: Coronavirus Disease; sars-cov-2;covid-19; statistical modelling; data analysis
Introduction
In December 2019, a series of acute respiratory illness were reported in Wuhan, Hubei Province, China [1,2]. A novel coronavirus, initially named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), was identified as the cause of this disease by the Chinese Center for Disease Control and Prevention (CDC) [3]. This disease, now designated as coronavirus disease 2019 (COVID-19) by the World Health Organization (WHO), rapidly spread to other cities of China, and has become a public health emergency of international concern (PHEIC) following its global spread. COVID-19 is clinically manifests as fever, cough, muscle pain, fatigue, diarrhea and pneumonia, and can cause death in severe cases [4-6]. As on 27th March, 2020, as per Johns Hopkins University and World Health Organization, it has spread in 200 countries with 552,943 cases, 25,045 deaths, 128,706 recovered.Several countries adopted a multipronged surveillance strategy that included applying the case definition at medical consults, tracing contacts of patients with laboratory-confirmed COVID-19, enhancing surveillance among different patient groups (all patients with pneumonia, hospitalized patients in intensive care units [ICUs] with possible infectious diseases, primary care patients with influenza like illness, and deaths from possible infectious etiologies),and allowing clinician discretion (i.e., option to order a test based on clinical suspicion, even if the case definition was not met) to identify COVID-19 patients. Containment measures, including patient isolation and quarantine, active monitoring of contacts, border controls, and community education and precautions, were performed to minimize disease spread. Hydroxychloroquine was found to be more potent than chloroquine to inhibit SARS-CoV-2 in vitro [8]. Further, Hydroxychloroquine is an analog of chloroquine that has fewer concerns about drug-drug interactions. In the previous SARS outbreak, hydroxychloroquine was reported to have anti- SARS-CoV activity in vitro [7]. This virus, which is the seventh coronavirus that has been proven to infect humans, has 75–80% genomic similarity to the severe acute respiratory syndrome coronavirus (SARS-CoV), 50% to the Middle East Respiratory syndrome coronavirus (MERSCoV) and 96% to a bat coronavirus and uses the same cell receptor, angiotensin-converting enzyme II (ACE2), that is used bySARS-CoV [1, 9, 3]In a study of 138 patients with 2019 nCoV, 36/138 were admitted to the ICU and they were significantly older than patients who did not require ICU admission (median of 66 compared to 51 years) and were more likely to have underlying comorbidities (72% compared to 37%). In the ICU, 11% of patients received high-flow nasal cannula and 15 (44%) received noninvasive ventilation. Invasive mechanical ventilation was required in 17 patients (47%), 4 of whom received extracorporeal membrane oxygenation as rescue therapy [6]. Interestingly, 44% were reported to develop arrhythmias in the ICU. In another study of 52 critically ill adult patients, the mean age was 60 years, with 40% of patients had at least one chronic illness. Of these patients, 67% developed ARDS, 29% acute kidney injury, 23% cardiac injury and 29% liver dysfunction. Invasive or noninvasive mechanical ventilation was required in 71% of patients. By day 28, 62% of patients died [10].
In this study, we are going to compile the results published through various authentic sources and will make statistical approaches to predict the future of the virus I different countries. Further, we will discuss the measures taken by several countries that leads its less effect.
