Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Research Article(ISSN: 2641-1725) 
Prognosis Value of the Coma Glasgow and Four Scales in Patients with Severe Cranioencephalic Injury from Emergency Adults from the InstitutoAutonomo Hospital Universitario De Los Andes Merida Venezuela January - June 2018 Volume 5 - Issue 3
Camilo Estarling Cazorla Hernández*, Luis Andrés Dulcey Sarmiento, Jonathan Antonio Pineda Parada, Hector Alonso Moreno Parra, Jose Jorge SampayoZuletaCiro Alfonzo la Cruz
- Hospital Universitario de los Andes NivelMezanina Internal Medicine Service, Venezuela
Received: August 12, 2020; Published: August 21, 2020
*Corresponding author: Camilo EstarlingCazorla Hernández Hospital Universitario de los Andes NivelMezanina Internal Medicine Service,Mérida Venezuela
DOI: 10.32474/LOJMS.2020.05.000212
Abstract
Objectives: To establish the prognostic role of the Glasgow and FOUR coma scales in patients with severe cranioencephalic trauma of the adults emergency of the autonomous university hospital of the andesmeridavenezuela January - June 2018. Materials and Methods: Prospective, field and longitudinal cut. We selected those patients older than 18 years with a diagnosis of cranial encephalic trauma, the corresponding variables were evaluated in each patient of the sample.
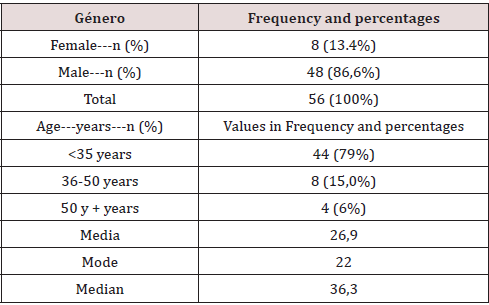
Results: 56 patients 86.6% men and 13.4% women, the average age was 26.9 years, the largest age group corresponded to those under 35 years, 44 (79%), the traffic accidents were the the main cause of head brain trauma 49 (87%), cerebral edema was the main tomographic finding, all neurotomographic findings showed statistical significance. Total mortality was 12 (21%) patients out of 56. Neurosurgical interventions were performed in 8 patients with a mortality of 5 (62.5%), (p <0.001). The Glasgow score in the live group was 9 compared to 6 points in the deceased subgroup (p <0.001). The correlations between tests were D of Somers (0.89), Gamma (0.91) and Tau-b Kendall (0.86).
Conclusion: There was an adequate correlation between the scales, there being the advantage of the FOUR scale in being able to evaluate the stem reflexes.
Keywords: Craniocerebral trauma; mortality; brain tomography; glasgowscale; four scale
Introduction
Brain trauma is a condition that man has suffered since it first appeared on the world1. Hippocrates (460-377 BC), was a pioneer in the treatment of skull injuries. In his treatise entitled: “On head injuries” a typical example of how the Hippocratic method led to the exact observation of the anatomy of the skull and its injuries is observed. References to craniotomy have also been found in the Egyptian papyrus of Edwin Smith and George Ebers.In the 1970s, with the care of these patients in Intensive Care Units, with the introduction into clinical practice of intracranial pressure monitoring (ICP) and later other monitoring techniques, treatment of these was carried out for the first time. patients from a scientific point of view knowing in real time each of the pathophysiological events that occurred in their evolution, and then treating them in a more rational way, giving rise to what is known as neurointensive management of specifically severe head trauma. With the advent of these techniques, mortality from this pathology has been reduced to figures that range from 20 to 45% 2. In more than 50% of patients with severe head trauma, intracranial pressure is elevated, and these uncontrolled increases are the main cause of mortality and permanent injury to the event[1,2].Scales have been developed to measure the state of consciousness and prognosis in ECG, of which the largest are the Glasgow Coma Scale (ECG) and the FOUR Coma Scale (EF). The ECG for coma has been adopted in a generalized way, despite presenting limitations, among which are the impossibility of assessing verbal response in intubated or aphasic patients, and the absence of assessment of brainstem reflexes, which provide important prognostic information[3,4]. Due to the limitations of the ECG, the PE has been designed for coma, which includes four components: ocular response, motor response, trunk reflexes and breathing, each of which scores from 0 to [3]. The total score can take therefore values between 16 (conscious) and 0 points (arreactive coma without brainstem reflexes). The FOUR scale has been validated by its authors, with a good agreement between observers and a linear relationship with mortality, also allowing different degrees of affectation to be distinguished between patients with low scores on the Glasgow scale[5-7]. Among the theoretical advantages of the FOUR scale are its ability to detect the “cloistered syndrome” as well as different stages of brain herniation. Attempts have been made to modify the GCS, however, in most of these scales the use is more complicated. Due to the above, the FOUR scale arises, this scale that could provide more detail in coma, is easy to use and can predict results(Tables 1-3).The ECG is the most used so far worldwide, however there are studies that have shown difficulty in applying it in intubated patients, so the verbal component cannot be tested. Some doctors use the lowest possible score, others do not take the verbal response on the basis of other neurological disorders. Second, the abnormal brainstem reflexes, changing breathing patterns, and the need for mechanical ventilation could reflect the severity of the coma, but the ECG does not include clinical indicators. Third, ECG cannot detect subtle changes on neurological examination[8-11].Due to the aforementioned, we propose to evaluate the prognostic value of both ECG and EF scales in patients with a diagnosis of severe head trauma admitted to the adult emergency area of the Autonomous Institute Hospital Universitario de Los Andes Mérida Venezuela in the period from January to June of 2018.
