Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Research Article(ISSN: 2641-1725) 
Clinical Effects of Poly Flexible Ureteroscopy Combined with Ultrasound Guided All Seeing Needle Microperc to Treatment of Lower Pole Renal Calculi Larger than 2cm With Infundibulopelvic Angle Less than 60Degrees Volume 4 - Issue 4
Jingyang Guo*, Wen Zeng Yang, Yanqiao Zhang, Xiangyang Lin, Deqiang Gu and Feng AN
- Department of Urology, Affiliated Hospital of Hebei University, China
Received: January 28, 2020; Published: February 05, 2020
*Corresponding author: Jingyang Guo, Department of Urology, Affiliated Hospital of Hebei University, China
DOI: 10.32474/LOJMS.2020.04.000194
Abstract
Objective: To observation on Poly- Flexible Ureteroscopy (FURS) retrograde intrarenal surgery (RIRS) combined with ultrasound guided all seeing needle Microperc to treatment of Lower Pole Renal Calculi larger than 2cm stone with infundibulopelvic angle (IPA)less than 60 degrees.
Method: From January 2016 to January 2017, 63 patients with IPA angle less than 60 degrees in our hospital were treated with Poly-FURS retrograde intrarenal surgery combined with ultrasound guided all seeing needle Microperc, the patients stone sized more than 2 mm and located in the lower-pole calyx were retrospectively reviewed. Multiple stones were found in 37 cases and solitary stones in 26. Male patients used 70cm Poly-FURS, and the female 42cm.The clinical data including the operation time, the amount of bleeding, the stone free rate (SFR), the incidence of postoperative complications.
Results: The operation time was 30~60min, mean 45min, FURS lithotripsy time was 20~35min, ultrasound guided all seeing needle puncture time was 3~5min, and lithotripsy time was 8~12min. 48 cases mainly lithotripsy with FURS and 15cases with micro-Percutaneous nephrolithotomy(micro-perc), 3 cases of fever as postoperative complications, 2 cases of pain; In non-blood transfusion patients. The postoperative hospital stay was 2~3 days, with an average of 2 days. Postoperative residual stones were observed in 3 cases (SFR 95.2%) and treated with ESWL after 2 weeks. The stone clearance rate was 98.4% (62/63) after one month.
Conclusion: The results of our study demonstrated that Poly-FURS retrograde intrarenal surgery combined with ultrasound guided all seeing needle Microperc had a significant effect on the success rate of lower Pole Renal Calculi larger than 2cm.