Review
Importantly, 2019-nCoV is the third fatal coronavirus that has emerged in the past two decades, following SARS and the Middle East respiratory syndrome (MERS) [11, 4]. The numbers of confirmed cases of COVID-19 infection and related deaths are still rising. A previous study revealed high levels of proinflammatory cytokiness/chemokines (e.g., IL-2, IL-7, IL-10, granulocyte-colony stimulating factor (GCSF), IP-10, MCP-1, macrophage inflammatory protein 1 α (MIP1A), and TNF-α) in severely and critically ill patients with COVID-19 infection; furthermore, the presence of cytokine storm was correlated with disease severity [5]. Up to 1st of March 2020, there are over 78,000 confirmed cases and 2700 dead in the world [3]. Patients with coronavirus disease 2019 (COVID-19) had respiratory symptoms and occasional gastrointestinal symptoms including fever, cough, shortness of breath, muscle ache, confusion headache, sore throat, rhinorrhea, chest pain, diarrhea, etc. [5]. It has been reported that the main ways of transmission are shortrange respiratory droplets and indirect transmission, and the other routes of transmission, including mother-to-child, fecal-oral and aerosol transmission, needs further confirmation. However, epidemiological investigation shows that the new infectors had a history of close contact with confirmed SARSCoV-2 patients [12]. The laboratory examinations(including blood routine examination, CRP, lymphocyte subpopulations, and SARS-CoV-2 RNA) as well as the chest CT examination play an important role in diagnosis, treatment and assessment [13].Surprisingly, the transmission of animals to humans is considered the origin of epidemics, as in November many patients reported to have visited a local fish and wild animal market in Wuhan. Apart from this, recently, evidence has been gathered for the animal to the human and interhuman transmission of the virus [14, 15]. An Exploratory Data Analysis (EDA) with visualizations has been made in order to understand the number of different cases reported (confirmed, death, recovered) in different provinces of China and outside of China. Overall, at the outset of an outbreak like this, it is highly important to readily provide information in order to begin the evaluation necessary to understand the risks and begin containment activities [16].As governments and institutions implement social distancing measures, including closures and stopping mass gatherings, they must mitigate the effects of these measures on vulnerable communities. School and university closures disproportionately affect vulnerable groups, [17] in particular students with disabilities and those reliant on their educational institution for food, shelter,residency, and safety.[18] Any institution closing physical locations must articulate plans for accommodating marginalised groups, ideally with input from representatives from such groups.[19] Clinical, laboratory, image findings, as well as the factors associated with evolution of the disease and outcomes, constitute critical knowledge that should be carefully studied when a new infectious disease emerges. Recently, in this context of the COVID-19 outbreak, several questions have been raised, including what is the full spectrum of disease severity (which can range from asymptomatic, to symptomatic-but-mild, to severe, to requiring hospitalization, to fatal)? [20]. With regard to complications and death, a third of patients presented with ARDS, but also, albeit in a lower frequency, acute cardiac injury, acute kidney injury, and shock, eventually followed by multiple organ failure. Therefore, early identification and timely treatment of critical cases are of crucial importance [5]. We observed a CFR of over 13% in 7 studies describing 632 hospitalized patients. In two studies in China (n=41, n=99), the case fatality rates were 15% [5] and 11% [18], respectively. Crude surveillance data [20], indicatedthat till March 9, 2020, from 111,363 reported cases, 3,892 patients have died (3.49%), with >89% of the deaths occurring in China [12,21]. Managing pregnant women with COVID-19 can be complex as the infection has the potential to adversely affect both the maternal as well as the fetal/neonatal outcome.[22] Recently, Liu et al reported clinical course and outcome of 13pregnant patients with COVID-19 showing high complication rates. Five of their patients (38%) had to be delivered by an emergency cesarean (including one stillbirth) due to a variety of indications, and six (46%) had preterm delivery. One mother had multiple organ failure and was on life support with extracorporeal membrane oxygenation at the time of reporting.[22] Another published case series of 9 pregnancies with COVID-19 by Chen et al. reported a cesarean section rate of 100 % but no stillbirth or neonatal death.[23] According to the recommendations from WHO, the United States Centers for Disease Control and Prevention and the European Center for Disease Prevention and Control, at least two sequential respiratory tract specimens, collected at least 24h apart, are required for discharge criteria in clinically recovered patients [24-26].
Material and Methods
The data were fetched from Johns Hopkins University, World Health Organization etc., upto 27th March, 202 for the whole world and for countries individually, data was collected from their official health websites. Percentages and means were calculated to describe the distributions of categorical and continuous variables, respectively. The figures of each country were evaluated with whole world to check the status of the country. Further, for some worst hit countries like Spain, Italy, China, US etc, individual modeling was fitted using graphical method to predict the future cases. In particular, the data of China has been presented with graphical representation.Further, the figures of Qatar has been presented using line graph, pictorial and mathematical representation has been made on the basis of data of China and Italy.
