Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2638-5945
Research Article(ISSN: 2638-5945) 
Understanding Limits of Parametrial Resection in Radical Hysterectomy: A Randomized Controlled Trial Volume 4 - Issue 2
Fortunato Genovese1, Stefano Siringo1*, Attilio Tuscano2, Francesco Cannone3, Vito Leanza1, Francesco Cosentino4, Stefano Palomba2 and Marco Palumbo1
- 1Institute of Obstetric and Gynecologic Pathology, Department of Surgery, San Marco Hospital, University of Catania, Italy
- 2UOC of Obstetrics and Gynaecology, GOM. Bianchi-Melacrino-Morelli, Italy
- 3Division of Obstetrics and Gynaecology, Italy
- 4UOC Gynecology Oncology, Gemelli Molise, Università Cattolica Sacro Cuore, Italy
Received: December 07, 2020 Published: December 17, 2020
Corresponding author: Stefano Siringo, Institute of Obstetric and Gynecologic Pathology, Department of Surgery, San Marco Hospital, University of Catania, Catania, Italy
DOI: 10.32474/OAJOM.2020.04.000184
Abstract
Objective: It is well known that the complexity of pelvic anatomy, although the large number of educational resources, sometimes makes it difficult for gynaecologists, not trained in surgical oncology, to understand operations performed for oncological indications. The purpose of this study is to evaluate if adding specific educational materials (medical illustrations realized ad hoc) to the reading comprehension alone of the latest Querleu-Morrow Classification of radical hysterectomy (2017) may help Ob-Gyn residents and general ob-gyn attendings to better understand limits of parametrial resection in radical hysterectomy from type A to type C2.
Study Design: randomized controlled trial.
Setting: Institute of Obstetric and Gynecologic Pathology, University of Catania, Italy.
Materials and methods: 30senior Ob/Gyn residents and 30 general Ob/Gyn attending were enrolled to the study, and randomly allotted in two groups, each made up by an equal number [15] of residents and attending, defined as group A and group B. The group A and B participants were both given copy of the article (2017 Update on the Querleu-Morrow Classification of Radical Hysterectomy) for reading comprehension. The group B participants, were given, beside the copy of article, 10 inedited medical illustrations, realized on the basis of this paper, as an educational aid to enhance the reading comprehension of the article. After a maximum of 1 month, allowed to both groups to review article and/or article and drawings, the level of self-perceived understanding related to parametrectomy limits in radical hysterectomy was ascertained in both groups using a numeric visual analog scale, graduated from 0to 10, where each participant was asked to rate his degree of comprehension. The data obtained were statistically analyzed using a Mann-Whitney U test.
Results: Group A participants (only article) had a lower level of comprehension of parametrectomy limits compared to group B participants (article plus drawings). The difference between the average scale score, reported by group A, equal to 5,9±1,4 and that reported by group B, equal to 7,2 ±1,5 was statistically significant (p< 0,01).
Discussion and Conclusions: The result of the present study, suggest, that beside the large body of Literature on the subject, educational materials such as , the proposed drawings may help both the general Ob/Gyn , to whom the patient may return for follow up after surgery and the Ob/Gyn resident, who is still in the learning process, to better comprehend the relationship between the extent of parametrial resection and cervical disease severity, and therefore the related post operative complications and long term sequelae.
