Lupine Publishers Group
Lupine Publishers
Menu
ISSN: 2641-1687
Research Article(ISSN: 2641-1687) 
Linguistic and Cognitive Validation of The Traditional Chinese Language Cantonese Acute Cystitis Symptom Score Questionnaire for Female Patients in Hong Kong with Acute, Lower, Uncomplicated Urinary Tract Infections Volume 4 - Issue 4
Kwok Hung Alastair Lai1, Jakhongir F Alidjanov2, Adrian Pilatz2, Florian M Wagenlehner2 and Kurt G Naber3*
- 1Tseung Kwan O Hospital, Accident and Emergency Department, Tseung Kwan O, Hong Kong
- 2Justus Liebig University, Clinic for Urology, Pediatric Urology and Andrology, Giessen, Germany
- *3Technical University of Munich, Department of Urology, Munich, Germany
Received: July 24, 2023; Published: July 28, 2023
Corresponding author: Kurt G. Naber, Department of Urology, Technical University of Munich, Germany
DOI: 10.32474/JUNS.2023.04.000193
Abstract
Since the clinical diagnosis of acute, lower, uncomplicated urinary tract infection (cystitis) can be made with high probability based on typical symptoms and absence of other genital infections, the clinical diagnosis and outcome should be established according to better defined parameters. Therefore, the Acute Cystitis Symptom Score (ACSS) was introduced as a standardized selfreporting diagnostic questionnaire for clinical diagnosis, differential diagnosis, and patient-reported outcome measure in women with acute uncomplicated cystitis. The ACSS originally developed in Uzbek and Russian language and validated and available in many other languages is now translated and linguistically validated in traditional Chinese language Cantonese according to internationally accepted guidelines and can be used for female patients with acute, lower, uncomplicated urinary tract infections in Hong Kong for clinical studies and daily practice.
Keywords: Acute cystitis symptom score; ACSS; traditional chinese language cantonese; acute uncomplicated cystitis; female patients; diagnostics; patient-reported outcome
Introduction
Urinary tract infections are a leading cause of bacterial infections in women [1] and amongst the most common bacterial infections in general, with the majority being attributable to Escherichia coli [2]. These infections tend to recur, and this tendency increases with each additional infection [3-6]. The frequency of recurrence varies depending on the type of infection, as well as patient age and gender. Despite acute treatment, 30–50% of women who have a urinary tract infection will experience a recurrence within 6-12 months [7]. Risk factors for recurrent urinary tract infection are discussed in depth by Cai [8]. The principal risk factor in sexually active pre-menopausal women is frequency of sex. Other behaviors including use of spermicide, having a new sexual partner within the past year, pre/post-coital voiding habits, delayed voiding habits or periodicity of urination and vaginal douching also affect risk of recurrence. In addition, early onset (below 15 years of age), family history, body-mass index and urine voiding disorders all increased risk in younger women [9].
Major risk factors in older women appear to be substantially related to the effects of reduced oestrogen levels and include atrophic vaginitis, cystocele, increased post-void urine volume and functional status deterioration [10-11]. Cai et al. have created a nomogram for the calculation of risk of recurrence which has substantial clinical utility [12]. The costs associated with community-acquired urinary tract infection overall are significant, amounting to around 1.6 billion US dollars each year in the United States of America [13]. According to the European Association of Urology guidelines on urological infections acute, lower, uncomplicated urinary tract infection (cystitis) is defined as acute, sporadic, or recurrent cystitis limited to non-pregnant women with no known relevant anatomical and functional abnormalities within the urinary tract or comorbidities. The diagnosis of acute, uncomplicated cystitis can be made with a high probability based on a focused history of lower urinary tract symptoms (dysuria, frequency, and urgency) and the absence of vaginal discharge [14].