Keywords: Poly-Flexible Ureteroscopy; Ultrasound guided; Micro PCNL; Lower Pole Renal Calculi; Infundibulopelvic angle
Introduction
from treatment of stones in other parts of the kidney, stones in the place should be completely cleaned up, because of infundibular, residual stones removal is difficult even the volume is very smaller [1]. With the continuous maturity and development of minimally invasive techniques, the technique of FURS is more and more widely used in clinic practice, and it has the trend of gradually replaced percutaneous nephrolithotomy in the treatment of small volume stones. The development of FURS equipment makes it more flexible, and the bending angle of the end becomes more and more bigger. It is an effective method for the treatment of Lower Pole Renal Calculi [2], but the degree of the IPA directly affects the effect of FURS. if the IPA is less than 30 degree, it is very difficult for the simple FURS [3]. Because it is very difficult to reach all the stone location, and powdered completely, we used Poly-FURS RIRS combined with ultrasound guided all seeing needle Microperc is a safe and effectiveness and had an ideal SFR, the report is as follows:
Materials and Methods
Patients data
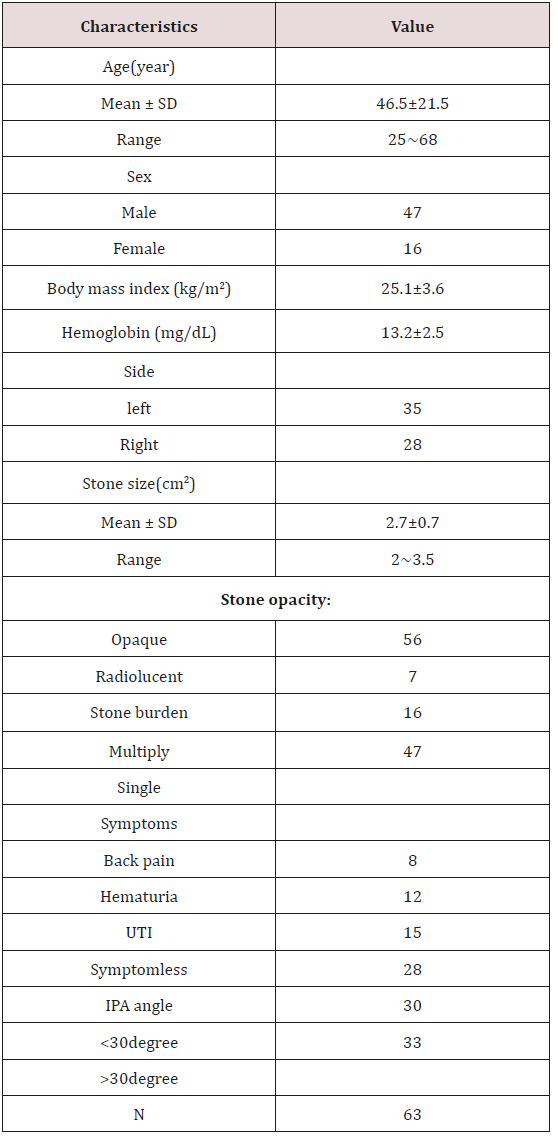
Inclusion criteria: Except for serious heart and lung diseases; urine analysis normal or urinary tract infection well controlled; preset DJ stent two weeks before surgery; Lower Pole Renal Calculithe stone diameter larger than 2cm, infundibulopelvic angle less than 60 degrees. A total of 63 patients, aged 25~68 years old, average 46.5; male 47 cases, female 16 cases; 35 cases of left renal calculi and 28 cases with right kidney stones; stones diameter 2~3.5cm, average 2.7cm, including 7 cases of X-ray negative calculi; 16 patients with multiple calculi, solitary stones in 47 cases; hematuria 12 cases, 15 cases of urinary tract infection, 8 cases of pain, no symptoms in 28 cases; IPA (Figure 1) 30~60 degrees in 33 cases, less than 30 degrees in 30 cases (Table 1) patient information.
Preoperative preparation
Before surgery, all patients were evaluated routinely with urinalysis, urine culture, coagulation tests, complete blood count, serum biochemistry and intravenous urography (IVU). Stone length was calculated on preoperative kidney-ureter-bladder (KUB) X-ray, CT imaging, ultrasonography, two weeks before surgery pre indwelling double J stent. Prophylactic antibiotics were started 30min before the procedure.