Keywords: Radical Hysterectomy; Parametrium; Paracervix; Parametrectomy; Subperitoneal Spaces; Numeric Visual Analog Scale; Understanding; Pelvic Anatomy; Terminologia Anatomica
Introduction
Cervical cancer treatment has always represented a challenge for surgeons, radiotherapist, radiologist and medical oncologist [1]. The purpose of the surgical treatment is that of removing, with the exception of microinvasion, beside the cervix the connective tissue around it and the upper vagina, known as paracolpos or paracolpium, in a measure progressively greater depending on the size and aggressiveness of the tumor [1]. Such connettival tissue in the present paper is called in general parametrium, which may not be anatomically correct, but since this term has gained an un replaceble place in the mind of most gynaecologic surgeons, the Authors continue to use it in its extensive meaning. At the same time it is important to precise that according to the Terminologia Anatomica [2] the term parametrium should be refered to the cranial portion (above the ureter) of the cardinal ligament (unofficial term), instead paracervix should be related to the caudal portion (below the ureter) of the same ligament. The reason to extend the resectionto the sorrounding parametrium is based on the fact that the more voluminose and poor differentiatied is the tumor, the higher is the chance that the tissue around the cervix and upper vagina is infiltrated by neoplastic cells [1]. In order to define and standardize the limit of such a resection in relationship with tumor grade and stage, clinicians had to balance the risks of surgery with the necessity to excise an amount of parametrium adeguate to ensure clear margins (>3 mm) [3]. Based on the amount of resected parametrium various classes of radical hysterectomy have been developed, starting from the old Piver-Rutlege-Smith [4] to the most recent Querleu-Morrow classification [5]. Recent recomended clinical indications [1], for such operation as those reported in Table 1. The description of radical hysterectomy given in the current Literature, is more or less directed to surgeons specialized in gynaecologic oncology. The aim of the current study was to evaluate if adding specific educational materials (medical illustrations realized ad hoc) to the reading comprehension of the latest Querleu-Morrow Classification of radical hysterectomy [6] help Ob-Gyn residents and general ob-gyn attending to better understand limits of parametrial resection in radical hysterectomy from type A to type C2.
Materials and Methods
On the basis of the necessary anatomical premise (see
Appendix 2), the Authors asked a medical illustrator to realizetwo
schematic topographic pictures of the female pelvis (Figure
1 and 2), whereideally all sub-peritoneal spacesare dissected
and all parametrium components, either dorsal (posterior),
ventral (anterior) and lateral (paracervix) are represented and
differentiated from each other using a color code for each of them.
The extent of parametrial resection, which characterizes each type
of radical hysterectomy taken in considerations: A, B1 and B2,
C1 and C2, according to latest Querleu-Morrow classification of
radical hysterectomy [6], is indicated in figure 3 to 10 by coloring
in gray the corresponding portions of ventral, dorsal and lateral
parametrium, which needs to be removed.
In order to establish if these 10 drawing (figure1 to 10) may have
a didactic value, 30 senior Ob/Gyn residents and 30 general Ob/Gyn
attending were enrolled as participants to a randomized controlled
trial. The participants were randomly allotted in two groups, each
made up by an equal number of residents and attending, defined
as group A and group B. The recruitment and randomization
process required 2 months, from July 1st to August 30, 2020. The
group A participants, were emaileda letter (see Appendix 1) with
attached only a copy of the article (2017 Update on the Querleu-
Morrow Classification of Radical Hysterectomy) [6] for reading
comprehension, while the group B participants received beside the
copy of the article, the 10 inedited medical illustrations realized on
the basis of the article, as a supposed didactic aid. A brief review of
the pertinent pelvic anatomy provided by the Authors for prompt
consultation (see Appendix 2) was also attached to the mail sent to
both groups. The level of understanding parametrectomy limits in
various types of radical hysterectomy, was tested in both groups by
asking the participants to rate their self-perceived comprehension
on a numeric scale graduated from 0 to 10, enclosed to the mails
(Figure 11) in Appendix 1) sent to both groups.