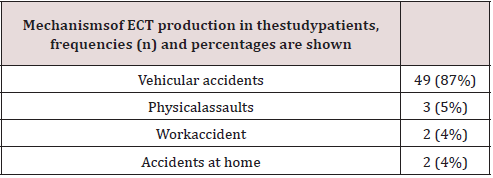
Table 2: Mechanisms of ECT production in thestudypatients, frequencies (n) and percentages are shown.
Objectives of The Study
Overall objective
Establish the prognostic value of the Glasgow and FOUR coma scales in patients with severe head trauma in the adult emergency of the autonomous institute hospital universitario de los Andes Merida Venezuela January - June 2018
Specificobjectives
a. Describe the sociodemographic variables of the patients.
b. Describe the mechanism of head injury
c. Describe the neurotomographic findings through the
Marshall scale during the follow-up period.
d. Describe the need for neurosurgical intervention in the
patients included in the study.
e. Evaluate the time of use of mechanical ventilation during
the first 7 days.
f. Describe the mortality of patients with head trauma.
5. Methodological Framework
Design of the investigation
Observational, analytical prospective study
Populationand Sample
All patients over 18 years of age of both genders with a
diagnosis of severe head trauma who were admitted to the IAHULA
Emergency Room, in the period from January to June 2018.
A. Inclusion criteria
a. Patient with severe head injury.
b. Both genres.
c. Entry during the first 24 hours of the event.
B. Exclusioncriteria
a. Open head trauma
b. Demonstrated Brain Death
c. Known liver disease
d. Chronic renal insufficiency
e. and. Heart failure
f. Mellitus diabetes
g. Diagnosed neoplasms.
h. Spinal cord trauma
VariablesSystem
The following baseline information will be evaluated in the patients included in the study.
Demographicvariables
a. Age
b. Gender
c. Origin
d. Occupation
Dependentvariables
a) Mechanism of head trauma
b) Mortality in the first 7 days
5.6. Independentvariables
a. Scores of the Glasgow and FOUR scales
b. Assisted mechanical ventilation
c. Death
Results
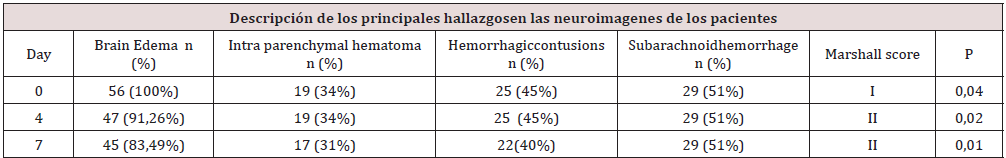
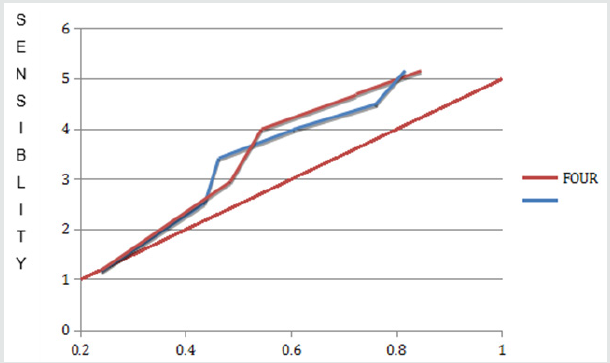
56 patients with clinical criteria for severe head trauma by the Glasgow scale who were admitted to the adult emergency service of IAHULA-in the city of Mérida were included. 86.6% (n: 48) corresponded to the male gender, the remaining 13.4% (n: 8) corresponded to the female gender.The distribution by age groups was carried out in three groups: under 35 years, 36 - 50 years and 50 or more years.According to the clinical records evaluated, the main mechanism of appearance of ECT corresponded to vehicular accidents with 87%, followed by physical aggressions with 5%, in third place work accidents 4% and with the same frequency home accidents 4%.The present graph below shows the distribution by frequencies and percentages of the patients in the sample according to the month in which the patient entered the study. Statistical significance was evaluated with the Chi square test or Student’s t test respectively. Values of p <0.05 were considered statistically significant.It was observed that upon admission, cerebral