Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Review Article(ISSN: 2641-1725) 
Burning: Etiologies, Pathophysiology and Prognosis Volume 5 - Issue 3
SalouaKhalfaoui*, Abdellah El Marbouh, Mustapha El Abbassi
- Department of Physical Medicine and Rehabilitation, Military Instruction Hospital Mohammed V, Morocco
Received: August 17, 2020; Published: August 21, 2020
*Corresponding author:SalouaKhalfaoui, Assistant Professor in physical medicine and rehabilitation.
Mohamed V University, Faculty of Medicine and Pharmacy of Rabat, Morocco
DOI: 10.32474/LOJMS.2020.05.000213
Abstract
The burn is a frequent accident most often of domestic origin. Causal agents are diverse and can be associated. The quality of the care depends initially on a good diagnosis of the different lesions with precision and description of their characteristics which play a primordial role in the evaluation and the prognosis of the burn.
Keywords: Burn ;etiologies ;physiopathology ;prognosis
Introduction General
Burns are an acute trauma to the skin with an increasing frequency. In France, it is estimated at 400,000 cases of burns per year, of which almost 4,000 require hospitalization in a specialized center. According to the World Health Organization, 300,000 burns people die each year worldwide [1].
Etiologies of the Burn
The destruction of the skin covering and the underlying tissues results from many factors. It can be:
Thermal burn
Definedby an attack on the skin by a liquid, a flame or an explosion with a temperatureabove 60 ° and the exposure time lasts a few seconds. It occurs on healthy skin and causes local skin reactionsleading to complications and sequelaesuch as hypertrophy and congestion.The thermal burncanbeassociatedwith the chemicalburn in the event of a gas or liquid explosion, thusaggravating the main skin consequencesmentionedabove; Hence the importance of preventive and curative management of bridles and after-effects [1].
Electrical Burns
Consideredabove all as a domestic accident thatcanbeencounteredatanyage (child or adult).The electriccurrentfollows a body passage from the hand (in adults) or the mouth (in children) and exits through the foot.In this case, thereis no hypertrophy or congestion becauseoften the segments of the affectedlimbs are destroyedimmediately and recoveryremainsdifficultdepending on the characteristics of the electriccurrentwhichcan cause immediatecardiacarrest.However, the heatreleased on contact withcurrent by flash or electric arc effect causes skin lesionssimilar to thosecaused by thermal burns.
Chemical burn
Is classified as the mostdangerous by itscutaneousconsequences. The causative agent must beidentifieduponreceipt of the patient withprecision of its nature, itsacidic or basic pH, its concentration, itsmolar mass and especially the duration of exposure. The initial treatmentisbased on hemodynamicstabilization, pain management and thenimmediatetransfer to a specialized center.
Pathophysiology of the burn
Beforeeachburn, there are rules to takeintoconsideration and measures to take and mention
Location of the burn
May determine the prognosis for life (in case of upperairwayinvolvement) or functional (in case of burns of the extremities).
Extent or area of burn
Estimatedinpercentage by Wallace’srule in adults:
a. 9% for the head and neck and eachupperlimb.
b. 18% for eachside of the trunk and eachlowerlimb.
c. And 1% for the perineum and externalgenitalia and for
the palm of each hand.
The Lund and Browder tables give more precision because the
area is estimated according to age [2].
Burn Depth
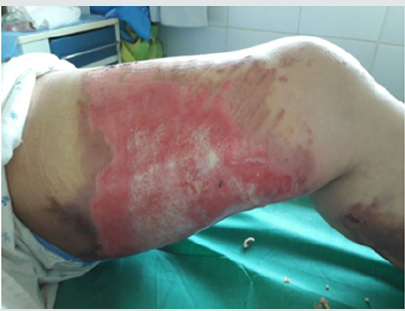
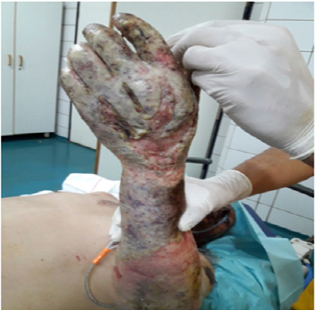
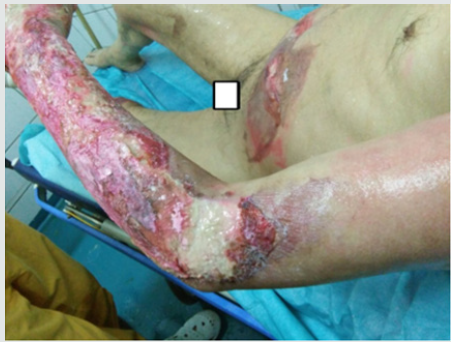
The main difficulty in the initial management of the burn remains the estimation of the depth when receiving the burn patient.We can distinguish 4 degrees: [2,3]1st degree burn: this is a sunburn or erythema where the blood circulation and capillary pulse are intact.Superficial 2nd degree burn: (Figure 1) corresponds to the destruction of the superficial part of the epidermis without or with partial damage to the basement membrane and Malpighi cells.Clinically, it results in blistering, redness and warmth of the underlying skin, severe pain with the possibility of a small hemorrhage on scarification.Healing takes place without unsightly sequelae after two to three weeks.Deep 2nd degree burn: (Figure 2) skin destruction affects the entire epidermis and part of the dermis. Clinically, after excision, a whitish or pinkish floor is observed with minimal bleeding and hypoaesthesia. The roots of the hairs, sweat and sebaceous glands remain intact hence the resistance of the hairs during traction.Spontaneous healing lasts longer up to a month unless there is significant malnutrition or superinfection.3rd degree burn: (Figure 3) corresponds to carbonization or necrosis secondary to the total destruction of the epidermis and dermis, hence the impossibility of spontaneous epidermization.Clinically: The skin appears dark, brown or black, cardboard and unresponsive with thrombosed veins. In this case, dermal-epidermal grafting preceded by excision of necrosis is required.