It is true that in general the level of comprehension in students,
is tested by administering them multiple choice questionnaires on
specific subjects [7] and that VAS (Visual Analog Score), instead are
generally used to self-assess pain [8], and or to measure anxiety or
pruritus [9,10]. However, there are examples in Literature in whom
a visual analog scale has been used for self-assessment of a specific
subject understanding [11-13]. Each study participant, after filling
out the scale (see word file 1 in Appendix 1), was invited to send it
back to the Authors within a month from its receipt (sometimes a
telephone call, about ten days before the end of the allowed month,
was made to solicit an answer). All answers were received within
October 30th 2020. Furthermore, in order to compare results also
between homogeneous categories of participants group A was
divided in 2 subgroups, identified as subgroup Ar (made only by
senior Ob/Gyn residents) and subgroup Aa (made only by general
Ob/Gyn attending), similarly group B was divided in subgroup
Brand subgroup Ba. The data obtained were statistically analyzed
using the Mann-Whitney U test. The level of statistical significance
was defined by ap value ≤ 0.01.
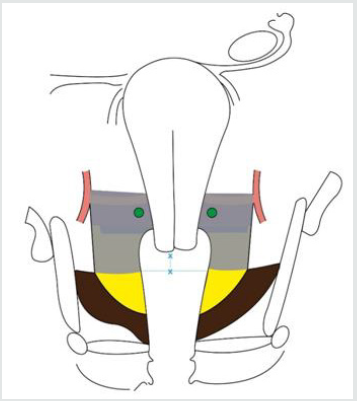
Figure 1: Schematic representation of dorsal and ventral parametrium in a paramedian sagittal section of the female pelvis (imagined after dissection of all subperitoneal spaces and going approximately through one of the bladder pillar and the omolateral uterosacral ligament).
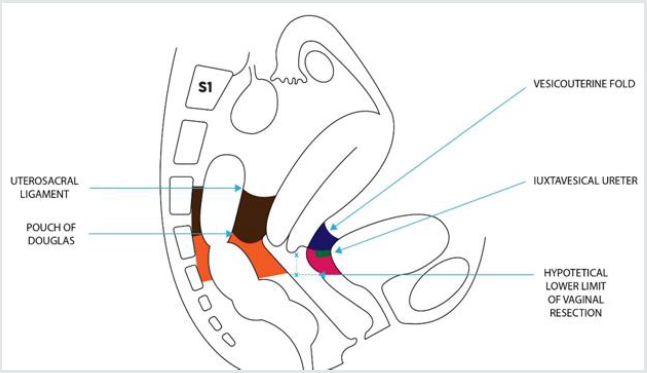
Dorsal Parametrium
• Cranial portion: retto-uterine ligament (from the utero-sacral ligament to the pouch of Douglas) with its sacral attachments.
• Caudal portion: retto-vaginal ligament (from the pouch of Douglas to the pelvic floor) with its sacral attachments.
Ventral Parametrium
• Cranial portion: vesico-uterine ligament medial and above the iuxtavesical ureter (from the vesicouterine fold to the upper limit of the iuxtavesical ureter).
• Caudal portion: vesico-vaginal ligament lateral and below the iuxtavesical ureter (from the ureter to the upper limit of the vesical trigon).
x-x: portion of upper vagina to be removed
Figure 2: Schematic representation of lateral parametrium (both sides) in a coronal section of the female pelvis going through the crossing of the uterine artery with the ureter (imagined after dissection of all subperitoneal spaces with the uterus placed in upward traction).
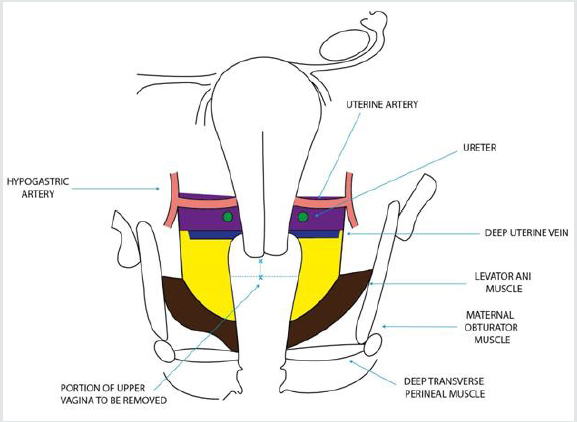
Figure 3:

Lateral Parametrium (Paracervix)
• Cranial portion: connective tissue from the uterine artery at its origin, included, to the deep uterine vein, not included.