According to European Medicines Agency (EMA) and U.S. Food and Drug Administration (FDA) guidelines female patients can be included in a clinical trial on acute, uncomplicated urinary tract infection (cystitis) if they complain about typical symptoms of cystitis and the urinalysis shows leukocyturia (>20 leukocytes per ml) [15,16]. It could, however, been demonstrated in earlier studies, that the diagnostic value can be significantly increased, if not only the presence, but also the severity of symptoms is taken into consideration [17]. At the same time, it is also important not to overlook additional symptoms indicating any infection of the upper urinary tract, such as pyelonephritis, or differentiation to other genital infections. According to clinical daily practice, systematic urine cultures are neither taken nor necessary before treatment if the clinical diagnosis of acute, uncomplicated cystitis is made with high probability, because the microbiological results are usually not received back from the laboratory within 2 or 3 days and the recommended treatment duration is also short, either single dose (Fosfomycin trometamol) or about 3, sometimes 5 days depending on the antibiotic chosen.
Any further investigation after start of treatment depends on the patient-reported clinical outcome, which should be considered not only as an overall assessment by the patient, but also by the gradual resolution of the typical symptoms and the resulting improvement in the quality of life. To be able to query all these items easily the Acute Cystitis Symptom Score (ACSS) was introduced as a simple and standardized self-reporting diagnostic questionnaire, which has proven its suitability for clinical diagnosis, differential diagnosis, and patient-reported outcome measure in women with acute uncomplicated cystitis [18-20]. The ACSS has been originally developed in Uzbek and Russian languages and has now been translated and validated linguistically and clinically in several other languages and is available online in different languages (http://www.acss.world). This study aimed to translate and linguistically validate the ACSS in traditional Chinese language Cantonese for female patients with acute, lower, uncomplicated urinary tract infections in Hong Kong for clinical studies and daily practice.
Methods and Results
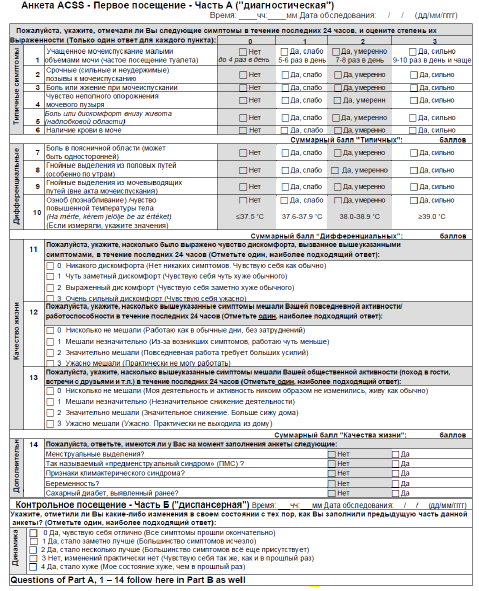
For translating health related questionnaires, we followed international recommendations. After reviewing the literature with 891 references and finally 23 publications meeting their inclusion criteria representing 17 sets of methods and 22 reviews Aquadro et al [24] recommended a multistep approach, which we followed in principle. Stage I: Two forward translations of the ACSS from the original Russian [21] (Table 1) and the American English [22] (Table 2) to traditional Chinese were performed by two professional, independent translators with Chinese as their mother language. Phase II: After discussion of the two translations (T1 and T2) by the scientific committee, consisting of physicians with traditional Chinese as mother language and the copyright holders, a consensus version (T12) was established. Phase III: This consensus version was then again translated backward to Russian and American English by two professional translators with Russian and American English as their mother language, respectively, in order to rule out any important discrepancies between the original and the target languages [23-25]. Phase IV: After discussion and approval by the scientific committee the consented version was used for the Phase V: cognitive assessment process by interviewing 7 female subjects with different ages and educational level and 5 physicians treating those patients in Hongkong. Phase VI: All comments were discussed within the scientific committee and the final study version of the ACSS in traditional Chinese language could be obtained (Table 3).
Alidjanov et al. Urologiia 2014, 6, 14-22 [22]
Alidjanov et al. Antibiotics (Basel) 2020, 9, 929 [23]
Table 3: Acute Cystitis Symptom Score (ACSS)—Questionnaire in traditional Chinese language Cantonese.