Burnprognosis
The estimation of the surface and the depth makes it possible to establish two prognostic indices [1,3].
The Baux rule(Professor Serge Baux, pioneer of world burn science), whichallows the vital prognosis of a burn patient to beassessed by takingintoaccount the age, area, depth of the burn and anyassociateddefects. The calculationis simple, itconsists of adding the age in years to the body surface area burned (SCB), and if there are defects, weadd 15 to the addition. The prognosisisstronglyinvolved and evendeathif the index exceeds the total of 100.
The UBS Index
Corresponds to the followingrule:
Sum of total burns in% + 3 times the% of deep burns (3rd degree).
a. Severeburn if UBS <40
b. Severeburn if 60
a. Involvement of the upperairwaysfollowing inhalation of
toxic fumes occurringin 20% of cases with the consequences of
chemicalburns of the tracheobronchialtree.
b. Certain localizations are sensitive by
theirrepercussionssuch as the face and the hand
(aestheticrepercussion), the joints and the extremities of
the limbs (functionalrepercussions) and natural orifices
(infectiousrepercussions). (Figure 4)
c. Small age, advancedage, essential defectssuch as
high blood pressure, diabetes, heartfailure, etc. act on the
progression and healing of initial lesions.
d. The table summarizes the different cases of burns
and classifies them as mild and severeaccording to the
parametersmentioned.
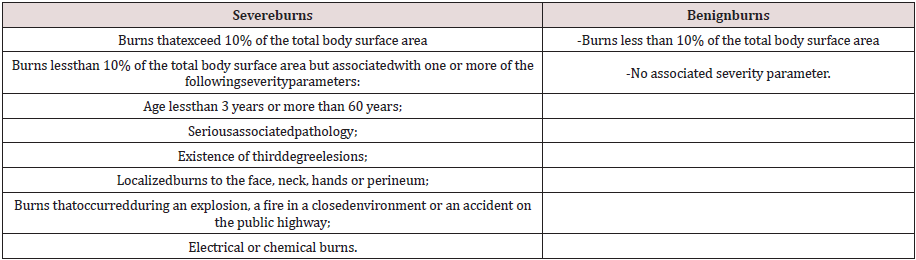
Table 1: Classifications of burns according to the French Society
for the Study and Treatment of Burns (SFETB) [2].
Table 1:Classifications of burns according to the French Society for the Study and Treatment of Burns (SFETB) [2].
CLD: Continuous Lumbar Drainage, LP: Lumbar Puncture, RBC: Red Blood Cells, WBC: White Blood Cells, CSF: Cerebrospinal Fluid, ICP: Intracranial Pressure.
Conclusions
Burn is a progressive disease and its parameters can change and worsen over time hence the need for a good initial examination upon reception of the burn patient and establishment of a prognosis; without forgetting the regular and close monitoring of any patient at risk of malnutrition and super infection.
Conflicts of Interest
The authors declare that they have no conflicts of interest.
References
- SociétéFrançaise (1996) Francophone des PlaiesetCicatrisations.
- Rochet JM, Wassermann D, Carsin H, Desmoulière A, Aboiron H, et al. (1998)Rééducation et réadaptation de l’adultebrûlé. EncyclMédChir (Elsevier, Paris) Kinésithérapie-Médecine physique-Ré
- Fitzpatrick JC, Cioffi WC (1996) Diagnosis and treatment of inhalation injury. In: Herndon DN (edn), Total burn care. London: WB Saunders1996 :184-192
- Ehde DM, Moore ML, Patterson DR, Mann R, Engrav LH (1997) Adherence to pressure garment therapy: a prospective study. In: McManus WF ed. XXIX annual meeting of the American Burn Association. J Burn Care Rehabil 18 (1): 80.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...