• Caudal portion: connective tissue from the deep uterine vein, included, to the pelvic floor.
x—x: portion of upper vagina to be removed
Figure 4: Limits of resection of the dorsal and ventral parametrium in type A radical hysterectomy (the area of parametrium to be excised is colored in grey, the dissection of the Okabayashi space is not necessary).
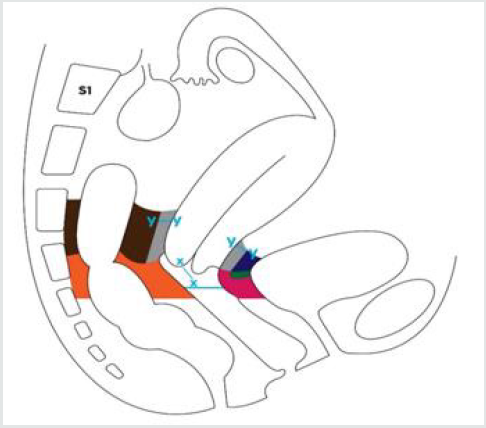
Parametrium to be Excised
y—y: 5 mm is the dorso-ventral length of parametrium to be removed.
x—x: < 10 mm from the caudal edge of the cervix.
Figure 5: Limits of resection of the lateral parametrium (paracervix) in type A radical hysterectomy (the area of parametrium to be excised is colored in grey).
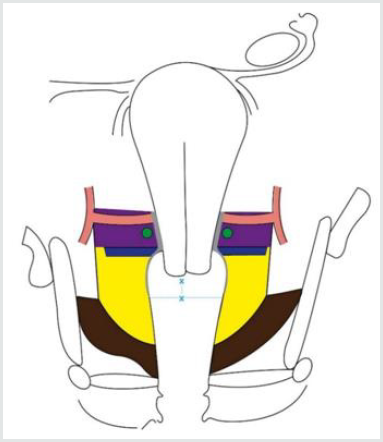
Parametrium to be excised.
x—x: < 10 mm from the caudal edge of the cervix.
Figure 6: Limits of resection of the dorsal and ventral parametrium in type B1 and B2 radical hysterectomy. Approximately half of the dorso-ventral length of the dorsal (except sacral attachments), and ventral parametrium (only upper portion) should be removed.
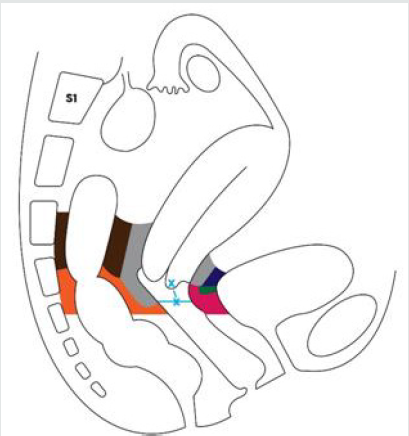
Parametrium to be excised
x—x: at least 10 mm from the caudal edge of the cervix.
Figure 7: Limits of resection of the lateral parametrium (paracervix) in type B1 and B2 radical hysterectomy.
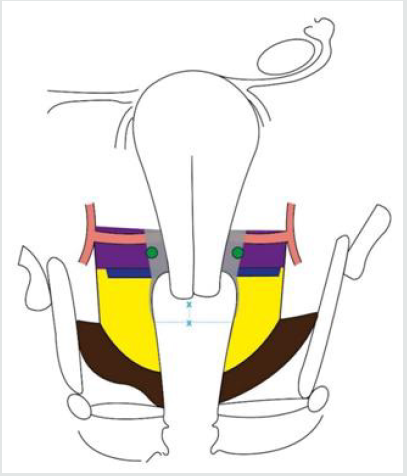
Parametrium to be excised
x—x: at least 10 mm from the caudal edge of the cervix.
