Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1725
Research Article(ISSN: 2641-1725) 
Attention Deficity Hyperactivity Disorder Under Pharmacological Treatment: Prevalence, Treatment Adherence and Comorbidity Volume 5 - Issue 5
Perejón López D1*, Serna Arnaiz MC2, Galvan Santiago L3, Siscart Viladegut J1 and Gasco Serna L4
- 1Resident Internal Medicine, University of Lleida, Spain
- 2Associate Professor University of Lleida, Spain
- 3Pharmacist, Lleida Health Department, Spain
- 4Master Clinical Psychology, UNIR University, Spain
Received: July 13, 2021 Published: July 29, 2021
*Corresponding author: Perejón López D, Resident Internal Medicine, University of Lleida, Spain
DOI: 10.32474/LOJMS.2021.05.000223
Abstract
Background: Few studies have analyzed use of or adherence to Attention Deficit Hyperactivity Disorder (ADHD) medication over the long term. The aims of this study were to determine the prevalence of ADHD under treatment in a general population, estimate treatment compliance, and analyze the presence of comorbidities based on the use of concomitant psychotropics.
Methods: Retrospective cohort study of ADHD drugs dispensed in a Spanish healthcare district between 2015 and 2017.
Results: Of the population studied, 0.3% were under pharmacological treatment for ADHD and of these 71.2% were male and 28.8% were female. The most common treatments were methylphenidate (79.7%) and lisdexamfetamine (11%). Five percent of patients were also taking antidepressants, 2.2% anxiolytics, 1.1% hypnotics, and 4.3% antipsychotics. Forty percent of patients had good adherence (defined as an adherence rate of ≥80). Mean ± SD overall adherence was 63% ± 32.8. The rates by age group were 64.8% in children <15 years, 55.1% in adolescents aged 15-19 years, and 65.4% in patients aged ≥20 years. Grouped by sex, adherence was 64.3% in females and 62.2% in males.
Conclusions: Three times as many male as female patients in our series were under pharmacological treatment for ADHD and a low proportion of the patients were taking concomitant psychotropic medication. Mean treatment compliance was two-thirds of the prescribed treatment duration. Male sex and adolescence were associated with the worst adherence rates
Abbreviations: ADHD: Attention Deficit Hyperactivity Disorder; DDD: Defined Daily Dose; MARS: Medication Adherence Rating Scale; MPR: Medication Possession Ratio; ODD: Oppositional Defiant Disorder; SD: Standard Deviation
Introduction
Attention Deficit Hyperactivity Disorder (ADHD) starts in childhood with symptoms of hyperactivity, impulsivity, and/ or inattention. These symptoms affect cognitive, academic, behavioral, emotional, and social functioning [1]. The reported prevalence of ADHD in children ranges from 2% to 18% depending on the diagnostic criteria used and the population studied (e.g. primary care versus hospital) [1]. The estimated prevalence in school-aged children is 8% to 11%, making it one of the most common disorders of childhood [2]. According to a multicenter meta-analysis of 175 studies involving 1,023,071 individuals, the estimated pooled prevalence of ADHD in adults aged over 36 years was 7.3% (95% CI, 6.7-7.8) [3]. Epidemiological studies of ADHD in the adult population have estimated a current prevalence of 3.4% nationwide and 4.4% in the United States [4,5]. Based on data from the 2015-2016 US National Survey of Children’s Health (NSCH), approximately 10% of children aged between 4 and 17 years had a diagnosis of ADHD [6]. ADHD is more common in boys, with a male to female ratio of 4:1 for primarily hyperactive ADHD and 2:1 for primarily inattentive ADHD [7]. According to the 2011-2012 NSCH, 15.1% of boys and 6.7% of girls in the United States had ADHD [6].
