
Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Case Report(ISSN: 2641-1725) 
In-toto Removal of an Intermuscular Myxoma of the Harmstring Compartment of the Thigh Volume 3 - Issue 5
Herry Herman*, Ricky Wibowo, Naseh Sajadi M Budi Irawan and Darmadji Ismono
- Department of Orthopaedic Surgery and Traumatology, Faculty of Medicine, Universitas Padjadjaran, Indonesia
Received: October 24, 2019; Published: October 29, 2019
*Corresponding author: Herry Herman, Department of Orthopaedic Surgery and Traumatology, Faculty of Medicine, Universitas Padjadjaran, Hasan Sadikin General Hospital, Jl. Pasteur 38, Bandung, West Java 40161, Indonesia
DOI: 10.32474/LOJMS.2019.03.000175
Abstract
Introduction: Myxoma is a rare benign soft tissue tumor derived from mesenchymal cells, composing of fibroblasts and abundant myxoid matrix. The incidence is approximately from 0,1 to 0,13 per 100,000 populations with the heart as its main site of involvement. Most are of intramuscular in nature, very rarely was it intermuscular Characterized by a slow progression painless mass, the main choice of treatment is radical excision of the whole tumor.
Case presentation: We reported a case of a 23-year-old female with a right lower gluteal painless mass arising insidiously over the course of three years. A perioperative magnetic resonance imaging revealed a well-circumscribed lobular cystic tumor measuring 15x10x13cm in size on the posteromedial aspect of the proximal part of the right thigh. Surgical excision of the tumor revealed its intermuscular location, with characteristic histopathology of a myxoma. Postoperative evaluation at 3 and 12 months showed no evidence of recurrence and a return to functional daily living without obvious limitation.
Conclusion: Intermuscular myxoma of the thigh is a very rare variation of the already rare type of a benign tumor of mesenchymal origins. Its complete in-toto removal assures a recurrence free procedure and preservation of satisfactory muscle function.
Keywords: ntermuscular Myxoma; Hamstring compartment of the thigh; surgical excision
Introduction
Myxoma is a rare benign soft tissue tumor arising from mesenchymal cells, composing of fibroblasts and an abundant myxoid matrix. It is characterized by slowly progressing and painless mass. Most Myxomas occurs between the fourth and seventh decades of life with female predominates in occurance (70%). The incidence is approximately 0,1 to 0,13 per 100.000 population [1]. The most common tumor predilection is the cardiac muscle, followed by the large muscles of the thigh, shoulder, buttocks, and arms [2, 3].
Myxomas may frequently be found together with fibrous dysplasia of the bones such as in Mazabraud’s or in McCune- Albright syndromes. Treatment of choice for muscle associated myxoma is a radical excision of whole tumor [4].
Case Presentation
Figure 1: Clinical presentation of the mass on right thigh posterior aspect. Left. Posterior view, Rigth. Lateral view.
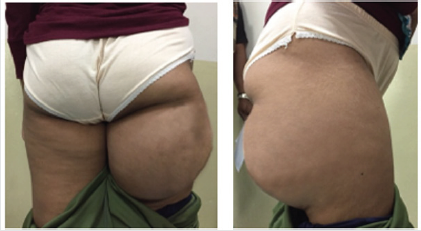
A 23-year-old female presented with a painless progressive mass in the posterior aspect of the right proximal thigh over the course of three years, causing an increasing discomfort during sitting. Physical examination revealed a well-defined mass, firm in consistency, mobile, non-tender, approximately 15x15 cm in size, without any skin pigmentation or skin breakdown (Figure 1). Hip and knee range of motion were not affected as well as no distal neurovascular deficit was found.
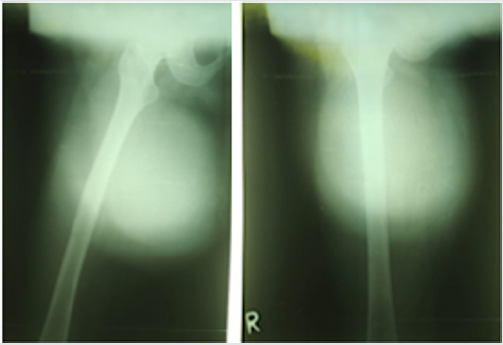
Femur plain X-ray revealed a huge well-circumscribed lobulated solid tumor at the proximal thigh, with well-defined margin without periosteal reaction (Figure 2). Laboratory findings were within normal limits.
Figure 2: Plain X-ray showed huge soft tissue tumor at proximal femur, Left. AP view, Right. Lateral view.