Figure 8: Limits of resection of the dorsal and ventral parametrium in type C1 radical hysterectomy.
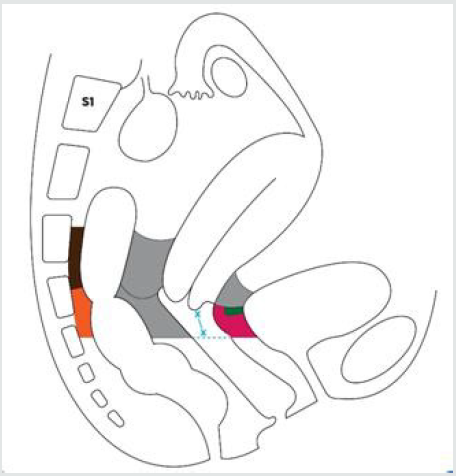
Parametrium to be excised
x—x: as necessary from the caudal edge of the cervix.
Figure 9: Limits of resection of the lateral parametrium (paracervix) in type C1 radical hysterectomy.
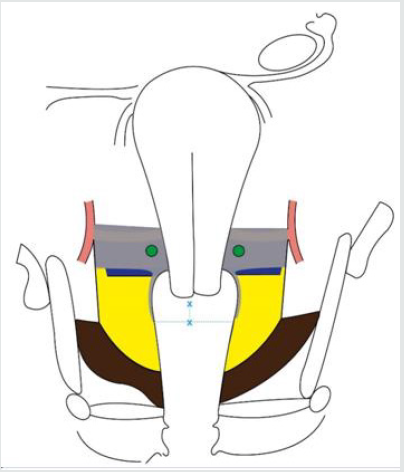
Parametrium to be excised
x—x: as necessary from the caudal edge of the cervix.
Figure 10: Limits of resection of the dorsal and ventral parametrium in type C2 radical hysterectomy (the area of parametrium to be excised is colored in grey, the dissection of the medial pararettal space, Okabayashi space, is omitted).
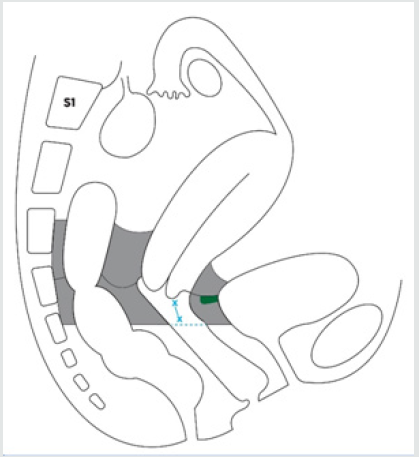
Parametrium to be excised
x—x: as necessary from the caudal edge of the cervix.
Table 1: Indications to different classes of radical hysterectomy - Guidelines 2018 ESGO.