Discussion
Although according to EMA and FDA guidelines female patients with typical symptoms of acute, uncomplicated cystitis and pyuria can be included into corresponding clinical studies, but only those patients with finally established significant bacteriuria (colony forming units (CFU) >105/ml) will be accepted for the primary study aim. However, bacteriuria of ≥105 CFU/mL in adults was originally defined as significant only for the diagnosis of pyelonephritis [26]. In 1982, however, Stamm et al. [27] documented that the levels of ≥ 105 CFU/mL of a pathogen in urine have a very high specificity (99%) but a very low sensitivity (51%) for the diagnosis of AC. Bacteriuria of ≥ 102 CFU/mL was suggested by the authors as the best diagnostic criterion (sensitivity, 95%; specificity, 85%). In 2013, Hooton et al. [28] confirmed that E. coli identified as low as 101–102 CFU/mL was sensitive and specific for the diagnosis of AC in symptomatic women. But still, about 20% of these symptomatic female patients were culture “negative” even when being tested for such low counts.
Quantitative PCR (qPCR) for E. coli and S. saprophyticus finally demonstrated that almost all women with symptoms suggestive for UTIs and a “negative” culture still have an infection with E. coli [29]. Therefore, according to several guidelines, such as European Association of Urology (EAU) guidelines and German National S3 Guideline, the clinical diagnosis of uncomplicated cystitis can be made with high probability based on a focused history of lower urinary tract symptoms (dysuria, frequency and urgency) and in absence of vaginal discharge [30]. Since, however, specific genitourinary symptoms may be not always necessarily related to cystitis, we could demonstrated that the consideration of most of the so-called „typical“ symptoms and also of their severity is important to improve the clinical diagnosis of acute cystitis, whereas all symptoms only with a mild severity did not significantly differentiate between patients with acute uncomplicated cystitis and controls as has been shown in this international study using the ACSS questionnaire in 517 female subjects with seven different languages comparing 285 patients with acute uncomplicated cystitis and 232 controls without acute uncomplicated cystitis.
The ROC (receiver operating characteristic) curve analysis revealed a difference in diagnostic value between the symptoms, while dysuria was showing the highest diagnostic value. Nevertheless, considering all symptoms and their severity together revealed the best diagnostic value. Using a summary score of the six typical symptoms included in the ACSS questionnaire of 6 and higher a clinical diagnosis [95% confidence interval] with a sensitivity of 0.87 [0.83; 0.91] and specificity of 0.88 [0.83; 0.91] could be established. If, however, the cut-off value of the ACSS is combined with positive leukocyturia (≥ 25 leukocytes per μL), then the specificity and sensitivity change to 0.96 [0.93; 0.98] and 0.73 [0.67; 0.78], respectively. For patient-reported outcome (PRO) measure not only the presence and absence of symptoms, but also the development of symptom severity and effect on quality of life need to be established, which can be done by using such a questionnaire as well. In this internationally performed study in female patients with AC several thresholds to define a successful clinical outcome were tested.
Finally, the reduction of the summary score of the typical symptoms to 5 or less with no symptoms more than 1 (mild) and without visible blood in urine was finally the recommended threshold for clinical studies to define clinical successful treatment at test of cure, which could be combined with the improvement of quality of life to not more than 1 of each of the three quality of life categories (in general because of the symptoms, work/everyday activity, social activity). Interestingly, if only the three symptoms (frequency, urgency, dyuria) mentioned by EMA or the four symptoms (frequency, urgency, dysuria, suprapubic pain) mentioned by FDA are considered in the same way, the so-called successful outcome was practically the same as using all 5 typical symptoms (frequency, urgency, dysuria, suprapubic pain, incomplete bladder emptying) asked for in the ACSS questionnaire. In all cases, visible blood in urine (gross hematuria) found at least mild in about one third of patients with acute uncomplicated cystitis at the first visit, should have disappeared at test of cure, because persistent visible blood in urine would need further diagnostic steps to exclude serious pathologies, such as bladder cancer.