Comorbidities
Children and adolescents with ADHD often have concomitant psychiatric disorders, such as oppositional defiant disorder (ODD), conduct disorder, depression, anxiety, and learning disabilities [8,9]. Anxiety disorder and ADHD coexist in approximately 20% to 40% of cases [7]. Anxiety may be secondary to childhood ADHD but in many cases, it appears to be a distinct disorder, independent of ADHD [10]. Depression coexists in one in three patients with ADHD [6] and appears to be more common in those with inattentive and combined ADHD [11]. Children with concomitant ADHD and depression may have relatives with a history of major depressive disorder [12], while adolescents with ADHD and mood disorder have been found to be at greater risk for suicide [13]. Adults with ADHD tend to have concomitant psychiatric disorders. One US study found that adults with ADHD had a higher risk of mood disorders (odds ratio [OR], 2.7–7.5; 95% CI, 3.0-8.2), anxiety disorders (OR, 1.5-5.5; 95% CI, 2.4-5.5); substance use disorders (OR, 3.0; 95% CI, 1.4-6.5); and intermittent explosive disorder (OR, 3.7; 95% CI, 2.2-6.2) [14]. Medication, with or without behavioral and/or psychological interventions, is the first-line treatment for schoolaged children (≥6 years), adolescents, and adults who meet the diagnostic criteria for ADHD [2]. The most common drugs used are methylphenidate and lisdexamfetamine (stimulants), followed by atomoxetine and modafinil used off-label; α2-adrenergic agonists are also used although they have been found to have limited efficacy in adults [15]. Few studies have analyzed use of or adherence to ADHD medication over the long term. The aim of this study was to determine the prevalence of ADHD under pharmacological treatment in a general population, estimate treatment compliance, and analyze the presence of comorbidities based on the use of concomitant psychotropics.
Materials and Methods
Data Sources
Retrospective study of prescription drug dispensation records to identify ADHD prescriptions in the healthcare district of Lleida, Spain between January 1, 2015 and December 31, 2017. Prescription data were obtained from the Catalan Health Department’s database, which classifies drugs using the World Health Organization’s Anatomical Therapeutic Chemical classification system [16]. Demographic information (date of birth and sex), administrative status (including death and change of residence), and medical diagnoses were obtained from primary care information systems.
Cohort Selection
All patients issued at least one ADHD prescription between January 2015 and December 2017 were eligible for inclusion. We excluded patients who had moved out of the region or died during the study period, patients for whom information on medication use was missing, patients with erroneous or duplicate entries, and patients from other healthcare districts who had at some stage been prescribed ADHD medication in Lleida. The following variables were recorded: age at start of study; prescription fills for centrally acting sympathomimetics (ATC code N06BA), guanfacine (CO2ACO2), antidepressants (N06A), anxiolytics (N05B), hypnotics and sedatives (N05C), and antipsychotics (N05A); and clinical diagnoses associated with the prescriptions. The total number of patients under pharmacological treatment for ADHD was 976 in 2015, 971 in 2016, and 1011 in 2017. Fifty-two patients were excluded in 2015, 57 in 2016, and 57 in 2017.
Treatment Duration and Adherence
Treatment duration was calculated by counting the number of months from the first prescription fill starting in January 2015 to the last fill in December 2017. Treatment episodes were complete when patients did not receive medication for a period of 6 months. Treatment durations were censored for patients who had not completed treatment by the end of the study period. Treatment adherence was estimated using the medication possession ratio (MPR). For each medication, we calculated the number of units needed per month according to the Defined Daily Dose (DDD) assigned to each drug by the World Health Organization’s Collaborating Centre for Drugs Statistics Methodology [16]. The MDR (adherence ratio) is calculated by dividing the number of units dispensed by the prespecified number of units required for the duration of treatment. A ratio of ≥80% was chosen to indicate good adherence. Good treatment compliance, in turn, was defined as an adherence rate of ≥80% up to completion of treatment in patients who had been treated for over 4 months. Comorbidities were analyzed by studying concomitant use of antipsychotics, antidepressants, anxiolytics, and hypnotics and sedatives. The study was approved by the clinical research ethics committee of IDIAP Jordi Gol i Gurina (code P18/063) and was conducted in accordance with good clinical practices, with appropriate safeguarding of ethical and confidentiality issues. Statistical analysis: A descriptive analysis of the cohort was performed using frequencies and percentages. Compliance rates were estimated with a confidence interval of 95%. Associations between compliance rates and study variables were analyzed using the chi-square test. Crude and adjusted odds ratios for treatment compliance were calculated using regression models (enter method). Statistical significance was established at p < .05.