Surgical technique
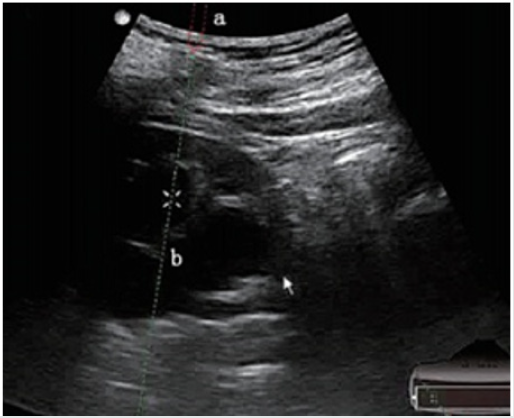
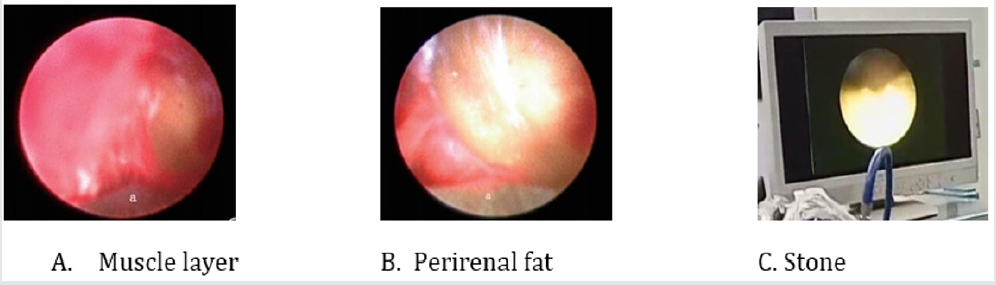
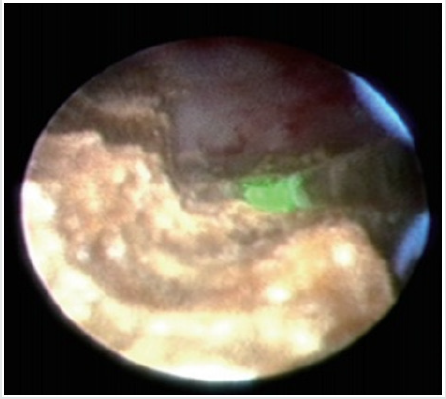
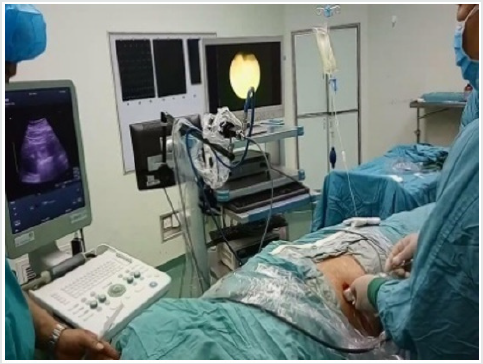
All patients were operated under general anesthesia by one experienced surgeon, supine lithotomy position, Trendelenburg, ipsilateral waist pad. FURS: Firstly, the zebra guide wire was implanted with rigid ureteroscope, meanwhile the ureter was observed to determine whether there was any complication such as stenosis, tumor or not. After successful indwelling guide wire, exit ureteroscopy and inserted urethral access sheath (UAS), followed by the application of 28cm sheath and 42cm FURS (poly flexible Mikroendoskop, Germany) for female, of 46cm sheath and 70cm FURS for male After the calculus was found, the stone was powedered by holmium laser fiber. the double J stent were retained though the UAS. Ultrasound guided all seeing needle Microperc: the visual puncture was carry on all seeing needle, under the ultrasound guidance to the target renal calyx (ultrasound and the screen double display 1) The puncture was selected generally at the 11 intercostal, 12 Rib tip as the point in the center of the circle 4cm range. Ultrasonic testing for the closest distance to the stone, precise puncture required (Figure 2) By mean of the process, pressure water injection through the water channel the puncture level and the stone site was clearly observed (Figure 3). Then indwelling guide wire exits the needle and expands the access to the F4.8 with a fascia expander. The F4.8 working sheath was placed and put into the 200um holmium laser fiber, and the stone was powdered (Figure 3). The Urinary catheter is retained. After the second day an evaluation of KUB or CT is done to observe the effect of the operation and DJ tube position, if no obvious complications existed. The catheter will be removed one day after post operation, discharged 2 days after operation and reassessment after 1month then the DJ stent removed.
Statistical analysis
Data analysis was performed using SPSS 16.0 software, all variables were expressed as mean ± standard (± S). Differences in patient’s index were analyzed by using the paired test before and after the operation. P < 0.05 considered the statistical was significant difference.