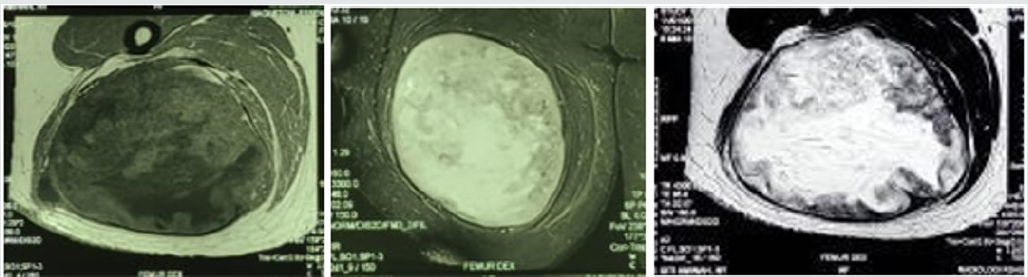
Magnetic Resonance Imaging (MRI) revealed a cystic, wellcircumscribed lobular tumor measuring 15x10x13 cm in size. A T1-weighted image showed the tumor as a well-circumscribed inhomogeneous, hypo-intense, regular edged, predominantly cystic mass that was opaque on T2-weighted image, signifying a possible watery (myxoid) content. The mass was located in posteromedial aspect of of the proximal part of the right femur, compressing but not infiltrating the biceps, semimembranosus, semitendinosus, and adductor magnus muscles, pointing toward its presumed location in-between the adductor and the harmstring compartment of the thight. No infiltration to the bone and neither involvement of the neurovascular bundle was noticed. On the contras-enhanced MRI, the tumor was shown to be heterogeneous, with an enhancement presumably due to an abundance of vascularity within its matrix. We reckoned that we were dealing with a muscle associated tumor, myxoid in matrix, representative of a myxoma (Figure-3). We predicted that it may well be an intramuscular myxoma of the biceps femoris muscle, a major muscle of the harmstring compartments. We preoperatively planned to do an in-toto removal of the containing biceps femoris muscle along with the tumors.
Figure 3: MRI of the right thigh Left.T1 Sagittal View, Center.T2 Sagittal View, Right. T2 Sagittal View + contrast.
We decided to perform an excision of the mass and was planning for a one step complete removal of the tumour. With the patient in prone position under general anesthesia, a lazy S-shaped incision was made from the right ischium to the insertion of the biceps muscle on the posterolateral aspect of the popliteal encompassing the whole length of the biceps femoris muscle. The tumour was found to be an encapsulated pocket of mass in between and separable from the adductor and the hamstring muscles compartments without infiltration to the muscles of either compartments or to the bone. It was located in the intermuscular plane between the biceps femoris muscle and the semimembranosus muscle. Intraoperatively the tumour was found to compress but did not infiltrate the sciatic nerve (Figure 4). The sciatic nerve was meticulously dissected and separated from the tumor with a safe margin. On gross examination, the tumour was consisted of a well-circumscribed, encapsulated soft cystic gray-brown tumor approximately 15x10x13 cm in size.
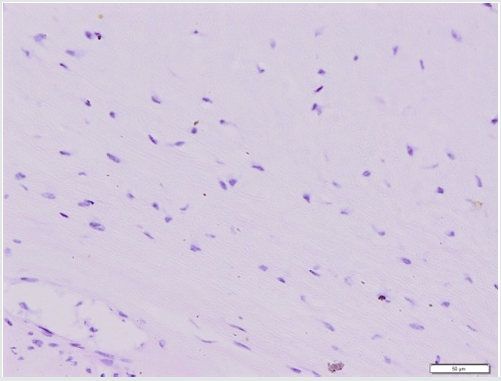
Microscopic examination revealed an abundant mucoid matrix with relative hypocellularity of benign spindle cells with no distinctive sign of malignancy (Figure 5).
Figure 4: Left. Intra operative finding following dissection Center. After tumor removal, sciatic nerve was preserved. Right. encapsulated mass sizing 15x13x10 cm.
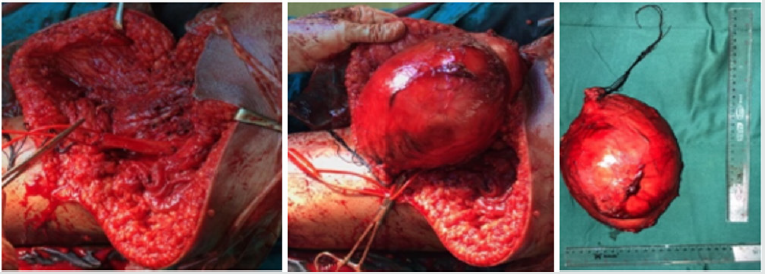
Figure 5: Histopathology examination showed spindle-and stellate shape cells, separated by an abundance of extracellular myxoid matrix.