Results
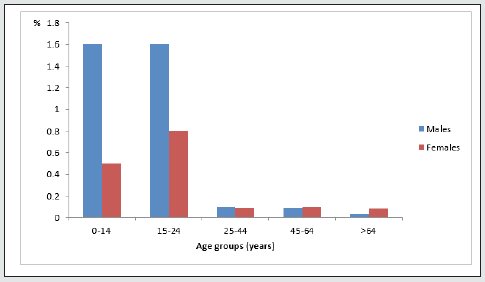
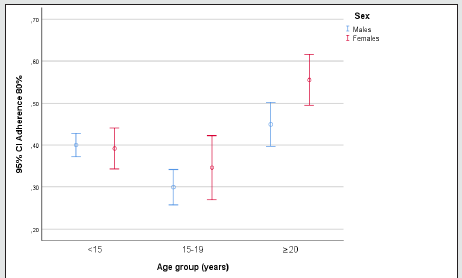
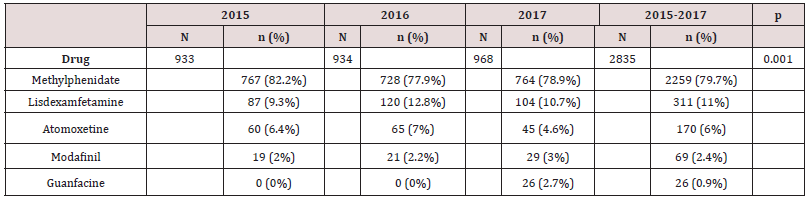
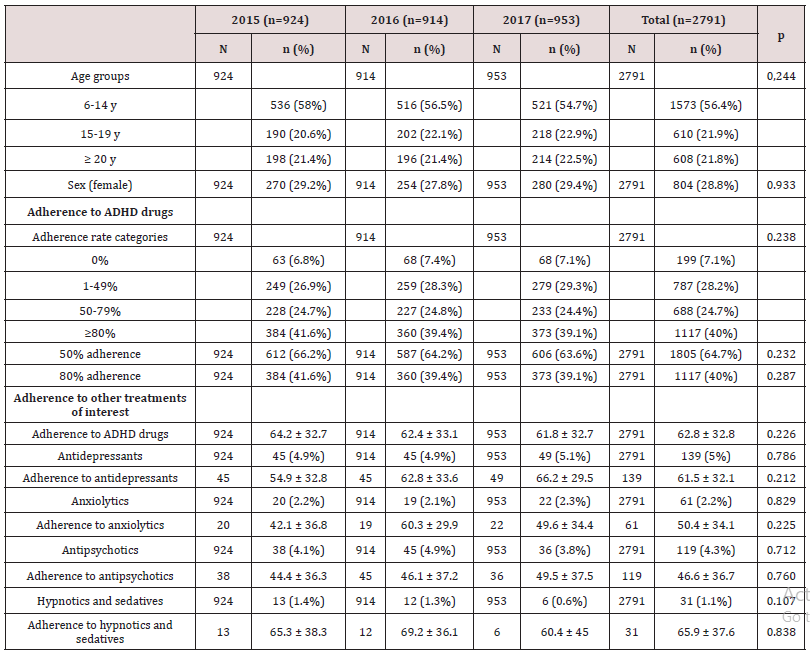
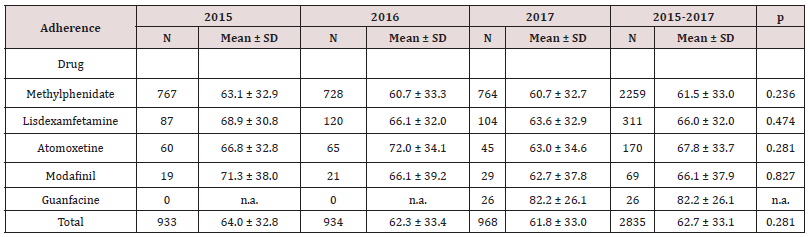
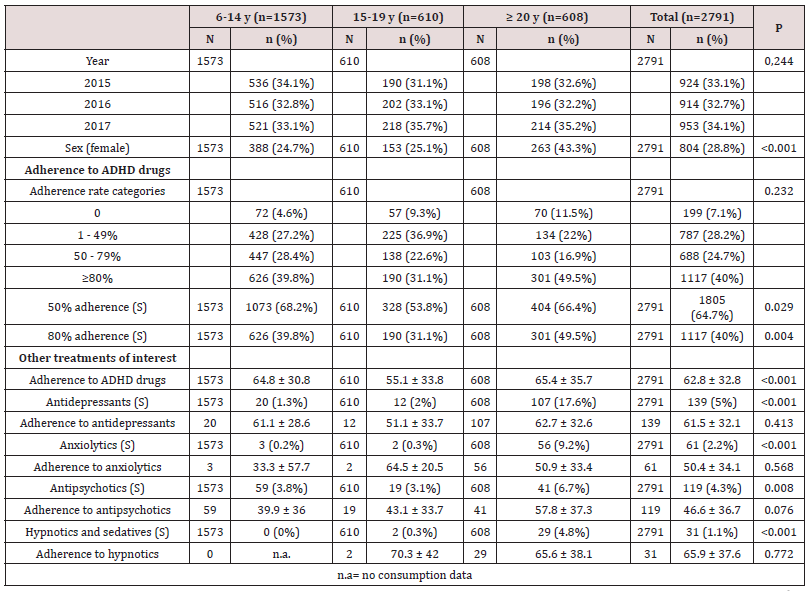
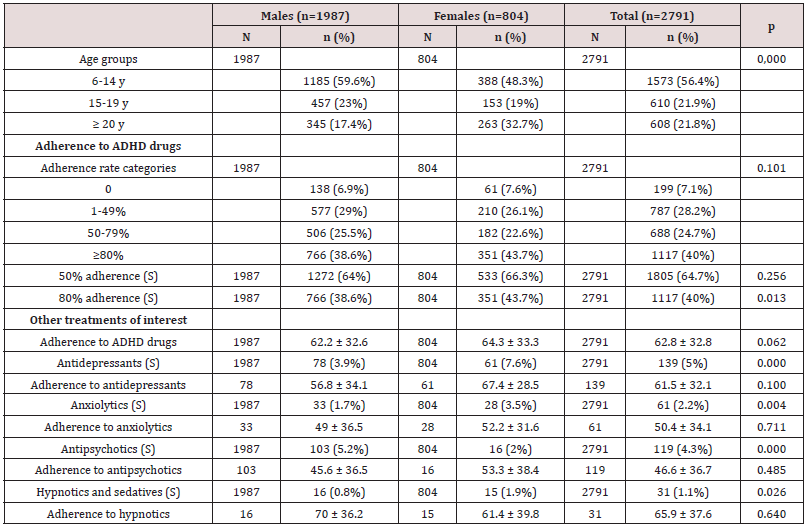
In total, 2791 patients were prescribed ADHD medication over the three study years (2015-2017). This corresponds to an annual incidence of 0.3%. There were 924 patients under treatment in 2015, 914 in 2016, and 953 in 2017. The largest group was the under-25 group, where 1.6% of males <15 years, 0.5% of females <15 years, and 0.8% of males and females aged 15-24 years had been prescribed an ADHD medication. The breakdown by age and sex for the last year of the study (2017) is shown in Figure 1. The most common ADHD medication was methylphenidate (79.7%) followed by lisdexamfetamine (11%). The breakdown of drug prescriptions per year and for the overall study period is shown in Table 1. Five percent of patients under treatment for ADHD were also taking antidepressants, 2.2% were taking anxiolytics, 1.1% hypnotics, and 4.3% antipsychotics. Of the 2791 patients under ADHD treatment between 2015 and 2017, 71.2% were male and 28.8% were female. Their mean ± SD ages were 16.8 ± 11.4 and 24 ± 19 years, respectively. Mean overall adherence was 63% ± 32.8% and 40% of patients were ≥80% adherent (Table 2). Adherence rates did not vary significantly according to type of medication, although patients on guanfacine, which was launched in just 2017, had the highest rate, at 82% (Table 3). Adherence