Result
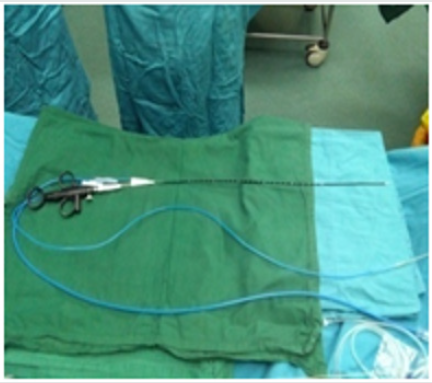
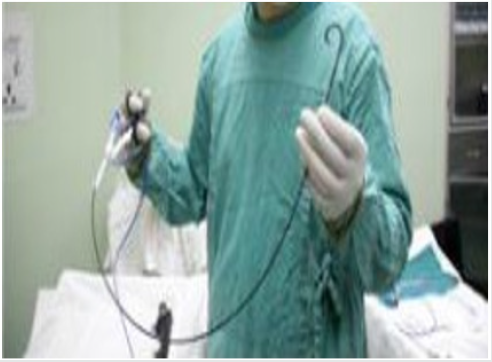
63 patients all underwent retrograde ureteroscopy surgery combined with micro-perc. 45 cases of male used 70cm FURS (Figure 4), 16 cases of female used 42cm FURS (Figure 5 & 6); the average operation time was 35~60min, mean 47min, retrograde well placed sheath and FURS time 4~7min, Lithotripsy time 20~35min, all seeing needle puncture and establishment access time 3~5min, Lithotripsy time 8~12min. 48 cases mainly lithotripsy with FURS and 15cases with micro-perc; postoperative KUB, 3 cases of residual stones, 5 cases of stone fragments with No clinical significance(NCSF), totally powdered in 53 cases; hemoglobin level before and after operation change 0.6~1.4g/ dl, mean 1.0g/dl; Cr level before and after operation change 1.34~7.26μmol/L mean 4.33μmol/L. 3 cases of postoperative fever, 2 cases remission after injection of antipyretic drugs, 1 case was relieved with not drug treatment. 5 cases of pain, 3 cases were remission after given analgesic drug treatment, another 2 patients were not given treatment. The catheter was removed one day after post operation, 2 days after operation the patients discharged. There were 3 cases with residual stones, the Extracorporeal shock wave lithotripsy (ESWL)were carried out after 2 weeks. One month after reassessment was found residual stones in 1 case. The one remaining stone was further treated (mirco-perc). The results were as follows: (Table 2)
Table 2: Perioperative and Operative Findings of the Patients.
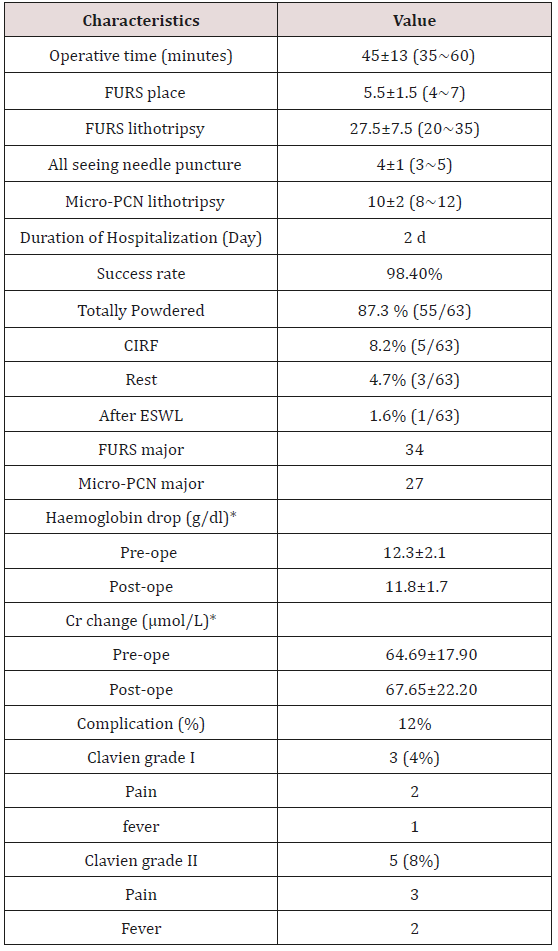
CIRF: Clinically Insignificant Residual Fragment
*p>0.05
Discussion
For the treatment of renal calculi, there were the following methods: PCNL, ESWL, and RIRS. However, for Lower Pole Renal Calculi, ESWL is often difficult to achieve ideal outcome. because of the infundibular and the angle with the long axis of the renal pelvis. After stone crushing, it is not easy to be expelled from the body. Kim et al. [4] reported that extracorporeal shock wave lithotripsy is suitable for stones less than 2cm.