Results
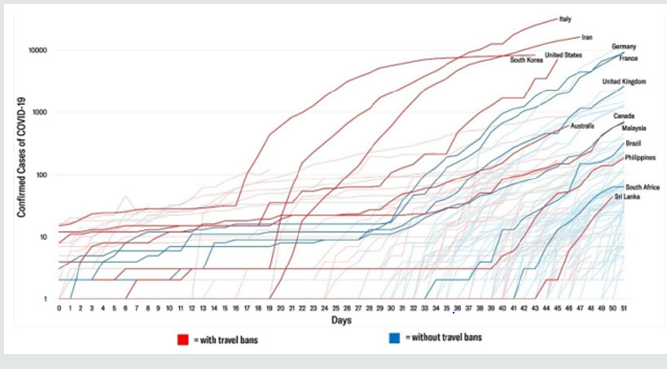
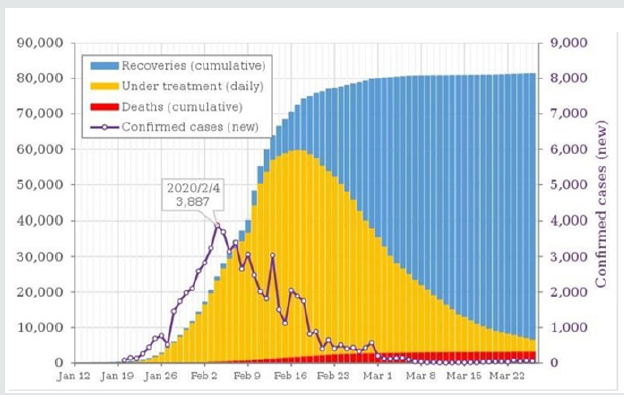
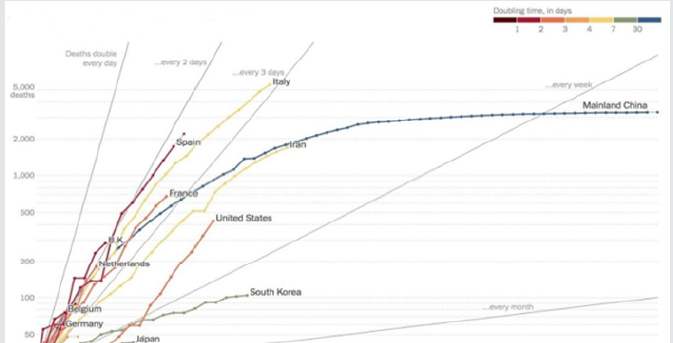
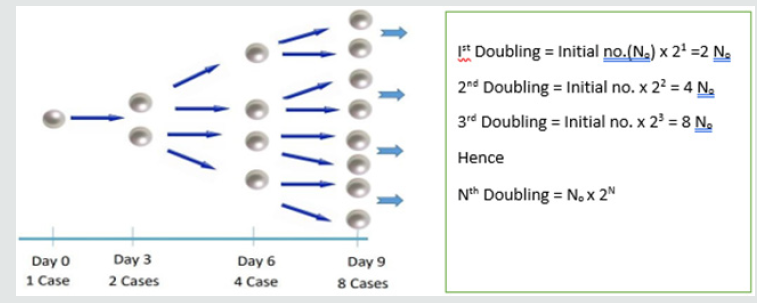
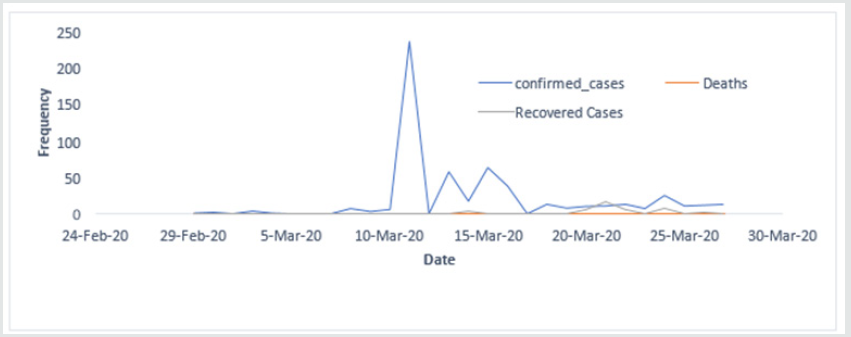
Table 1 demonstrates the data fetched from Johns Hopkins University and World Health Organization up to 27th March, 2020, presented in Table 1 (major countries) for the whole world demonstrated the total confirmed cases, deaths, recovered. The total number of confirmed cases 528171, total deaths is 24599 and the recovered cases 126192. It is observed that the highest number of cases have been noted in USA 85762 which constitutes 15.51% of the total cases in the world followed by China 81340 which constitutes 14.71% of the total cases confirmed in the world. The highest number of deaths is 8215 in Italy which constitutes 32.8% of the total deaths in the world followed by Spain which has 4858 deaths constitutes 19.4% of the total deaths in world. Out of total 528171 cases 126192 cases were recovered which is about 24% of the total recovered cases. Maximum number of cases recovered were in China which is around 91% casesrecovered and found negative which is followed by South Korea which is about 48.5% recovered of the total confirmed cases in the country. About 20% of the total cases in Spain were serious or critical followed by Italy in which 17% cases were in critical condition. We know that the china was the main source of COVID-19, the Figure. 1 identifies the countries who put travel restrictions on china are having decreasing trend in the number of cases rather than those country which did not put the travel restrictions on china. Thus, it can be concluded that putting travel restrictions on the country which has become main hub for the COVID-19 can show less number of confirmed cases. In Figure 2, it shows Confirmed cases, Cumulative deaths, daily under treatment and cumulative recoveries from January 19 to March 22 and is clear that the number of cases were having increasing trend initially, but once the steps like lockdown, disinfect etc. were taken by the government of China the confirmed cases shows the decreasing trend. Thus, it can be concluded that the restrictions like lockdown could show decreasing trend in the number of confirmed cases. Countries having more than 23 deaths are presented in Figure3, it can be observed that the Italy has an increasing trend at this point of time while as China which is origin of COVID-19 and was leading ion the deaths, shows decreasing trend. Further, the South Korea shows a little smooth trend but has decreasing trend. Trend of Italy is followed by Spain and Iran having high number of daily as well as total