Lupine Publishers Group
Lupine Publishers
Menu
Case Report(ISSN: 2770-5447) 
Hypertrophic Cardiomiopathy in Children: The Need of Heart Transplantation Volume 2 - Issue 1
Daniela Di Lisi1*, Francesca Macaione1, Giuseppina Novo1 and Calogero Comparato2
- 1Division of Cardiology, Italy
- 2Division of Pediatric Cardiology, Italy
Received: April 04, 2019; Published: April 17, 2019
Corresponding author: Daniela Di Lisi, Division of Cardiology, Palermo, Italy
DOI: 10.32474/ACR.2019.02.000130
Abstract
Hypertrophic cardiomyopathy (HCM) is the most common cardiac disease affecting the cardiac muscle. It can manifest in different forms with or without left ventricular outflow obstruction, with or without right ventricle involvement. Forms with biventricular hypertrophy seem to have poor prognosis. In our case, we describe a young patient with sarcomeric biventricular hypertrophic cardiomyopathy (MYH7 mutation), the poor prognosis of this form and strategies options adopted after failure of medical treatment. It is not always easy the management of hypertrophic cardiomiopathy, after medical treatment failure, especially in children. In some cases, heart transplantation is the only one therapeutic option.
Keywords: Hypertrophic Cardiomiopathy; Right Ventricular Hypertrophy; Heart Transplantation
Introduction
Hypertrophic cardiomiopathy (HCM) is the most common cardiac disease affecting the cardiac muscle and is characterized by heterogeneous genetic, morphological, functional, and clinical features. It is also one of the main causes of sudden cardiac death (SDC) in the young. Left ventricular hypertrophy with left ventricular outflow obstruction (LVOTO) is the most characteristic feature of HCM. There are also variant of HCM without LVOTO, with apical hypertrophy, with medio-ventricular obstruction and with right ventricular hypertrophy. The treatment and the prognosis of HCM seem to be variable on the basis of different forms, the age at presentation, sarcomeric gene mutations or rare phenocopies. Heart transplantation (HT) is the only therapeutic option for selected patients with HCM and refractory heart failure. In effect ESC guidelines recommend heart transplantation in eligible patients who have an LVEF < 50% and NYHA functional Class III–IV symptoms despite optimal medical therapy or intractable ventricular arrhythmia (II a); in eligible patients with normal LVEF (50%) and severe drug refractory symptoms (NYHA functional Class III–IV) caused by diastolic dysfunction (II b)[1].
Right ventricular hypertrophy (SRVH) is a relatively rare subtype of HCM. The anatomic, genetic, clinical, and prognostic characteristics of patients with SRVH and the clinical relevance of these characteristics have not been described widely in the literature [2,3]. MYBPC3 gene mutations have previously been described in two patients with RV hypertrophy. In a recent study, 90% of HCM patients with SRVH were found to possess relevant sarcomere protein mutations and variations in the MYH7 (Myosin heavy chain 7) and TTN genes, followed by variations in MYBPC3. Always in this study 73% of HCM patients with SRVH and multiple sarcomere gene mutations had poor prognosis. 7 In addiction MYH7 mutations can cause hypertrophic cardiomyopathy or skeletal myopathies with or without cardiac involvement, on the basis of the side of mutation. In our case, we describe the poor prognosis and treatment strategies of a young patient with biventricular hypertrophic cardiomyopathy and MYH7 mutation.
Case Report
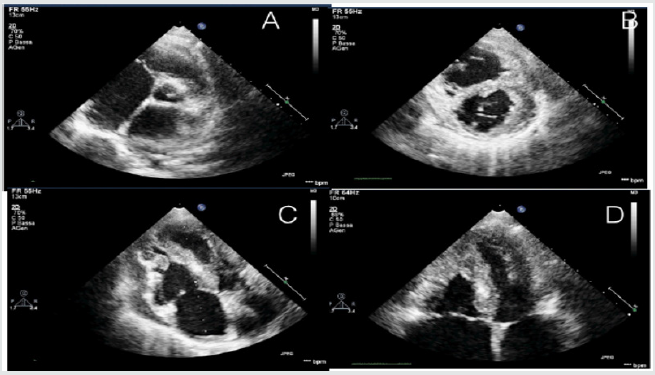
A 12-year-old young woman with familiarity for hypertrophic cardiomyopathy (mother and mother’s twin with biventricular hypertrophic cardiomiopathy and MYH7 mutation) was hospitalized in our hospital for dyspnea after mild-moderate efforts and reduced functional capacity (NYHA Class II). Mother and aunt of the patient were asymptomatic with good functional capacity. Patient had the same genetic mutation of mother and aunt (p.Asn696Ser heterozygosis MYH7) but with increased and poor phenotypic expression [4]. Echocardiography and cardiac magnetic resonance were performed showing a hypertrophic cardiomyopathy with right ventricular involvement. Precisely, cardiovascular imaging showed left ventricle asymmetric hypertrophy especially at the level of anterior and inferior wall (basal and mild anterior wall =14 mm, z score= 3,5; antero-lateral basal wall = 12 mm, z score 2,78; mild inferior wall = 14 mm and apical inferior wall = 12 mm) with normal ejection fraction (FE = 62% at CMR) and moderate diastolic dysfunction (panel B and D). In addiction wall thickness of right ventricle outflow and basal-mild free wall were increased (= 13 mm) with apical obstruction and development of maximum gradient of 10 mmHg (PANEL A and C) [5,6] (Figure 1).