rates by age group were 39.8% for the <15 group, 31.1% for the 15-19 group, and 49.5% for the >20 group. These differences were significant. Concomitant psychotropic medication was more common in patients aged >20 years. Age had no significant influence on adherence rates (Table 4). Male patients under pharmacological treatment for ADHD outnumbered female patients in all age groups. Good treatment compliance (adherence ≥80%) was significantly more common in females (43.7% vs. 38.6% for males). Antidepressants, anxiolytics, and hypnotics were prescribed more frequently to females, while antipsychotics were more common in men. The differences in both cases were significant. No significant differences were observed for adherence to concomitant medication among males and females (Table 5, Figure 2).
Discussion
Exposure to ADHD medication
Overall, we detected an annual prevalence of 0.3% of ADHD under pharmacological treatment for the period January 1, 2015 to December 31, 2017. By age group, treatment was most common in patients aged <25 years: 1.6% of males and 0.5% of females aged <15 years and 0.8% of males and of females in the 15-24 age group had been prescribed ADHD medication. Prevalence rates for childhood ADHD in the literature range from 2% to 18% and vary according to diagnostic criteria and setting (e.g. primary care versus hospitals) [1]. The estimated prevalence in adults is 4.4% according to a US study [14] and 3.4% (range 1.2%-7.3%) according to a nationwide study spanning 10 countries. ADHD is four times more common in boys than in girls [7]. In our cohort, the male to female ratio was 3:1 for children and 2:1 for adolescents aged 15-19 years. According to the 2015-2016 NSCH, 14% of boys and 6% of girls in the United States had ADHD [6].
The vast majority of patients were being treated with stimulant medication (methylphenidate in 79.7% of cases and lisdexamfetamine in 11%). Stimulant medication, combined with cognitive-behavior therapy, is generally the first-line treatment for children and adolescents with uncomplicated ADHD [2,9]. It is also the most widely used and prescribed treatment for adult ADHD [17]. Stimulant drugs are also the first choice of treatment for adult ADHD and their use is supported by data from over 40 studies involving 4793 individuals. As mentioned by Wilens, et al [17]: “Despite this relatively large body of evidence, however, much remains to be understood about the role of factors such as age, dosing, long-term adverse effects, and subgroup variations”.
Comorbidity
Between 20% to 40% of patients with ADHD have anxiety disorders, while a third have concomitant depression or conduct disorders [4,18,19]. Between 20% and 45% of children with ADHD meet the diagnostic criteria for at least one anxiety disorder [8]. Five percent of patients under treatment for ADHD in our series were taking antidepressants, 2.2% anxiolytics, 1.1% hypnotics, and 4.3% antipsychotics. These rates are lower than the rates reported above, but as we only analyzed patients who had been prescribed ADHD medication, our population does not include patients not receiving pharmacological treatment or patients not yet diagnosed.