edema was present in the entire sample, subarachnoid hemorrhage was also observed in 29 (51%) patients, hemorrhagic contusions in 25 (45%) patients and parenchymal hematoma in 19 (34%) patients. All showing statistical significance (0.04). On day 4, it was observed that the cerebral edema decreased to 47 (91.26%), the subarachnoid hemorrhage remained the same percentage compared to admission, the hemorrhagic contusions were maintained in terms of frequency and the intraparenchymal hematoma remained the same. proportion compared to income with one (p 0.02), the Marshall mode was II.Finally, on day 7, the number of patients with cerebral edema decreased to 45 (83.49%), the subarachnoid hemorrhage remained, hemorrhagic contusions also decreased to 22 (44%) and in the case of intraparenchymal hematomas it decreased to 17 ( 31%), all these correlations showed statistical significance (p 0.027) and the Greene mode was maintained compared to day 4.The following graph shows the number of patients who required neurosurgical intervention by percentage.Student’s t test with significance p <0.05. Chi square test with significance p <0.05, CI = confidence interval of the OR with a reliability of 95%.As could be seen, 12 (22%) deaths occurred, the mean age being greater in this group compared to the group of living patients, this finding showed a fairly important statistical significance (<0.001). Regarding gender, the highest frequency of events occurred in the group of males, with percentages greater than 90% for both living and deceased (<0.001).Regarding the association between days of mechanical ventilation and mortality, the mean was 6.8 days for the group of deceased and 4.6 days for the group of living patients with a statistical significance of (p 0.046).The neurosurgical intervention variable was performed in 8 patients, with a higher mortality in this group of patients 5 (62.5%), with a value of p <0.001. The Glasgow score in the living group was 9 compared to 6 points in the deceased subgroup, the p value for this variable was <0.001.The FOUR score in the living group was 13 compared to 8 points in the deceased subgroup, the p value for this variable was <0.001.The ROC curve analysis showed that the FOUR scale was superior to the Glasgow scale in terms of sensitivity 0.88 vs. 0.84 and specificity 0.92 vs. 0.87.The scales were compared through the Somers D tests (0.89), Gamma (0.91) and Kendall’s Tau (0.86), through the 3 a good to excellent correlation was observed between both 2 scales.
Analysis and Conclusion
Once the results of our study have been presented, we can
conclude and infer the following. Regarding the distribution by
gender, the male gender group was much higher, the largest age
group was made up of those under 35 years of age, this finding agrees
with that found in other studies such as that of Chicote et al[12-14]
where the population it is mostly young people of productive ages.