deaths score. Pictorial and Mathematical representation of the COVID-19 cases in China and Italy are presented in Figure4, it represents how the number of cases is increasing. At this doubling rate of 3 days, we would have 10doublings in a month i.e. 10 doubling = initial no (N0) x 210 = 1024 N0. Using Ghana as an example, on 21st March, 2020, 21 confirmed cases were recorded. Thus by 21st April, 2020 the expected number of confirmed cases = 1024 x 21 = 21,504. Providing for mild and undetected cases (Which still add to the speed of the infection); using experts projected projections of 10 to 50 times confirmed case the range of infected individuals in a month times will between 215,040and 1,075,200 statistically speaking with 21,504 being confirmed cases. Figure 5 demonstrates that total number of confirmed cases in Qatar as on upto 27th March, 2020 is 562 and 43 were recovered. There has been no death record till yet in Qatar.
Discussion
Another example of the importance of animal-human interface infections is the current outbreak of the COVID-19 disease. And the issues resulting from the advent of a newly identifiedorganism as it spreads through individuals and across national and international frontiers. At the advent of an outbreak such as this, readily available data and information are equally important to begin the evaluation needed to understand the risks and start containment outbreak activities. Such information includes initial reports of countries with confirmed, death and recovered cases ratio, also, how the countries outside china are affecting, how the province of china are struggling to handle the situation of COVID-19 and more importantly ratio analysis of these real- world data, as well as information obtained from specific regions of globally from past outbreaks. Information and understanding of the consequences are needed to help refine the risk assessment as the outbreak continues and to ensure that patients are best managed. Much of this information emerges in real-time, challenges our understanding, yet refines our responses. The analysis presented here based on exploratory data analysis (EDA) and visual exploratory data analysis (V-EDA) with the help of the dataset provided by John Hopkins University, World Health Organization (WHO), Chinese Center for Disease Control and Prevention (CDC), National Health Commission (NHC), and DXY.Over the last two months, majority cases of a new infectious disease have been confirmed in China and other countries in Asia, Europe, Africa, and the Americas [27-30]. The COVID-19 is an emerging condition that primarily threatens the preparedness and biosecurity conditions of all countries on this planet [31].