Although reports of patients concerning symptoms can only be subjective by definition, by answering the same, in the meantime, familiar questionnaire at any follow-up visit, one can at least expect that by scoring the symptoms not only the presence or absence, but also the increasing or decreasing severity of each symptom reported by the patient can be considered as a quasi-objective measure. Nevertheless, the amount of the reported change may still be somehow subjective. Since, however, acute uncomplicated cystitis still can be considered a benign infection ultimately the subjective patient-reported clinical outcome is most important. Since non-antibiotic therapy also has become an alternative approach to treat acute uncomplicated cystitis in women, such a suitable patient-reported outcome measure is urgently needed, because under these conditions not the elimination of bacteriuria but the improvement of symptoms and quality of life will become the main study aim, because asymptomatic bacteriuria at test of cure would not justify further treatment [31-35]. In female patients with recurrent urinary tract infections, it was shown, that asymptomatic bacteriuria after successful treatment of the acute episode may even be preventive for recurrences [36].
Conclusion
The ACSS, a standardized self-reporting diagnostic questionnaire for clinical diagnosis, differential diagnosis, and patient-reported outcome measure in women with acute uncomplicated cystitis can be recommended for epidemiological and interventional studies, but also allows women for self-diagnosis of acute uncomplicated cystitis, which makes the ACSS also cost-effective for healthcare. The ACSS translated in traditional Chinese language Cantonese is now available to be studied clinically to get more information and experience how the ACSS will be accepted by patients and physicians with traditional Chinese Cantonese as their mother language, which also may be used for clinical studies and daily practice.
Supporting Information
Patents
The ACSS is copyrighted by the Certificate of Deposit of Intellectual Property in Fundamental Library of Academy of Sciences of the Republic of Uzbekistan, Tashkent (Registration number 2463; 26 August 2015) and the Certificate of the International Online Copyright Office, European Depository, Berlin, Germany (Nr. EU-01-000764; 21 October 2015). The Rightholders are Jakhongir Fatikhovich Alidjanov (Uzbekistan), Ozoda Takhirovna Alidjanova (Uzbekistan), Adrian Martin Erich Pilatz (Germany), Kurt Günther Naber (Germany), Florian Martin Erich Wagenlehner (Germany).
Supplementary Materials: Supplementary Tables 1-3: The ACSS versions in Russian as source language, in American English as 2nd master language, and in traditional Chinese language Cantonese (each in full version).
Authors Contribution
Conceptualization, J.F.A., A.P., F.M.W. and K.G.N.; methodology, J.F.A., A.P., F.M.W. and K.G.N.; validation, K.H.A.L. and K.G.N.; formal analysis, K.H.A.L. and K.G.N.; investigation, K.H.A.L.; resources, K.H.A.L.; data curation, K.H.A.L.; writing-original draft preparation, K.G.N.; writing-review and editing, K.H.A.L. und K.G.N.; supervision, A.P. and F.M.W.; project administration, K.H.A.L. All authors have read and agreed to the published version of the manuscript.
Funding
This study received no specific grant from any funding agency, commercial or not-for-profit sectors.
Institutional Review Board Statement:
not needed in this study.
Informed Consent Statement:
not needed in this study.
Acknowledgments
The authors thank the professional translators for their contribution and support and the participants (female subjects and physicians), who contributed by their comments to the cognitive assessment process.
Conflict of interest
K.H.A.L. declares no conflict of interest. J.A., A.P., F.M.W., and K.G.N. are copyright holders of the ACSS questionnaire.
References
- Schappert SM, Rechtsteiner EA (2011) Ambulatory medical care utilization estimates for 2007. Vital Health Stat 169: 1-38.
- Ennis SS, Guo H, Raman L, Tambyah PA, Chen SL, et al. (2018) Premenopausal women with recurrent urinary tract infections have lower quality of life. Int J Urol 25(7): 684-689.
- Foxman B (2010) The epidemiology of urinary tract infection. Nat Rev Urol 7(12): 653-660.
- Hooton TM (2001) Recurrent urinary tract infection in women. Int J Antimicrob Agents 17: 259-268.
- Foxman B (2014) Urinary tract infection syndromes: occurrence, recurrence, bacteriology, risk factors, and disease burden. Infect Dis Clin North Am 28(1): 1-13.
- Pitout JD (2010) Infections with extended-spectrum beta-lactamaseproducing enterobacteriaceae: changing epidemiology and drug treatment choices. Drugs 70(3): 313-333.
- Bonkat G, Bartoletti R, Bruyère F (2022) EAU guidelines on urological infections. EAU Guidelines Office, European Association of Urology (EAU): Arnhem, The Netherlands.
- Cai T (2021) Recurrent uncomplicated urinary tract infections: definitions and risk factors. GMS Infect Dis 9: Doc03.
- Scholes D, Hooton TM, Roberts PL, Stapleton AE, Gupta K, et al. (2000) Risk factors for recurrent urinary tract infection in young women. J Infect Dis 182(4): 1177-1182.
- Lüthje P, Brauner H, Ramos NL, Ovregaard A, Glaser R, et al. (2013) Estrogen supports urothelial defense mechanisms. Sci Transl Med 5(190): 190ra80.
- Raz R, Stamm WE (1993) A controlled trial of intravaginal estriol in postmenopausal women with recurrent urinary tract infections. N Engl J Med 329(11): 753-756.