The main generating mechanism of the TEC corresponded to road
events of any kind, which is consistent with studies carried out in
other latitudes such as that of Stolwyk and collaborators[15] where
it was observed that the main mechanism producing the TEC is
secondary to automobile accidents.Regarding the distribution by
time of year, a higher frequency was observed during the months
of March and June 2018, some authors have shown the association
of alcohol consumption with this type of events and it was also
determined as a factor with a worse prognosis[16].The main
finding observed in the skull tomographies of the patients in our
study corresponded to cerebral edema as a consequence of the
ECT, followed by subarachnoid hemorrhage, later hemorrhagic
contusions and finally intraparenchymal hematoma, additionally
the mode of the Marshall score to evaluate the tomography it was
II on admission and IIIA for days 4 and 7, the findings found in
the tomography are consistent with those found in the study by
Mariños[17], where the main finding was the Marshall II.For the
variable need or not for neurosurgical intervention in the first 7
days, it was observed that only 8 of the 56 patients of which 5 were
performed on the 4th day and 3 of them on the 7th day of the event, no
patient was operated on in the day of admission, these findings are
consistent with the review by Dr. Morrison[18] of 22,229 patients
over a 10-year period in Pennsylvania, where the proportion of
patients operated on is close to 10% of admissions with severe ECT,
results very similar to our study.Finally, it was observed that among
the factors associated with mortality in the patients in our study,
the mean age was 24.6 years for the group of the living and 38.9
years for the group of the deceased, finding a statistical correlation
of higher mortality in the oldest age groups, as seen in the study
by Murray[19] and collaborators. There was a higher mortality
in the male gender related to thehigher frequency of this type of
event with motorcycle driving.A higher mortality was observed in
the group that underwent a longer mechanical ventilation time 6.5
days compared to the group that only stayed 4.3 days, this finding
agrees with that reported by Omar[20] and collaborators where
the longer the mechanical ventilation time the longer were the
complications for these patients.For the neurosurgical intervention
variable, it was observed that only 3 of the patients who underwent
this behavior survived and the remaining 5 died, this finding can
be inferred that it is a consequence of the greater severity of the
lesions and the prognosis of the group of patients operated as has
been validated in studies such as that of Owens[21] carried out in
Ireland where mortality was much lower, only 12% compared to
the 21.35% reported in the present study.
Finally, it can be seen that the group of patients who survived
had a Glasgow mean of 9 compared to the group of the deceased,
where the mean was 6 with a p value <0.001, this finding is correlated in the study by Roccheti and collaborators[22], where
the Glasgow score below 10 points was correlated as a determining
variable of mortality. Also demonstrated that neurological score
influences prognosis. [23] Demonstrated the advantages of an
early decompressive craniectomy in the management of these
complications.The analysis in the ROC curve showed that the FOUR
scale was more sensitive (0.88 vs 0.84) and specific (0.92 vs 0.87)
than the Glasgow to define prognosis and mortality in the statistical
analysis performed[24].
Recommendations
a. Expand the medium and long-term follow-up to observe
complications in patients with head trauma.
b. Expand the sample of patients in order to improve the
statistical power of this study and to be able to carry out a
multicenter study, including highly complex hospital centers in
other latitudes.
c. Sensitize adult emergency service personnel regarding
the high mortality rate and the prognostic implications of the
TEC.
d. Generate guidelines in the management of these patients
to improve their prognosis and reduce morbidity and mortality
in head trauma.
e. Implement traffic accident prevention programs and also
explain to the population the potential risks of the association
between driving some type of vehicle combined with alcoholic
beverages.
f. Establish in the clinical practice of the Adult Emergency
Service tools to assess the risk stratification of these patients,
establishing an adequate prognosis.
g. Continue with related research in the line of head trauma.
h. Carry out neuroimaging studies at the most opportune
moment for the patient, prioritizing their stabilization.
i. Coordinate actions with other services so that the
multidisciplinary management of these patients improves the
results in terms of morbidity and mortality.
j. We recommend the use of the FOUR scale in the evaluation
of patients with a diagnosis of head trauma as an alternative to
the Glasgow scale.
References
- AlMufti F, Amuluru K, Lander M, Mathew M, ElGhanem M, et al. (2018) Low Glasgow Coma Score In Traumatic Intracranial Hemorrhage Predicts Development Of Cerebral Vasospasm. World Neurosurg 120: e68-e71.
- Kasprowicz M, Burzynska M, Melcer T, Kübler A (2016) A comparison of the Full Outline of UnResponsiveness (FOUR) score and Glasgow Coma Score (GCS) in predictive modelling in traumatic brain injury. Br J Neurosurg30(2):211-220.
- Leitgeb J, Mauritz W, Brazinova A, Majdan M, Wilbacher I (2013) Impact of concomitant injuries on outcomes after traumatic brain injury. Arch Orthop Trauma Surg133(5):659-668.
- Roberts I, Shakur H, Coats T, Hunt B, Balogun E, (2013) The CRASH-2 trial: a randomised controlled trial and economic evaluation of the effects of tranexamic acid on death, vascular occlusive events and transfusion requirement in bleeding trauma patients. Health Technol Assess17(10):1-79.
- Wijdicks EF, Bamlet WR, Maramatton BV, Manno EF, McClellanel RL (2006) Validation of a new coma scales the FOUR score. Annals of Neurology.