PCNL and retrograde flexible ureteroscopic lithotripsy were often used as minimally invasive methods for treatment of Lower Pole Renal Calculi. Bozkurt et al. [5] compared surgical outcomes between PNL and RIRS for renal stones sized less than 20 mm, and they showed that the PNL and RIRS procedures were safe and effective methods for renal stones in the lower-pole calyces. And there is no significant correlation between anatomical factors such as infundibulum length, width, angle [6]. Compared with PCN, FURS with more minimally invasive and lower incidence of complications (Figures 7 & 8). Therefore, PCNL is often used for larger stone selection (>2cm) [7]. While the smaller the size of the stones, retrograde FURS was often performed. Although PCNL is the gold standard for the treatment of larger stones [8], it has the advantages of shorter operation time and higher rate of stone removal. But the complication rate was higher than that of FURS. When the stone was larger than 2cm, the incidence of complications and the level of hemoglobin decrease were significantly higher than those of FURS surgery [9]. The curved degree of the flexible ureteroscope has certain limitation, especially when the working access is occupied by holmium laser fiber, sensitivity will be reduced. So, it has a high stone residual rate when the flexible ureteroscopy for the treatment of lower Pole Renal Calculi [10]. Especially when the IPA is less than 30 degrees the stone free rate significantly reduced [11]. The treatment of lower Pole Renal Calculi with greater than 2cm, Simple FURS retrograde surgery is less effective. And Jeong et al. [12] suggest that PCNL had a high SFR than FURS for treatment of lower Pole Renal Calculi. Therefore, we used retrograde FURS lithotripsy combined with ultrasound guided F4.8 all seeing needle puncture the target renal calyx and micro-perc lithotripsy improved the SFR of lower Pole Renal Calculi (95.2%). The disadvantage of nephrostomy no matter Standard PCN or mini PCN is that it sometimes involves longer distances from the skin to the lower calyx, so was easy to cause bleeding and injury [13]. Ultrasound guided F4.8 micro-perc is more delicate and has dual role of guidance and positioning. The puncturing Pathway is monitored by ultrasound and performed at the point of less blood flow. Each anatomical layer can be observed during the puncture, so the injury of the blood vessel and surrounding organs can be avoided. When seen the stones was stopped immediately, to avoid the damage caused by deep puncture, in accordance with the precise surgical concept, which is important for the stones in the lower-anterior minor calyx. The site of stone is not easy to find, and it is considered to be the independent risk factors for residual stones [14]. This research results show that retrograde flexible ureteroscope combined with ultrasound guided F4.8 micro-perc in the treatment of lower Pole Renal Calculi greater than 2cm Clavien I complications is 4%, 8% in grade II, with mild complications, no significant changes of hemoglobin and Cr level before and after surgery, success rate of 95.2% postoperation , with safety and effectiveness. There are two types of adult Poly-FURS with 42cm and 70cm, and different types are selected according to the patient’s sex. 42cm type mainly used in female patients, FURS length of 42cm and the sheath length was 29cm. Individualized selection of different length can be avoided damage caused the sheath placed deeper, and outside part in short, so have a large supporting force, good concentricity, more conducive to perform, has the advantages of increased comfort, reduced fatigue and improved efficiency. Through the study, we summarize the advantages of the operation: 1. all seeing needle puncture at different anatomical using different guided mode, make the process to become more clear, more accurate, and reduce the complications; 2. FURS combined with micro-perc decrease the vision of dead ends and increase the stone clearance rate; 3.Ultrasound guided all seeing needle puncture technology learning curve is short, easy to grasp. 4. Lower Pole calyx space is small, single FURS or single micro-perc is easy to cause the intrarenal pressure and this combine can reduce the pressure of the calyces, effectively reducing the stone debris flying, and giving clearer vision. Our experience: 1.The use of UAS during operation, not only can reduce intrapelvic pressure, attract out of the stone fragments, well controlled the perfusion flow and reduce the operative time [15]; 2. Selection the type of the FURS according to the sex make the operation more convenient; 3. During all seeing needle procedure, pulse not continuous water injection make the puncture more clear, and reduced perfusion fluid extravasations; 4. Due to the difficulty in removing the lower calyceal calculi, during the surgery the stones should try to “powdered”, and after the surgery often keep the head down and the hip high body position; 5, DJ stent located time is around 1month, increase in the excretion of the stones, oral traditional Chinese medicine anti-inflammatory drugs, and there is low incidence of catheter-related inflammation in 7.9% (5/63).
Conclusion
Poly-FURS combined with ultrasound guided all seeing needle puncture Micro-perc used to treatment of Lower Pole Renal Calculi larger than 2cm with infundibulopelvic angle less than 60 degrees it is safe, effective and easy to master.