Preparedness at different levels, facing a new clinical disease, demands efforts in epidemiological, diagnostic, therapeutic, and preventive fields during a potential pandemic [32], that threatens to spread to new territories (>115) and areas with the risk of epidemics.Clinical, laboratory, image findings, as well as the factors associated with evolution of the disease and outcomes, constitute critical knowledge that should be carefully studied when a new infectious disease emerges. Recently, in this context of the COVID-19 outbreak, several questions have been raised, including what is the full spectrum of disease severity (which can range from asymptomatic, to symptomatic-but-mild, to severe, to requiring hospitalization, to fatal)? [20] Up to now, regardless whether of report type (cross-sectional studies or case reports) the clinical findings are consistent, but more data are needed to define the risk factors for admission in ICU and for fatal outcomes. However, data suggest that older age and comorbidities play a vital role in influencing severe disease and negative clinical outcomes. These data would be useful to guide patient risk groups management in the current epidemic, especially in those countries about to receive cases, as is the situation in Latin America. COVID-19 cases have beenconfirmed in Brazil, Mexico, Ecuador, Argentina, Chile, Peru, Costa Rica, Dominican Republic, Paraguay, Colombia, Panama, Honduras, and Bolivia, among others, as of the time of writing [33]. Early recognition of cases will allow clinicians to ensure adequate clinical monitoring, institution of supportive interventions, and preventing further transmission by implementing of infection control measures. There is a need for prospective studies to evaluate the epidemiology, pathogenesis, duration of viral shedding, and the clinical spectrum of disease associated with this emerging viral infection [32-34]. Unlike SARS, with it is well-characterized twostage clinical course of the disease, COVID-19, still needs further definition [35]. The first week of the condition is also similar, coinciding with recent data of the viral load during this stage [36]. However, case-control studies and cohort studies are necessary to define the clinical evolution of disease better. A second stage, as occurs in SARS, is maybe also seen in COVID-19, with the lower respiratory tract bilateral compromise, observed in more than 72% of the patients across nine studies with more than 500 patients, also experiencing a dry cough, and dyspnea [4, 35, 10] and with chest X-ray images of ground-glass opacity frequently observed in two-thirds of patients – this is also seen in SARS [37].
Conclusion
In conclusion, the dataset we have used for our experiment 2019 Coronavirus dataset (January - February 2020), COVID-19 (nCOV-19) Corona Virus Spread Dataset, and Novel Corona Virus 2019 Dataset can be useful to monitor the emerging outbreaks, suchas 2019-nCoV. Such activities can help generate and disseminate detailed information to the scientific community, especially in the early stages of an outbreak when there is little else available, allowing for independent assessments of key parameters that influence interventions. We observe an interesting different case reported based on the different datasets of 2019-nCoV, which helps us to understand that it needs more epidemiological and serological studies. We also investigated early indications that the response is being strengthened in China and worldwide on the basis of a decrease in the case of detection time and rapid management of internationally identified travel-related cases. As a caveat, this is an early data analysis and visualization approach of a situation that is rapidly evolving. Using the trend line for different countries for their confirmed number of cases, we can predict their future cases. Further, we have identified the steps that leads towards the decreasing trend of the confirmed cases taken by China on othercountries whose trend line shows a decreasing trend with respect to time. We suggest all the affected countries should take steps like Lockdown, stay at home, testing more and more persons etc. such that the locations can be identify and the approach will be taken to defeat the COVID-19. Hopefully, in the coming weeks, we will continue to monitor this outbreak’s epidemiology data that we have used in this research and from other official sources.
References
- Zhu N, Zhang D, Wang W (2020) A Novel Coronavirus from Patients with Pneumonia in China, 2019. N Engl J Med 2020.
- Li Q, Guan X, Wu P (2020) Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N Engl J Med 382(13): 1199-1207.
- Lu R, Zhao X, Li J (2020) Genomic characterization and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet395(10224): 565-574.
- Huang C, Wang Y, Li X (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395(10223): 497-506.
- Chen N, Zhou M, Dong X, Qu J, Gong F, et al. (2020) Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet395(10223):507-513.
- Wang D, Hu B, Hu C, Zhu F, Liu X, et al. (2020) Clinical characteristics of 138 hospitalized patients with 2019 novel Coronavirus-infected pneumonia in Wuhan, China. JAMA323(11): 1061–1069.
- Biot C, Daher W, Chavain N (2006) Design and synthesis of hydroxyferroquine derivatives with antimalarial and antiviral activities. J Med Chem49(9): 2845-2849.
- Xueting Y, Fei Y, Miao ZIn Vitro Antiviral Activity and Projection of Optimized Dosing Design of Hydroxychloroquine for the Treatment of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2). 71(15):732-739.
- Zhou P, Yang X-L, Wang X-G, Hu B, Zhang L, et.al. (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature579(7798): 270-273.
- Yang X, Yu Y, Xu J (2020) Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med 8(5): 475-481.
- Munster VJ, Koopmans M, van Doremalen N, van Riel D, de Wit E (2020) A novel coronavirus emerging in China-key questions for impact assessment. N Engl J Med 382:692–694.
- Chan JF W, Yuan S, Kok KH (2020) A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet 395(10223):514-523.