Adherence to treatment
Good adherence to ADHD medication, defined as an adherence rate of ≥80%, was observed for 40% of the patients in our series, and the mean ± SD adherence rate for the overall group was 63% ± 32.8%. Adherence did not vary significantly according to type of medication, but we did observe a particularly high rate for guanfacine (82%), but this was based only on data for 2017, when the drug was launched. The COMPLY study is a prospective, open-label, 12-month observational study that assessed medication adherence in children and adolescents aged 6-17 years with ADHD using the Pediatric Compliance Self-Rating instrument and the first four items of the Medication Adherence Rating Scale (MARS). No significant differences were found between adherence to psychostimulants and adherence to non-stimulants [20]. We observed significant differences in adherence according to age. Adherence was poorest in the 15-19 group (31.1% vs 39.8% for under-15s and 49.5% for those aged >20 years). The authors of a Swedish study of ADHD medication and criminality in individuals aged >16 years found an association between increased criminality and non-adherence as well as a reduction in criminality during treatment and an increase off treatment (21). Their findings highlight the potential benefits of interventions designed to improve treatment compliance, but they also show that benefits are lost when treatment is discontinued [22]. Irregular use of medication is common in adolescents. While adult patients are generally responsible for their own health, health care decisions for children are usually taken by parents. When a child reaches adolescence, however, their beliefs about treatment may change, leading them to skip doses [23]. Self-reported adherence tends to be overestimated by parents, adolescents, and young adults [24]. Suboptimal medication adherence is more likely to be detected when a teenager is asked “How many pills have you skipped this month?” rather than “Have you skipped any pills this month”? [25]. An observational study of 51 university students with ADHD in the United States found an overall adherence rate of 54%, but this varied between 34% and 68% depending on the year they were in and the time of the semester [25]. Respondents’ perceptions of the burden of medication use tend to be negative. Its potential short- and long-term adverse effects also cause concern and are often mentioned by this population as the reason for discontinuation. Improvements in shared decision-making among practitioners, parents, and young patients, and careful monitoring of treatment effectiveness and safety, are necessary in order to optimize outcomes [26]. Studies in children and adolescents have reported adherence rates over a period of 12 months ranging from 56% for long-acting stimulants to 67% for atomoxetine, a nonstimulant [27]. All the studies evaluated adherence as the ratio between number of days of medication supplied and number of days the medication should have been taken during a prespecified period. This method, MPR, is the same as that used in our study [28]. In our series, female patients adhered significantly better to ADHD treatment (≥80% adherence rate of 43.7% vs. 38.6% for males). Other studies have also reported better adherence rates among women together with differences in treatment compliance according to age [29]. The typical cutoff to define good adherence in these studies is ≥80% [30]. Marcus, et al [31], for example, found that 18% of intermediate-grade school children adhered well to treatment (≥70% adherence per marking period), while Hodgkin, et al. [32] found a mean adherence rate of 49% among similarly aged adolescents. In our series, use of antidepressants, anxiolytics, and hypnotics was significantly higher in females, while that of antipsychotics was significantly higher in males. These differences are similar to those reported for the general population [33]. Our study has some limitations. As we only analyzed data from the Spanish National Healthcare system, we may have missed out on prescriptions issued in private practice or within occupational health insurance schemes. Nonetheless, we believe that these prescriptions will have accounted for only a small proportion of all prescriptions in the region, as the Spanish healthcare system offers universal coverage [34]. By not analyzing medical records, we may also have missed cases not included in the databases analyzed. Finally, we did not investigate clinical causes of poor adherence and this information is important for addressing this problem. These limitations should be considered when evaluating our results.
Conclusion
In conclusion, we have described a cohort of patients receiving pharmacological treatment for ADHD. The overall prevalence, at 0.3%, is, in our opinion, low. Males were three times more likely than females to be prescribed ADHD medication. The most widely prescribed drug was methylphenidate and the most widely used drugs for concomitant psychiatric disorders were antidepressants (5%) and antipsychotics (4.2%).