Deficiencies
The sample is less, this study does not distinguish between stones in lower-anterior minor calyx and lower- posterio minor calyx, not cleanly recording length and width of the infundibulum. There is a need for further accumulation and fine grouping of the samples, to further improve the defects of the study.
References
- Kawahara T, Ito H, Terao H, Tanaka K, Ogawa T, et al. (2012) Ureteroscopy assisted retrograde nephrostomy for lower calyx calculi in horseshoe kidney: two case reports. Journal of Medical Case Reports 6(): 194.
- Takazawa R, Kitayama S, Tsujii T (2012) Successful outcome of flexible ureteroscopy with holmium laser lithotripsy for renal stones 2cm or greater. Int J Urol 19(3): 264-267.
- Ghoneim IA, Ziada AM, Elkatib SE (2005) Predictive factors of lower caliceal stone clearance after extracorporeal shock wave lithotripsy (ESWL): A focus on infundibulopelvic anatomy. Eur Urol 48(2): 296-302.
- Kim TB, Lee SC, Kim KH, Jung H, Yoon SJ, et al. (2013) The feasi-bility of shockwave lithotripsy for treating solitary, lower caly-ceal stones over 1 cm in size. Can Urol Assoc J 7(3-4): E156-160.
- Bozkurt OF, Resorlu B, Yildiz Y, Can CE, Unsal A, et al. (2011) Retrograde intrarenal surgery versus percutaneous nephrolithotomy in the management of lower-pole renal stones with a diameter of 15 to 20 mm. J Endourol 25(7): 1131-1135.
- Resorlu B, Oguz U, Resorlu EB, Oztuna D, Unsal A, et al. (2012) The impact of pelvicaliceal anatomy on the success of retrograde intrarenal surgery in patients with lower pole renal stones. Urology 79(1): 61-66.
- Ozgor F, Tepeler A, Basibuyuk I, Kucuktopcu O, Kayaliy Y et al. (2017) Supracostal access for miniaturized percutaneous nephrolithotomy: comparison of supracostal and infracostal approaches. Urolithiasis. 46(3): 279-283.
- Vicentini FC, Serzedello FR, Thomas K, Marchini GS, Torricelli FCM, et al. (2017) What is the quickest scoring system to predict percutaneous nephrolithotomyoutcomes? A comparative study among S.T.O.N.E score, guy's stone score and croes nomogram. Int Braz J Urol 43(6):1102-1109.
- Zhi Gang Li, Zhao Y, Tao An, Han CH, Zang GH, et al. (2016) Clinical effects of FURL and PCNL with holmium laser for the treatment of kidney stones. Experimental and Therapeutic Medicine 12(6): 3653-3657.
- Jung GH, Jung JH, Ahn TS, Lee JS, Cho SY, et al. (2015) Comparison of retrograde i ntrarenal surgery versus a single-session percutaneous nephrolithotomy for ower-pole stones with a diameter of 15 to 30 mm: A propensity score-matching study. Korean J Urol 56(7): 525-532.
- Kilicarslan H, Kaynak Y, Kordan Y, Kaygisiz O, Coskun B, et al. (2015) Unfavorable Anatomical Factors Influencing the Success of Retrograde Intra renal Surgery for Lower Pole Renal Calculi. Endourology and Stone Disease Urol J 12(2): 2065-2068.
- Jeong CW, Jung JW, Cha WH, Lee BK, Lee S, et al. (2013) Seoul National University renal stone complexity score for predicting stone-free rate after percutaneous nephrolithotomy. PLoS One 8(6): e65888.
- Ghoneimy MN, Kodera AS, Emran AM, Orban TZ, Shaban AM, et al. (2009) Percutaneous nephrolithotomy in horseshoe kidneys: is rigid nephroscopy sufficient tool for complete clearance? A case series study. BMC Urol 9: 17.
- Jung GH, Jung JH, Ahn TS, Lee JS, Cho SY, et al. (2015) Comparison of retrograde intrarenal surgery versus a single-session percutaneous nephrolithotomy for ower-pole stones with a diameter of 15 to 30 mm: A propensity score-matching study. Korean J Urol 56(7): 525-532.
- Breda A, Territo A, López Martínez JM (2016) Benefits and risks of ureteral access sheaths for retrograde renal access. Curr Opin Urol 26(1): 70-75.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...