- Wijdicks EF, Bamlet WR, Maramatton BV, Manno EF, McClellanel RL (2007) Validation of a new coma scales the FOUR score. Annals of Neurology 58(4): 585-593.
- Bruno MA, Ledoux D, Lambermont B, Damas F, Schnakers C, et al. (2011)CuidadoNeurocut. 15 (3): 447-453.
- Sadaka F, Patel D, Lakshmanan R (2012)CuidadoNeurocut. 16 (1): 95-101.
- Okasha AS, Fayed AM, Saleh AS (2014) The FOUR score predicts mortality, endotracheal intubation and ICU length of stay after traumaticbrain injury. Neurocrit Care21(3):496-504.
- Heim C (2014) Is trauma in Switzerland any different? epidemiology and patterns of injury in major trauma - a 5-year review from a Swiss trauma centre. Swiss Med Wkly144:w13958.
- Teasdale G, Maas A, Lecky F, Manley G, Stocchetti N, et al. (2014) The Glasgow Coma Scale at 40 years: standing the test of time. Lancet Neurol 13(8):844-854.
- Wintermark M, Li Y, Ding VY, Xu Y, Jiang B (2018) Neuroimaging Radiological Interpretation System for Acute Traumatic Brain Injury. J Neurotrauma 35(22): 2665-2672.
- Chicote Álvarez E, González Castro A, Ortiz Lasa M, Jiménez Alfonso A, Escudero Acha P, et al. (2018) Epidemiology of traumatic brain injury in the elderly over a 25 year period. Rev EspAnestesiolReanimS0034-9356(18): 30115-30124.
- Stolwyk RJ, Charlton JL, Ross PE, Bédard M, Marshall S, Gagnon S, et al. (2018) Characterizing onroad driving performance in individuals with traumatic brain injury who pass or fail an on-road driving assessment. DisabilRehabil 41(11): 1313-1320.
- Gerritsen H, Samim M, Peters H, Schers H, van de Laar FA (2018) Incidence, course and risk factors of head injury: a retrospective cohort study. BMJ Open8(5):e020364.
- Maycol Santos MariñosMariños (2018)Hallazgostomográficosenpacientes con traumatismocraneoencefálicosegún la clasificación de Marshall, en el Hospital Nacional Hipolito Unanuejunio – diciembre 2014 Lima – Perú [Internet]. Universidad nacional mayor de San Marcos facultad de medicina: E.A.P. de tecnologíamédicaFecha de publicaciónDisponibleen.
- Morrison CA, Gross BW, Cook AD, Estrella L, Gillio M, (2016) An analysis of neurosurgical practice patterns and outcomes for serious to critical traumatic brain injuries in a mature trauma state. J Trauma Acute Care Surg80(5):755-761.
- Murray GD, Brennan PM, Teasdale GM (2018) Simplifying the use of prognostic information in traumatic brain injury. Part 2: Graphical presentation of probabilities. J Neurosurg128(6):1621-1634.
- Omar M, Moore L, Lauzier F, Tardif PA, Dufresne P, et al. (2017) Complications following hospital admission for traumatic brain injury: A multicenter cohort study. J Crit Care41:1-8.
- Owens PW, Lynch NP, O'Leary DP, Lowery AJ, Kerin MJ (2018) Six-year review of traumatic brain injury in a regional trauma unit: demographics, contributing factors and service provision in Ireland. Brain Inj32(7):900-906.
- Rocchetti NS, EgeaGuerrero JJ, Ruiz de AzuaLopez Z, MartinVillen L, RodriguezRodriguez A, et al. (2018) APACHE II and SAPS II as predictors of brain death development in neurocritical care patients. Rev Neurol 67(4):121-128.
- Ziaeirad M, Alimohammadi N, Irajpour A, Aminmansour B (2018) Association between Outcome of Severe Traumatic Brain Injury and Demographic, Clinical, Injury-related Variables of Patients. Iran J Nurs Midwifery Res23(3):211-216.
- Khan AD, Elseth AJ, Head B, Rostas J, Dunn JA, et al. (2017) Indicators of Survival and Favorable Functional Outcomes after Decompressive Craniectomy: A Multi-Institutional Retrospective Study. Am Surg83(8):836-841.
- Drake SA, Holcomb JB, Yang Y, Thetford C, Myers L, et al. (2018) Establishing a Regional Trauma Preventable/Potentially Preventable Death Rate. Ann Surg 271(2): 375-382.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...