- Weijie Guan, Zhengyi Ni, Yu Hu (2020) Clinical characteristics of 2019 novel coronavirus infection in China. MedRxiv.
- Lu H, Stratton CW, Tang YW (2020) Outbreak of pneumonia of unknown etiology in Wuhan China: the mystery and the miracle. J Med Virol 92(4):401-402.
- Ji W, Wang W, Zhao X, Zai J, Li X (2020) Homologous recombination within the spike glycoprotein of the newly identified coronavirus may boost cross‐species transmission from snake to human. J Med Virol.
- Samrat KD, Md Mahbubur R, Umme RS,Arpita H (2020) Analyzing the Epidemiological Outbreak of COVID-19: A Visual Exploratory Data Analysis (EDA) Approach. 92(6):632-638.
- Berkman BE (2008) Mitigating pandemic influenza: the ethics of implementing a school closure policy. J Public Health ManagPract 14(4):372-378.
- Baylis F, Kenny N, Sherwin S (2008) A relational account of public health ethics. Public Health Ethics 1(3):196-209.
- Raub A, Chung P, Batra P (2018) Paid leave for personal illness: a detailed look at approaches across OECD countries. World Policy Analysis Center.
- Lipsitch M, Swerdlow DL, Finelli L (2020) Defining the Epidemiology of Covid-19 - Studies Needed. N Engl J Med 382(13):1194-1196.
- Baharoon S, Memish ZA(2019) MERS-CoV as an emerging respiratory illness: A review of prevention methods. Travel Med Infect 32:101520.
- Liu Y, Chen H, Tang K, Guo Y. Clinical manifestations and outcome of SARS-CoV-2 infection during pregnancy. J Infect.
- Chen H, Guo J, Wang C, Luo F, Yu X, et al. (2020) Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: a retrospective review of medical records. Lancet395(10226):809-815.
- (2020) World Health Organization (WHO). Clinical management of severe acute respiratory infection when novel coronavirus (2019-nCoV) infection is suspected. Interim guidance. Geneva, WHO.
- (2020) Centers for Disease Control and Prevention (CDC). Interim guidance for discontinuation of transmission-based precautions and disposition of hospitalized patients with COVID-19. Atlanta, CDC.
- (2020) Novel coronavirus (SARS- CoV-2). Technical Report. Discharge criteria for confirmed COVID-19 cases. European Centre for Disease Prevention and Control (ECDC).
- (2020) Novel Coronavirus (2019-nCoV)Situation report. World Health Organization.
- (2020) Pneumonia of unknown cause World Health Organization.
- Dong E, Du H, Gardner L (2020) An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect Dis 20(5):533-534.
- (2020) Statement on the meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus (2019- nCoV). World Health Organization.
- Biscayart C, Angeleri P, Lloveras S, Chaves T, Schlagenhauf Pet al. (2020) The next big threat to global health? 2019 novel coronavirus (2019-nCoV): What advice can we give to travellers? - Interim recommendations January 2020, from the LatinAmerican society for Travel Medicine (SLAMVI). Travel Med Infect Dis 33:101567.
- Srikantiah P, Charles MD, Reagan S, Clark TA, Pletz MW, et al. (2005) SARS clinical features, United States, 2003. Emerg Infect Dis 11:135-138.
- RodriguezMorales AJ, Gallego V, EscaleraAntezana JP, Mendez CA, Zambrano LI, et al. (2020) COVID-19 in Latin America: The implications of the first confirmed case in Brazil. Travel Medicine and Infectious Disease 35:101613.
- Holshue ML, DeBolt C, Lindquist S, Lofy KH, Wiesman J, et al. (2020)First Case of 2019 Novel Coronavirus in the United States. N Engl J Med382(10): 929-936.
- RodriguezMorales AJ, MacGregor K, Kanagarajah S, Patel D, Schlagenhauf P (2020) Going global - Travel and the 2019 novel coronavirus. Travel Med Infect Dis33: 101578.
- Zou L, Ruan F, Huang M, Liang L, Huang H, et al. (2020) SARS-CoV-2 Viral Load in Upper Respiratory Specimens of Infected Patients. N Engl J Med382(12):1177-1179.
- Zhao W, Zhong Z, Xie X, Yu Q, Liu J (2020) Relation Between Chest CT Findings and Clinical Conditions of Coronavirus Disease (COVID-19) Pneumonia: A Multicenter Study. AJR Am J Roentgenol214(5):1072-1077.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...