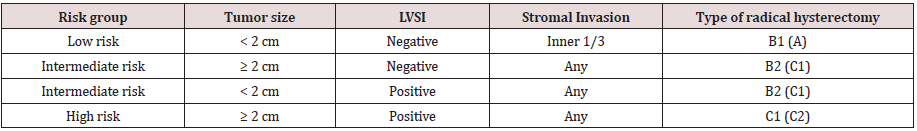
ESGO = European Society of Gynaecologic Oncology
LVSI = Lynphovascular Space Invasion
Results
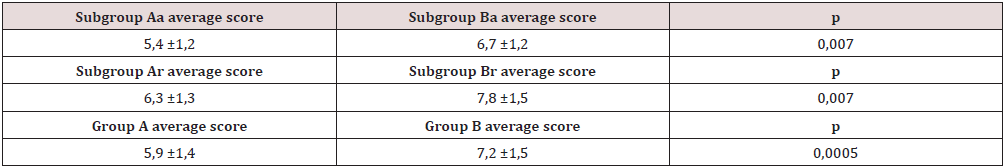
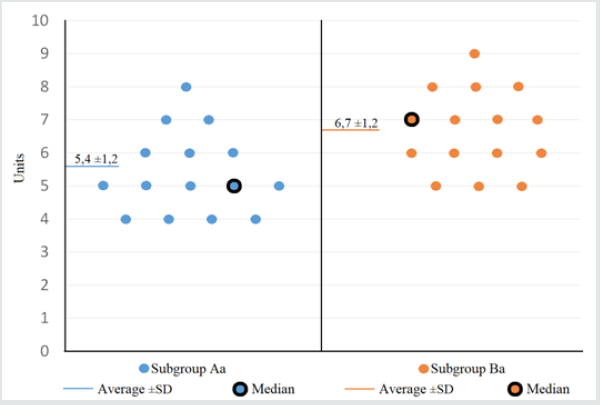
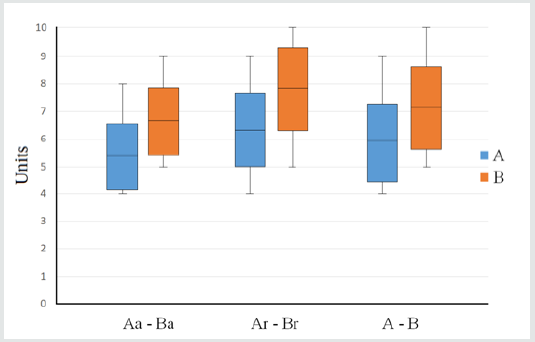
All the recruited participant adhered to the protocol and mailed their answer to the Authors within the allowed month. The numeric analogue scale scores, obtained by each participant to the study, are reported for every different subgroup in (Figure 11, 12). As shown in (Figure 13) (Table 2), the average understanding value for both attendings (5,4±1,2) and residents (6,3 ±1,3) is significantly lower (p<0.01) in subgroups Aa and Ar compared with that in subgroups Ba (6,7 ±1,2) and Br (7,8 ±1,5). Similarly, the cumulative average score of residents and attendings, taken together, seen in group A (5,9±1,4) is also significantly lower (p<0.01), than that found in group B (7,2±1,5).
Figure 11: Limits of resection of the lateral parametrium (paracervix) in type C2 radical hysterectomy (the area of parametrium to be excised is colored in grey).
Parametrium to be excised
x—x: as necessary from the caudal edge of the cervix.
Figure 13: Comparison of score averages (± SD) between subgroups and groups A and B. SD = Standard Deviation.
Discussion
It is true that in the Western Countries procedures such as
radical hysterectomy today are generally performed by gynaecologic
surgeons trained in gynaecologic oncology, and therefore such
didactic illustrations, may be seen as pleonastic and superfluous in
certain environments; however, considered that:parametrectomy
is the main cause of postoperative complications[1,14],both the
general Ob/Gyn attending and the Ob/Gyn residents, often deal
with the patient in the immediate and/or subsequent postoperative
period, and that, sometimes, the patient return to them for clinical
follow up,the Authors think that the 2 aforementioned professional
figures deserve a clearer comprehension of the postoperative
clinical implications correlated with the extent of parametrium
removal, which characterized each type of radical hysterectomy.
Undoubtedly the results of this study show that adding the 10
graphs to the simple reading of the article on the classification of radical hysterectomy [6] ameliorates significantly the level of
comprehension of parametrectomy extent in both residents and
general attendings and this seems to, somehow, fulfil the Author’s
study objective.
Nevertheless the Authors are aware that the present study has
a few limits, such as: the limited number of participants, the fact
that the drawings are based on their inter pretation of the Querleu’s
article, and that, in other words, the illustrations proposed, even
if thought as faithful to the text, are not validated by the article’s
Authors, and, last but not least, the difficulty to objectively measure
the level of understanding of the participants, measure simply
based on a numeric analogous scale score. The study has at least
two biases. The first one is that the self-perceived understanding
of parametrectomy limits measured in both groups of participants
with visual analog scales not necessarily reflect a real improvement
in comprehension. The true of the matter is that this type of
understanding is hard to test even all the correct answers to an
hypothetical multiple choice questionnaires does not guarantee a
real understanding of this specific subject; the Authors think that
this particular type of comprehension probably could be better
verified only by an expert gynaecologic oncology surgeon either in
the operating room or in the cadaver dissection room.