- Cai T, Mazzoli S, Migno S, Malossini G, Lanzafame P, et al. (2014) Development and validation of a nomogram predicting recurrence risk in women with symptomatic urinary tract infection. Int J Urol 21(9): 929-934.
- Foxman B, Gillespie B, Koopman J, Zhang L, Palin K, et al. (2000) Risk factors for second urinary tract infection among college women. Am J Epidemiol 151(12): 1194-1205.
- Stamm WE, Hooton TM (1993) Management of urinary tract infections in adults. N Engl J Med 329(18): 1328-1334.
- European Medicines Agency (2018) Draft guideline on the evaluation of medicinal products indicated for treatment of bacterial infections, Revision 3. European Medicines Agency 30.
- Food and Drug Administration (2019) Uncomplicated Urinary Tract Infections: Developing Drugs for Treatment. Guidance for Industry. In: U.S. Department of Health and Human Services, Food and Drug Administration, Center for Drug Evaluation and Research (CDER).
- Alidjanov JF, Naber KG, Pilatz A, Radzhabov A, Zamuddinov M, et al. (2019) Evaluation of the draft guidelines proposed by EMA and FDA for the clinical diagnosis of acute uncomplicated cystitis in women. World J Urol 38(1): 63-72.
- Alidjanov JF, Abdufattaev UA, Makhsudov SA, Pilatz A, Akilov FA, et al. (2014) New self-reporting questionnaire to assess urinary tract infections and differential diagnosis: acute cystitis symptom score. Urol Int 92(2): 230-236.
- Alidjanov JF, Abdufattaev UA, Makhsudov SA, Pilatz A, Akilov FA, et al. (2016) The Acute Cystitis Symptom Score for Patient-Reported Outcome Assessment. Urol Int 97(4): 402-409.
- Alidjanov JF, Naber KG, Pilatz A, Radzhabov A, Zamuddinov M, et al. (2019) Additional assessment of Acute Cystitis Symptom Score questionnaire for patient-reported outcome measure in female patients with acute uncomplicated cystitis: part II. World J Urol 38(8): 1977-1988.
- Alidjanov JF, Abdufattaev UA, Makhmudov D, Mirkhamidov D, Khadzhikhanov F, et al. (2014) Development and clinical testing of the Russian version of the Acute Cystitis Symptom Score - ACSS. Urologiia 6: 14-22.
- Alidjanov JF, Naber KG, Pilatz A, Wagenlehner FM (2020) Validation of the American English version of the Acute Cystitis Symptom Score. Antibiotics (Basel) 9(12): 929.
- Acquadro C, Jambon BDE, Marquis P (1996) Language and translation issues. In Quality of Life and Pharmacoeconomics in Clinical Trials. Spilker B, Ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA. pp. 575-586.
- Acquadro C, Conway K, Giroudet C, Mear I (2004) Linguistic Validation Manual for Patient-Reported Outcomes (PRO) Instruments. MAPI Research Trust, Lyon, France.
- Acquadro C, Conway K, Giroude, C, Mear I (2012) Linguistic validation manual for health outcome assessments. Lyon: Mapi Research Trust, Lyon, France.
- Kass EH (1955) Chemotherapeutic and antibiotic drugs in the management of infections of the urinary tract. Am J Med 18(5): 764-781.
- Stamm WE, Counts GW, Running KR, Fihn S, Turck M, et al. (1982) Diagnosis of coliform infection in acutely dysuric women. N Engl J Med 307(8): 463-468.
- Hooton TM, Roberts PL, Cox ME, Stapleton AE (2013) Voided midstream urine culture and acute cystitis in premenopausal women. N Engl J Med 369(20): 1883-1891.
- Heytens S, De Sutter A, Coorevits L, Cools P, Boelens J, et al. (2017) Women with symptoms of a urinary tract infection but a negative urine culture: PCR-based quantification of Escherichia coli suggests infection in most cases. Clin Microbiol Infect 23(9): 647-652.
- Kranz J, Schmidt S, Lebert C, Schneidewind L, Mandraka F, et al. (2018) The 2017 Update of the German Clinical Guideline on Epidemiology, Diagnostics, Therapy, Prevention, and Management of Uncomplicated Urinary Tract Infections in Adult Patients: Part 1. Urol Int 100(3): 263-270.
- Gágyor I, Bleidorn J, Kochen MM, Schmiemann G, Wegscheider K, et al. (2015) Ibuprofen versus fosfomycin for uncomplicated urinary tract infection in women: randomised controlled trial. BMJ 351: h6544.
- Vik I, Bollestad M, Grude N, Baerheim A, Damsgaard E, et al. (2018) Ibuprofen versus pivmecillinam for uncomplicated urinary tract infection in women-A double-blind, randomized non-inferiority trial. PLoS Med 15(5): e1002569.
- Kronenberg A, Bütikofer L, Odutayo A, Muhlemann K, Costa B, et al. (2017) Symptomatic treatment of uncomplicated lower urinary tract infections in the ambulatory setting: randomised, double-blind trial. BMJ 359: j4784.
- Wagenlehner FM, Abramov-Sommariva D, Höller M, Steindl H, Naber KG (2018) Non-antibiotic herbal therapy (BNO 1045) versus antibiotic therapy (Fosfomycin Trometamol) for the treatment of acute lower uncomplicated urinary tract infections in women: A double-blind, parallel group, randomized, multicentre, non-inferiority phase III trial. Urol Int 101(3): 327-336.
- Kaußner Y, Röver C, Heinz J, Hummers E, Debray T, et al. (2022) Reducing antibiotic use in uncomplicated urinary tract infections in adult women: a systematic review and individual participant data meta-analysis. Clin Microbiol Infect 28(12): 1558-1566.
- Cai T, Koves B, Johansen TE (2017) Asymptomatic bacteriuria, to screen or not to screen - and when to treat? Curr Opin Urol 27(2): 107-111.