Overall adherence was low, at 63%, and less than half the patients were ≥80% adherent.
Adolescent Boys had the Worst Adherence Rates
More studies are needed to analyze treatment compliance in ADHD, particularly among more vulnerable groups, and to investigate interventions that will favor compliance.
References
- American Psychiatric Association. Attention-deficit/hyperactivity disorder. In: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, American Psychiatric Association, Arlington, VA 2013. p.59.
- Subcommittee on Attention-Deficit/Hyperactivity Disorder, Steering Committee on Quality Improvement and Management, Wolraich M, Brown L, Brown RT, et al. (2011) ADHD: Clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics 128: 1007-1022.
- Thomas R, Sanders S, Doust J, Beller E, Glasziou P (2015) Prevalence of attention-deficit/hyperactivity disorder: A systematic review and meta-analysis. Pediatrics 135: 994-1001.
- Visser SN, Danielson ML, Bitsko RH, Holbrook JR, Kogan MD, et al. (2014) Trends in the parent-report of health care provider-diagnosed and medicated attention-deficit/hyperactivity disorder: United States, 2003-2011. J Am Acad Child Adolesc Psychiatry 53: 34-46.
- Fayyad J, R De Graaf, R Kessler, J Alonso, M Angermeyer, et al. (2007) Cross-national prevalence and correlates of adult attention-deficit hyperactivity disorder. Br J Psychiatry 190: 402.
- Xu G, Strathearn L, Liu B, Yang B, Bao W (2018) Twenty-Year Trends in Diagnosed Attention-Deficit/Hyperactivity Disorder Among US Children and Adolescents, 1997-2016. JAMA Netw Open 1: e181471.
- Agency for Healthcare Research and Quality. Diagnosis of Attention-Deficit/Hyperactivity Disorder. Clinical Focus. Rockville, MD, October 1999. www.ahrq.gov/clinic/tp/adhddtp.htm.
- Larson K, Russ SA, Kahn RS, Halfon N (2011) Patterns of comorbidity, functioning, and service use for US children with ADHD, 2007. Pediatrics 127: 462.
- Pliszka S, AACAP Work Group on Quality Issues (2007) Practice parameter for the assessment and treatment of children and adolescents with attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry 46: 894.
- Wolraich ML, Hannah JN, Pinnock TY, A Baumgaertel, J Brown (1996) Comparison of diagnostic criteria for attention-deficit hyperactivity disorder in a county-wide sample. J Am Acad Child Adolesc Psychiatry 35: 319-324.
- Jensen PS, Hinshaw SP, Kraemer HC, N Lenora, J H Newcorn, et al. (2001) ADHD comorbidity findings from the MTA study: comparing comorbid subgroups. J Am Acad Child Adolesc Psychiatry 40: 147-158.
- Wolraich ML, Hannah JN, Baumgaertel A, Feurer ID (1998) Examination of DSM-IV criteria for attention deficit/hyperactivity disorder in a county-wide sample. J Dev Behav Pediatr 19: 162-168.
- Biederman J, Newcorn J, Sprich S (1991) Comorbidity of attention deficit hyperactivity disorder with conduct, depressive, anxiety, and other disorders. Am J Psychiatry 148: 564-577.
- Kessler RC, Adler L, Barkley R, Joseph Biederman, C Keith Conners, et al. (2006) The prevalence and correlates of adult ADHD in the United States: Results from the National Comorbidity Survey Replication. Am J Psychiatry 163: 716-723.
- Butterfield ME, Saal J, Young B, Young JL (2016) Supplementary guanfacine hydrochloride as a treatment of attention deficit hyperactivity disorder in adults: A double blind, placebo-controlled study. Psychiatry Res 236: 136-141.