Early Post operation, no neurological deficit was reported. Subsequent follow up 3 months (Figure 6) and 12 months (Figure 7) postoperatively revealed no evidence of relapse, or wound problem and a return to functional daily activities.
Figure 6: 3 Month after surgery. Left. Range of motion hip extension and knee extension. Rigth. Range of motion hip flexion and knee flexion
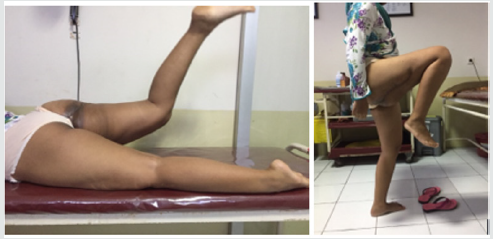
Figure 7: 12 Month after surgery. Left. Range of motion hip extension and knee extension, Center. Range of motion hip flexion and knee flexion, Right. Appearance of scar at post-operative month 12th.

Discussion
Myxoma is a rare benign tumor of mesenchymal origin consisting of undifferentiated stellate cells with myxoid matrix. Women are more commonly affected than men with the cardiac muscle being the most common site of predilection. More than half of all myxomas can be found in the thigh muscles. The characteristic presentation is a slowly growing painless tumor with an average size tumor between 1.5 and 17 cm. Myxoma usually occurs Intramuscularly as an isolated tumor, but may occur as a multiple myxomas associated with fibrous dysplasia of the bone in Mazabraud’s syndrome or in McCune-Albright syndrome accompanying the presence of polyostotic fibrous dysplasia, café-au-lait spots, and precocious adolescence [4-6]. Intermuscular myxoma, such as the one we reported here was even scarcer in occurence, our search of PubMed identified only one other publication from Russia dating back to 2006 [7].
While X ray, may not be of much of help to identify myxoma, except for an intraosseous location, soft tissue myxoma may readily be identified by MRI; which may reveal its cystic, well defined encapsulated organization, predominantly occupied by watery matrix identified as an hyperintense image on T2 weighted MRI. MRI will also pinpoint to the location of myxoma relative to involved muscle compartments; In our case, the predicted intercompartmental location, was actually found to be intermuscular instead. Histopathology provide definitive diagnosis for the tumor, revealing the distinctive sparsely separated spindle or stellate cells, swamped by the abundantly produced myxoid matrix.
Surgical management of myxoma, shall be directed at achieving a complete excision with safe margins, to prevent residual mass, recurrence or malignant transformation [4,8]. Our case illustrates this principle nicely, with healed wound, absence of recurrence while still preserving satisfactory muscle activity to allow the return to routine daily activities.
References
- Fletcher CD (2013) WHO Classification of Tumours of Soft Tissue and Bone. Fourth Edition. p. 193-197.
- Allen PW (2000) Myxoma is not a single entity: a review of the concept of myxoma. Ann Diagn Pathol 4(2): 99-123.
- Reynen K (1995) Cardiac myxomas. N Engl J Med 333(24): 1610-1617.
- Logel RJ (1976) Recurrent intramuscular myxoma associated with Albright’s syndrome. J Bone Joint Surg Am 58(4): 565-568.
- Szendroi M (1998) Fibrous dysplasia associated with intramuscular myxoma (Mazabraud’s syndrome): a long-term follow-up of three cases. J Cancer Res Clin Oncol 124(7): 401-416.
- van der Wal WA, Unal H, de Rooy JW, Flucke U, Veth RP (2011) Fibrous dysplasia of bone associated with soft-tissue myxomas as well as an intra-osseous myxoma in a woman with Mazabraud’s syndrome: a case report. J Med Case Rep 5: 239.
- Chikoteev SP, Shanturov VA, Andreeva NI, Gumerov RR (2006) [Intermuscular myxoma of the pelvis]. Khirurgiia (Mosk) 11: 63-64.
- van Roggen JF, McMenamin ME, Fletcher CD (2001) Cellular myxoma of soft tissue: a clinicopathological study of 38 cases confirming indolent clinical behaviour. Histopathology 39(3): 287-297.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...