The other bias, less relevant, is that an improving in
comprehension is in general expected when the amount of
educational material on a specific subject is increased. However,
such improvement is not automatically achieved and sometimes
the added educational resource not only does not ameliorate
comprehension, but even it has a detrimental effect on it.
Although the aforesaid confounders and bias, the Authors retain
that their results may, at least, encourage and stimulate future and
better didactic efforts in the direction of making the anatomical and
functional meaning of parametrectomy and its clinical relevance (in
relation to the various class of radicality) more understandable for
general gynaecologist or future professionals, not necessarily going
to be specialized in gynaecologic oncology.
Conclusion
the Authors, on the basis of the appreciation expressed by residents and attending for their didactic initiative, think that the improvement in knowledge triggered by the graphs will positively affect patient care and that further simplified educational models, either two or three-dimensional should be developed in the near future to better serve this purpose. Furtherly illustrations are those presented could be used by clinicians at the time of informed consent to give also patients affected by cervical cancers a better idea of the type of surgery to whom they will undergo.
References
- David Cibula, Richard Pötter, François Planchamp, Elisabeth Avall-Lundqvist, Daniela Fischerova, et al. (2018) The European Society of Gynaecological Oncology European Society for Radiotherapy andOncology/European Society of Pathology Guidelines forthe Management of Patients With Cervical Cancer. International Journal of Gynecological Cancer 28(4): 641-655.
- Ercoli A, Delmas V, Fanfani F, Gadonneix P, Ceccaroni M, et al. (2005) Terminologia Anatomica versus unofficial descriptions and nomenclature of the fasciae and ligaments of the female pelvis: a dissection-based comparative study. American Journal of Obstetrics and Gynecology. 2005; 193(4): 1565-1573.
- Bisseling KC, Bekkers RL, Rome RM, Quinn MA (2007) Treatment ofmicroinvasive adenocarcinoma of theuterine cervix: a retrospective study andreview of the literature.GynecologicOncology 107: 424-430.
- Piver MS, Lee JY (2008) the 21st century role of Piver type II hysterectomy in FIGO stage IA, IB cervical cancer: a personal perspective. European Journal of Gyneacological Oncology 29(2): 109-113.
- Querleu D, Morow CP (2008) Classification of Radical Hysterectomy. The Lancet Oncology 9(3):297-303.
- Denis Querleu, David Cibula, Nadeem R Abu-Rustum (2017) 2017 Update on the Querleu-Morrow Classification of Radical Hysterectomy. Annals of Surgical Oncology 24(11): 3406-3412.
- Moss E (2001) Multiple choice questions: their value as an assessment tool. Current Opinion in Anaesthesiology.2001;14(6): 661-666.
- Marianne Jensen Hjermstad, Peter M Fayers, Dagny F Haugen, et al. (2011) Studies comparing Numerical Rating Scales, Verbal Rating Scales, and Visual Analogue Scales for assessment of pain intensity in adults: a systematic literature review 41(6):1073-1093.
- Jessica M A Purcell-Jones, Marlis Haasbroek , Justine L Van der Westhuizen, Robert A Dyer, Carl J Lombard, et al. (2019) Overcoming Language Barriers Using an Information Video on Spinal Anesthesia for Cesarean Delivery: Implementation and Impact on Maternal Anxiety. Anesthesia andanalgesia. 129(4): 1137-1143.
- Keir ST, Calhoun-Eagan RD, Swartz JJ, Saleh OA, Friedman HS, et al. (2008) Screening for distress in patients with brain cancer using the NCCN's rapid screening measure Psycho-oncology. 17(6): 621-625.