- WHO Collaborating Centre for Drug Statistics Methodology.
- Wilens TE, Morrison NR, Prince J (2011) An update on the pharmacotherapy of attention-deficit/hyperactivity disorder in adults. Expert Rev Neurother 11: 1443-1465.
- Barbaresi W, Katusic S, Colligan R, A Weaver, V Pankratz, et al. (2004) How common is attention-deficit/hyperactivity disorder? Towards resolution of the controversy: Results from a population-based study. Acta Paediatr Suppl 93: 55-59.
- Boyle CA, Boulet S, Schieve LA, Cohen RA, Blumberg SJ, et al. (2011) Trends in the prevalence of developmental disabilities in US children, 1997-2008. Pediatrics 127: 1034-1042.
- Wehmeier PM, Dittmann RW, Banaschewski T (2015) Treatment compliance or medication adherence in children and adolescents on ADHD medication in clinical practice: Results from the COMPLY observational study. Atten Defic Hyperact Disord 7: 165-174.
- Lichtenstein P, Halldner L, Zetterqvist J, Sjölander A, Serlachius E, et al. (2012) Medication for attention deficit-hyperactivity disorder and criminality. N Engl J Med 367: 2006-20
- Charach A, Gajaria A (2008) Improving psychostimulant adherence in children with ADHD. Expert Rev Neurother 8: 1563–15
- Grootens-Wiegers P, Hein IM, van den Broek JM, de Vries MC (2017) Medical decision-making in children and adolescents: Developmental and neuroscientific aspects. BMC Pediat 17: 120.
- Schaefer MR, Wagoner ST, Young ME, Rawlinson AR, Kavooet al. (2019) Subjective Versus Objective Measures of Medication Adherence in Adolescents/Young Adults with Attention-Deficit Hyperactivity Disorder. J Dev Behav Pediatr 40: 54-59.
- Gray WN, Kavookjian J, Shapiro SK, Wagoner ST, Schaefer MR, et al. (2018) Transition to College and Adherence to Prescribed Attention Deficit Hyperactivity Disorder Medication. J Dev Behav Pediatr 39: 1-9.
- Charach A, Fernandez R (2013) Enhancing ADHD medication adherence: challenges and opportunities. Curr Psychiatry Rep 15: 371.
- Treuer T, Méndez L, Montgomery W, Wu S (2016) Factors affecting treatment adherence to atomoxetine in ADHD: A systematic review. Neuropsychiatr Dis Treat 12: 1061-83.
- Gajria K, Lu M, Sikirica V, Greven P, Zhong Y, et al. (2014) Adherence, persistence, and medication discontinuation in patients with attention-deficit/hyperactivity disorder-a systematic literature review. Neuropsychiatr Dis Treat 10: 1543-1569.
- Barner JC, Khoza S, Oladapo A (2011) ADHD medication use, adherence, persistence and cost among Texas Medicaid children. Curr Med Res Opin 27: 13-22.
- Cramer JA, Roy A, Burrell A, Fairchild CJ, Fuldeore MJ, et al. (2008) Medication compliance and persistence: Terminology and definitions. Value Health 11: 44-47.
- Marcus SC, Durkin M (2011) Stimulant adherence and academic performance in urban youth with attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry 50: 480-489.
- Hodgkins P, Sasane R, Christensen L, Harley C, Liu F (2011) Treatment outcomes with methylphenidate formulations among patients with ADHD: Retrospective claims analysis of a managed care population. Curr Med Res Opin 27: 53-62.
- Emilsson m, Gustafsson PA, Öhnström G, Marteinsdottir I (2017) Beliefs regarding medication and side effects influence treatment adherence in adolescents with attention deficit hyperactivity disorder. Eur Child Adolesc Psychiatry 26: 559-571.
- Women and Psychotropic Drugs: Research in Primary Care.Rev Asoc Esc Neuropsiq 91: 37-61.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...