The function of right ventricle was at inferior limits (FE = 51% at CMR, TAPSE = 16 mm at echocardiography). Thus the patient had an interesting right ventricle involvement and moderate diastolic dysfunction of left ventricle. She had not arrhythmia at ECG-Holter but she had reduced functional capacity. also demonstrated at stress test. Stress test was suspended at 6 min (Bruce Protocol) after pre-syncopal symptoms: lack of adaptation of the blood pressure to the effort was observed. In addition, from several months she had pre-syncopal episodes at the peak of the effort. ECG showed left ventricular hypertrophy and biatrial enlargement. Pro BNP was increased = 5841 pg/ml. Considering clinical situation, we decided to start medical treatment with betablockers (bisoprolol) but the patient didn’t tolerate medical treatment. Thus, we decided to start low dose of captopril without improvement of symptomatology. Also, treatment with diuretic was not tolerate by patient [7,8]. Therefore, considering symptom refractory to medical therapy, the poor prognosis and the impossibility to optimize medical treatment, we decided to plan cardiac transplantation, the only option possible at this moment.
Thus right catheterization was performed and patient was inserted in heart transplantation list. ICD implantation was not considered in the absence of ventricular arrhythmia and other factors. Discussion: hypertrophic cardiomyopathy associated with MYH7 mutation and right ventricle involvement seems to have poor prognosis, especially if right ventricle hypertrophy is severe [9]. In effect the young patient had a greater right ventricular hypertrophy compared than mother and aunt. In these cases, after medical treatment failure, heart transplantation seems to be the only strategy to improve symptomatology and quality of the life of the patient. Especially in pediatric population, it is not always easy the management of hypertrophic cardiomiopathy after medical treatment failure and heart transplantation seems to be the only one therapeutic option. Other study are needed to study some variants of HCM with right ventricle hypertrophy, their treatment and prognosis.
References
- Elliott P, McKenna WJ (2004) Hypertrophic cardiomyopathy. Lancet 363(9424): 1881-1891.
- Maron MS, Olivotto I, Zenovich AG, Link MS, Pandian NG, et al. (2006) Hypertrophic cardiomyopathy is predominantly a disease of left ventricular outflow tract obstruction. Circulation 114(21): 2232-2239.
- Rosmini S, Biagini E, O’Mahony C, Bulluck H, Ruozi N, et al. (2017) Relationship between aetiology and left ventricular systolic dysfunction in hypertrophic cardiomyopathy. Heart 103(4): 300-306.
- Biagini E, Spirito P, Leone O, Picchio FM, Coccolo F, et al. (2008) Heart transplantation in hypertrophic cardiomyopathy. Am J Cardiol 101(3): 387-392.
- Elliott PM, Anastasakis A, Borger MA, Borggrefe M, Watkins H, et al. (2014) 2014 ESC Guidelines on diagnosis and management of hypertrophic cardiomyopathy: the Task Force for the Diagnosis and Management of Hypertrophic Cardiomyopathy of the European Society of Cardiology (ESC). Eur Heart J 35(39): 2733-2779.
- Girolami F, Ho CY, Semsarian C, Baldi M, Will ML, et al. (2010) Clinical features and outcome of hypertrophic cardiomyopathy associated with triple sarcomere protein gene mutations. J Am Coll Cardiol 55(14): 1444-1453.
- Marziliano N, Merlini PA, Vignati G, Orsini F, Motta V, et al. (2012) A case of compound mutations in the MYBPC3 gene associated with biventricular hypertrophy and neonatal death. Neonatology 102(4): 254-258.
- Guo X, Fan C, Tian L, Liu Y, Wang H, et al. (2017) The clinical features, outcomes and genetic characteristics of hypertrophic cardiomyopathy patients with severe right ventricular hypertrophy. PLoS One 12(3): e0174118.
- Fiorillo C, Astrea G, Savarese M, Cassandrini D, Brisca G, et al. (2016) MYH7-related myopathies: clinical, histopathological and imaging findings in a cohort of Italian patients. Orphanet J Rare Dis 11(1): 91.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...