- Kennedy G, Rea JNM, Rea IM (2019) Prompting medical students to self-assess their learning needs during the ageing and health module: a mixed methods study. Medical Education Online. 2019 24(1): 1579558.
- Bensoussan L, Collado H, Viton JM, Delarque A (2009) Should European PRM residents be taught in English? The experience of the European school Marseille. Annals of Physical and Rehabilitation Medicine 52(10): 729-745.
- Daniel Hogan, Tina DiMartino, Jianfang Liu, Kari A Mastro, Elaine Larson (2018) Video-based Education to Reduce Distress and Improve Understanding among Pediatric MRI Patients: A Randomized Controlled Study. Journal of Pediatric Nursing S0882-5963(17): 30455-30464.
- Lee SH, Cho KJ, Ko MH, Cho HY, Lee KB, et al. (2018) Lim S. Factors associated with parametrial involvement in patients with stage IB1 cervical cancer: Who is suitable for less radical surgery? Obstetrics e Gynecology Science 61(1): 88-94.
- Ceccaroni M, Ceccarello M, Clarizia R, Roviglione G (2019) Anatomia chirurgica della pelvi femminile. Trattato di chirurgia ostetrica e ginecologica Italy
- Einarsson JI, Wattiez A (2016) Minimally invasive gynecologic surgery: evidence-based laparoscopic, hysteroscopic and robotic surgeries. London: JP Medical p.270
- Yabuki Y, Asamoto A, Hoshiba T, Nishimoto H, Satou N, et al. (1996) A new proposal for radical hysterectomy. Gynecologic Oncology. 1996;62(3): 370-378.
- Yabuki Y, Asamoto A, Hoshiba T, Nishimoto H, Nishikawa Y, et al. (2000) Radical hysterectomy: and anatomic evaluation of parametrial dissection. Gynecologic Oncology 77(1): 155-163.
- Tribos JB, Maas CP, Deruiter MC, Peters AA, Kenter GG, et al. (2001) A nerve-sparing radical hysterectomy: guidelines and feasibility in Western patients. International Journal of Gynecological Cancer. 11(3): 180-186.
- Masaru Nakamura, Kyoko Tanaka, Shigenori Hayashi, Tohru Morisada, Takashi Iwataet al. (2019) Local anatomy around terminal ureter related to the anterior leaf of the vesicouterine ligament in radical hysterectomy. European Journal of Obstetrics, Gynecology, and Reproductive Biology 235: 66-70.
- Shingo F, Kenji T, Noriomi M, Toshihiro H, Shigeo Y, et al. (2007) Precise anatomy of the vesico-uterine ligament for radical hysterectomy. Gynecologic Oncology 104 (1):186-191.
- Ceccaroni M, Clarizia R, Roviglione G, Ruffo G (2013) Neuro-anatomy of the posterior parametrium and surgical considerations for a nerve-sparing approach in radical pelvic surgery. Surgical Endoscopy 27(11):4386-4394.
- Ercoli A, Delmas V, Gadonneix P, Fanfani F, Villet R, ett al. (2003) Classical and nerve-sparing radical hysterectomy: an evaluation of the risk of injury to the autonomous pelvic nerves. Surgical and Radiologic Anatomy 25(3-4): 200-206.
- Okabayashi H (1921) Radical abdominal hysterectomy for cancer of the cervix uteri, modification of the Takayama operation. Surgery Gynecology Obstetrics 33: 335-341.
- Ceccaroni M, Clarizia R, Bruni F, D’Urso E, Gagliardi ML, et al. (2012) Roviglione G, Minelli L, Ruffo G. Nerve-sparing laparoscopic eradication of deep endometriosis with segmental rectal and parametrial resection: the Negrar method. A single-center, prospective, clinical trial. Surgical Endoscopy. 26(7): 2029-2045.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...