Top Editors
-

Mark E Smith
Bio chemistry
University of Texas Medical Branch, USA -

Lawrence A Presley
Department of Criminal Justice
Liberty University, USA -

Thomas W Miller
Department of Psychiatry
University of Kentucky, USA -

Gjumrakch Aliev
Department of Medicine
Gally International Biomedical Research & Consulting LLC, USA -

Christopher Bryant
Department of Urbanisation and Agricultural
Montreal university, USA -

Robert William Frare
Oral & Maxillofacial Pathology
New York University, USA -

Rudolph Modesto Navari
Gastroenterology and Hepatology
University of Alabama, UK -

Andrew Hague
Department of Medicine
Universities of Bradford, UK -

George Gregory Buttigieg
Maltese College of Obstetrics and Gynaecology, Europe -

Chen-Hsiung Yeh
Oncology
Circulogene Theranostics, England -
.png)
Emilio Bucio-Carrillo
Radiation Chemistry
National University of Mexico, USA -
.jpg)
Casey J Grenier
Analytical Chemistry
Wentworth Institute of Technology, USA -
Hany Atalah
Minimally Invasive Surgery
Mercer University school of Medicine, USA -

Abu-Hussein Muhamad
Pediatric Dentistry
University of Athens , Greece

The annual scholar awards from Lupine Publishers honor a selected number Read More...